Gastrointestinal System components
A) GASTROINTESTIINAL TRACT
1) Alimentary canal
- oral cavity
- pharynx
- oesophagus
- stomach
- small intestine (duodenum, jejunum, ileum)
- large intestine (caecum, colon, rectum)
- anus
2) Sphincters
- upper esophageal sphincter
- lower esophageal sphincter
- pyloric sphincter
- ileocaecal sphincter
- anal sphincter
B) ACESSORY ORGANS
3) Salivary glands
4) Liver & gall bladder
5) Pancreas
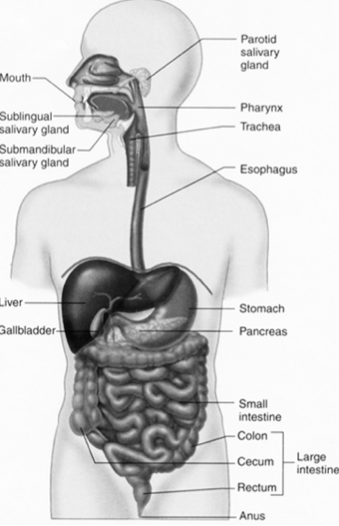
GIT innervation overview
Controlled involuntarily via the autonomic nervous system:
1) Parasympathetic
- Vagal nuclei
- Sacral spinal cord
2) Sympathetic
- paravertebral and prevertebral ganglia
The above two leads to the local enteric nervous system:
3) Submucosal plexus (Meissner’s plexus)
4) Myenteric plexus (Auerbach’s plexus)
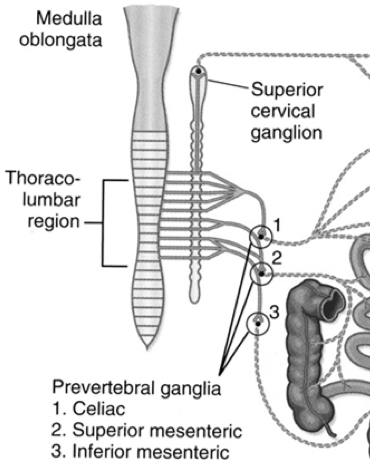
GIT sympathetic innervation
Originates from preganglionic nerve fibres from the central nervous system. Via the thoracolumbar region of spinal cord, they enter:
1) Paravertebral sympathetic ganglion
- Superior cervical ganglion
2) Prevertebral sympathetic ganglion
- Coeliac ganlion
- Superior mesenteric ganglion
- Inferior mesenteric ganglion
3) Hypogastric plexus
Function: Usually inhibit motility & secretion; excitatory to sphincters
Nature: Adrenergic
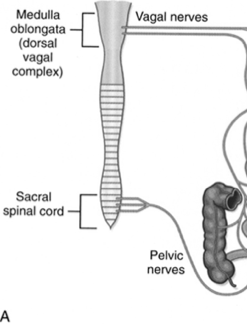
GIT parasympathetic innervation
Originates from the vagal nuclei in the medulla oblongata and the neurons in the sacral spinal cord. Connected to the GIT via the vagal nerve and pelvic spinal nerves respectively.
Extrinsic innervation terminates on neurons of enteric nervous system, influences motor & secretory activity via the enteric nervous system
Function: Usually stimulates motility & secretion
Nature: Cholinergic
Enteric Nervous System
Consists of:
1) Myenteric plexus
- between circular and longitudinal muscles of muscularis externae)
- control smooth muscle activity (muscularis externae)
2) Submucosal plexus
- in submucosal layer
- control submucosal gland secretion and smooth muscle activity of muscularis mucosae (secretomotor)
- Submucosal & myenteric plexuses contain motor, sensory & interneurons;
- Form reflex arcs that are located wholly within the GIT
- Can coordinate GI activity in the absence of extrinsic innervation; also influenced by extrinsic autonomic innervation
- Releases mediators like acetylcholine, nitric oxide, vasoactive intestinal peptides (VIP), enkephalins, serotonin, substance P & other neuropeptides
Processing of Food in GI Tract
1) Digestion
- Chemical breakdown of food into molecules able to cross mucosa and absorbed into the blood
- Availability of digestive enzymes depends on regulation of secretion; enzyme functions at optimal pH
2) Absorption
- Absorption of nutrients, vitamins, minerals, water & electrolytes
- Large absorptive capacity
- Almost all digestive products absorbed completely in early part of small intestine
- About 90% ingested and secreted fluid absorbed in small intestine, remainder absorbed in colon, about 100 ml excreted in feces
Exocrine Secretions of GI System
Salivary glands
- amylase (digest starch)
- electrolyte & water (moisten food)
- mucus (lubrication)
Esophagus
- mucus (lubrication)
Stomach
- mucus (lubrication)
- HCl (kill microbes, activate enzymes)
- intrinsic factor (absorption of vitamin B12 in small intestine)
- enzyme (protease)
Pancreas
- enzymes (protease, lipase, amylase)
- Bicarbonate (neutralize HCl from stomach, activate enzymes)
Liver
- Bile salt (emulsification of fat)
- bicarbonate (neutralize HCl from stomach, activate enzymes)
- organic waste products (to be eliminated in feces)
Small intestine
- mucus (lubrication)
- enzyme (disaccharidease, peptidase)
- electrolyte & water (maintain fluidity of lumenal content)
Large intestine
- mucus (lubrication)
Functions of GI Organs
Mouth
- intake of food
- mastication
- site of carbohydrate digestion
Pharynx
- Swallowing
Esophagus
- Transit of food to stomach
Stomach
- Store, mix and dissolve food
- controlled emptying
- initiation of protein digestion
Duodenum
- Carbohydrate digestion & absorption
- Protein digestion & absorption
- Fat digestion & absorption
Jejunum
- Electrolyte & water transport
Ileum
- Bile salt & Vitamin B12 transport
Colon
- Storage, concentration of undigested material
- Electrolyte & water transport
- Propulsion of content
Rectum & Anus
- defecation
Functions of GI motility
- Chewing & swallowing
- Propulsive movement from mouth to anus
- Mixing of luminal content
- Reduce size of food particles
- Storage function
- Sphincter function
- Optimize time needed for digestion & absorption
- Defaecation
Phases of GI Control
Three Phases:
1) Cephalic phase
- Stimuli from higher centers (thought, sight, smell of food) or mouth (taste, chewing of food)
2) Gastric Phase
- Stimuli from food in the stomach (gastric distension, chyme acidity, osmolarity)
3) Intestinal Phase
- Stimulus arising from chyme in intestine
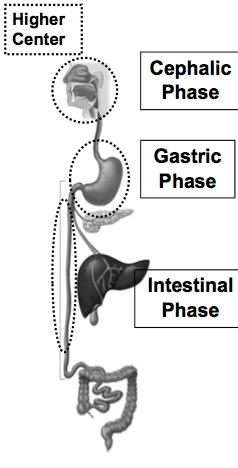
GI Control Mechanisms
Regulated by GI reflexes which involve:
1) Neural regulation (Neurocrine)
- Short neural reflex
- Long neural reflex
2) Chemical regulation
- Endocrine
- Paracrine
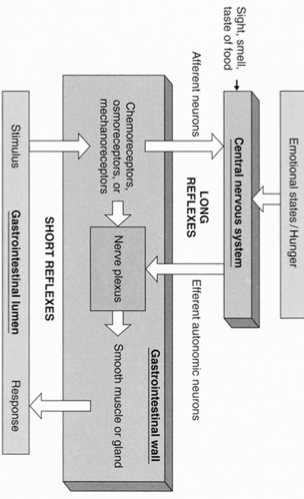
GI neurocrine Control
Higher centers in CNS can initiate control from CNS to enteric nerve plexuses and effector cells via ANS
1) Short reflexes (Enteric reflexes)
- from GI receptors through enteric nerve plexuses to effector cells
2) Long reflexes
- from GI receptors to CNS by afferent nerves & back to enteric nerve plexuses and effector cells by way of ANS
- e.g. vagovagal reflex
Parasympathetic: excitatory
Sympathetic: inhibitory
GI Chemical regulation
Regulation of GI functions like:
- Rate & composition of GI secretion
- Motility of gut & sphincters, gallbladder
- Release of other GI peptides & hormones
- Trophic effects on exocrine glands & mucosa
Mucosal endocrine cells are not organized into discrete isolated glands, but as single cells scattered over a wide area of the mucosa
Hormones:
- Gastrin
- cholecystokinin (CCK)
- secretin
- Gastric inhibitory peptide (GIP)
- Motilin
(-) Vasoactive intestinal peptide (VIP)
(-) Bombesin or Gastrin releasing peptide (GRP)
(-) Enkephalin
Paracrine:
- somatostatin
- histamine
Gastrin features
Action:
- Stimulates gastric acid secretion
- Trophic effect of gastric oxyntic gland mucosa
Site of release: Antrum (& duodenum)
Triggers:
- Peptides
- Amino acids
- Gastric distension
- Vagal stimulation
cholecystokinin features
Action:
- gall bladder contraction
- pancreatic enzyme secretion
- pancreatic bicarbonate secretion
- growth of exocrine pancreas
- inhibits gastric emptying
Site of release: duodenum & jejunum
Triggers:
- Peptides
- Amino acids
- Fatty acids > 8C
(- Acids ?)
Secretin features
Action:
- pancreatic bicarbonate secretion
- Biliary bicarbonate secretion
- growth of exocrine pancreas
- Pepsin secretion
- inhibits gastric acid secretion
- inhibits trophic effect of gastrin
Site of release: duodenum
Triggers:
- Acid
(- fat ?)
Gastric inhibitory peptide features
Action:
- stimulates insulin releas
- inhibits gastric acid secretion
Site of release: duodenum & jejunum
Triggers:
- glucose
- amino acids
- Fatty acids
Motilin features
Action:
- stimulates gastric motility
- stimulates intestinal motility
Site of release: duodenum & Jejunum
Triggers:
- Nerves
- Fat
- Acid
Vasoactive Intestinal peptide features
Action:
- Relaxes sphincters
- Relaxes gut circular muscles
- Stimulates intestinal secretion
- Stimulates pancreatic secretion
Site of release: mucosa & smooth muscle of GIT
Bombesin/ GRP features
Action: Stimulates gastrin release
Site of release: gastric mucosa
Enkephalins
Action:
- Stimulates smooth muscle contraction
- Inhibits intestinal secretion
Site of release: Mucosa and smooth muscle of GIT
Somatostatin features
Action:
- inhibits gastrin release
- inhibits peptide hormone release
- inhibits gastric acid secretion
Site of release: GI Mucosa and pancreatic islets
Triggers:
- Acid
- Vagus inhibits release
Histamine features
Action: Stimulates gastric acid secretion
Site of release: parietal cells (oxyntic gland mucosa) and ECL cells
Triggers: Gastrin


