The following is the general “criteria” for what?
- Fever >38.3degC (100.9F)
- At least 3wks duration
- No dx after 3 outpt visits or 3 days of hospitalization
Fever of unknown origin
What are the 3 MC etiologies of Fever of Unknown Origin (FUO)?
- Infection
- Malignancy
- Connective Tissue Disease
What is the #1 MC malignancy to cause FUO (fever of unknown origin)?
Lymphoma, especially non-hodgkins
What is the main site of colonization of staphylococcal infections?
Nose
Is staph aureus coagulase negative or positive
positive
(Staph epidermidis and staph saprophyticus are both coag neg)
- Which staphylococcal strain is a frequent skin contaminant of blood cultures?
- What do you do to confirm whether a contaminant or a true cause of bacteremia?
- Staph epidermidis
- May have to draw from 2 sites
Which bacteria causes infections of:
- Urine catheters
- IV lines
- Prosthetic joints/heart valves
- Dialysis catheters
Staph epidermidis
Which staphylococcal strain is coagulase negative and is a leading cause of UTIs?
Staphylococcus saprophyticus
What is the etiology of TSS?
Staph aureus
Clinical presentation of what?
- Abrupt onset high fever
- Vomiting & watery diarrhea
- Sore throat, myalgias, h/a
- Hypotension with kidney and heart failure
- Diffuse macular erythematous rash and nonpurulent conjunctivitis
- Desquamation, esp. of palms & soles (late finding)
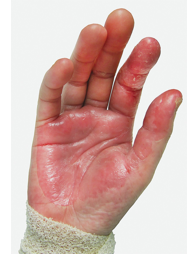
TSS
Lab findings in TSS are consistent with what?
shock and organ failure
What is empiric antibiotic tx for TSS?
Clindamycin + Vanco
(Also needs rapid rehydration–> 3L)
What condition is caused by Staph aureus and is primarily in neonates 3-15 days old?
Staph Scalded Skin Syndrome (SSSS)
Clinical presentation of which condition?
- Prodrome: fever, irritability
- Erythematous patches with large superficial fragile blisters
- When blisters rupture, skin appears red and scalded
- Nikolsky sign (only the first layer)
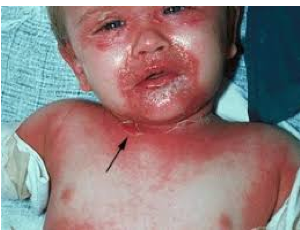
Staph Scalded Skin Syndrome (SSSS)
Diagnosis of what?
- Clinical with cultures
- Skin biopsy shows intraepidermal cleavage without necrosis**
Staph Scalded Skin Syndrome (SSSS)
What type of abx should be used to tx SSSS? If there is no response, what 2 meds should you consider?
- Penicillinase-resistant beta-lactam agents (Nafcillin)
- If no response, consider MRSA & tx with vancomycin
Etiology of Anthrax?
Bacillus anthracis
T/F: there has been bioterrorism w/ anthrax spores
True
Hallmark of what condition?
- Painless eschar with extensive surrounding edema
(will be on exam)
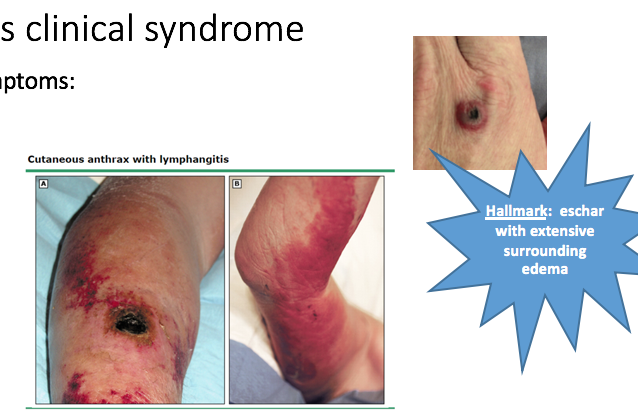
Cutaneous clinical syndrome of Anthrax
What causes:
- hemorrhagic mediastinitis
- occasionally necrotizing pneumonia
- Bacteremia
Inhalation clinical syndrome of Anthrax (the most dangerous form)
Which clinical syndrome has a prodrome including sxs like hemoptysis and dyspnea and can resultmin death within days
INHALATION clinical syndrome of Anthrax
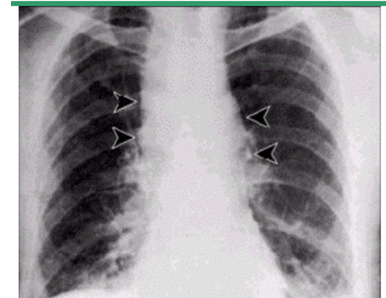
What is seen on CXR of the inhaled form of Anthrax?
(will be on exam)
Widened mediastinum
What is the GI form of Anthrax from?
consumptom of undercooked, infected meat from animals infected with anthrax
Which infectious disease causes:
- Necrotic ulcers surrounded by extensive edema of infected intestinal segment and adjacent mesentery
- Can cause GI hemmorrhage
GI tract clinical syndrome of Anthrax









