Describe the spirometry and symptology required for diagnosis of COPD.
Spirometry: FEV1 <80% and FEV1/FVC <70% post bronchodilator - confirm presence of persistent airflow limitation Symptoms: SOB, cough, increased sputum production
What are the 8 key aspects of COPD management?
- Vaccination 2. Smoking cessation 3. Nutrition 4. Managing comorbidities 5. Pharmacotherapy 6. Pulmonary rehab 7. Action plan 8. Self management
Risk factors for COPD.
*** SMOKING *** - relationship exists between amount of tobacco smoked and rate of decline in FEV1 Other risk factors: parental smoking, genetic factors, asthma, SES status, nutritional and environmental factors
Pitfalls of spirometry
May under diagnose younger patients and over diagnosed elderly patients
Is it COPD or Asthma?
- asthma is diagnosed by increased FEV1 > 12% and by > 200ml post bronchodilator - if FEV1 improves by > 400ml this would suggest underlying asthma or co-existing asthma and COPD
Which other investigations would you order to r.o other pathologies which are not COPD?
- CXR - haematology/biochemistry - complex lung function tests - EST - ECG - TTE
How is severity of COPD confirmed?
MILD - FEV1 60-80% predicted - few symptoms, SOB with moderate exertion - little or now effect on daily activities MODERATE - FEV1 40-59% predicted - SOB when walking on level ground - increasing limitation of ADLs - recurrent chest infections - exacerbations requiring steroids/antibiotics SEVERE - FEV1 <40% - SOB on minimal exertion - severely limited ADLs - increasing frequency and severity of exacerbations
What are the 5 most prevalent comorbidities in patients with COPD?
- HTN 2. Hyperglycaemia 3. Atherosclerosis 4. Dyslipidaemia 5. Osteoporosis
What does COPD- X stand for?
Case finding/confirm diagnosis Optimise function Prevent deterioration Develop plan of care Manage eXacerbations
What are the physical activity recommendations for patients with COPD?
- aim to walk for at least 150min/week (30min/day x 5 a week) - instruction patients to walk until the feel too breathless to continue, have a rest and then resume walking
Describe the non-pharmacological strategies recommended to optimise COPD.
- smoking cessation - pulmonary rehab, all symptomatic patients should be referred - regular physical activity - self management and support groups
What are the 2 main aims of pharmacological treatment in COPD?
- treat symptoms 2. reduce risk fo severe exacerbations and deterioration
What is the evidence behind the current COPD pharmacological agents?
- SABA/SAMA –> provide short term relief of SOB 2. LAMA/LABA –> may improve lung function, symptoms, quality of life and exacerbation frequency 3. ICS/LABA –> may reduce exacerbation frequency and improve QOL ** Triple therapy results in reduced rate of moderate of severe COPD exacerbations, better lung function and quality of life in comparison to dual therapy.
Does LABA/LAMA combination work better than single LAMA or LABA inhalers?
Yes! Used in combination results are better than monotherapy.
What things would trigger you to consider altering pharmacotherapy in COPD?
- exertional dyspnoea - functional status - history of exacerbations - patient preference
When should you re-assess alteration of pharmacotherapy in COPD?
6 weeks would be reasonable
What is the risk of ICS?
Increased risk of pneumonia
What are some non-pharmacological options for symptomatic management?
- handheld fans - use of breathlessness recovery positions r.e. forward lean
When should you consider adding LAMA/LABA?
In patients who are on SABA who have persistent dysnpea you should consider adding LABA or LAMA or both LAMA/LABA.
When would you consider LAMA/LABA dual therapy?
In patients with a SABA and a either mono LABA or LAMA who have ongoing symptoms of breathlessness.
What is triple therapy and when is it indicated?
- triple therapy = ICS/LAMA/LABA - indicated for patients with repeat exacerbations and more severe COPD symptoms that are not managed on dual LABA/LAMA therapy
Describe the stepwise management of stable COPD.
- Confirm diagnosis and severity 2. Optimise with non-pharmacological interventions 3. Optimise with pharmacological interventions > start with SABA or SAMA for symptom relief > consider adding LABA or LAMA if ongoing sx > from here could consider LABA/LAMA combination > if still symptomatic consider adding ICS ** should always assess adherence and technique prior to changing pharmacotherapy **
When to consider referral to respiratory physician?
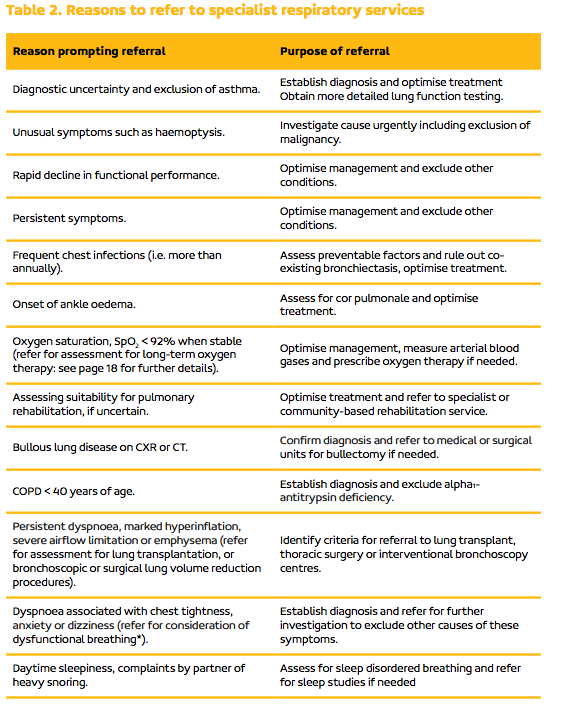
At what saturations would you consider referral for home O2?
Stable COPD with SpO2 <92%



