What are the 5 main ways that antibiotics work and give some examples of each?
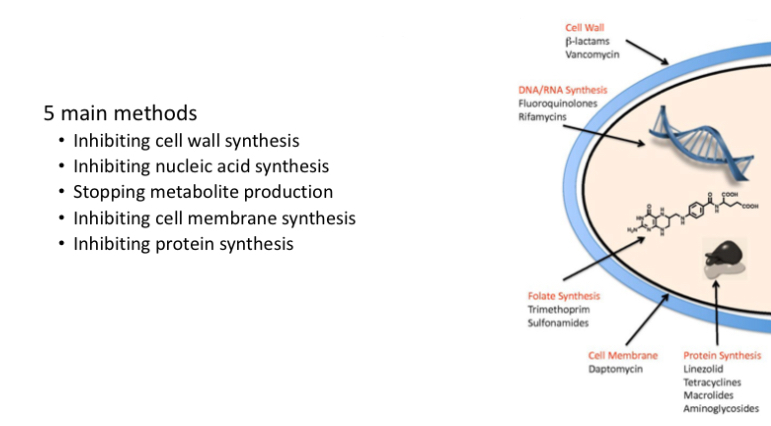
What is the difference between bactericidal and bacteriostatic antibiotics?
- Cannot use two together as bacteriocidal work best on bacteria that are replicating and bacterostatic stop division
- Bacteriostatic: macrolides, tetracycline
- Bactericidal: penicllin, ceflasporins
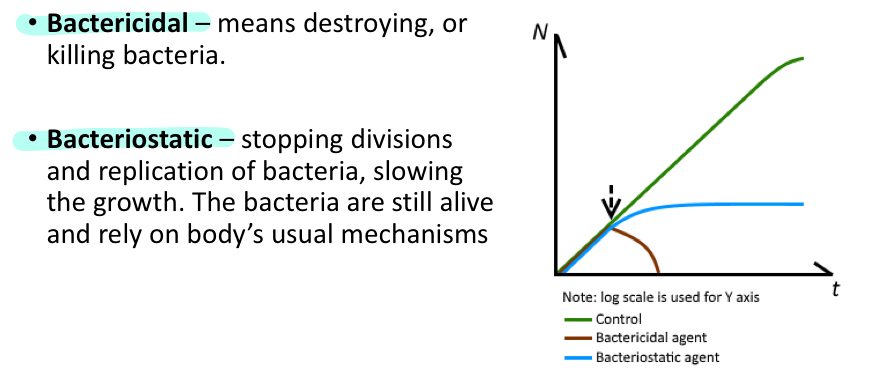
What are some ways that bacteria develop resistance to antibiotics?
- Usually beta lacatamases
- Plasmid DNA can be passed from cell to cell
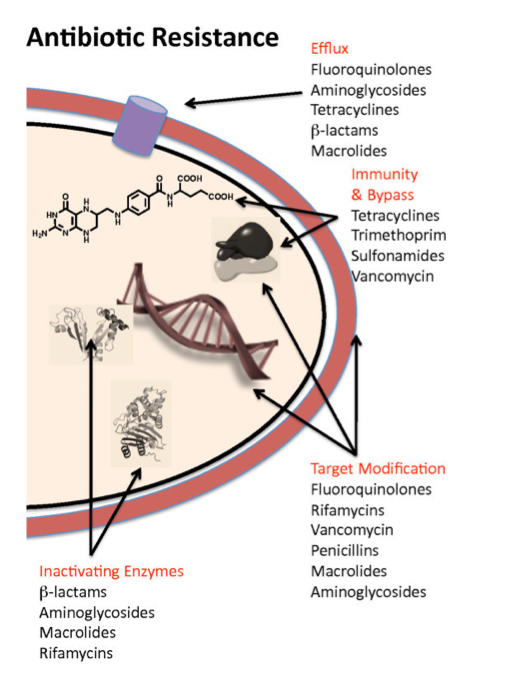
When do we need to drug monitor antibiotics?
Vancomycin monitored every 4th dose
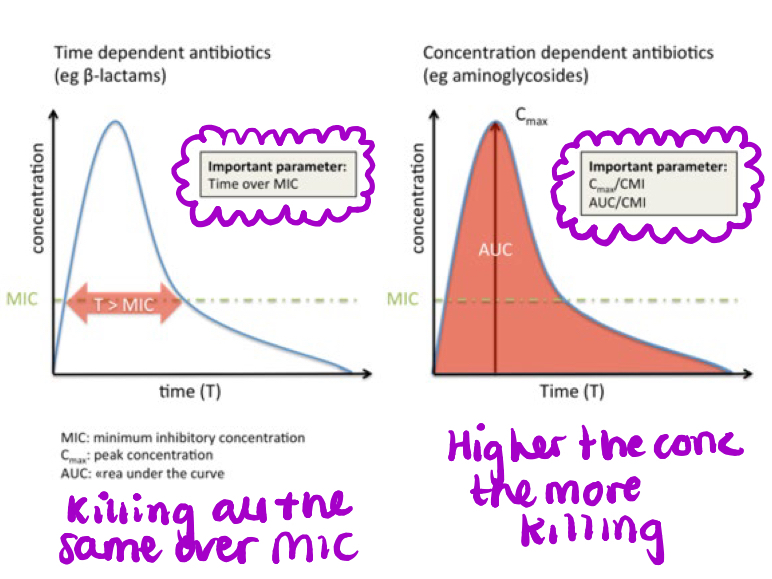
What does it mean when an antibiotic has time dependent or concentration dependent killing?
The major killing effect against an organism is produced by either the time or the concentration of the drug at the binding site
Time dependent: drugs spend a long time at binding sites as have long half life so this is what kills them e.g penicillins and macrolides
Concentration Dependent: need a certain concentration at binding sites e.g aminoglycosides
Why do we use antibiotics in general?
- Post infective treatment
- Prophylaxis before high risk surgery or for those who have conditions like asplenic to prevent infections
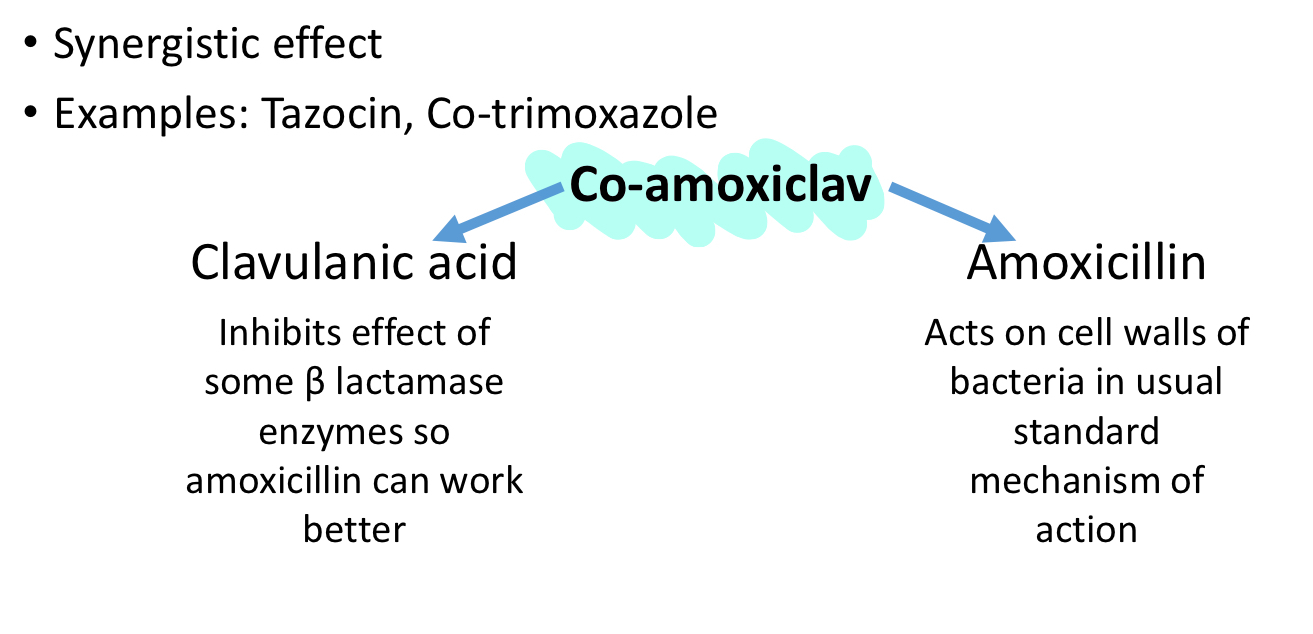
What is co-amoxiclav and why is it prescribed as a combination?
Which groups of people are at increase risk of infection?

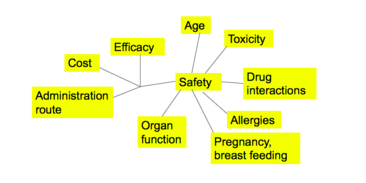
Which factors helps one determine which antibiotic is the best choice?
- Allergies and reactions e.g metronidazole and drinking
- Hepatic/Renal Impairment or Pregnancy
- What is the likely infectious agent?
- Is the patient in a high risk group? If so use 2nd line antibiotics as likely to be carrying resistant bacteria
What are the adverse events of antibiotics?
- Toxicities
- Allergic reactions
- Idiosyncratic reactions (Type B)
- Ecological effects – C.difficile, selection of resistance
- Drug interactions
What are some antimicrobial stewardship practices in place in UHL?
- Restricted antibiotics need authorisation from microbiology department
- Start broad and then narrow to appropriate antibiotics when get swabs and cultures back
- Questioning if patient actually needs antibiotics, thinking of resistance and side effects, e.g C.Diff
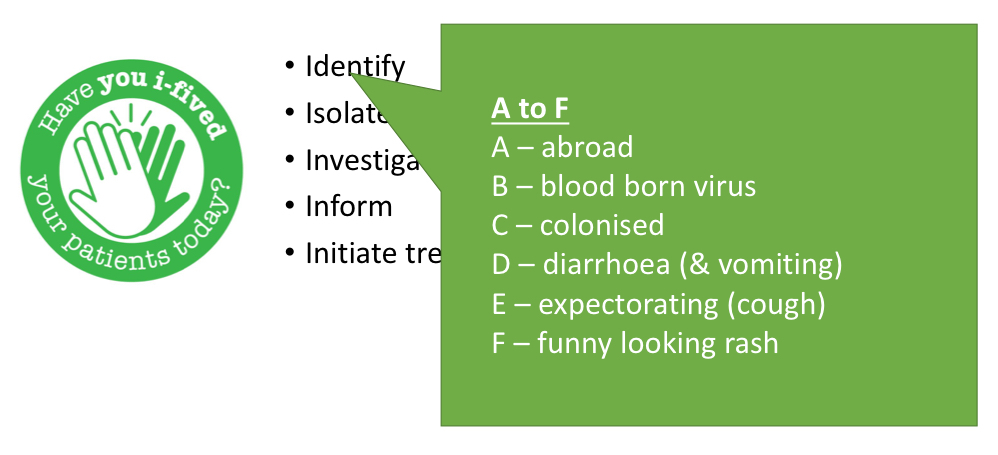
What is the A to F approach of identifying infection in the I5 model?
When can aciclovir be usedin the treatment of herpes simplex virus?
Same for genital, dose depends if immunocompromised or relapsing
Can also be used in varicella zoster and herepes zoster!
Slows the growth of the virus so speeds up the healing process by about half but doesn’t eradicate the virus!

What is the MOA of cephalexin, what are the DDIs and ADRs?
- Cephalosporin - Inhibits cell wall synthesis
- Used for prophylaxis of recurrent UTI, hospital acquired pneumonia, acute pyelonephritis
- DDIs: can increase blood metformin levels
- ADRs: diarrhoea, ab pain, headache, vomiting, thrush, eosinophillia
What is the MOA of azithromycin and clarithromycin, what are the DDIs and ADRs?
Macrolides: stop protein synthesis
Used for: resp infections, ear infections and skin/soft tissue infections in those that are allergic to penicillin
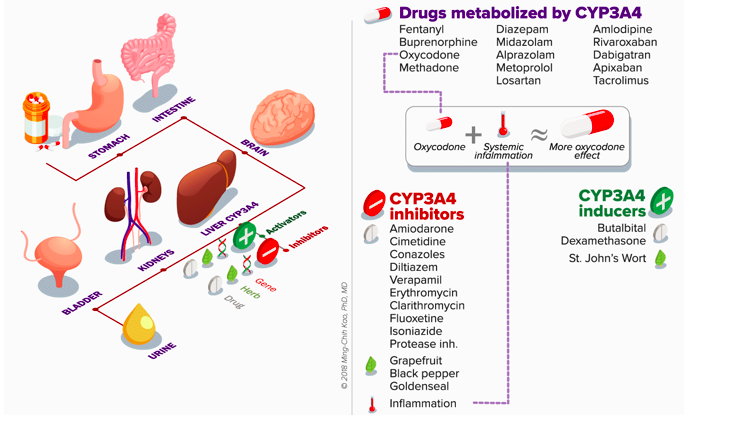
DDIs: Clarithromycin with CCBs can cause AKIs, clarithromycin is CYP3A4 inhibitor
ADRs: Hepatotoxicity, Nausea, Diarrhoea, QT prolongation so arrhythmias, anaphylaxis, Steven Johnson syndrome, C.Diff, can aggravate Myasthenia Gravis
What is the MOA of amoxicillin, flucloxacillin, co-amoxiclav and penicillin V, what are the DDIs and ADRs?
Penicillins so inhibit cell wall synthesis, co-amoxiclav being used for severe respiratory infections
ADRs: hepatotoxic so can cause jaundice, allergies diarrhoea, nausea, thrombocytopenia

What is the MOA of ciprofloxacin, what are the DDIs and ADRs?
Quinolone: inhibits DNA synthesis by inhibiting DNA gyrase
Used for eye and ear infections
ADRs: headache, N+V, rash
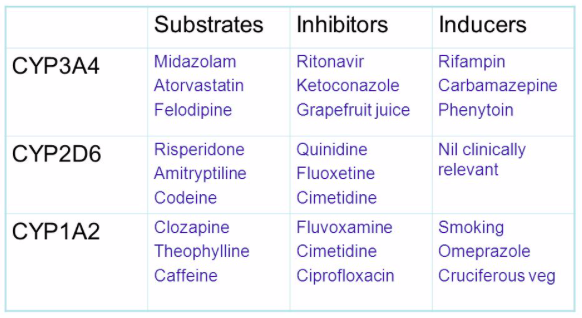
DDIs: Inhibits CYP1A2 and 3A4 so can interact with warfarin, theophylline and phenytoin and etc
What is the MOA of doxycycline, what are the DDIs and ADRs?
Tetracycline: Inhibits protein synthesis
Used for: H Pylori, Chlamydia, Acne
ADRs: photosensitivity, discolouring of teeth, angiooedema, pericarditis, thrush, rash, diarrhoea
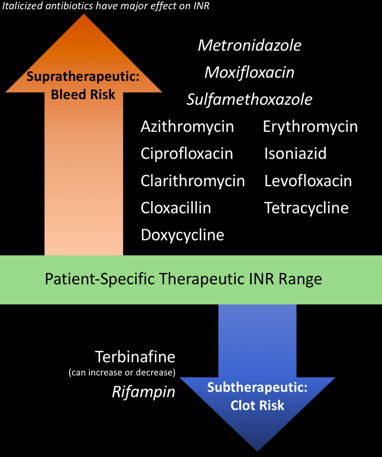
DDIs: Can worsen myasthenia gravis and SLE, inhibits CYP3A4 so bleeding risk with warfarin and other drugs metabolised by this
What is the MOA of trimethoprim, what are the DDIs and ADRs?
Binds to dihydrofolate reductase and inhibits the reduction of dihydrofolic acid (DHF) to tetrahydrofolic acid (THF)
Used for: UTIs and acne
ADRs: diarrhoea, electrolyte imbalance, headache, nausea, rash
DDIs: Don’t use with spironolactone as risk of hyperkalaemia, can inhibit CYP2C8 so can potentiate warfarin and phenytoin
What is the MOA of metronidazole, what are the DDIs and ADRs?
Inhibits DNA synthesis
Used for BV, PID and endocarditis
ADRs: metallic taste in mouth, loss of appetite, thrush, headache, vomiting
DDIs: don’t drink as will vomit, see image

What is the MOA of nitrofurantoin, what are the DDIs and ADRs?
Stop DNA synthesis, used for UTIs and prophylaxis of UTIs
ADRs: see image
DDIs: minimal but may decrease activity of quinolones, can use with warfarin, bad if renally impaired

What are the ADRs and DDIs with aciclovir?
ADRs: nausea, photosensitivity reactions, thrombocytopenia, rash
DDIs: may interact with other antibiotics like tobramycin and amphotericin B
Which heparin has a lower risk of osteoporosis?
LMWH


