Tube mechanism for urine formation (Ludwig)
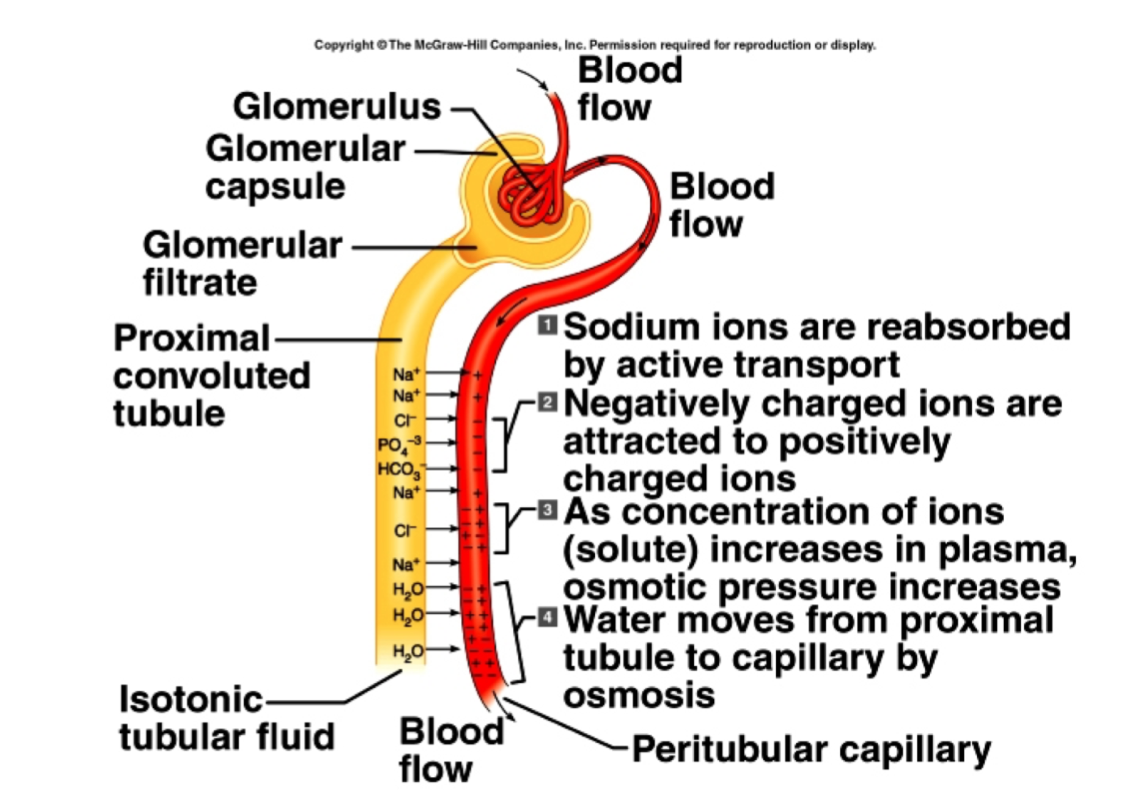
- Filtration occurs at the glomeruli - BP pushes fluid through the wall of the glomerular capillaries into tubules - fluid carries all components of blood except proteins - part of fluid entering the nephron is re-absorbed by an ‘endosmotic force’ due to presence of protein in peritubular capillary blood
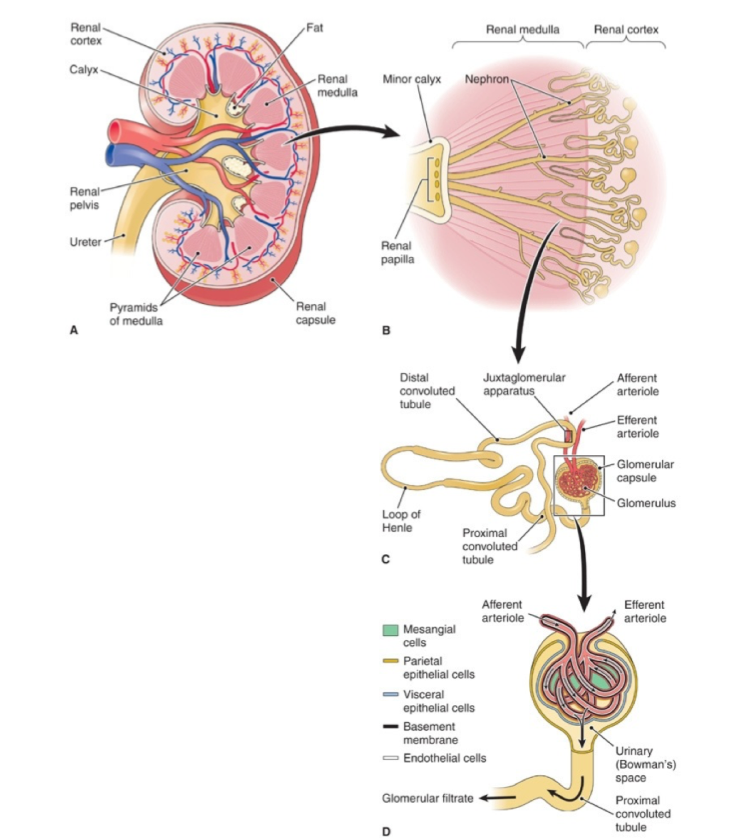
Functional unit - The Nephron
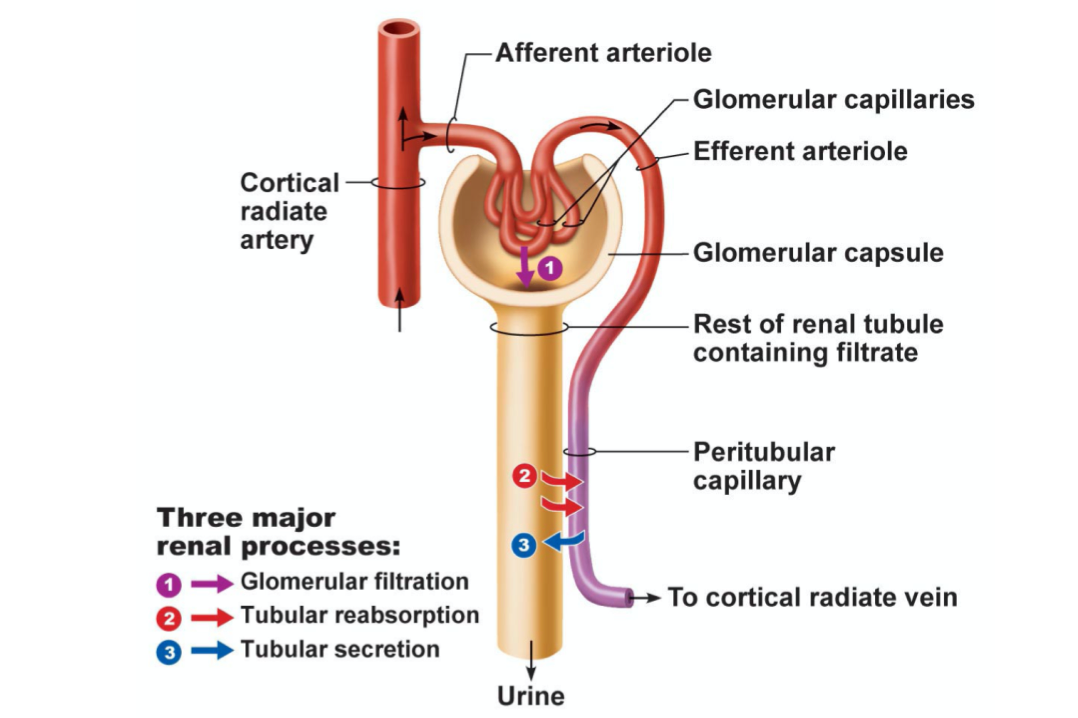
Each nephron has its own control centre => 1 million control centres
Composition of urine
90-95% water
Other 5%:
- Metabolic wastes (urea, uric acid, creatinine)
- Ions (Na, K, PO43-, SO42-, Ca, Mg)
- Toxins, pigments and hormones
Characteristics:
- Yellow, ammonia odour
- pH (4.5-8, usually acidic)
- Specific gravity 1.001 - 1.035
How much CO does the kidney receive
20%
What are the 2 hormones the kidney produces
EPO
Vit D
7 functions of the kidney
- Regualtion of body fluid vol
- Regulation of osmotic balance
- Regulation of electrolyte composition
- Regulation of acid-base balance
- Regulation of BP
- Erythropoiesis
- Excretion of waste products & foreign substances
What is the deepest layer of the kidney
Renal calyxes & pelvis leading to ureter
What is the nephron composed of
- A real corpsucle
- Vascular glomerulus within a matrix formed by mesangial cells
- Epithelial Bowman’s Capsule
What is the structure of the proximal tubule
Intermediate segments S1 & S2 in the renal cortex
Straight segment (S3) which enters outer medulla
What is the structure of the loop of Henle
Medullary thin descending & thin ascending limbs and a thick ascending limb with outer medullary and cortical segments
What does the cortical diluting segment include
Early distal tubule that makes contact with the afferent arteriole at the macula densa cells forming the juxta glomerular apparatus, followed by the cortical distal convolutions and the connecting segment
What segments does the collecting duct have
- Cortical
- Outer medullary
- Inner medullary
What are the 3 types of cortical nephrons
Superficial (30%)
Midcortical (60%)
Juxtamedullary (10%)
Where are superficial nephrons found
Glomerulus in outer cortex and loop of Henle that bends in the outer medulla
Where are midcortical nephrons found (2 types)
Glomerulus in mid cortex and short loops that bend in the outer medulla - 10%
Loops of intermediate length that bend at various points in the inner medulla - 50%
Where are juxtamedullary nephrons found
Glomeruli in inner cortex next to the medulla and long loops that reach the tip of the papilla
What influences the proportion and length of the loops of Henle
proportion and length of the long loops of Henle increase in proportion to the urine concentrating capacity of the animal
What is special about cells of the Proximal Convoluted Tubule and the Thick Ascending Limb
- high rates of solute transport
- abundant mitochondria
- extensive microvilli on the luminal plasma membrane
- infoldings of the basolateral membrane
- rich in basolateral Na+/K+ ATPase
What is special about cells in S2 segment of the proximal convoluted tubule
- Prominent basolateral infoldings
- Less microvilli and mitochondria than in S1 - consistent with participation of S2 in secretory transport
What is special about the cells in S3
- Abundant microvilli
- basolateral infoldings and mitochondra are LESS prominent than in S1
- The thin limbs of Henle have flattened cells with no mitochondria and little ATPase activity
3 different types of cells in the collecting ducts
- Principle cells - abundant water channels (aquaporins) & NA/K ATPase
- alpha intercalated, mitochondria rich cells with abundant proton ATPases
- beta intercalated, mitochondria rich cells with abundant proton ATPases
What is the initial step in renal function and how is it carried out
Formation of a plasma ultrafiltrate (plasma without cells or proteins) at Bowman’s space through the action of hydrostatic pressure in the glomerular capillaries
Where does the ultrafiltrate flow and how is it modified
Flows along tubules
Modified by reabsorption (retrieval) of important solutes (sodium, salts, glucose, AAs) and most water from lumen of the tubules back into the peritubular capillary blood
ALSO modified by secretion (addition) of solutes from peritubular capillaries (or from tubule cells) into lumen
What do the proximal tubules reabsorb back into the peritubular capillaries
2/3 of the Na+ and water & most of the bicarbonate, glucose, AAs filtered & little albumin that may have been filtered at the glomeruli


