Describe the general GI anatomy, function, and innervation
- 5% of total human body mass
- main functions: motility, digestion, absorption, excretion, and circulation
- GI tract innervation: Autonomic nervous system (extrinsic NS) and Enteric NS
- extrinsice includes SNS and PSNS
Describe the SNS innervation in the gastrointestinal system.
- Function: primarily inhibitory
- stimulation decrease or cease GI motility.
- Location: Preganglionic fibers (originate at T5-L2 segments of SC) → travel to sympathetic chain of ganglia → synapse with postganglionic neurons → travel to gut → then terminate at enteric nervous system.
- Sympathetic signal transmission:
- Norepinephrine (Primary neurotx)
- Vasoactive intestinal polypeptide (VIP)
- Sympathetic signal transmission:
Describe the PSNS innervation to the gastrointestinal system.
- Function: primarily excitatory
- activates GI motility/function
- Location: Parasympathetic preganglionic fibers originate in medulla and sacral region of SC.
- Innervation:
- Vagus nerve fibers: esophagus, stomach, pancreas, SI, and 1st half of LI.
- Pelvic nerve fibers: 2nd half of LI, sigmoid, rectal, and anal regions.
- Signal transmission:
- Acetylcholine (ACh)
Describe the esophagus and its sphincters.
- Muscular tube
- 18-25 cm long
- extends C6 to T11
- Composition:
- Upper 1/3rd: striated muscle
- Lower 2/3rd: smooth muscle
- Two areas of high pressure:
- Upper esophageal sphincter (UES)
- Location: Level of cricoid cartilage
- Resting tone: 30-200 mmHg
- opening and closing coordinated with pharyngeal pushing of food
- Lower esophageal sphincter (LES).
- Formation:
- Intrinsically- circular esophageal muscle
- Extrinsically- diaphragm muscle
- Innervation: both SNS & PSNS.
- Resting tone: 10–45 mmHg
- Formation:
- Upper esophageal sphincter (UES)
What is the basic pathophysiology behind reflux and some esophageal or gastric disorders that cause it?
Patho:
- Luminal pressures increase to overcome resting pressures of UES and LES
Esophageal etiologies:
- Achalasia
- smooth muscles unable to relax/move food down
- increased LES tone does not allow for complete relaxation
- RESULT: dysphagia, regurgitation, and significant pain.
- diffuse esophageal spasm
- muscle contractions are uncoordinated and, as a result, food does not properly move downward.
- hypertensive LES
- LES with a mean pressure of > 45 mm Hg → leading to dysphagia and chest pain.
- Neurologic disorders
- Ex: stroke, vagotomy, or hormone deficiencies
- Patho: alter nerve pathways such that appropriate sensing and feedback are disrupted.
- RESULT: dysphagia.
Slow emptying (Gastric motility disorders) → increased incidence of GE reflux dx
- Drug induced: (often given intraop or to critically ill pts for BP control)
- Opioids
- Vasoactive agents
- Ex: increase catecholamine [] → sympathetic stimulation → decreased motility.
- Neurologic:
- vagal neuropathies
- gastroparesis
- Critical illness
- Conditions commonly present in severely compromised pts: Examples → decrease gastric motility
- Hyperglycemia
- increased ICP
- mechanical ventilation
- Conditions commonly present in severely compromised pts: Examples → decrease gastric motility
What are some drugs that can increase gastric motility?
:
- Increase Gastric Motility:
- Erythromycin
- Metoclopramide
What is succinylcholines effect on intragastric pressure?
- fasciculations increase intragastric pressure
- may overcome tone of the LES and allow reflux (could increase risk of aspiration*)
What are the 4 regions of the stomach and what are the 4 main cell types?
What promotes stomach emptying?
- Stomach: four regions: cardia, fundus, body, and antrum
- 4 main cell types
- mucous cells: protection from HCl acid
- parietal cells: secrete HCl acid
- chief cells: secrete pepsin
- G cells: secrete gastrin
- 4 main cell types
- Promotion of stomach emptying:
- Gastric distention
- Gastrin
- Nitric Oxide (NO)
- Stomach physiology:
- Solid foods must be broken down into 1-2mm particles before entering duodenum
- Takes 3-4 hrs to empty from stomach
- Leads to duodenum
- Solid foods must be broken down into 1-2mm particles before entering duodenum
Describe the sections of hte small bowel?
- Duodenum:
- 1st and smallest section of SI
- pancreas, liver, and gallbladder secrete digestive enzymes through the ampulla of Vater into mid-duodenum
- Jejunum:
- Primary absorption of nutrients
- Ileum:
- final section of SI
- ends at ileocecal valve
- Function:
- B12 absorption
What are some common etiologies for small bowel dysmotility?
Mechanical obstruction
- Etiologies: Hernias, malignancy, adhesions, and volvuluses
Other reversible causes:
- Ileus: D/t →
- manipulation of intestines << main reason
- Surgical stress response d/t postop pain
- Multifaceted, neurohormonal resp to sx stim
- SIRs - release of systemic inflammatory response and adrenaline and noradrenaline hormone
- → sympathetic overactivity will constrain mobility and directly inhibit gut smooth muscle via activation of α- and β-adrenergic receptors → resulting in postop ileus
- Suppression of response → LA and opioid epidural admin
- Multifaceted, neurohormonal resp to sx stim
- Electrolyte abnormalities
- Critical illness
Nonreversible structural causes:
- Ex: scleroderma
- connective tissue disorders
- short bowel syndrome
Neuropathic causes
What are the sections of the large intestine?
- Composed of cecum, appendix, ascending colon, transverse colon, descending colon, sigmoid colon, and rectum
- Function:
- absorbs water, nutrients, and vitamins
What are the effects of general anesthesia on bowel function? goals and considerations?
- Overall goals → enhance bowel function:
- attenuate stress response
- hemodynamic stability
- ideal fluid balance
- → Fluid loss r/t exposure of gut!
- normothermia (keep warm)
- Considerations:
- No evidence for recommendations on specific anesthetic and analgesic agents to avoid adverse GI effects
- Anxiety inhibits GI function
- GI tract inhibition directly proportional to amount of NE secreted from sympathetic stimulation
- Tx: REDUCE stress response!
- GI tract inhibition directly proportional to amount of NE secreted from sympathetic stimulation
- Volatile anesthetics affect bowel function through various mechanisms
- changes in intestinal tissue oxygenation
- depress the spontaneous, electrical, contractile, and propulsive activity in the stomach, small intestine, and colon
- Colon recovers 30-40 hrs postop
What are the effects of nitrous, muscle relaxant, and anticholinesterase reversal on bowel function?
- TIVA vs volatile doesn’t seem to make a significant difference
- Nitrous: 30x more soluble than nitrogen but no adverse outcomes on motility
- Cause gut to expand → visualization difficult for surgeons
- Muscle relaxant: skeletal muscle affected
- GI motility unaffected
- Anticholinesterase reversal:
- increase parasympathetic activity
- increases bowel peristalsis
- → lead to fresh anastomosis dehiscence (falls apart when sew together)
- **Sugammadex preferred with fragile anastomosis (instead of neostigmine)
How do opioids affect bowel function?
- Reduced GI motility
- Action on central and peripheral receptors: mu, delta, and kappa
- Peripheral receptors cause adverse effects
- High density of peripheral mu-opioid receptors in the myenteric and submucosal plexuses
- Other adverse effects:
- Nausea
- Anorexia
- delayed digestion
- abdominal pain
- excessive straining during bowel movements
- Incomplete evacuation.
- Methylnaltrexone: pure peripherally acting opioid (Mu) receptor antagonists are a potential solution
- Methylnaltrexone: peripheral mu-opioid receptor antagonist and does not cross the blood-brain barrier
Effect of surgery on bowel function?
- Abdominal surgery predisposes patients to ileus
- Uncomplicated ileus usually lasts 3-4 days
- Ileus → complications:
- Perforation
- Bleeding
- peritonitis
- MAIN REASON FOR ILEUS → Manipulation of intestines
- Additional contributors include: immobility, electrolyte imbalance from fluid shifts and insensible losses, and intestinal wall swelling from excessive fluid administration.
- Mesenteric ischemia: 100% mortality if untreated
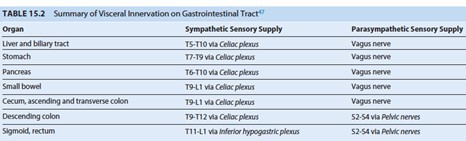
Give a summary of the visceral innervation of the GI tract.
- Celiac plexus: innervation of the GI organs up to the proximal transverse colon
- Inferior hypogastric plexus: innervation of the descending colon and distal GI tract
- Know chart:
What are some regional anesthetic techniques that will cover abdominal visceral pain?
- Spinal anesthesia
* extending to at least T5
- Spinal anesthesia
- Epidural anesthesia
* covering T5 to Tl2 dermatomes
- Epidural anesthesia
- Paravertebral blocks
* Cover/comprising T5 to L2 spinal segments
- Paravertebral blocks
- Selective T5 to L2 sympathetic chain block
- Celiac/splanchnic nerve block
* Done under Fluoro/radiology guidance → risk of aortic injury**- Other risks: Chart
* Indications: intractable pain (ex: severe biliary or pancreatic CA) - Block w/ ETOH- temporary relief
- Comes with risks!
* Splanchnic/celiac plexus blocks have been used for biliary and pancreatic cancers/ intractable pain.
* Celiac plexus block usu done under fluoro or other radilological guidance or direct surgical visualization- risk of aortic injury, etc. (see chart)
- Other risks: Chart
- Celiac/splanchnic nerve block
What are some risks for celiac/splanchnic nerve block?
- hypotension
- diarrhea
- intravascular injection/vascular trauma
- subarachnoid or epidural injection and paraplegia
- renal injury
- pneumothorax
- chylothorax
- damage to surrounding structures and retroperitoneal hematoma
- peritonitis and abscess
What are some effects of regional anesthesia technique on bowel function?
- Epidural analgesia → decrease incidence of postoperative ileus
- Leads to blockade of afferent and efferent sympathetic-mediated GI reflexes, BUT
- → parasympathetic innervation left intact
- Leads to blockade of afferent and efferent sympathetic-mediated GI reflexes, BUT
- Neuraxial blockade → Improvement of GI blood flow and tissue oxygenation
- Avoid hypotension associated with neuraxial as this will negate the benefits (when goal is to increase bowel fx)
What are some considerations in ERAS for GI procedures?
- Regional anesthesia
- Avoidance of opioids
- Multimodal analgesia
- Nutrition and preoperative carbohydrates
- Selective bowel preparation
* AE of bowel prep:- decreased exercise capacity, lower weight, increased plasma osmolality, decreased urea and phosphate, and reduced plasma Ca & K
- These effects + fasting → produce unpleasant pt experience.
- The routine use of bowel preparation has been questioned repeatedly. In fact, recent studies have shown mechanical bowel preparation can be safely omitted before elective colorectal surgery
- Selective bowel preparation
- Fluid optimization
- Temperature control
- Early removal of drains and tubes
- Early mobilization
- Early oral intake
Describe considerations and goals in fluid management for bowel surgery.
- All patients are exposed to a preoperative starvation period that results in a fluid deficit:
- Consequences of fasting:
- Stimulate prod of ADH, atrial natriuretic peptide, renin-angiotensin-aldosterone system, and increase in sympathetic activity
- Relative hypovolemia
- More pronounced in patients who receive bowel preparation, experience diarrhea/vomiting, high temp exposure, high NGT output
- Consequences of fasting:
- Excessive/ liberal fluid administration=
- increased capillary hydrostatic pressure
- tissue and bowel edema
- anastomotic leaks
- Goals:
- Optimizing fluid administration
- → increase tissue perfusion and oxygen delivery
- Modulation of hormonal and inflammatory response
- Ex: mitigate stim of ADH, ANP, RAAS, and increase symp activity
- Optimizing fluid administration
What are some preoperative considerations in patients with GI disease?
- intravascular fluid volume
- fluid status (renal fx)
- electrolyte []
- nutrition status (albumin levels , BMI, plasma osmolarity)
- Pre-existing conditions: examples
- GERD
- bowel obstruction
- vomiting
- hypersecretion of acid
- Clotting abnormalities
- Malabsorption of fat-soluble vit K (often malabsorbed) is necessary for the synthesis of CF II, VII, IX, and X in liver
- Gastric lesions/resections often have iron deficiency anemia with megaloblastic vitamin B12 anemia (lack intrinsic factor or overgrowth B12 consuming bacteria in blind loop)
- Check H&H for baseline anemia/active lesions
Describe some population where you may be concerned for aspiration.
What are some measures you would take to decrease the risk for aspiration in these populations?
- Especially important in high risk populations: → FULL STOMACH
- Pregnancy
- DM
- bowel obstruction
- peritonitis
- cirrhosis
- Follow NPO times:
- ASA recommends fasting 4 hours for breast milk, 6 hours for non-human milk/formula, 6 hours for a light solid meal
- Increase gastric emptying-
- Ex: prokinetics (metoclopramide)
- Reduce gastric volume and acidity
- Volume: Decompression w/ NG tube
- Not guarantee gastric empty
- Impair fx of LES and UES
- Does NOT diminish effect of cricoid pressure
- Acidity:
- Nonparticulate acid (Na Citrate)- 15-30 ml
- 1 hr preop
- Increases gastric pH > 2.5. when combo w/ 10 mg metoclopramide → reduces contents < 25 mls
- 1 hr preop
- H-2 receptor antagonists
- Famotidine → reduces gastric volume and increases gastric pH better than rantidine given a few hours before surgery.
- proton pump inhibitors –
- AM of sx: rapbeprazole and lansoprazole
- PM before sx: omeprazole
- Nonparticulate acid (Na Citrate)- 15-30 ml
- Volume: Decompression w/ NG tube
- AW techniques:
- Cricoid Pressure- not really proven
- Contraindications:
- cricotracheal injury
- active vomiting
- unstable c-spine.
- Complications:
- esophageal rupture
- cricoid ring fracture
- impede ventilation/visualization w/ DL
- Cuffed ETT
- Proseal LMA- gastric port for decompression
- Avoiding airway instrumentation with inadequate levels of anesthesia
- Ex: avoid wrenching
- Avoidance of Aspiration Techniques:
- RSI w/ cricoid
- Awake ETT intubation
- NG sx Preop
- Histamine receptor blockers preop
What are some factors that reduce LES tone?
- Drugs:
- Anesthetics:
- VA
- TPL
- Propofol
- Opioids
- Anticholinergics
- B-agonists
- TCAs- tricyclics
- Glucagon
- Anesthetics:
- Cricoid Pressure
- Obesity
- Hiatal hernia
- Pregnancy


