Define ‘immunity’.
Ability of a host (usually your patient) to resist invasion and damage by pathogens (usually micro-organisms such as bacteria, viruses, fungi or parasites).
Define immunocompetence.
‘Normal’ immunity, conferring similar ability to resist invasion and damage by pathogens as other indiviuals in the population.
Define immunocompromise.
Attenuated or absent immuity, leaving the patient more vulnerable to invasion and damage by pathogens than others in the population.
What causes the innate immune system to be compromised?
- Broken skin
- Cellulitis and abscesses
- Base of skull fractures
- Pneumococcal meningitis
- Ciliary dysfunction
- Increased respiratory infection
- Bladder outflow obstruction
- UTI and pyelonephritis
- Chemotherapy
- Bone marrow suppression and neutropaenia
What causes the adaptive immune system to be compromised?
- HIV
- Immune cell depletion (especially helper (CD4) T cells)
- Drugs (e.g. for autoimmune disease / post-transplant)
- Deliberate targeted suppression of specific immune activities
What are the 3 primary organs of the immune system and what causes them to become compromised?
- Thymus
- Key organ of T-cell development, especially in children.
- Failure to develop or dysfunction causes T cell deficiency.
- Bone marrow
- Site of WBC synthesis.
- Dysfunction (e.g. leukaemia, drugs) causes neutropaenia ad other cell subset deficiencies.
- Spleen
- Synthesises antibodies, removes antibody-coated bacteria, stores monocytes and lymphocytes.
- Loss increases the risk of sepsis from encapsulated bacteria.
Describe primary (congenital) immune deficiency.
- Rare
- Often hereditary
- (Autosomal recessive or X-linked)
- Some causes:
- Di George’s syndrome
- X-linked agammaglobulinaemia
- Severe combined immunodeficiency
- Ataxia telangiectasia
- Chronic granulomatous disease
- Complement deficiencies
Describe secondary (acquired) immune deficiency.
- Common
- Multiple causes
- Risk factors:
- Extremes of age
- Concurrent illness
- Cancer
- DM
- Organ failure (e.g. liver cirrhosis)
- Some causes:
- HIV
- Splenectomy (trauma, infarct, surgery)
- Immune suppressive medication
What is the relationship between immune deficiency and immune dysregulation?
- Immune deficiency
- Increased predisposition to infection.
OFTEN GOES TOGETHER WITH
- Immune dysregulation
- Inappropriate inflammatory responses.
- Adverse drug reactions.
- Higher risk of malignancy.
Describe the charateristics of infection in immunocompromised patients.
- Often chronic, severe or recurrent.
- May only partially resolve after ABx therapy.
- The organisms involved are often unusual (‘opporunistic’).
- Clinical presentation can by atypical.
- Risk of antimicrobial resistance.
- The organisms involved are influenced by the nature of the immune defect.
What are the possible causes and high risk pathogens for neutropaenia or neutrophil dysfunction?

What are the possible causes and high risk pathogens for complement deficiency?

What are the possible causes and high risk pathogens for T cell deficiency?
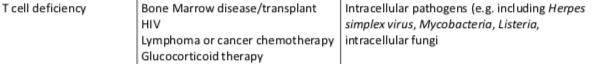
What are the possible causes and high risk pathogens for B cell / antibody deficiency?

What are the warning signs for primary immunodeficiency?
- Sometimes part of multi-system ‘syndromes’ with other key features.
- Often identified in early childhood. Consider if:
- Recurrent ear / sinus / chest infections
- Failure to gain weight or meet growth milestones
- Persistent oral candida in mouth, or fungal infections on skin
- ≥2 deep-seated infections, including sepsis
- FHx of primary immunodeficiency
- Investigation and management requires speciality immunology input.
Describe Di George syndrome.
- 1-5 / 100,000 live births.
- Autosomal dominant deletion on chromosome 22.
- Failure of 3rd & 4th pharyngeal arches to develop.
- Parathyroid gland, aortic arch and thymus do not develop.
- Dysmorphic faces, hypo-PTH.
- Increased incidence of fungal and protozoan infection.
- Specialist care includes:
- Calcium supplementation
- Correction of cardiac abnormalities
- Prophylactic ABx
- Thymic transplantation
Give examples of other conditions which cause primary T & B lymphocyte deficiencies.
- Severe combined immunodeficiencies (SCID)
- Hyper IgM syndrome
- Ataxia telangiectasia
Give examples of conditions which cause primary B lymphocyte deficiency.
- X-linked agammaglobulinaemia (XLA)
- Selective IgA deficiency
- Common variable immunodeficiency (CVID)
Give examples of conditions which cause primary neutrophil function deficiency.
- Chronic granulomatous disease
- Leucocyte adhesion defect (LAD)
What is neutropaenia?
Define mild, moderate and severe.
- A decrease in peripheral blood neutrophil count.
- Mild - 1.0-1.5 x 109 /L
- Moderate - 0.5-1.0 x 109 /L
- <0.5 x 109 /L
- Common in oncology patients post-chemotherapy (day 8-10 nadir), post-radiotherapy, or due to marrow infiltration by malignancy.
What is febrile neutropaenia?
- Neutropaenia (especially severe) and temperature >38.
- 50-60% of febrile neutropaenic patients will have infection.
- 16-20% of febrile neutropaenic patients will have bacteraemia.
- Sepsis may present without a focal source.
- The illness may progress rapidly.
Describe the treatment and prevention of neutropaenia and sepsis.
- Look carefully for an infective source including lines.
- Treatment:
- Remember your sepsis 6
- IV ABx within the first hour
- Piperacillin-tazobactam + gentamicin or meropenem
- Prevention:
- Vaccines up to date?
- Screen for opportunistic infections
- Prophylactic medications
- IVIg and G-CSF
Which drugs can be implicated in immunocompromise?
- Corticosteroids
- Disease-modifying antirheumatic drugs (DMARDs)
- Conventional
- Azathioprine
- Hydroxychloroquine
- Methotraxate
- Sulfasalazine
- Biological
- Abatacept
- Adalimumab
- Etanercept
- Infliximab
- Rituximab
- Tocilizumab
- Organ transplantation and anti-rejection medication
- Cyclosporin
- Tacrolimus
- Conventional
17-year old trauma patient.
Spleen removed after road traffic accident.
What are the specific risks? What should be done?
- Highest risk is sepsis from capsulated organisms.
- Overwhelming post-splenectomy infection (OPSI)
- ~0.5% per year, 5% lifetime risk
- Vaccinations:
- Pneumococcal
- H. influenzae b
- Meningococcal influenzae
- Preventative ABx:
- At least 2 years, maybe lifelong


