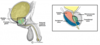
What happens to the mesonephric and paramesonephric ducts in male development? What part of the male DNA allows these changes to occur?
Mesonephric - becomes vas deferens
Paramesonephric - obliterated by production of mullerian inhibiting substance in males
SRY genes on the Y chromosome
What are the mesonephric and paramesonephric ducts AKA?
Mesonephric - Wolffian duct
Paramesonephric - Mullerian duct
What occurs in Turner’s syndrome? When and how is it diagnosed? What is the chromsomal classification?
- 45,XO.
- Results in degeneration of ovaries at 15th week of gestation.
- Diagnosis only occurs post puberty, when a lack of a menstrual cycle and secondary sexual characteristics are revealed.
What is the function of hCG and hPL (human placental lactogen)?
HCG - Promotes progesterone release form corpus luteum
hPL - Decreases maternal insulin and glucose utlitisation. Increases lipolysis.
What is the name of the visceral layer that covers the testis?
Tunica Vaginalis
What occurs post puberty with regards to spermatogenesis? How long does spermatogenesis take? How long does it take for new groups of spermatogonia to arise? What occurs during copuluation? Where do spermatozoa mature?
- At intervals, A1 spermatogonia emerge from population of stem cells, marking beginning of spermatogenesis in that part of the tubule.
- The A1 spermatogonia divide to produce more type A (stem) cells or Type B cells
- Type B spermatogonium divides to produce 64 clones of primary spermatocytes all linked together by a cytoplasm bridge
- Chain of primary spermatocytes push out of lumen of tubule and begin meiosis, producing 256 sperms per A1 spermatogonium.
- After meiosis complete, spermatids remodelled to form sperm by spermiogenesis and the cytoplasmic bridges are broken down. They are then released into the tubule lumen and washed down the rete testis by fluid secreted from Sertoli cells.
- Spermatogenesis takes 70 days and new groups of spermatogonia arise every 16 days.
- Production of sperm is continuous as different sections of the tubule begin the process at different times, therefore some part is always released sperm – Spermatogenic wave of production.
- Spermatozoa mature during progress through epididymis.
- During copulation, contraction of vas deferens sweep sperm to be mixed with seminal and prostate secretions.
Stem cells –> A1 Spermatogonia –> Type B spermatogonia –> primary spermatocytes (linked) –> Spermatids –> sperms (unlinked)
Distinguish between a spermatogenic cycle and a spermatogenic wave
Spermatogenic cycle – Development of A1 spermatogonia through to 256 sperms. Time taken for the same stage of the cycle to reappear in the same segment of tubule.
Spermatogenic wave – Different parts of tubule start the spermatogenic cycle at different times, so a constant ‘wave’ of production of sperm occurs. This can be thought of as the distance between 2 parts of the tubule on the same stage in the spermatogenic wave.
What happens before birth in the ovarian cycle? What are the 3 stages that a follicle must go through to mature? Can a woman produce more oocytes, why?
- Primordial germ cells in the primordial gonad, AKA oogonia, proliferate by mitosis to form primary oocytes.
- Oogonia’s entry to meiosis 1 stimulated by mesonephric cells which surround the primary oocytes to form primordial follicles.
- Meiosis arrested at prophase due to oocyte maturation inhibitor (OMI) secreted by primordial follicles.
- A woman therefore has all the oocytes she will ever have at birth. The longer the oocytes remain in an arrested stage the increases chances there are of cell damage.
- A small number of follicles begin further development each day post puberty, formation of a mature gamete requires follicles to go through 3 stages.
3 stages are - primordial follicle, secondary follicle, pre-ovulatory follicle
What happens in the primordial follicle stage to form the primary follicle?
- The primary oocyte grows dramatically
- Squamous granulosa cells become cuboidal Granulosa cells
- Zona pellucida forms around oocyte
What happens to the primary follicle to get to the secondary follicle? What substance does the theca produce?
- Inner and outer theca forms
- Theca secretes oestrogens
- Fluid filled vesicles develop among granulosa cells
What happens in the secondary follicle stage? What cells do FSH and LH bind to?
- Fluid filled vesicles combine to make one antrum
- Continued development depends on reproductive hormones.
- FSH – Binds only to Granulosa cells
- LH – Binds only to Thecal cells
What happens in the pre-ovulatory stage? How many hours before ovulation does the phase start? After how many hours do unfertilised cells degenerate?
- Phase begins 37 hours before ovulation
- Oestrogen causes receptors for LH to appear on outer Granulosa cells
- LH surge stimulates these receptors, leading to rapid changes in the follicle
- Within 3 hours of the LH surge, the follicle restarts meiosis, and the first meiotic division is completed. This division is asymmetric; cytoplasm remains with one daughter cell and the other forms a condensed polar body.
- The secondary follicle then enters meiosis II and arrests again 3 hours prior to ovulation.
- LH stimulates collagenase activity leading to follicle rupture
- Ovum is carried out in the fluid and gathered up into the fallopian tube by fimbria
- Meiosis is not completed unless the ovum is fertilised
- Unfertilised cells degenerate 24 hours after ovulation
What would happen to an XY individual with genitalia that are insensitive to testosterone or DHT?
- Testes remain in abdomen but removed post puberty due to high risk of malignancy
- Well developed breasts, no pubic hair or menstruation
- Genital ambiguity
What would happen in an XX individual and excessive androgen secretion?
External appearance is male but genetically female with internal genitalia of both sexes
What would happen to an XY individual with resistance to MIH?
Genetically and gonadally male but internal genitalia of both sexes due to test promoting external genitalia and wolffian duct.
Testes will fail to descend
What are the glycoprotein hormones that the ant pit secretes? What cell type produces each hormone?
FSH – produced by gonadotrophs
LH - produced by gonadotrophs
TSH - produced by thyrotrophs
What are the polypeptide hormones that the ant pit secretes? What cell type produces each hormone?
GH - produced by somatotrophs
ACTH - produced by Corticotrophs
Prolactin - produced by lactotrophs
What are the hormones that the post pit produces?
ADH Oxytocin (important for reproduction)
What is the action of GnRH in males? What is the action of FSH and LH? What is inhibin secretion rate related to? What else can affect the production of testosterone?
- Testosterone reduced GnRH secretion
- Spermatogenesis occurs continuously and male must be ready for action at any time. Therefore, hormone levels constant in medium and long term, achieved by –ve feedback
- FSH binds to Sertoli cells
- LH binds to Leydig cells:
- Promotes testosterone release and spermatogenesis
- Inhibin secretion related to rate of spermatogenesis.
- Testosterone is higher in mornings due to circadian rhythms and can be affected by environmental stimuli

What does inhibin do in both sexes? What is inhibin secretion related to?
Inhibin from gonad reduces FSH secretion
Inhibin secretion related to developing gametes - More developed gametes release more inhibin
What is the action of LH during the luteal phase? What about progesterone? How do progesterone only contraceptives function?
LH maintains corpus luteum
Progesterone in this stage acts on oestrogen primed cells:
Further thickening of endometrium
Thickening of myometrium
Thick, acid cervical mucus – barrier against sperm and bacteria between uterus and vagina. This is how progesterone only contraceptives work.
Changes in mammary tissue
At the beginning of the menstrual cycle, what are the levels of progesterone and oestrogen? What happens here?
Low progesterone and oestrogen
FSH levels rise:
- Binds to granulosa cells
- Theca interna develops
- Secretes oestrogen stimulated by LH
- Secretes inhibin
What happens in the mid follicular stage?
- Oestrogen levels rising
- Inhibin levels rising – inhibit FSH, no new follicles can develop
- Oestrogen exerts +ve feedback at hypothalamus and pituitary
- LH levels rise but not FSH
What happens in the pre-ovulatory phase?
LH surge. Precise timing may be influenced by environmental factors