What are indications for NSAID use?
- Mild-to-moderate pain
- Pain related to inflammation - particularly MSK
What inflammatory conditions are NSAIDs particularly useful for?
- RA
- Severe osteoarthritis
- Acute gout
What is the mechanism of action of NSAIDs?
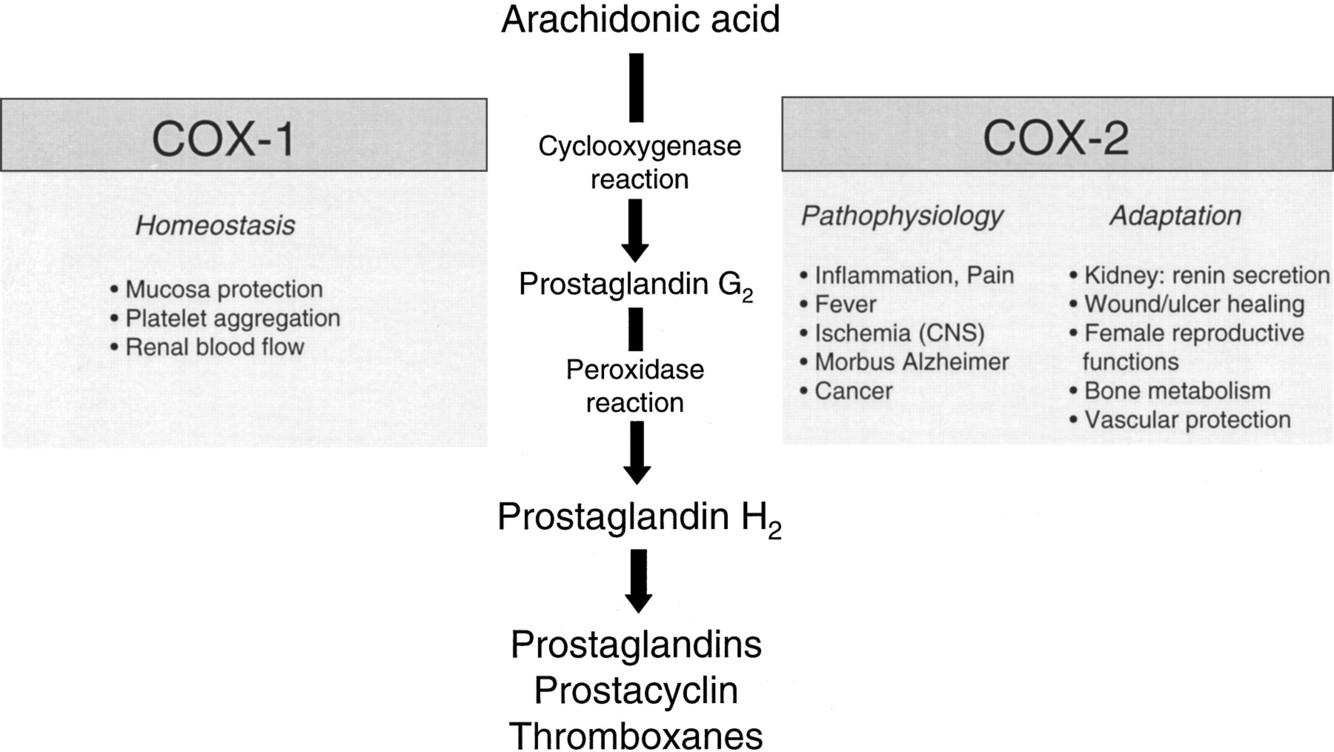
Inhibits synthesis of prostaglandins from arachadonic acid by COX-1 and COX-2. The analgesic effects stem from COX-2 inhibition, which blocks COX-2 influence on the production of prostaglandins which cause inflammation and pain
What is cyclooxygenase?
Enzymes that produce prostaglandins
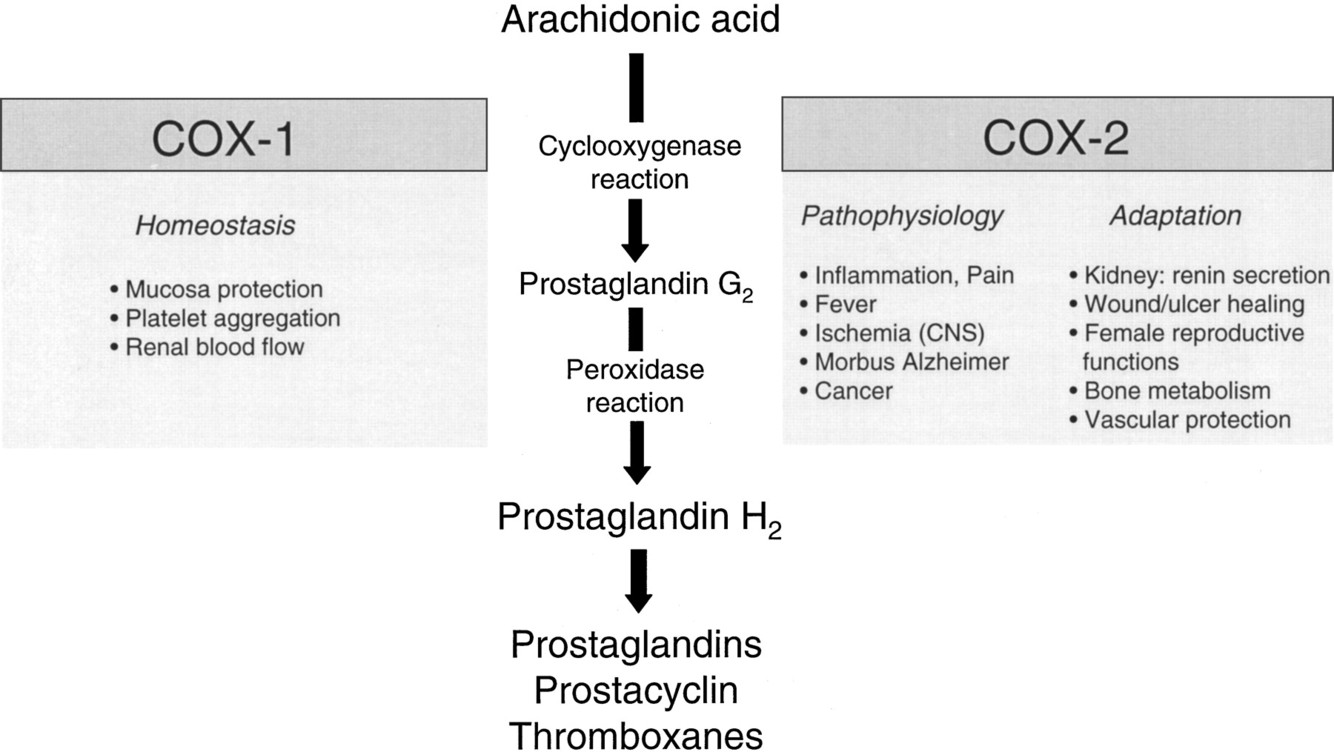
What is the function of COX-1?
COX-1 is the constitutive form. It stimulates prostaglandin synthesis that is essential to preserve integrity of the gastric mucosa; maintain renal perfusion (by dilating afferent glomerular arterioles); and inhibit thrombus formation at the vascular endothelium
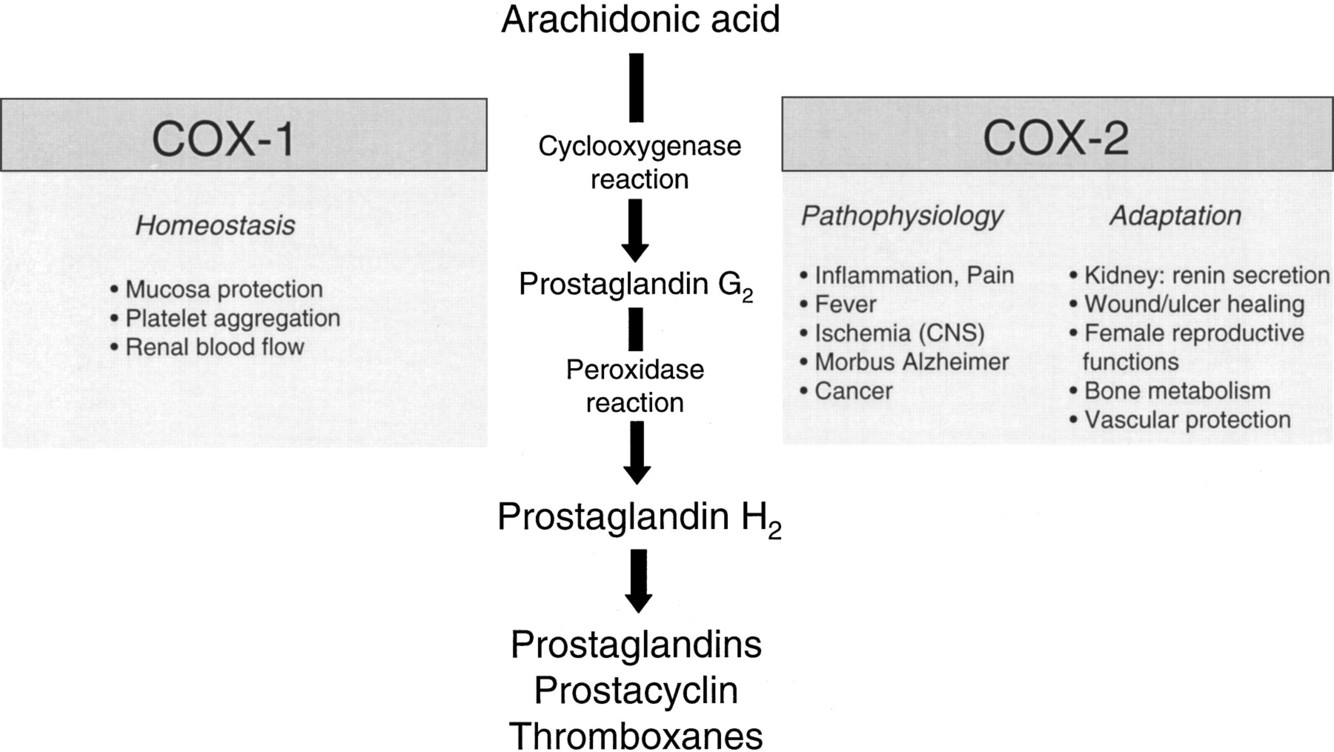
What is the function of COX-2?
COX-2 is the inducible form, expressed in response to inflammatory stimuli. It stimulates production of prostaglandins that cause inflammation and pain
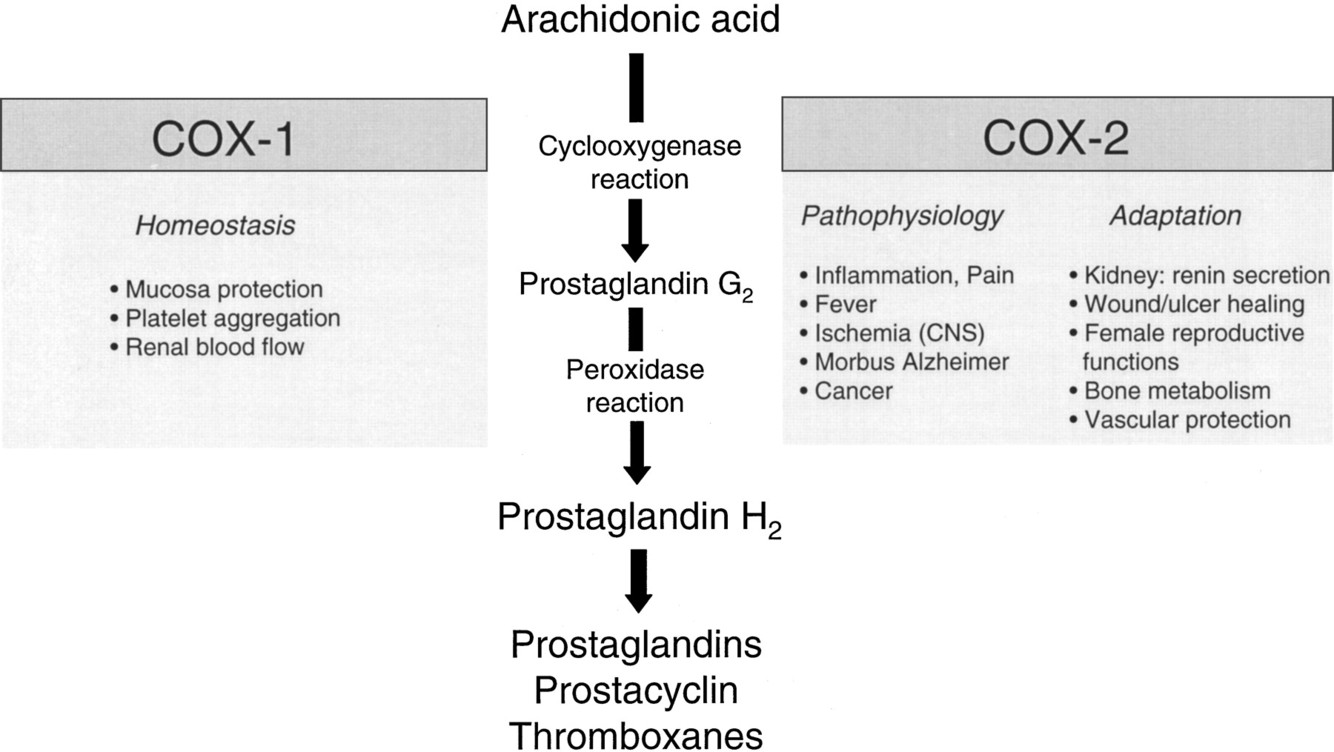
What are the side effects of COX-1 inhibition?
- Damage to gastric mucosa
- Renal hypoperfusion
- Increased CV events risk
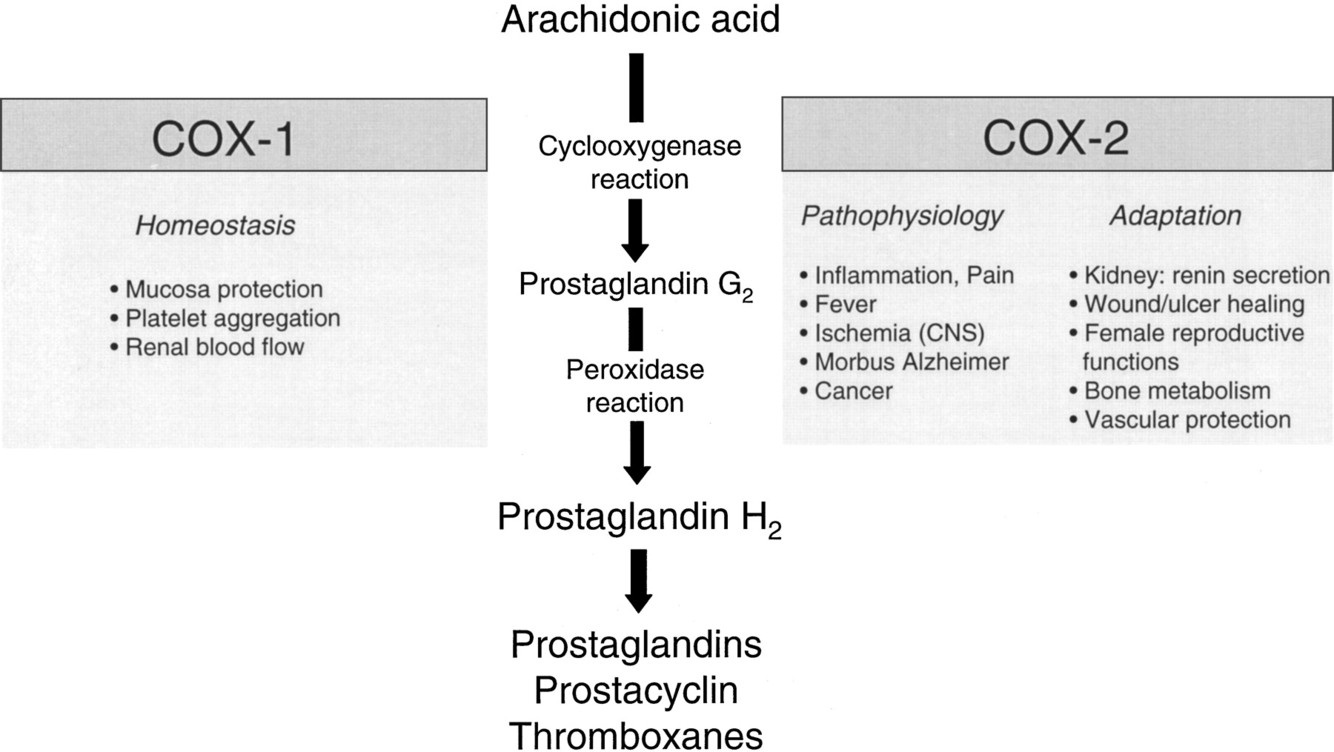
What are side effects of COX-2 inhibition?
Inhibition of prostaglandin production - > inhibition of inflammation and pain
How do NSAIDs affect the kidneys?
COX-1 inhibition leads to constriction of the afferent glomerular arteriole -> AKI. Also causes acute interstitial nephritis
What are side effects of NSAIDs?
- GI toxicity/ulcers
- Renal impairment
- Increased CV tisk - Stroke/MI
- Hypersensitivity reactions
- Fluid retention
When do you need to be cautious when using NSAIDs?
- Severe renal impairment
- Heart Failure
- Liver Failure
- NSAID hypersensitivity
- Peptic ulcer disease
- GI bleeding
- CV disease
What interactions do you need to be aware of when using NSAIDs?
- Low-dose aspirin
- Corticosteroids
- Anticoagulants
- SSRIS
- ACEi
- Diuretics
- Warfarin
How long does treatment with Naproxen take to reach full effect?
3 weeks
What advise would you give someone when giving them NSAIDs?
- Warn of indigestion and to seek medical advise if thise occurs
- Explain risk of long term use
- Advise to stop use if acutely unwell - risk of AKI
What are risk factors for GI complications with NSAID use?
- >65 years
- Previous peptic ulceration
- CVD
- Diabetes
- Concurrent therapy with GI side effects
What drugs do you need to be particularly careful with when using NSAIDs with regards to gastric side effects?
- Low-dose aspirin
- Prednisolone
What would you want to consider prescribing in someone with increased GI risk factors who is prescribed NSAIDs?
Gastroprotection
WHat are examples of NSAIDs?
- Ibuprofen
- Naproxen
- Diclofenac
What dose of ibuprofen would you consider starting someone on for acute pain?
300-400mg, 3-4 times per day


