Precursors of Platelets?
Come from Megakaryoblasts that are: Large, small cytoplasm, immature with nucleoli
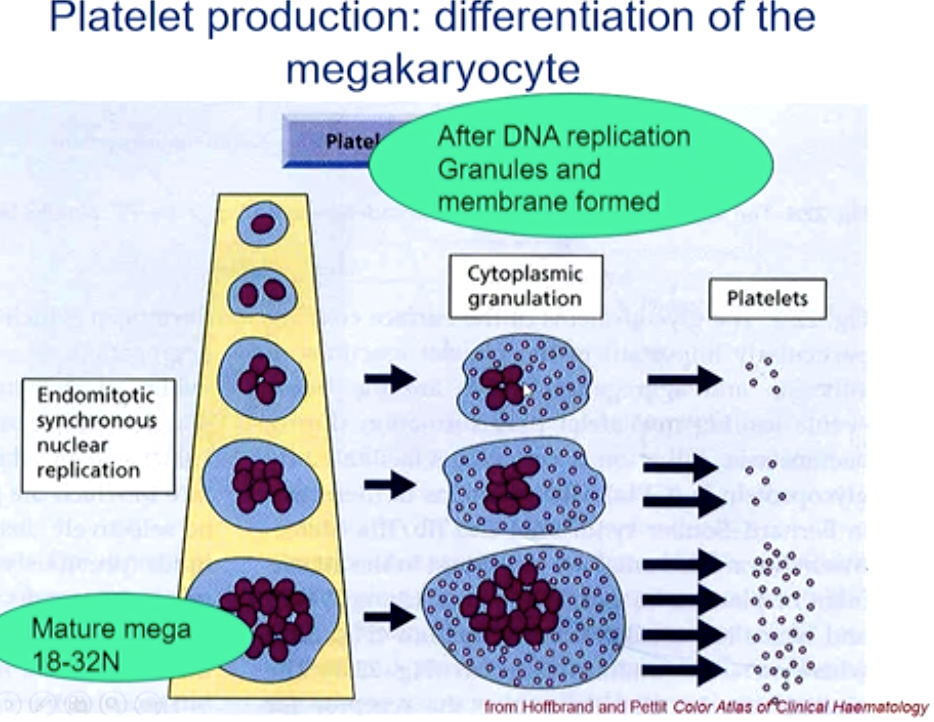
Megakaryocytes are the next step. The have small granules and are found next to the sinusoidal endothelial cells. About 4000 platelets are formed from the breaking up of a single megakaryocyte.
Hormones involved in thrombocytopoiesis? Homeostasis?
- Steel (stem cell) Factor - (early on)
- LIF (leukaemia inhibitory factor)
- Interleukin 6 and 11
- Thrombopoietin (TPO) - MAJOR
Number maintains at a constant level and so we require about 10%- 40000 new platelets/uL/day. (clinically important as Aspirin irreversibly blocks COX enz so after 5 days off it you have 50% of normal platelets at least)
They last about 7-10 days and are consumed by utelisation or senscence.
Platelet ultrastructure?
These are discoid in shape and contain an intricate system of channels continuous with the phospholipid plasma membrane. No Nucleus but does have mitochondria. A and B granules contain various things that are to be released.
Primary Haemostasis? Supression normally?
Primary Haemostasis is the process of forming a platelet plug at the site of vessel injury (trauma or just the general wear and tear)
- phase one is vascular constriction
- phase two is the formation of an unstable platelet plug by aggregation of platelets.
Normally this is stopped by NO and PGI2 being released from intact endothelium.
Platelet interactions?
Von Willebrand factor binds to exposed collagen in the endothelial matrix then binding to resting platelets via Glycoprotein (GP) 1B-V-IX
In a rolling motion the platelet is pulled in releasing granules (eg. thromboxane A2 )that expose Integrin and bring in more platelets and also exposes Integrin AIIbB<strong>3</strong> which is a target for stopping clotting
Fibrinogen then binds between this integrin and the integrin on another activated platelet.
What are the main influences on blood platelet levels?
Decreased Production
- Viral infections, Drugs, Bone marrow failure (rare)- aplastic anaemia, leukaemia, carcinoma
Increased Destruction
- Immune thrombocytopenia (ITP), DIC
Increased Production
- Myeloproliferative neoplasms (essential thrombocythemia)
Names for different types of bruising?
Petechiae - small spots
purpura - larger spots/small bruises
ecchymoses - large bruising


