Reading an ABG?
Respiratory failure:
- Low O2 = T1RF (PaO2 <8kPa)
- Low O2 + High CO2 = T2RF (PaO2 <8kPa, PaCO2 >6kPa)
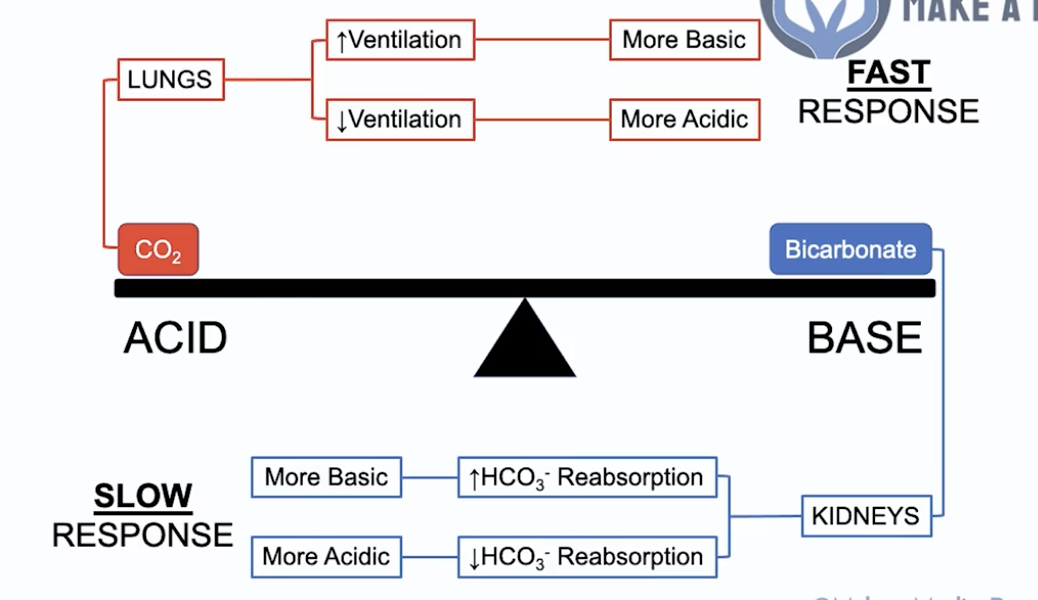
Determining acid: base balance:
- Low pH + high CO2 = Respiratory acidosis (low CO2 = metabolic)
- High pH + low CO2 = Respiratory alkalosis (high CO2 = metabolic)
- NOTE: if bicarb is high in RA = chronic RA (compensation by bicarb is slow) –> this determines if should be on scale 1/2 O2 (scale 2 = 88-92%)
Causes of acid: base balance:
- RA causes: COPD, ILD, hypoventilation, asthma (normally resp alkalosis but can be acidotic if severe)
- MA causes: lactic acid, ketoacids (CO2 blown off to compensate –> Kussmaul breathing)
Asthma - def? Presentation? Ix? Severity? Short-term/long-term Mx incl. conservative? Mneumonic for conservative long-term Mx?
Def: chronic inflammatory airway disease characterized by reversible airway obstruction + airway hyperresponsiveness
Presentation
- Dry cough, polyphonic wheeze ( worse@night/morning)
- Triggers: cold air, pollen, pollution, exercise
- Atopic features - eczema, nasal polyps
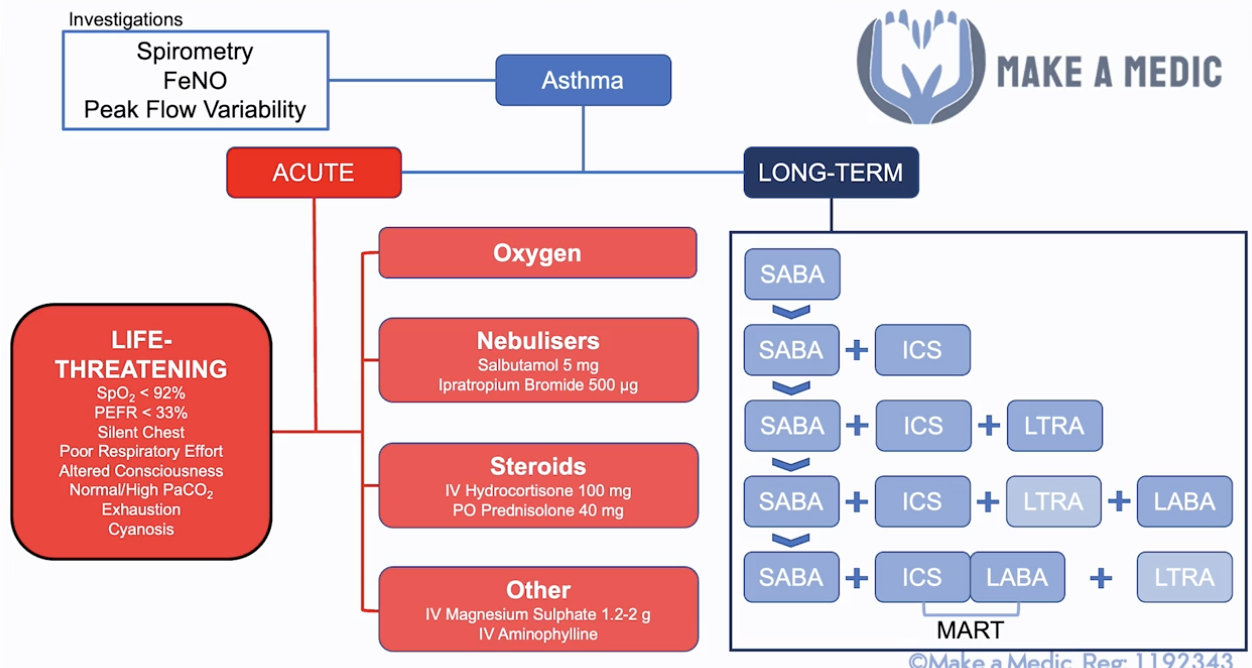
Ix:
- Peak flow variability (in peak flow diary)
- Spirometry (shows reversibility after bronchodilator)
- FeNO (fractional exhaled nitric oxide - a marker of airway inflamme, in uncertain Dx)
- On exacerbation:
- ABG, peak flows (min x4/day), CXR
- Other:
- Allergy testing - total IgE, specific IgE (RAST), serum eosinophil count
Asthma severity:
- Life-threatening: PEF <33% of baseline/SpO2 <92%/PaO2 <8/Normal or raised PaCO2 - should be low with resp alkalosis due to excess breathing only becomes acidotic when get tired
- CHEST: Cyanosis, Hypotension, Exhaustion, Silent chest, Tachycardia
- Acute severe: PEF <50% of baseline/RR >25/HR >110/can’t complete sentence without taking a breath
- Moderate: PEF <75% of baseline
Short-term Mx:
- A-E approach, seek senior support (call for help if life-threatening)
- O2 - 15L NRM (if hypoxaemic)
- Burst therapy:
- SABA (spacer up to 10 puffs every 20 mins –> nebs)
- Ipratropium Bromide (add to nebs if poor response/severe, every 4-6hrs)
- Corticosteroids (min 5-day course, give within 1 hour, give IV if can’t take orally)
- Other Tx options:
- IV Magnesium sulfate (STAT dose if poor response above/severe) - consult senior before use
- IV salbutamol (if on ventilation) - consult senior before use
- IV Aminophylline - consult senior before use, requires ITU setting
- If less distressed/more tired/shallow breaths/confused –> call critical care outreach team (CCOT) for ITU support
Long-term Mx (>16yrs):
- Conservative: TAME
- Technique
- Avoid triggers
- Monitor peak flow
- Educate - formulate Personalised Asthma Action Plan (PAAP), Annual flu vaccine
- Medical:
- SABA (reliever)
- SABA + ICS (preventer)
- SABA + ICS + LTRA (leukotrine receptor antagonist e.g. montelukast)
- SABA + ICS + LABA (+ LTRA stopped unless good response)
- SABA + MART (ICS + LABA COMBO) (+ LTRA)
- NOTE: maintenance & reliever therapy (MART) - used as preventer & maintenance inhaler
- Specialist input (e.g. for oral steroids)
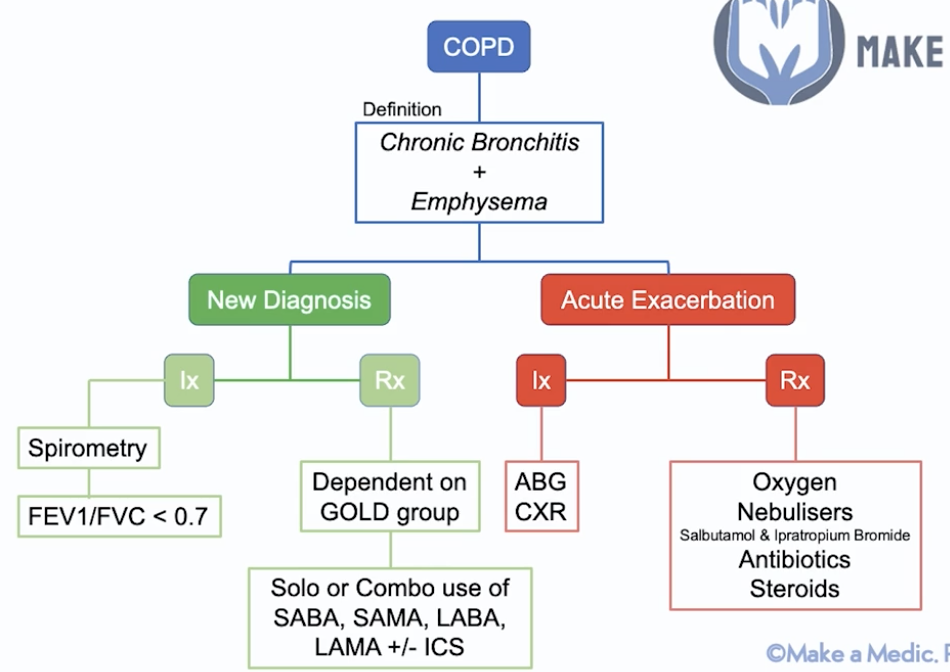
COPD - definition? Signs & Sx? New Dx & exacerbation Ix/Mx? Prognosis factors?
Def: chronic bronchitis (damaged to cilia in bronchi - blue bloater) + emphysema (damage to alveoli - pink puffer)
Presentation:
- Cough (productive), SoB (starts on exercise)
- RF exposure - smoking/pollution
- Signs:
- Barrel chest
- Hyper-resonant (air trapping)
- Reduced breath sounds
- Widespread expiratory wheeze
- Coarse crackles if exacerbation (mucus in airways)
- Other - asterixis (CO2 retention flap), raised JVP (cor pulmonale)
- NOTE: COPD does not cause clubbing –> cancer/bronchiectasis
New Dx Mx:
- Ix:
- Bedside - mMRC dyspnoea scale, O2 sats, ECG (cor pulmonale)
- Spirometry - FEV1/FVC <0.7 (forced exp volume in 1s)
- Mild - FEV1 ≥ 80%
- Moderate - FEV1 ≥ 50%
- Severe - FEV1 ≥ 30%
- Very severe - FEV1 <30%
- Bloods - FBC, ABG, eosinophil count, alpha1-antitrypsin level
- Imaging - CXR, CT chest
- Other: serial peak flows if asthma DDx, sputum culture (in freq exacerbation), pul funct tests
- Mx:
- Conservative - stop smoking, influenza + pneumococcal vaccine, inhaler device training
- Persuade to stop smoking
- Pul rehab
- Prick them - influenza + pneumococcal vaccine
- Psych issues
- Medical - depends on severity - GOLD group –> solo/combo of:
- SABA e.g. salbutamol
- SAMA e.g. Ipratropium bromide
- LABA e.g. salmeterol
- LAMA e.g. tiotropium
- ± ICS e.g. beclomethasone
- Other: mucolytic e.g. acetylcysteine, O2 therapy, theophylline
- Medical pathway:
- 1 - SABA/SAMA
- 2a - Steroid-responsive (eosinophilia/atopy): LABA + ICS
- 2b - Not steroid-responsive: LABA + LAMA
- 3 - LABA + LAMA + ICS
- 4 - specialist input e.g. theophylline
- Surgical - lung reduction surgery (large bullae)
- Other: long-term O2 therapy
- Only if non-smoker (smoker –> burns)
- Only if <7.3 PaO2/<8 if also pul HTN
- Only if PaCO2 does not rise excessively on O2
- Conservative - stop smoking, influenza + pneumococcal vaccine, inhaler device training
Acute Exacerbation Mx:
- Ix: ABG, ECG, CXR
- Mx:
- 15L O2 NRM
- Nebs - salbutamol + IpB
- Steroids (PO pred/IV hydrocortisone)
- Abx if infective –> prophylactic abx if persistent infections - azithromycin
Prognosis factors:
- Body mass - worse if obese
- Obstruction - worse if reduced FEV1
- Dyspnoea
- Exercise capacity - how far can you walk in 6 minutes?
Complication –> vasoconstriction to redirect blood flow to well-oxygenated areas of the lungs –> if widespread –> pul HTN –> cor pulmonale
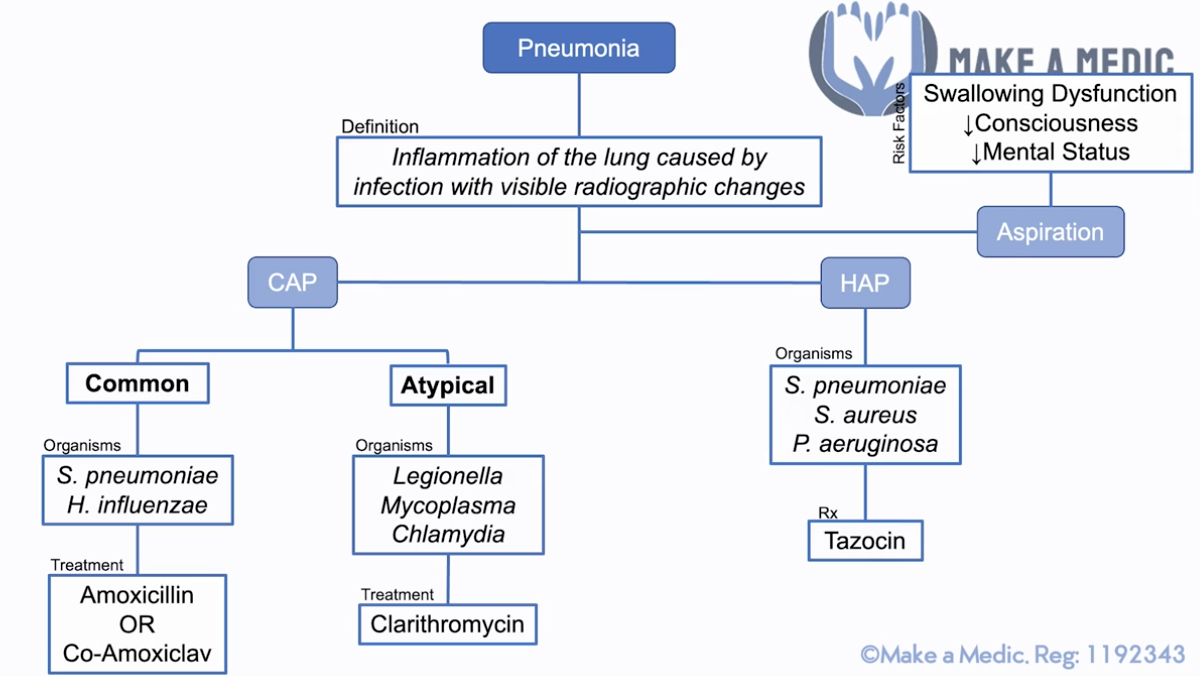
Pneumonia - def? Presentation? Types? Ix? Scoring? Mx?
Def: inflammation of lung caused by inf w/ visible radiographic changes
Presentation:
- Decreased chest expansion, dull on percussion, increased sound vocal resonance
- Coarse crackles
- Bronchial breathing – bronchial airflow instead of alveolar airflow (due to transmission of sounds through consolidation) – check by listening to sound at the throat
Ix: ABG, CXR, sputum culture (mod/high severity)
Scoring for CAP: CURB-65 (confusion, urea ≥7mmol/L, RR ≥30, BP <90/60, ≥65yrs)
- +1 = outpatient; +2 = outpatient/inpatient, +3 = inpatient ± ITU
- NOTE: urea is no longer used
Types & Mx –> local abx guidelines
- CAP:
- Typical (S. pneumo, H. influenzae) –> Amox/Co-Amox
- Atypical (Legionella, Mycoplasma, Chlamydia) –> Clari
- Dry cough (instead of productive), myalgia, confusion, diarrhoea
- NOTE: if not sure often given Co-Amox + Clari
- HAP - pneumonia arising >48hrs after admission to hospital (S. pneumo, S. aureus, P. aeruginosa) –> Taxocin (pseudomonal cover)
- Aspiration - RFs: swallowing dyfunct, reduced consciousness, reduced mental status –> elderly/frail
Goes into septic shock –> give IV fluid + senior help + check abx sensitivity (ring lab) –> ITU (intropic support - NA to increase PVR)
- Other aspects of septic-6
- NOTE: dobutamine is for cardiogenic shock to increase CO - this is not relevant here
PE - def? Sx? RFs? Scoring & Ix? Mx?
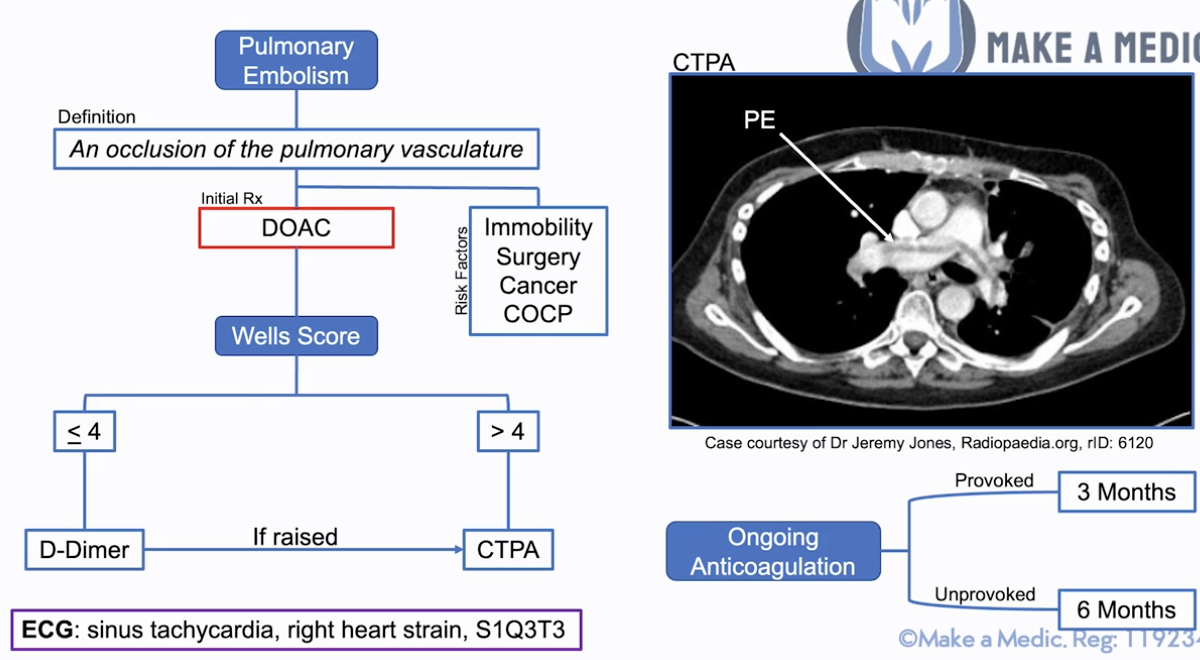
Def: occlusion of pulmonary vasculature characterized by sharp pleuritic chest pain
Sx: SYNCOPE, sudden SoB, pleuritic chest pain, haemoptysis
RFs: SICC - Surgery, Immobility, Cancer, COCP
Initial Tx:
- DOAC (e.g. Apixaban) or unfractionated heparin (if bleeding risk, can be reversed easily)
- Massive PE –> IV unfractionated heparin for hours before and after thrombolysis e.g. IV alteplase
Scoring & Ix: Well’s score
- ≤4 = D-Dimer –sign raised–> CTPA
- >4 = CTPA
- ECG useful - sinus tachycardia, right heart strain, S1Q3T3
- NOTE: Troponin = useful markers for PE severity (indicates right heart strain)
Ongoing anticoagulation - DOAC/Warfarin
- Provoked - 3 months (SICC)
- Unprovoked - >6 months + cancer & thrombophilia testing
- Ix for cancer –> any Sx?
- If yes - CT TAP
- If no - FBC, U&E, LFTs, clotting, physical exam –> if concern –> CT TAP
- Consider thrombophilia screen if no cancer for anti-phospholipid syndrome (anticardiolipin, lupus anticoagulant, anti-beta-2-glycoprotein)
- Ix for cancer –> any Sx?
Bronchiectasis - definition? causes? presentation? Ix? Mx?
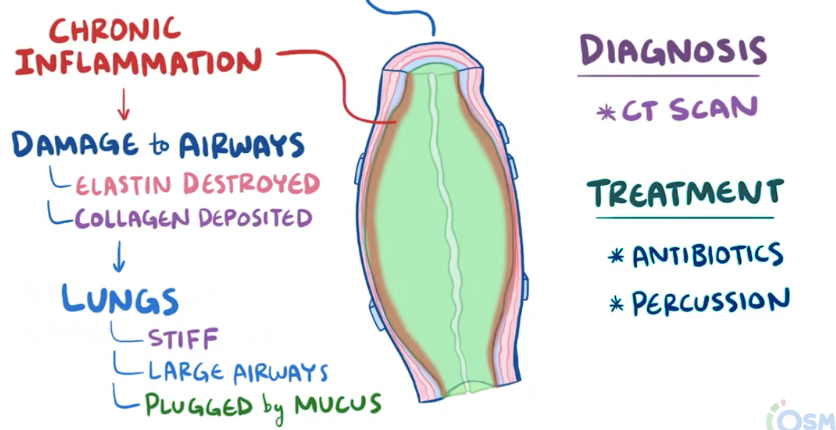
Def: obstructive lung disease characterised by permanent dilation of bronchi from the destruction of elastic & muscular components of the bronchial wall
- Results from diseases causing chronic inflammation:
- Primary ciliary dyskinesia - cilia don’t move –> mucus trapped in airways –> recurrent pneumonia –> chr inflammation
- Cystic fibrosis - mucus thick & sticky –> recurrent pneumonia –> chr inflammation
- Airway obstruction - tumour inside/outside airway or inhaled foreign body –> mucus can’t clear –> recurrent pneumonia –> chr inflammation
- NOTE: worse with certain infections e.g. aspergillosis –> hypersensitivity response
- Chr inflammation - has immune cells that release cytokines –> damage ciliated epithelial cells + destroys elastin –> airways dilated + clogged with mucus –> fibroblasts deposit collagen –> stiff lungs + mucus plug –> obstructive lung disease
Presentation:
- RFs: CF, PCD, congenital disorders of airway, host immunodef (incl. HIV), recurrent lung inf
- Less common - inhaled foreign body, connective tissue disease, IBD, alpha1-antitrypsin def
- Productive cough (large amounts of sputum) ± haemoptysis - worse lying flat/one side
- Dyspnoea (with increased severity)
- Fever (on exacerbation)
- Crackles, inspiratory squeaks & rhonchi, clubbing (from long-term hypoxia)
Ix: CXR (ring shadows, tramlines), high-res CT (signet ring sign), FBC + sputum culture & sensitivity (inf e.g. pseudomonas), pul function tests
- Genetic testing (for possible RF causes): serum alpha1-antitrypsin, serum Ig lvls (ID), specific IgE for Aspergillus, sweat Cl test (CF), rheumatoid factor (CTD), HIV test, nasal nitric oxide (PCD)
Mx:
- Conservative:
- Persuade to stop smoking
- Pul rehab
- Prick them - influenza + pneumococcal vaccine
- Psych issues
- Medical:
- Mucoactive agent (nebulised hypertonic saline)
- Inhaled bronchodilator (SABA/SAMA/LABA/LAMA) - ONLY If co-existing asthma/COPD
- Surgical: depending on primary cause e.g. IFB, tumour –> lobectomy/lung transplant
- Exacerbation: short-term abx (azithromycin)
Sarcoidosis - def? presentation? Ix? Mx?
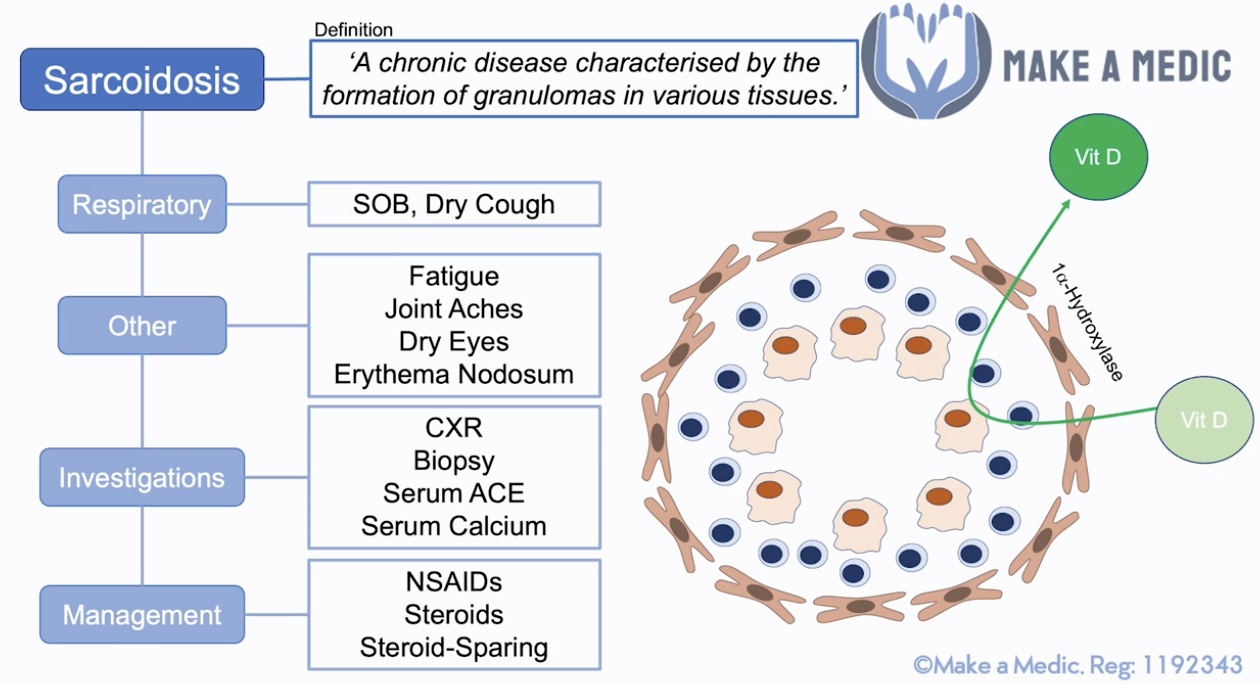
Def: a chronic multisystem disease characterized by the formation of non-caseating granulomas across various tissues
- Physiologically granulomas are supposed to form around insulting body e.g. infection but in sarcoidosis form for no apparent reason
Presentation:
- Profile - Afro-Caribbean, female, 20-40yrs
- Lungs - SoB, dry cough
- Skin - erythema nodosum & lupus pernio
- Other - dry eyes (uveitis, conjunctivitis, optic neuritis), polyarthralgia, fever/fatigue/weight loss, cardiac (cardiomyopathy, conduction defects), neuro (cranial nerve palsies)
- Lofgren’s syndrome = triad: erythema nodosum + bilateral hilar lymphadenopathy + polyarthralgia
Ix:
- Bloods:
- Serum ACE (high), serum soluble IL-2 receptor, ESR
- Serum Ca (activated macrophages in sarcoidosis prod 1alpha-hydroxylase –> excess activated vitamin D)
- CXR (bilateral hilar lymphadenopathy)
- Gold-standard: transbronchial biopsy (non-caseating granulomas)
Mx:
- Asymptomatic - NSAIDs/no Tx
- Symptomatic:
- Long-term steroids + bisphosphonates (osteoporosis protection)
- Steroid-sparing agents - Methotrexate/Azathioprine
Interstitial lung disease - causes? presentation? Ix? Mx? Prognosis?
Interstitial lung disease
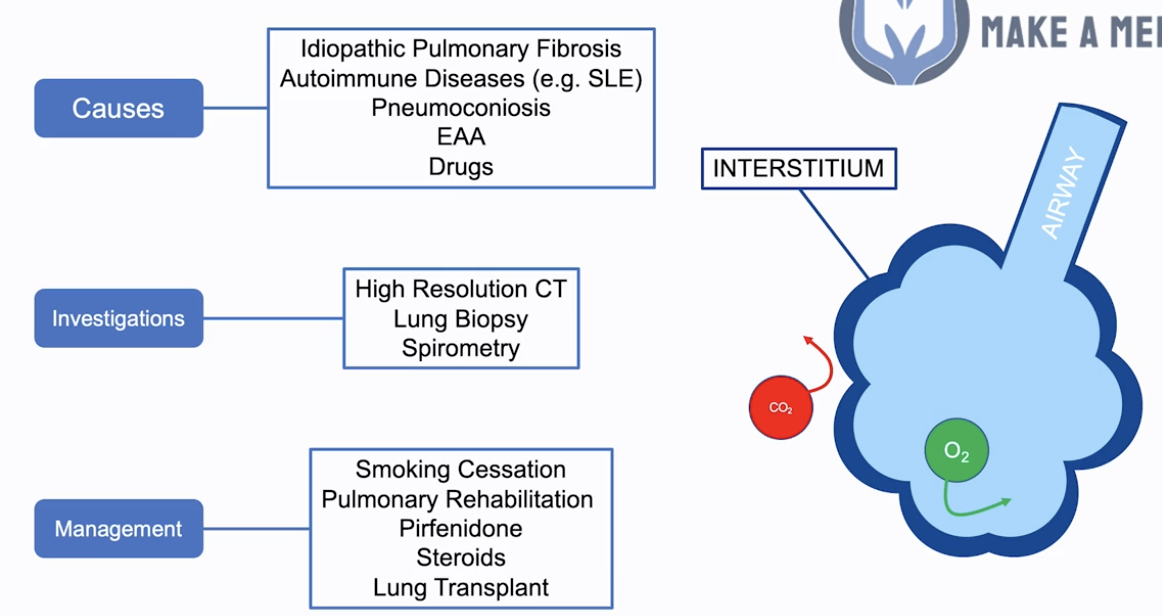
- Refers to the tissue the gasses pass through e.g. surface of alveoli –> reducing gas exchange
Causes:
- Upper zone fibrosis: PATEN (more occupational causes)
- Pneumoconiosis (not asbestosis) - caused by inorganic dust (e.g. soot)
- Aspergillosis/ABPA
- TB
- Extrinsic allergic alveolitis - caused by organic dust e.g. animal shedding
- Negative seroarthropathies
- Lower zone fibrosis: STAIR
- Sarcoidosis
- Toxins: B-MANS (Bleomycin, Methotrexate, Amiodarone, Nitrofurantoin, Sulfasalazine)
- Asbestosis
- Idiopathic pulmonary fibrosis
- Rheum: SLE, RhA etc
- Signs of conditions associated w/ pulmonary fibrosis:
- MCP swelling - RA
- Malar rash - SLE
- Kyphosis - Ank Spond (apical fibrosis)
- Lupus pernio - sarcoidosis
- Thick skin/’bird beak’ nose - systemic sclerosis
- Aphthous ulcers, abdo scars - Crohn’s
- Grey skin - amiodarone
Main Sx: progressive SOBOE, dry cough, fatigue, weight loss
Signs: find end-insp creps, clubbing
- Other: reduced chest expansion, normal/reduced percussion, normal vocal fremitus
Investigations: spirometry, high-res CT & lung biopsy
- Bedside: spirometry (low FEV1, low FVC, FEV1/FVC>0.8 = restrictive lung disease), ECG (right heart strain), drug review
- Bloods
- FBC, U&E, LFTs, CRP, ESR, ABG (T1RF)
- AI screen - Serology (CTD): ANA, RhF, anti-CCP
- Serum ACE for sarcoidosis
- TB testing
- Imaging
- CXR: reticulonodular shadowing (honeycombing) + rule out lung cancer
- High-res CT: more detailed view of alveolar structure –> ‘honeycombing’ + lung biopsy
- Echo (right heart strain/cor pulmonale)
- Invasive
- Bronchoscopy + lung biopsy (gold-standard)
Management:
- Conservative (4Ps):
- Persuade to stop smoking, reduce exposure (meds, EAA)
- Pul rehab
- Prick them - influenza + pneumococcal vaccine
- Psych issues
- Medical: anti-fibrotic e.g. pirfenidone +/- prednisolone ± O2 (if hypoxaemic)
- Surgical: lung transplant if severe deterioration/impairment/oxygen dependent
Prognosis: 3-4yrs post-Dx (no Mx increases survival)
Restrictive vs Obstructive lung conditions
Restrictive (belt around lungs) - reduced lung volume (restricted expansion) + FEV1/FVC ratio > 80% (normal/increased - from decrease in FVC)
- Poor breathing mechanics - Myasthenia gravis, scoliosis, obesity
- Interstitial lung disease - pulmonary fibrosis, sarcoidosis
Obstructive (hand choking airway) - increased lung volume (air trapped) + FEV1/FVC ratio < 80% (decreased - reduced expiratory volume)
- Airway obstruction (from inflammation of airways & problem exhaling) - Asthma, COPD (chronic bronchitis, emphysema), Bronchiectasis
What is FEV1 and FVC? WHat does FEV1/FVC ratio indicate?
FEV1 - total air expired forcibly in 1s (spirometry reading)
FVC - total air expired in a complete breath
FEV1/FVC ratio - decrease <80 indicates an obstructive condition
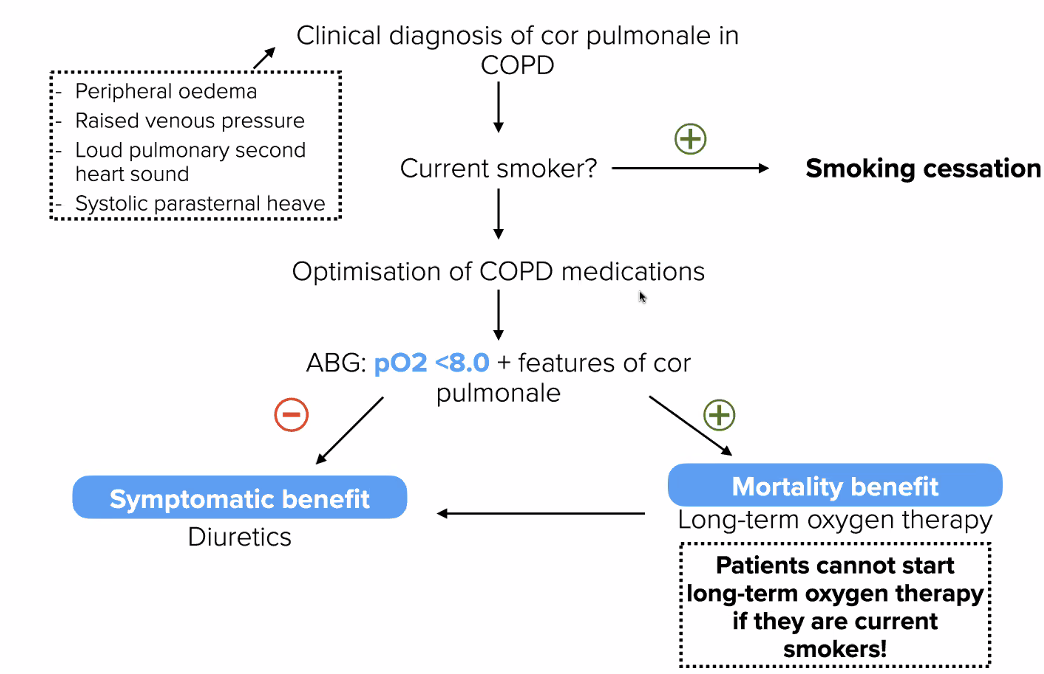
Cor Pulmonale Def? Dx? Mx?
Def? RHF secondary to lung disease
Dx: (clinical Dx –> confirm with ECHO)
- Peripheral oedema
- Raised JVP
- Loud pul second HS
- Sytolic parasternal heave
Mx:
- Smoking cessation
- Optimise COPD meds
- If PaO2 <8 + features of Cor Pulmonale –> long-term O2 therapy (not if smoker)
- If not above –> Sx control = diuretics
Chronic bronchitis vs emphysema?
Chr bronchitis - defined by clinical features (productive cough for ≥ 3 months/yr for ≥ 2 yrs - excess mucus & less mobile cilia) - airflow blocked by mucus –> decreased O2, increased CO2 –> cyanosis = BLUE BLOATER
Emphysema - defined by structural changes (enlarged air spaces –> reduced gas exchange) - breath slowly through pursed lips to increase airway pressure = prevent collapse –> PINK PUFFER
- Centriacinar - proximal alveoli affected, assoc w/ smoking, upper lobes
- Panacinar - entire alveoli affected, assoc w/ alpha1-antitrypsin def, lower lobes
- Paraseptal - distal alveoli affected, lung peripheries –> can rupture –> pneumothorax
NOTE: commonly co-exist
Both = COPD –> airway obstructed –> reduced FVC (air expired in complete breath) & very reduced FVC1 (air expired in 1s) –> low FVC1/FVC ratio (<0.7 for Dx)
- COPD –> vasoconstriction to redirect blood flow to well-oxygenated areas of the lungs –> if widespread –> pul HTN –> cor pulmonale
Pleural effusion - signs? causes? Ix? Mx?
Signs (if fluid > 300ml):
- Key:
- Stony dull in lung base
- If large: tracheal deviation away
- Reduced chest expansion
- Reduced breath sounds
- Reduced vocal fremitus
Causes:
- Transudative (<30g/L protein)
- HEART FAILURE
- Hypoalbuminaemia: liver disease, nephrotic syndrome, malabsorption
- Hypothyroidism
- Meig’s syndrome (benign ovarian tumor + ascites + pleural effusion)
- Exudative (>30g/L protein)
- Infection: PNEUMONIA, TB, subphrenic abscess
- Connective tissue disease; RA (also low glucose), SLE
- Neoplasia: lung cancer, mesothelioma, metastases
- Pancreatitis: high amylase in pleural fluid
- Pulmonary embolism
Ix:
- Bedside: obs, urinalysis for protein
- Bloods:
- ABG, BC
- FBC, U&E, LFTs, CRP
- Clotting (before needle aspiration), albumin (nephrotic syndrome)
- Mantoux/ELISPOT (TB)
- Imaging:
- CXR: meniscus sign, dense shadowing, pleural effusion if ≥300mL fluid
- CT chest - identify the cause
Management: US-guided pleural aspiration = thoracocentesis (21G needle, 50ml syringe) - above rib to avoid NV bundle
- LDH & protein in pleural fluid & serum + RBCs, WBCs, cytology, culture, pH & glucose of pleural fluid
- MC&S
- Biochemistry: PPALS
- Protein (also serum)
- pH
- Amylase
- LDH (also serum)
- Sugar (glucose)
- Cytology
- Immunology - if indicated (RF, ANA, complement)
- Findings:
- Protein > 30g/L: exudate
- Protein < 30g/L: transudate
- Protein 25-35g/L: use Light’s criteria. An exudate is likely if at least 1 of:
- Pleural protein/serum protein > 0.5
- Pleural LDH/serum LDH > 0.6
- Pleural LDH > 2/3 upper limits of normal serum LDH
- Tx cause e.g. abx for infection, furosemide for HF
- Management of recurrent pleural effusion
- Recurrent aspiration (thoracocentesis)
- Pleurodesis
- Indwelling pleural catheter
Pleural fluid features:
- Heavy blood staining - mesothelioma, TB, PE, trauma
- Purulent/turbid/cloudy - empyema secondary to bacterial pneumonia –> insert chest tube to allow drainage
- Milky - chylothorax via lymphatic obstruction secondary to malignancy
Pneumothorax - Def? RFs? Causes? Ix? Mx? How do you identify a Tension Pneumothorax?
Pneumothorax = accumulation of air in pleural space (subdivided into primary and secondary)
RFs: pre-existing lung disease, Marfan’s, RA, smoking
Causes: cystic pathology, parenchymal necrosis, iatrogenic, trauma
Ix: CXR
Mx:
- Primary (no pre-existing lung disease)
- <2cm (betw lung margin & chest wall), no SoB – observe 4-6hrs ± supplemental O2
- SoB/≥2cm – needle aspiration (16-18G) –> observe 4-6hrs
- Do NOT repeat needle aspiration x2
- Chest drain if above fails + ADMIT ± supplemental O2
- NOTE: correct clotting before inserting if possible
- Surgery
- Secondary (pre-existing lung disease) - ADMIT all secondary pneumothorax (for at least 24hrs observation)
- <1cm - high-flow O2 + ADMIT (24hrs observation)
- 1-2cm - needle aspiration (16-18G) –> high-flow O2 + ADMIT (24hrs observation)
- SoB/≥2cm/previous failed - chest drain + ADMIT ± supplemental O2
- Surgery
Tension pneumothorax = pushes away the trachea to the opposite side
- Non-traumatic:
- IMMEDIATE peri-arrest call (2222)
- Needle decompression = emergency Tx, 2nd ICS MCL (grey cannula) + high-flow O2
- Follow-up = ADMIT + chest drain
- Traumatic:
- Open thoracostomy
- Follow-up = ADMIT + chest drain
- Traumatic non-tension pneumothorax:
- High-flow O2 + ADMIT (24hrs observation)
- If open pneumothorax/penetrating chest wound –> occlusive dressing + observe
- Refer to thoracic surgeons - chest drain/thoracotomy
Location:
- Needle aspiration = 2nd ICS, MCL
- Chest drain = triangle of safety (axilla, pectoralis major, latissimus dorsi, 5th ICS) - 4th/5th ICS, MAL
Surgery:
- Open thoracotomy (or video-assisted thoracoscopic surgery = VATS)
- Follow-up surgery –> pleurodesis (mechanical abrasion/chemical irritation)
Causes of different ABGs? Resp/Met Acidosis/Alkalosis
Resp acidosis (not breathing out enough) - asthma, COPD, GBS
Resp alkalosis - pain, panic attack, PE, pneumothorax
Metabolic acidosis - DKA, LA, diarrhoea, renal failure
Metabolic alkalosis - vom/diarrhoea, diuretics (loop/thiazide), Conn’s syndrome, liver cirrhosis, HF
T1RF vs T2RF causes?
T1RF: low/normal CO2 –> pul oedema, ARDS, collapse
T2RF: high CO2 –> opiate OD, COPD, neuromusc disease
Respiratory causes of clubbing?
Lung cancer, bronchiectasis (& CF), pul fibrosis
NOT COPD (but if COPD is smoker with clubbing –> lung cancer)
Causes of lung consolidation? How do you know it is a consolidation?
Pus (infection)
Fluid (pul. oedema)
Cancer
Blood (pulm haemorrhage)
Protein (alveolar proteinosis = rare)
Consolidation has lung bronchograms
Allergic bronchopulmonary aspergillosis (ABPA) - def? presentation? Ix? Mx?
Def: results from T1 hypersensitivity reaction to Aspergillus spores (in exam often Hx of bronchiectasis + eosinophilia)
Presentation:
- SoB, wheeze (bronchoconstriction), productive cough, recurrent chest infections
- Coarse crepitations (if bronchiectasis)
- RFs: asthma, CF, atopy
Ix:
- Bedside - allergic skin-prick, spirometry, oxygen sats
- Bloods - eosinophilia, raised total IgE (>1000), Aspergillus +ve IgE & G
- Imaging - CXR, CT-chest (bronchiectasis, mucus plugging)
Mx:
- Conservative - chest physio (if features of bronchiectasis)
- Medical:
- Oral glucocorticoids (low-medium dose tapered over 3-12 months)
- 2nd line - Itraconazole
Cystic fibrosis - def? presentation? Ix? Mx? Prognosis?
Def: hereditary AR disorder caused by a mutation in CFTR gene characterised by the production of thick sticky mucus
Presentation:
- Commonly presents in infancy (Muconium ileus, genetic testing)
- Multi-systemic:
- Resp - recurrent chest inf
- GI - weight loss, malnutrition
- Endo - infertility, T1DM
- MSK - poor muscle mass
Ix:
- Bedside:
- Immunoreactive trypsinogen test (IRT) - newborn screening, not diagnostic
- Faecal elastase - abn pancreatic function
- Sweat test (+ve if Cl >60mmol/L; -ve <30)
- Sputum culture (pseudomonas)
- Pul funct tests (obstructive pattern)
- Lab:
- Genetic testing - CFTR gene mutations, ciliary genetic defects after (kartagener’s)
- Bloods - FBC, Ig, Aspergillus precipitins, nutrition status (vit, protein, Fe)
- Imaging:
- CXR/CT-chest - hyperinflation, bronchiectasis
- Abdo USS - fatty liver
Mx: MDT approach
- Conservative - airway clearance techniques (chest physio), GI nutritional support
- Medical:
- Nebs mucolytics (Dornase alfa, hypertonic saline)
- Bronchodilator therapy (SABA/LABA)
- Long-term abx (azithromycin)
- Surgical: lung transplant (if FEV1<30% predicted, refractory haemoptysis, failure of medical therapy)
Prognosis:
- No cure, mean survival = 40yrs (determinant of age is severity of lung disease)
- Death from chronic resp failure, cor pulmonale (from pul HTN), resp complications (pneumothorax, pneumonia)
Hypersensitivity pneumonitis aka extrinsic allergic alveolitis - Def? Ix? Mx & specific Mx of psittacosis?
Def: immune-mediated ILD precipitated by hypersensitivity to inhalation of micro-organisms
- Examples: Mushroom worker’s lung (thermactinomyces vulgaris), Malt-worker’s lung (Aspergillus clavatus)
- DDx: pulmonary fibrosis, pneumoconiosis
Ix:
- Bedside - O2 sats, inflammatory markers
- Imaging: CXR (90% have consolidation), CT chest (apical lung fibrosis)
- Confirmation with serology (as part of atypical pneumonia screen)
Mx:
- Conservative - avoidance
- Acute - pred tapered for 6 weeks
- Chronic - long-term low-dose pred
- Psittacosis: Tetracycline e.g. Doxy (2nd line - Macrolide e.g. erythromycin)
Lung cancer - epi? presentation? types? Ix? Mx?
Epi: Second most common cancer in UK
Presentation: chronic cough, haemoptysis, FLAWS
- Monophonic wheeze, pleural effusion signs (dull on percussion, reduced BS), cachexia, SVCO (face swelling & engorged veins in venal-caval distribution), hypertrophic pulmonary osteoarthropathy (HPOA)
- RFs: smoking, asbestos exposure, FHx
Types:
- Non-small cell lung cancer (MOST)
- Adenocarcinoma (MOST COMMON LC)
- Non-smoking women (40% cases)
- Squamous cell carcinoma (SCC)
- Affects large airways of lungs (central)
- Classically assoc w/ paraneoplastic hypercalcaemia, as tumour may release PTHrP
- 2nd most common in non-smokers
- Most common cause of Pancoast tumour
- Keratinization (keratin pearls)
- Large cell carcinomas (Dx of exclusion)
- Alveolar cell carcinoma = ++sputum
- Bronchial adenoma = mostly carcinoid
- Carcinoid syndrome - flushing, diarrhoea, episodes of dyspnoea
- Urinary 5-Hydroxyindoleacetic Acid (5-IAA) levels may be used to screen for carcinoid syndrome
- Adenocarcinoma (MOST COMMON LC)
- Small cell lung cancer (15%)
- Almost exclusively smokers
- Can be assoc w/ neuroendocrine syndrome (SIADH, Cushing’s)
- Early mets BUT chemo sensitive
Ix:
- Bloods - FBC, haematinics, Ca
- Imaging - CXR, CT chest (2WW referral), CT PET scan (staging, mets)
- Interventional if suspicious CXR:
- Endobronchial US-guided biopsy (EBUS) & biopsy
- Video-assisted Tracheostomy & Biopsy (VATS - BIOPSY) of accessible nodes
Mx:
- Conservative: lung cancer MDT
- Smoking cessation
- Psych support (McMillan Nurses, specialist lung cancer nurse involvement)
- Palliative care (if terminal, Sx control & planning)
- Medical:
- Systemic chemo - esp. for small cell lung cancer (chemosensitive)
- Adjuvant/radical radiotherapy
- Surgical - if NSCLC
- VATS-lobectomy
- Open lobectomy/Pneumonectomy
4Ps of respiratory conservative Mx?
Persuade to stop smoking
Pul rehab
Prick them - influenza + pneumococcal vaccine
Psych issues
Resp scars? Lobectomy/Pneumonectomy DDx? Presentation?
- Axillary thoracotomy scar - chest drains
- Postero/anterolateral thoracotomy scar - lobectomy, pneumonectomy & oesophageal surgery
- Radiotherapy-associated skin changes: dry, thickened, hypopigmented and telangiectasia
Lobectomy/pneumonectomy
- DDx:
- Lung cancer/mets
- Bronchiectasis, lung abscess(s), TB
- Sarcoidosis, COPD
- Presentation: dull percussion & absent breath sounds over affected area
- Complications:
- Fluid - pul oedema
- Bleed - haemothorax
- Inf - wound infection

























































































