What are the vertebral ligaments?
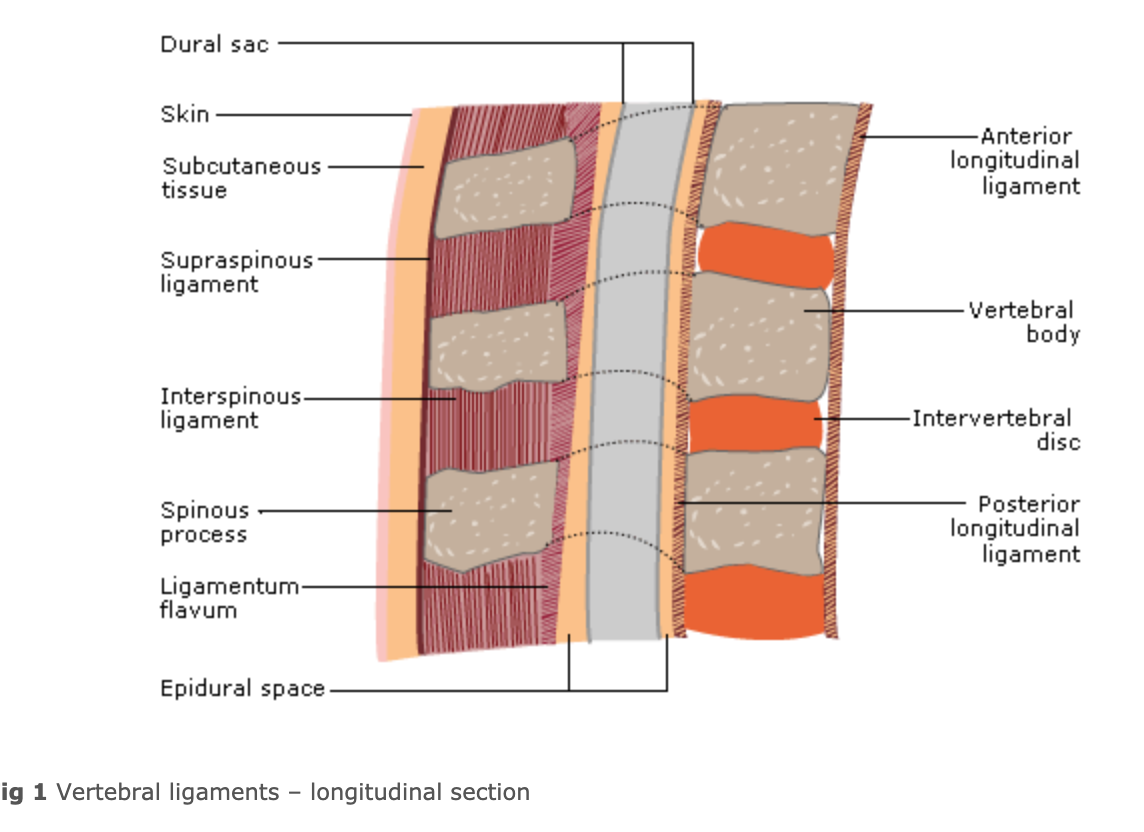
Anterior longitudinal ligament
- adheres to anterior surface of vertebral bodies and discs, runs from C2 to sacrum
Posterior longitudinal ligament
- extends along posterior aspect of the vertebral bodies and discs
Ligamentum flavum
- connects adjacent vertebral laminae
- thick elastic fibres are more developed in lumbar than thoracic regions
Interspinous ligaments
- connect adjacent spinous processes
Supraspinous ligaments
- a tough, fibrous ligament that attaches tips of spinous processes from C7 to sacrum
What are the meninges?
The three membranes surrounding the brain and spinal cord
- dura mater
- arachnoid mater
- pia mater
They’re separated from the periosteum by the epidural space
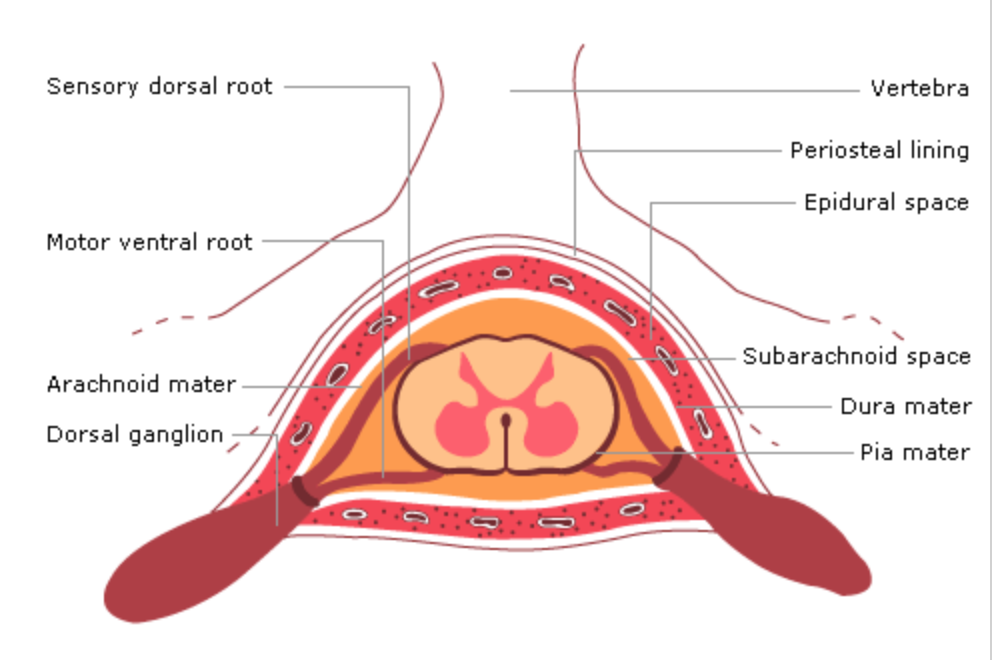
What does the epidural space contain?
- lymphatics
- spinal nerve roots
- loose fatty tissue
- small arteries
- network of large, thin walled blood vessels called the epidural venous plexus
What are the boundaries of epidural space?
Superior - foramen magnum
Inferior - sacrococcygeal membrane
Anterior - posterior longitudinal ligaments and the vertebral bodies
Posterior - ligamentum flavum and vertebral laminae
Lateral - pedicles and intervertebral foraminae
What is the subarachnoid space?
- spinal or intrathecal space
- space between the arachnoid mater, which lines the dural sheath and the pia mater
- contains CSF
What afferent fibres does the pain of labour and delivery affect?
Afferent fibres from T10 to L4.
For C-Section, what sections of the spinal cord needs to be blocked?
T10 to S5 is necessary
What are the characteristics of a Tuohy needle?
- 8cm shaft, 2.5cm hub
- 1cm markings
- 16 or 18G
- snap on wings
- curved blunt tip - Huber point, exit hole at 20° to shaft
- stylet introducer to prevent coring of tissues
What are the characteristics of the loss of resistance syringe?
- low resistance plunger
- plasic single use
- can be used with saline or air to detect LOR
- graduated barrel
What are the characteristics of an epidural catheter?
- narrower than the corresponding epidural needle
- 90cm long, transparent flexible tube
- biologically inert
- standardized markings
- single at tip
- 1cm from 5 - 14cm
- double marking at 10cm
- triple at 15cm
- quadruple 20cm
- distal end has multiple side holes with a closed smooth tip to minimize risk of dural or vascular puncture
- proximal end attaches to Luer lock and filter
What are the characteristics of the epidural filter?
- luer lock connections to epidural catheter and infusion set
- 0.22 micrometre hydrophilic two-way filter for bacteria/viruses/glass
- transparent
What are the characteristics of a spinal needle?
- used for intrathecal injection of drugs and sampling CSF
- transparent hub for early identification of CSF
- 18-32 Gauge available, 25G most common
- 9 or 10cm length is most common
- cutting bevel (Yale/quincke) or blunt (whitacre/sprotte)
- stylet to prevent coring and strengthen shaft
- Introducer for 25G and finer needles
What local anaesthetics are licensed from obstetric epidural and spinal use?
Bupivacaine, levobupivacaine, ropivacaine and lidocaine are all licensed for obstetric epidural use, whilst hyperbaric bupivacaine is the only local anaesthetic licensed for obstetric spinal use.
How do local anaesthetics work?
Bind to voltage-gated sodium channels in the nerve cell membranes slowing depolarization and inhibiting conduction in nerve fibres transmitting painful stimuli to the spinal cord.
How does increasing lipid solubility affect potency of local anaesthetics?
Increasing lipid solubility allows more rapid penetration of nerve cell membrane and therefore greater potency
What is the duration of action of local anaesthetic dependent on?
To the degree of protein binding.
Bupivacaine, levobupivacaine and ropivacaine are approximately 95% protein-bound and therefore have a longer duration of action than lidocaine, which is approximately 65% protein-bound.
What is the speed of onset of local anaesthetic dependent on?
The degree of ionization, which is dependent on the pKa of the drug (it’s the non-ionized form of the local anaesthetic which diffuses across the nerve sheath)
Bupivacaine, levobupivacaine and ropivacaine have a pKa of 8.2. They are therefore more ionized and have a slower onset of action at body pH than lidocaine, which has a pKa of 7.7.
Why are opioids used in epidural/spinal anaesthesia?
- they enhance quality of analgesia
- reduce mass of local anaesthetic required
- reduce motor block produced in epidurals
- enhance surgical anaesthesia
- postop analgesia
What is the action of opioids in epidurals?
Bind to opioid receptors in the substantia gelatinosa of the spinal cord. They have to penetrate the dura first.
Speed of penetration increases with lipid solubility +


