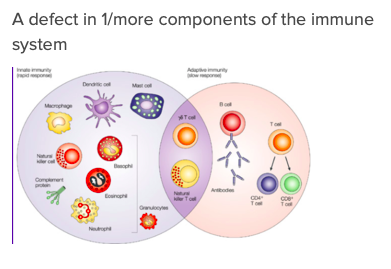
What is an immunocompromised host?
State in which the immune system is unable to respond appropriately and effectively to infectious microorganisms due to a defect in the immune system
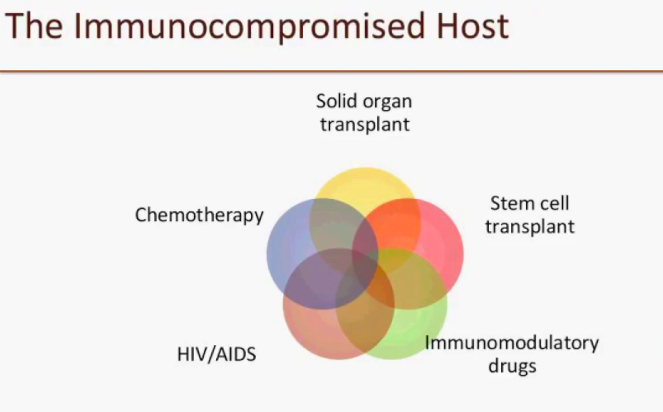
What causes an immunocompromised state?
What are the two types of immunocompromised state and what are the causes?
Secondary could be malnutrition, HIV, chemo, malignancy

In general when should you suspect an immunodeficiency?
Severe
Persistent
Unusual
Recurrrent

What are some warning signs of PID in adults?
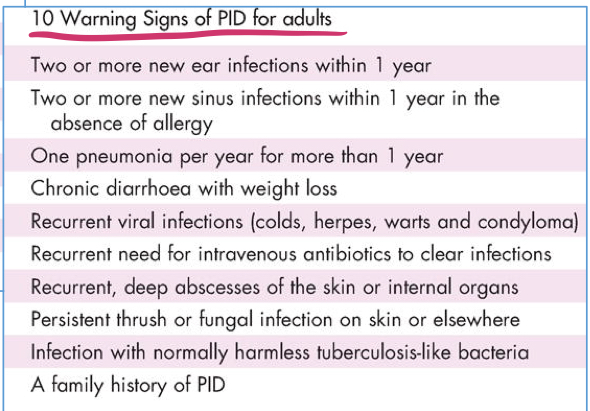

What are some warning signs of PID in children?
- 4 or more new ear infections in year
- 2 or more sinus infections or pneumonia in year
- 2 or more months on antibiotics with no effect
- 2 or more deepseated infections
- Family history of PID

What are the limitations of the warning signs for PID?

What are some primary immunodeficiency diseases of clinical importance?
- Bruton’s disease (X-linked agammaglobulinaemia): defect in B-cell development
- Common variable immunodeficiency (CVID): antibody production defect
- Severe combined immunodeficiency (SCID): combined T and B cell defect so no immunity
- Chronic granulomatous disease: defect in respiratory burst, NADPH oxidase
Identify some PID’s due to antibody defects, T cell defects and phagocytic defects.

What are the different ages of onset that can help you to distinguish what PID a patient has?

When diagnosing a PID, what are some of the factors that can help you narrow down what type it is?
- Age
- Site of infections
- Type of microorganisms and infections
- Family history (X-linked)
- Lab results
How do PIDs due to a complement deficiency present?
- Pyogenic infections (C3)
- Meningitis / sepsis / arthritis (C5-C9)
- Angioedema (C1 inhibitor)
- Often infected by neiserria, streptococci, HiB and other encapsulated bacteria, not viruses and fungi

How do PIDs due to a phagocytic defects present?
- Skin/mucous infections
- Deep seated infections (abscesses)
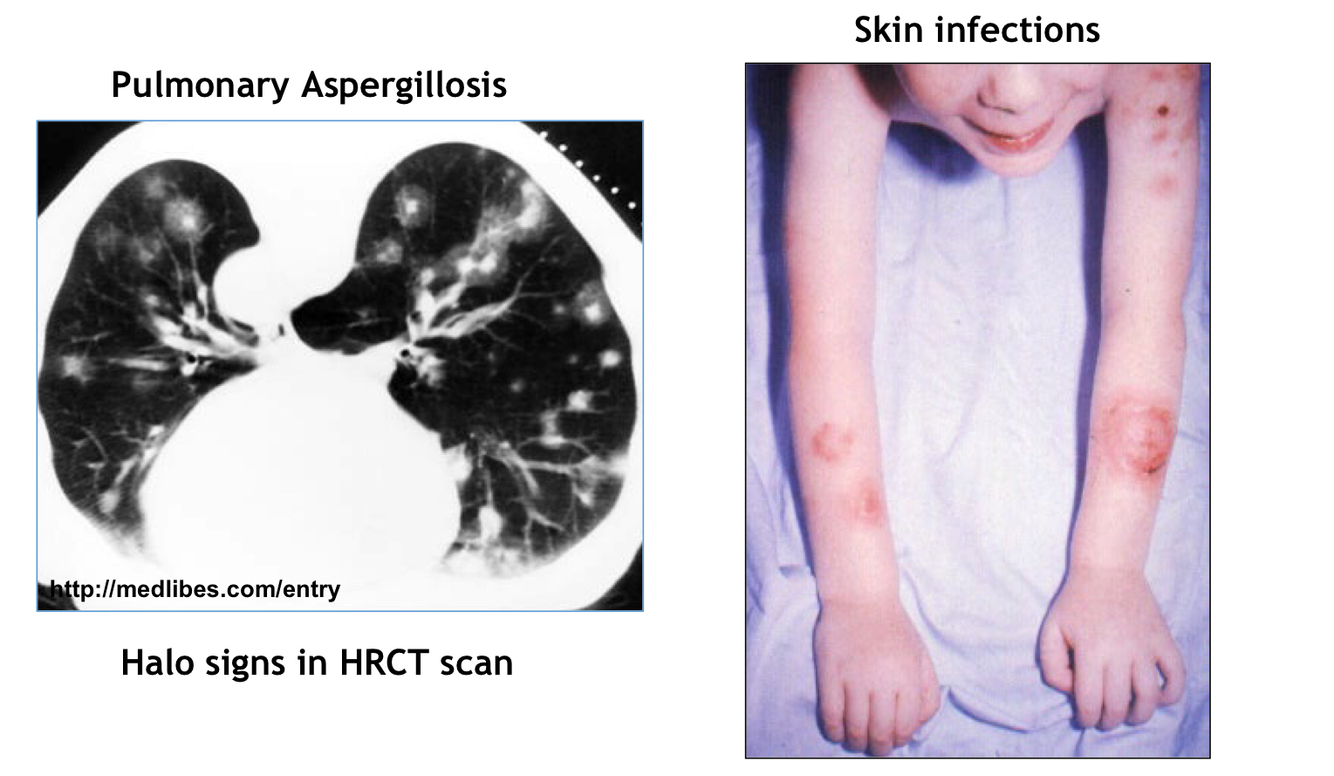
- Invasive fungal infection (aspergillosis)
Usually staph aureus, non TB mycohacteria, candida and aspergillus

How do PIDs due to an antibody deficiency present?
- Sinorespiratory infections
- Arthropathies
- GI infections
- Malignancies
Mainly strep, staph, HiB, enteroviruses and protozoa giardia lamblia

How do PIDs due to T cell defects present?
- Death if not treated
- Failure to thrive
- Deep skin and tissue abscesses
- Opportunistic infection
Similar organisms to antibody deficiency plus salmonella typhii, all viruses and all HIV infections like toxoplasma gondii, cryptococcus neoformans

What is Severe Combined Immunodeficiency, Bruton’s disease, CGD and Common Variable Immunodeficiency?
- SCID is a primary immunodeficiency characterised by a severe defect in both the T- & B-lymphocytes
- CVID is a primary immunodeficiency characterised by recurrent infections and low antibody levels (specifically IgG, IgM and IgA)
- Bruton’s disease is an inherited primary immunodeficiency caused by a severe block in B cell development and a reduced immunoglobulin production
- Chronic granulomatous disease is an X-linked inherited primary immunodeficiency wherein the body cannot phagocytose pathogens due to difficulty forming the superoxide radical (no respiratory burst)
- This increases susceptibility to infections by bacteria and fungi
What is the diagnosis for the following clinical case?
“A 6 month-old boy was born at term physically normal and apparently healthy. In last 3 months, he has had recurrent fungal (diaper rash, oral candidiasis), viral (upper respiratory tract infections), and bacterial (otitis media) infections, all of which resolved with appropriate pharmacologic intervention
He is below the 50% percentile for weight and has weak IgG response to vaccines. Both sexes of the family have been affected by these infections.”
Severe combined immunodeficiency

Bruton’s

CGD

Common Variable Immunodeficiency (might see Halo signs on CT with pulmonary aspergillosis and skin infections)
What is the supportive treatment for PIDs?

What is some specific treatment for PIDs?
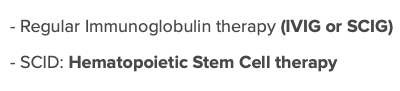
When managing PIDs, what comorbidities should you look out for and how would you prevent comorbities occurring?
- Autoimmunity and malignancies

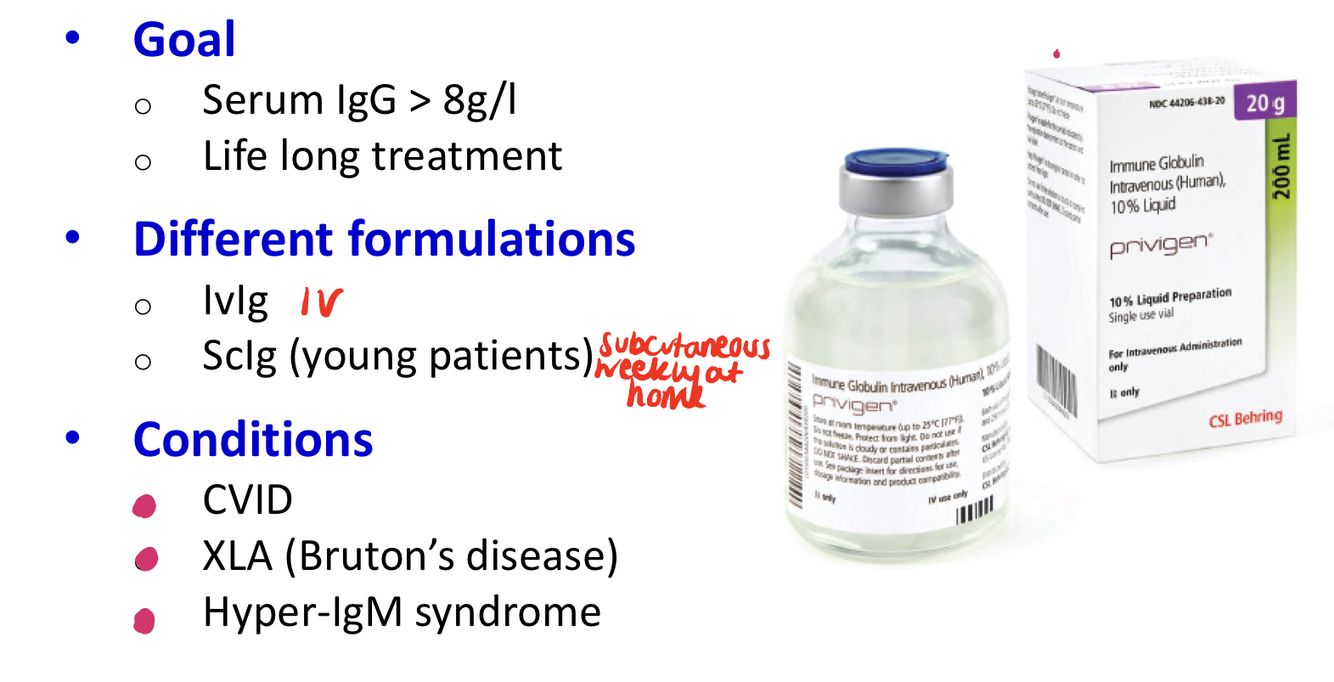
Which conditions is immunoglobulin replacement therapy used for, what is the formulation and what is the goal?