What are the principles of haemostasis?
- Prevent bleeding
- Prevent unnecessary coagulation (allow blood to flow)
- Make clot
- Control clotting
- Break it down
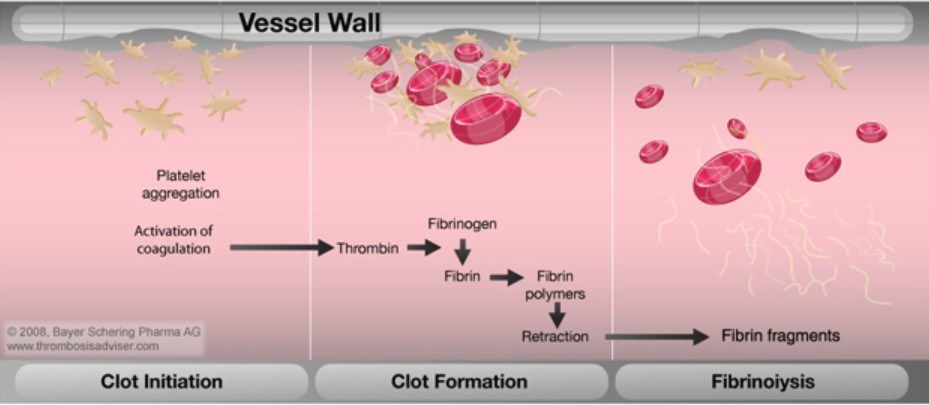
What are the essentials for haemostasis?
- Pump: heart, venous valves, calf pump
- Blood vessels are important
- Platelets
- Coagulation factors
- Anticoagulant factors
What are platelets?
Platelets are components of blood produced by megakaryocytes in the bone marrow and bud from cytoplasm
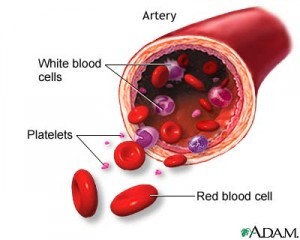
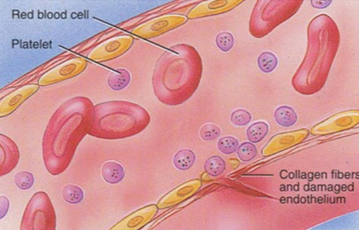
In three steps, outline platelet adhesion
⇒ Damage to the vessel wall
⇒ Exposure of underlying tissues
⇒ Platelets adhere to collagen via vWF/receptor
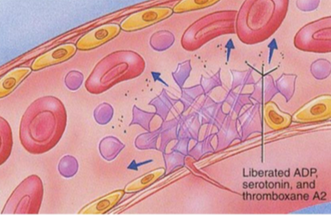
In 3 steps, outline platelet activation
⇒ Platelets secrete ADP, thromboxane, etc to become activated and activate other platelets
⇒ Involved in activation of the clotting cascade
⇒ Provide some coagulation factors by secretion from internal stores
What does platelet aggregation involve?
Platelet aggregation involves the cross linking of platelets to form a platelet plug
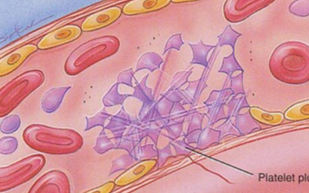
Identify 6 mediating factors in haemostasis
- Von willebrand factor
- Fibrinogen
- Collagen
- ADP
- Thromboxane
- Thrombin
What is the clotting cascade?
- The clotting cascade is a controlled amplification system involving the activation of precursor proteins to generate thrombin (IIa)
- Thrombin converts soluble fibrinogen into insoluble fibrin
- Fibrin enmeshes the initial platelet plug to make stable clot
Describe the control of the clotting cascade
- Natural anticoagulants inhibit activation
- Clot destroying proteins are activated by the clotting cascade
Identify some coagulation factors
- Fibrinogen
- Prothrombin
- Factor V, VII - XIII
- Tissue factor
Identify some natural anticoagulants
- Protein C
- Protein S
- Antithrombin
- Tissue factor pathway inhibitor
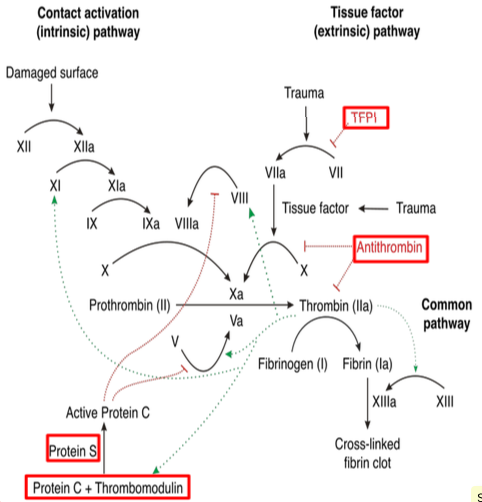
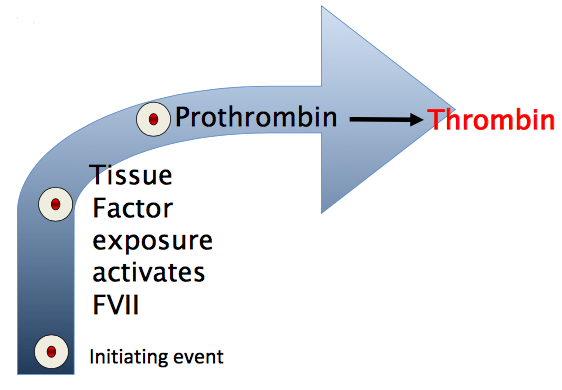
Describe the process of initiation in the clotting cascade?
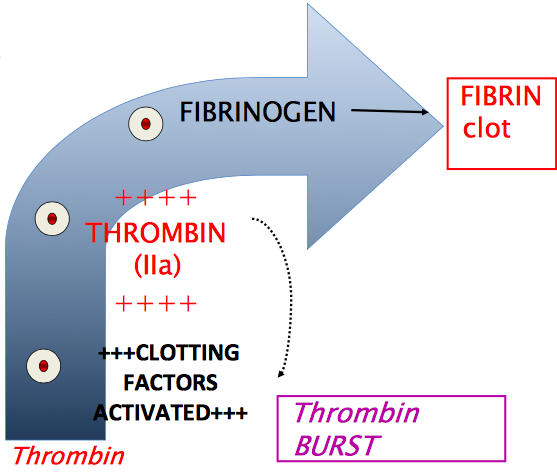
Describe the process of amplification in the clotting cascade?
What is the role of Von Willebrand Factor?
VWF carries factor VIII and mediates platelet adhesion to the endothelium
Describe changes in the vessel wall during blood clotting
- Vasoconstriction
- Production of vWF (platelet adhesion, carrier of Factor 8)
- Exposure of collagen and tissue factor initiates activation of clotting factors
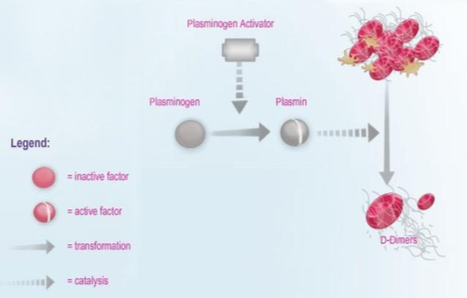
What is fibrinolysis?
Fibrinolysis is a process which prevents blood clots from growing and becoming problematic by breaking down fibrin clot, a product of coagulation
What is the clinical relevance of understanding haemostasis?
- Bleeding disorders
- Arterial thrombotic disorders
- Venous thrombotic disorders
- Abnormal blood test results
- Drug therapy for pro- or anti-thrombotic purposes
What are bleeding disorders?
Bleeding disorders are inherited/acquired conditions arising due to abnormality in the vessel wall, platelets or coagulation factors
Identify two congenital coagulation factor disorders
- Haemophilia A
- Haemophilia B
In coagulation factor disorders, clinical severity correlates with extent of deficiency.
Identify 5 clinical presentations of these disorders
- Muscle haematomas
- Recurrent haemarthroses
- Joint pain and deformity
- Prolonged bleeding (after dental extraction, operation, trauma)
- Intracerebral haemorrhage
What is Haemophilia A?
- Haemophilia A is an X-linked recessive disorder due to a congenital lack of factor VIII
- It can be mild/moderate/severe depending on amount of factor VIII present and is treated with recombinant factor VIII or DDAVP
What is Haemophilia B?
Haemophilia B is an X-linked recessive disorder due to the congenital reduction in factor IX
Identify two acquired coagulation factor disorders
- Liver disease
- Vitamin K deficiency
What is Von Willebrand’s Disease?
- Von Willebrand’s disease is a relatively common autosomal dominant disease often due to a reduction in vWF production
- There is abnormal platelet adhesion to the blood vessel wall as well as reduced FVIII amount/activiy




