What is the following clinical sign and what does it indicate?
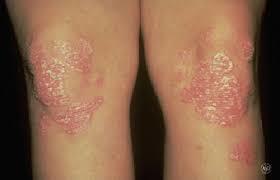
Psoriasis plaques: typically present over extensor surfaces and important to note due to the increased risk of psoriatic arthritis.
What can cause abnormal patellar position?
Patellar position: the patella is normally located over the centre of the knee joint and any deviation from this central position may indicate patellar dislocation or subluxation (i.e. partial dislocation).
What can cause knee hyperextension?
Extension abnormalities: knee hyperextension can occur secondary to cruciate ligament injury.
What can cause fixed flexion deformity?
Flexion abnormalities: fixed flexion deformity at the knee joint may suggest the presence of contractures secondary to previous trauma, inflammatory conditions or neurological disease.
What is the patellar apprehension test?
Patellar apprehension test
The patellar apprehension test is not usually performed in an OSCE, but it’s useful to understand how the test is carried out.
With the patient’s knee fully extended lateral pressure is applied to the patella whilst simultaneously slowly flexing the knee joint. The presence of active resistance from the patient is suggestive of previous patellar instability and dislocation (as the patient is apprehensive about it recurring).
What can cause tenderness upon palpation of the medial and lateral joint lines of the knee including the collateral ligaments?
Palpate the medial and lateral joint lines of the knee including the collateral ligaments for evidence of tenderness which may suggest:
Fracture
Meniscal injury (e.g. meniscal tear)
Collateral ligament injury (e.g. rupture)
Palpate the tibial tuberosity for evidence of a bony elevation and tenderness which is typically associated with ?
Osgood-Schlatter disease.
How would you assess the posterior cruciate ligament?
Posterior sag sign
The posterior cruciate ligament (PCL) is responsible for preventing backward displacement of the tibia or forward sliding of the femur. As a result, if the PCL is ruptured the tibia can sag posteriorly in relation to the femur and this is what is known as the ‘posterior sag sign’.
To screen for the posterior sag sign make sure the patient is relaxed and ask them to flex their knee to 90º with their foot placed flat on the bed. Inspect the lateral aspect of the knee joint for evidence of posterior sag.
It is important to identify this sign before proceeding to the anterior drawer test, as a posterior cruciate ligament tear can result in a false positive anterior drawer sign. This is because an anterior movement of the tibia will occur during the anterior drawer test due to the tibia moving from a posteriorly subluxed position back to its neutral position. This relocation of the tibia to its neutral position may then be misinterpreted as excessive anterior movement secondary to anterior cruciate ligament laxity or rupture.
Alternatively can do posterior drawer test
How would you assess the anterior cruciate ligament?
Anterior drawer test
The anterior drawer test is used to assess the integrity of the anterior cruciate ligament.
- Position the patient supine on the clinical examination couch with their knee flexed to 90º.
- Wrap your hands around the proximal tibia with your fingers around the back of the knee joint.
- Rest your forearm down the patient’s lower leg to fix its position.
- Position your thumbs over the tibial tuberosity.
- Ask the patient to keep their legs as relaxed as tense hamstrings can mask pathology.
- Pull the tibia anteriorly and feel for any anterior movement of the tibia on the femur. With healthy cruciate ligaments, there should be little or no movement noted. Significant movement may suggest anterior cruciate ligament laxity or rupture.
What is Lachmans test?
Lachman’s test
Lachman’s test is an alternative test assessing for laxity or rupture of the anterior cruciate ligament (ACL). This test is rarely required in an OSCE scenario, with the anterior drawer test being the preferred method of ACL assessment.
- Flex the patient’s knee to 30°.
- Hold the lower leg with your dominant hand with your thumb on the tibial tuberosity and your fingers over the calf.
- With the non-dominant hand, hold the thigh just above the patella.
- Use the dominant hand to pull the tibia forwards on the femur while the other hand stabilises the femur.
Significant anterior movement of the tibia on the femur suggests ACL laxity or rupture.
Describe the cruciate ligaments in the knee
Cruciate ligaments of the knee
The cruciate ligaments of the knee include the anterior cruciate ligament (ACL) and the posterior cruciate ligament (PCL).
The ACL originates from deep within the notch of the distal femur and inserts in the anterior region of the intercondylar area of the tibia. Its primary purpose is to stabilise the knee joint by preventing anterior tibial subluxation (i.e. prevent anterior displacement of the tibia relative to the femur). ACL injury (i.e. rupture) typically occurs when a patient lands on a leg and then quickly pivots in the opposite direction resulting in a valgus twisting injury (e.g. in football).
The PCL originates from the lateral edge of the medial femoral condyle and attaches in the posterior region of the intercondylar area. Its primary purpose is to stabilise the knee joint by preventing posterior tibial subluxation (i.e. prevent posterior displacement of the tibia relative to the femur). PCL injury typically occurs secondary to hyperflexion of the knee joint (e.g. a fall onto a flexed knee).
The ACL and PCL cross over each other, forming a cross shape (the Latin translation of cruciate is “cross-shaped”).
Describe the collateral ligaments in the knee
Collateral ligaments of the knee
The collateral ligaments of the knee include the medial collateral ligament (MCL) and the lateral collateral ligament (LCL).
The primary function of the MCL is to stabilise the knee by resisting valgus forces that would push the knee medially. Injury of the MCL typically occurs secondary to excessive valgus force when the knee is partially flexed (e.g. a direct blow to the lateral aspect of the knee joint).
The primary function of the LCL is to stabilise the knee by resisting varus forces that would push the knee laterally. Injury of the LCL typically occurs secondary to excessive varus force (e.g. a direct blow to the medial aspect of the knee joint).
How would you assess the Lateral collateral ligament ?
Lateral collateral ligament assessment (varus stress test)
The lateral collateral ligament (LCL) assessment involves the application of a varus force to assess the integrity of the LCL of the knee joint.
The instructions below are for examining the right knee, use the opposite hands if assessing the left knee.
- Extend the patient’s knee fully so that the leg is straight.
- Hold the patient’s ankle between your right elbow and side.
- Position your right palm over the medial aspect of the knee.
- Position your left palm a little lower down over the lateral aspect of the lower limb, with your fingers reaching upwards to palpate the lateral knee joint line.
- Push steadily outward with your right palm whilst pushing inwards with the left palm.
- Whilst performing this manoeuvre, palpate the lateral knee joint line with the fingers of your left hand.
With healthy collateral ligaments, there should be no abduction or adduction possible.
If there is LCL laxity or rupture your fingers should be able to feel a palpable gap caused by the lateral aspect of the joint opening up secondary to the varus force being applied.
How would you assess the Medial collateral ligament?
Medial collateral ligament assessment (valgus stress test)
The medial collateral ligament (MCL) assessment involves the application of a valgus force to assess the integrity of the MCL of the knee joint.
The instructions below are for examining the right knee, use the opposite hands if assessing the left knee.
- Extend the patient’s knee fully so that the leg is straight.
- Hold the patient’s ankle between your right elbow and side.
- Position your left palm over the lateral aspect of the knee.
- Position your right palm a little lower down over the medial aspect of the lower limb, with your fingers reaching upwards to palpate the medial knee joint line.
- Push steadily inward with your left hand whilst pushing outwards with the right hand.
- Whilst performing this manoeuvre, palpate the medial knee joint line with the fingers of your right hand.
With healthy collateral ligaments, there should be no abduction or adduction possible.
If there is MCL laxity or rupture your fingers should be able to feel a palpable gap caused by the medial aspect of the joint opening up secondary to the valgus force being applied.
How would you assess for a meniscal tear?
McMurray’s test is used to assess the menisci for evidence of a meniscal tear. This test is not usually expected in an OSCE scenario as it can cause significant pain and even meniscal injury if performed incorrectly. It is important however to have an awareness of how and why the test is performed.
McMurray’s test for assessing the medial meniscus
The instructions below are for examining the right knee, use the opposite hands if assessing the left knee.
- With the patient supine on the clinical examination couch, passively flex the knee being assessed as far as is possible.
- Hold the patient’s right knee with your left hand, with your thumb over the medial aspect and fingers over the lateral aspect of the joint lines.
- Hold the patient’s right foot by the sole using your right hand.
- Create valgus stress on the knee joint with your left hand by applying outward pressure as if trying to abduct the leg at the hip whilst fixating and externally rotating the foot. At the same time slowly extend the knee joint.
The presence of a click and discomfort is suggestive of a medial meniscal tear.
McMurray’s test for assessing the lateral meniscus
The instructions below are for examining the right knee, use the opposite hands if assessing the left knee.
- With the patient supine on the clinical examination couch, passively flex the knee being assessed as far as is possible.
- Hold the patient’s right knee with your left hand, with your thumb over the medial aspect and fingers over the lateral aspect of the joint lines.
- Hold the patient’s right foot by the sole using your right hand.
- Create varus stress on the knee joint with your left hand by applying inward pressure as if trying to adduct the leg at the hip whilst fixating and internally rotating the foot. At the same time slowly extend the knee joint.
The presence of a click and discomfort is suggestive of a lateral meniscal tear.
Describe the menisci of the knee
Menisci of the knee
The menisci of the knee are two crescent-shaped pads of fibrocartilagenous tissue which function to stabilise the knee joint and distribute friction between the femur and tibia. Injury to the menisci can occur secondary to sudden twisting of the knee (e.g. in football) which tears the meniscal tissue. Typically symptoms of meniscal injuries include sudden-onset pain, a popping sensation, locking and instability of the knee joint.
What further investigations/Examinations will you do?
Further assessments and investigations
Neurovascular examination of both lower limbs.
Examination of the joints above and below (e.g. ankle and hip).
Further imaging if indicated (e.g. X-ray and MRI).


