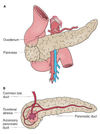
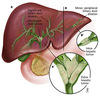
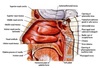
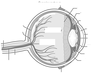
Pathophysiology of acute pancreatitis
Pancreatic enzymes released and activated-> multi stage process
Oedema + fluid shift + vomiting —> hypovolaemic shock
Enzymes—-> autodigestion
Vessel autodigestion—> retroperitoneal haemorrhage
Inflammation—–> pancreatic necrosis
Implications of pancreatic necrosis
Super-added infection in 50% of patients with necrosis
Epidemiology of acute pancreatitis
1% of surgical admissions
4th and 5th decades
10% mortality
Aetiology of pancreatitis
Idiopathic (?microstones)
Gallstones
Ethanol
Trauma
Steroids
Mumps (+ other infections e.g. Coxsackie B)
Autoimmune: PAN
Scorpion (Trinidadian)
Hyperlipidaemia, Hypercalcaemia, Hypothermia
ERCP
Drugs: thiazides, azathioprine
Severe epigastric pain radiating to the back
May be relieved by sitting forward
Vomiting
?Acute pancreatitis
Raised HR, Raised RR
Fever
Hypovolaemia—> shock
Epigastric tenderness
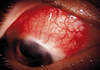
Jaundice
Ileus (absent bowel sounds)
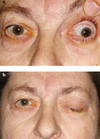
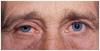
Ecchymoses
?Acute pancreatitis
Grey turner’s
Flank ecchymoses
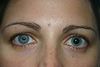
Cullen’s
Periumbilical ecchymosis (tracks up falciform)

Grey Turner’s sign
Flank ecchymosis
Acute pancreatitis

Cullens sign
Peri-umbilical ecchymosis
Acute pancreatitis
Ddx for acute pancreatitis
Perforated duodenal ulcer
Mesenteric infarction
MI
Difference between Glasgow and Ranson criteria
Glasgow criteria valid for EtOH and gallstones
whereas Ranson only applicable to Etoh and can only be fully applied after 48 hours
Components of modified glasgow score
PANCREAS
PaO2 <8kPA
Age >55
Neutrophils >15 x 10^9
Ca <2mM
Renal function, U >16mM
Enzymes: LDH >600iu/L, AST >200 iu/L
Albumin <32 g/L
Sugar >10mM
Modified Glasgow criteria cut offs
1= mild
2= moderate
3= severe
Ix in acute pancreatitis and what would be seen
Bloods
Bloods:
FBC- raised WCC
Raised amylase (>1000/3x ULN) and raised lipase
U+Es: dehydration and renal failure
LFTs: cholestatic picture, raised AST, raised LDH
Ca: reduced
Glucose: raised
CRP: monitor progress, >150 after 48 hours= severe
ABG: reduecd O2 suggests ARDS
Ix in acute pancreatitis and what would be seen
Urine
Glucose
Raised conjugated bilirubin
Reduced urobiliongen
Ix in acute pancreatitis and what would be seen
Imaging
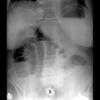
CXR: ARDS, exclude perforated DU
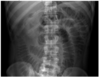
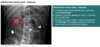
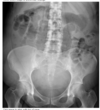
AXR: sentinel loop, pancreatic calcification
USS: gallstones and dilated ducts, inflammation
Contrast CT: Balthazar severity score
Cut offs for amylase in acute pancreatitis
>1000/ 3xULN
Difference between lipase and amylase
Lipase is more sensitive and speciic
CRP >150 after 48hrs in acute pancreatitis
Severe
What is used to grade severity of pancreatitis on CT?
Balthazar severity score
Complications of acute pancreatitis
Early: systemic
Respiratory: ARDS, pleural effusion
Shock: hypovolaemic or septic
Renal failure
DIC
Metabolic: hypocalcaemia, raised glucose, metabolic acidosis
Complications of acute pancreatitis
Late (>1w)
Pancreatic necrosis
Pancreatic infection
Pancreatic abscess: may form in pseudocyst or in pancreas, may require open or percutaenous drainage
Bleeding: e.g. from splenic artery, may require embolisation
Thrombosis: splenic artery, GDA or colic branches of SMA, may subsequently lead to bowel necrosis. Portal vein, may subsequently lead to portal HTN
Fistula formation: pancreato-cutaneous due to skin breakdown
Def: pancreatic pseudocyst
Collection of pancreatic fluid in the lesser sac, surrounded by granulation tissue
Occurs in 20% especially in EtOHic pancreatitis