Define primary hyperparathyroidism.
Autonomous overproduction of PTH causes derangement of calcium metabolism. In 80% this is due to a single parathyroid adenoma
Define secondary hyperparathyroidism.
Any disorder that results in hypocalcaemia will elevate PTH and can cause this. The most frequent causes: CKD, malabsorption, and inadequate sunlight, acting via alterations in vitamin D, phosphorus, and calcium.
What is the function of parathyroid hormone? (3)
Secreted in response to low ionized Ca2+ levels, by four parathyroid glands situated posterior to the thyroid. The glands are controlled by −ve feedback via Ca2+ levels.
PTH acts by:
- Bone:
- ↑osteoclast activity releasing Ca2+ and PO43− from bones
- Kidney:
- ↑Ca2+ and ↓PO43− reabsorption in the kidney
- active 1,25dihydroxy-vitamin D3 production is ↑. Overall effect is ↑Ca2+ and ↓PO4.
Describe how the parathyroid gland regulates calcium.
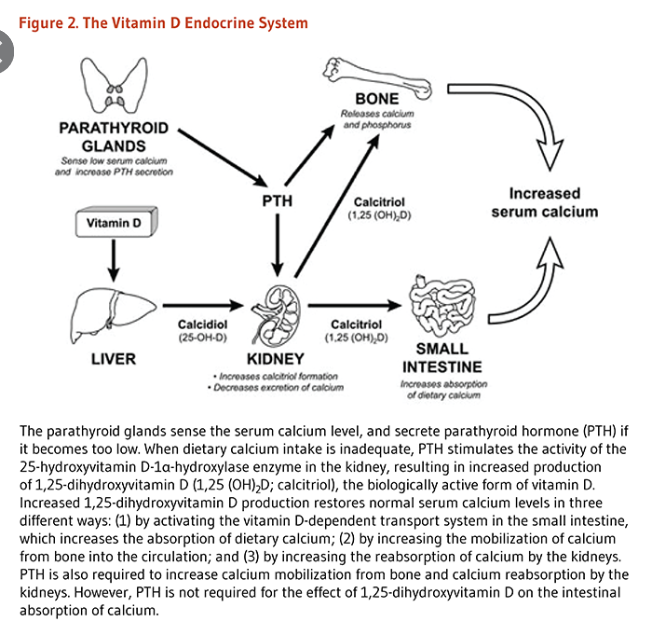
What are the biochemical features of primary hyperparathyroidism?
- Raised (unsuppressed) PTH
- Raised or inappropriately normal Ca
- Low phosphate
What is the difference between causes of primary and secondary hyperparathyroidism?
PRIMARY = no negative feedback, autonomous PTH release despite hypercalcaemia usually due to adenoma
SECONDARY = vitamin D deficiency so low calcium but high PTH from parathyroid hyperplasia which tries to normalise the serum calcium
What is the aetiology of primary hyperparathyroidism?
Caused by:
- parathyroid adenomas - 85%
- inherited hyperfunctioning parathyroid gland - 10-20% (check for multi gland disease e.g. in MEN1/2/4)
- parathyroid malignancy - 1%
- external neck irradiation e.g. lithium therapy used for bipolar disorder may over-stimulate the parathyroid glands
What are the three ways in which calcium is increased in primary hyperparathyroidism?
PTH secretion is not suppressed by high calcium levels –>
- over-stimulation of bone resorption with cortical bone affected more than cancellous bone
- reabsorption of calcium from the kidneys
- conversion of 25-hydroxyvitamin D3 to its more active form of 1,25-hydroxyvitamin D3 (which is responsible for GI absorption of calcium)
What are the signs and symptoms of primary hyperparathyroidism?
HYPERCALCAEMIA
“Stones, bones, abdominal moans, psychic groans” - REDUCED NEURONAL EXCITABILITY (atonal muscles)
- Stones – renal effects (you excrete Ca in kidneys)
- Polyuria & thirst, nephrocalcinosis (calcium oxalate), renal colic, chronic renal failure
- Bones
- Bone pain, osteoporosis/osteopenia, muscle weakness and high fatigability, paraesthesia, muscle cramps
- Abdominal moans - GI effects
- Anorexia, nausea, dyspepsia, constipation, pancreatitis
- Psychic groans - CNS effects
- Fatigue, depression, impaired concentration, memory loss, coma (usually >3mmol/L), poor sleep, anxiety
Hard, dense neck mass in parathyroid carcinoma.
What investigations would you do for primary hyperparathyroidism?
- Serum calcium - high (normal is 2.2-2.6mmol/L)
- Serum PTH - high
- 25-hydroxyvitamin D
- Serum phosphorus - low
- 24hr urinary calcium - high or normal
- DXA scan with TBS- T scan of -1 to 1 is normal, >-2.5=osteopenia, <-2.5 = osteoporosis. TBS evaluates bone microstructure.
What is the treatment of primary hyperparathyroidism?
- Parathyroidectomy
- Vitamin D supplementation - ergocalciferol
- Monitor serum calcium, creatinine and bone density
- Bisphosphonate - if osteoporosis is present
- Cinacalcet - lowers serum calcium and PTH; modulates activity of calcium sensing receptor which regulates PTH secretion.
What are the complications of parathyroidism and its treatment?
- Neck haematoma after surgery
- Recurrent/superior laryngeal nerve injury
- Hypocalcaemia after surgery - **
- Pneumothorax after surgery
- Osteoporosis
- Bone fractures
- Nephrolithiasis
What is the aetiology of secondary hyperparathyroidism?
3 MAIN AETIOLOGIES:
- CKD - loss of 1 alpha hydroxylase in the kidney (so no vit D conversion to active form) causing hyperphosphataemia and hypocalcaemia
- malabsorption syndromes - fat malabsorption causes reduced absorption of Vit D and dietary calcium
- chronic inadequate exposure to sunlight - sun helps synthesise 90-95% of required vitamin D
Other causes:
- Diminished dietary Ca, Vit D intake
- Malabsorption syndromes: lactose intolerance, pancreatic disease, Crohn’s disease, Coeliac disease, gastric bypass, Whipple’s disease
- Increased requirement of calcium or increased loss - bone growth, after pregnancy/breastfeeding, bisphosphonate treatment, loop diuretics, rhabdomyolysis, sepsis
- Diminished parathormone effect - CKD, pseudohypoparathyroidism (G-protein deficiency)
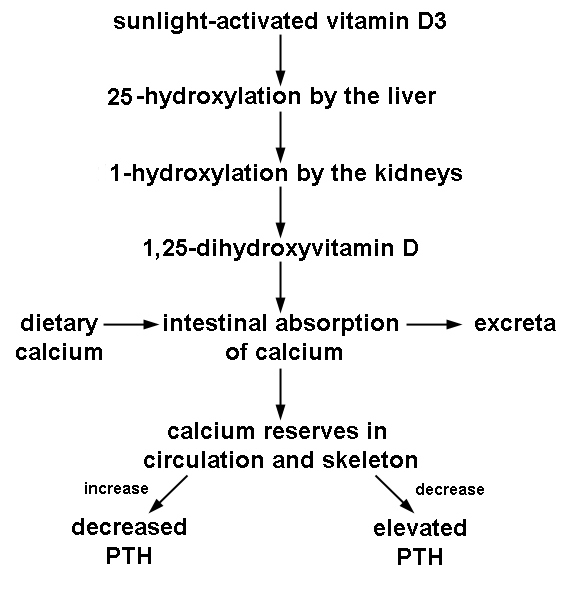
List 5 causes of vitamin D deficiency that could lead to Ca deficiency and therefore secondary hyperparathyroidism.
- Diet or GI malabsorption of dietary D2 eg coeliac disease, inflam bowel disease,
- Lack of sunlight (so lack of UVB)
- Renal failure (so no conversion to active form)
- Liver failure (no D3 synthesis)
- Vitamin D receptor defects (autosomal recessive, rare, resistant to vitamin D treatment)
What are the signs and symptoms of secondary hyperparathyroidism?
Signs and symptoms of hypocalcaemia:
- Pseudofractures
- These show neuromuscular irritability due to hypocalcaemia (enables greater Na+ influx, so MORE membrane excitability)
- Chvostek’s Sign – tap facial nerve below zygomatic arch -> twitching of facial muscles = (positive sign)
- Trousseau’s sign – inflate BT cuff for several minutes ->carpopedal spasm (positive sign). This is inducing tetany (clawing of the hand).
- Muscle cramps
- Bone pain on pressing - poorly mineralised osteoid becomes hydrated and cannot provide sufficient support for sensory fibres in the periosteum
- Paraesthesia/tingling
- Rickets - bowed legs/knock-knees
- Fractures
OR features of underlying malabsorption syndromes/ chronic renal failure
What investigations would you do for secondary parathyroidism?
- Serum calcium - <2.10mmol/L
- Serum iPTH (intact) - >88nanograms/L
- Serum creatinine - high in CKD (>91.5micromol/L)
- Serum urea nitrogen - high in CKD
- Serum phosphorus - high in CKD
- Serum 25-hydroxyvitamin D - may be low
- Serum magnesium - may be low
- US neck - parathyroid gland hyperplasia
How do you manage secondary hyperparathyroidism?
- UV radiation exposure - 5 to 15 minutes/day between 10 a.m. and 3 p.m., on arms and legs or hands, face, and arms, during spring, summer, and autumn provides the body with its required 1000 international units of colecalciferol
- Vitamin D supplementation - ergocalciferol
- Calcium supplementation - Ca carbonate
In CKD stage 5 with PTH >800ng/K - parathyroidectomy
What are the complications of secondary hyperparathyroidism?
- Osteodystrophy - loss of Ca and Vit D causes demineralisation of the skeleton
- Osteoporosis - loss of bone mass due to dysregulation between bone formation and resorption
- Uraemia
- Calciphylaxis - vascular and tissue manifestation of chronic hypercalcaemia; systemic calcification of the tunica media of small vessels
Prognosis - mirrors underlying disease.
What is activated vitamin D called?
Calcitriol 1,25hydroxyvitamin D
Where is 25 hydroxylase found?
Liver
What is the diagnostic test for osteoporosis?
DEXA - very safe as much less radiation than XR
What is the range for normal calcium levels in plasma?
2.2 - 2.6mmol/L
What is a genetic cause of hypercalcaemia?
Familial hypocalcuric hypercalcaemia
Who is more affected by primary hyperparathyroidism?
Females


