LO
- To understand how T cells recognise antigens and how the T cell receptor is generated
- To know that T cell activation involved 3 signals: antigen, co-stimulation, and cytokines
- To know that multiple subsets of CD4 T cells exist and perform different role during immune responses
- To know the mechanism by which cytotoxic CD8 T cells kill infected cells
What are the two main types of T cells?
T helper cells= CD4
T cytotoxic cells= CD8
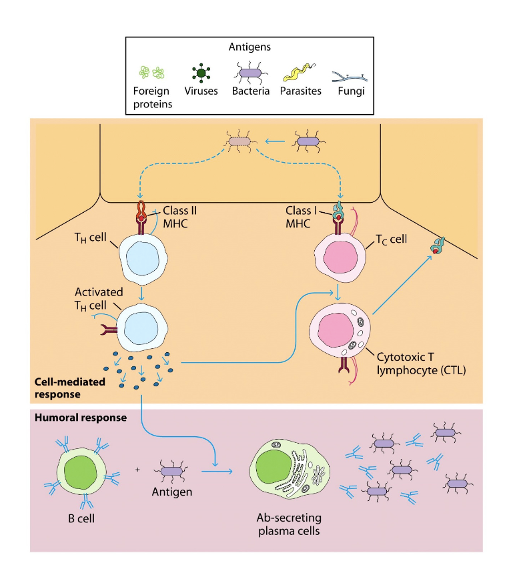
Tell me about the T cells and their respective MHC molecules
MHC molecules are antigen presenting cells (APC)
There are two types of MHC; MHCI and MHCII
MHCI present peptides which are recognised by CD8 cytotoxic T cells
MHCII present peptides which activate CD4 helper T cells
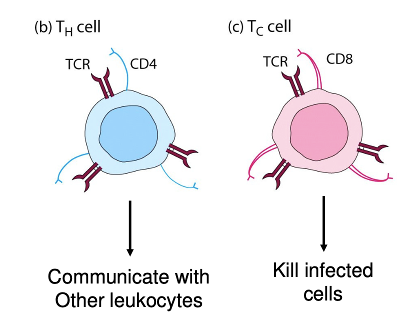
Whats the role of the CD4 and CD8 cells?
Soluble mediators communicate with other cells (CD4)
CD8 also involved in antigen recognition and cell-cell communication. It kills infected cells which express things they don’t usually express via peptide fragments on APC
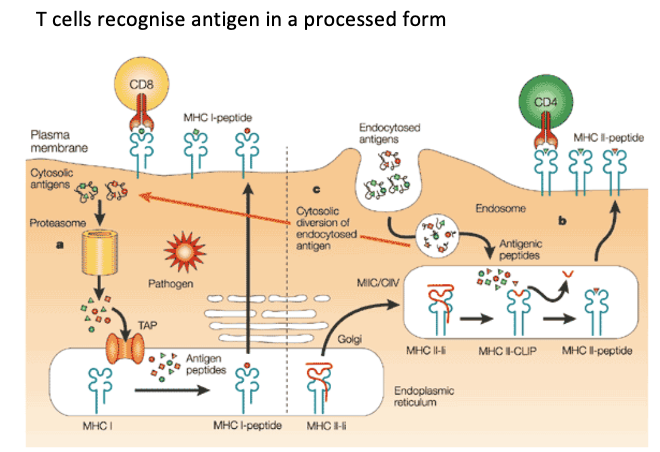
Tell me the steps to how the CD4 T cells work
CD4
antigens recognise MHCII, antigens come from the extracellular environment, antigens get taken up by APC, macrophages, dendritic cells, and B cells are the APC. Degradation in the vesicles within cells which leads to peptide production. These peptides are loaded onto the now MHC molecules being made in the cell.
What are the three APC?
Macrophages
Dendritic cells
B cells
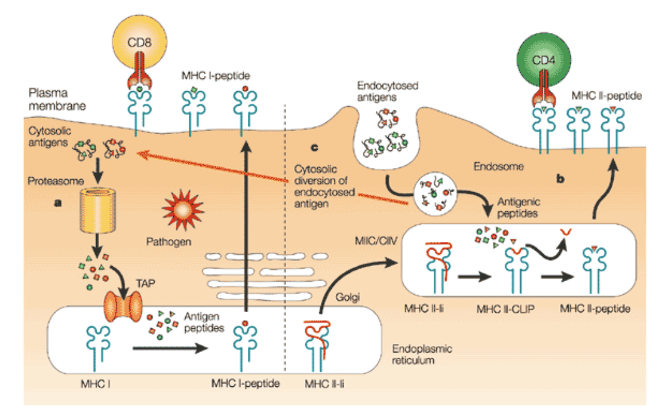
What are the stages to how CD8 cells work and specifically their two mechanisms
CD8
start of immune response is priming and this requires a professional APC. A dendritic cell needs to prime CD8. 2 ways.
1) pathogen can infect dendritic cell, DC starts to produce virus and viral proteins, these proteins are processed via proteolytic complex called proteasome which releases peptides which are transported to ER where they are loaded on MHCI, these MHCI are then transported to cell surface where they are recognised by CD8 T cells
2) cross presentation pathway- process takes place in professional APC, dendritic cell is the most efficient cross presentation cell because these cells can cross present antigens. Antigen present outside of DC –> taken up by DC –> degradation takes place in endosome and lysosome –> some peptides enter cytoplasm –> undergo same process as when protein is translated in cytoplasm of cells like in 1) where they go on to be loaded onto MHC molecules (involves exogenous uptake of pathogens into lysosome and endosome)
Where are the T cells developed?
Precursor cells are produced in the bone marrow, they then migrate to the thymus where they develop into T cellls
What determines whether a cell is a T cell
The expression of TCR (which recognise MHC) determines a T cell
The process in how TCR are generated are random and are not antigen determined
Tell me about the production of new T cells
Production of new T cells occurs in the foetus and the juvenile but slows down in the adult
The thymus begins to shrink after puberty
What does T cell development in the thymus involve?
Rearrangement of the T cell receptor genes to generate the diversity in the T cell repertoire (with intermediate affinity to be remaining)
Selection/ survival of T cells with a T cell receptor capable of recognised self MHC- positive selection
Removal of those T cells which express T cell receptors that bind strongly to self-antigens- negative selection
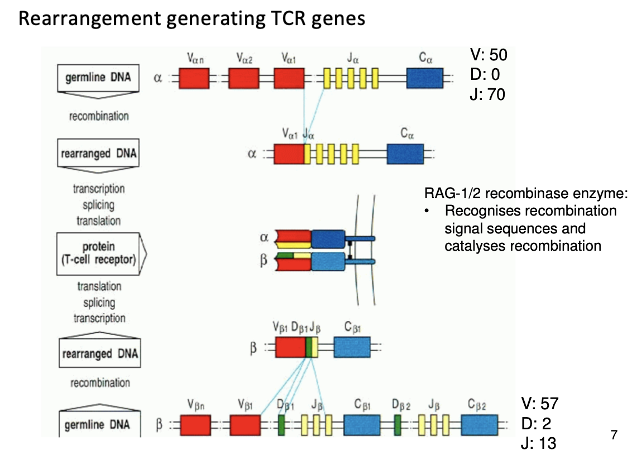
Tell me about the rearrangmenet which helps to generate the TCR genes
- TCR is comprised of alpha and beta chain
- Blue part shown in diagram is constant. These are short and don’t extend too far into cytoplasm.
- The alpha and beta heterodimer is connect via a disulphide bridge
- Variable domains recognise peptide MHC
- In alpha chain: variable domain consists of V genes (we have about 50), the J gene (we have about 70), there’s recombination signals surrounding these genes which allow enzymes to bind to recombination sequences and allow recombination of V with J, leads to juxta positioning of gene which means an V and J gene are next to one another
- In the beta chain: more diversity, there’s recombination as has V, D and J genes.
- Diversity from multi segment gene that encode antibody variable chain (recombination)
- Also get diversity from somatic hypermutation (this is not present in…)
- Can get additional AA in the junctions which are not encoded in the genome (additional diversity in this process)
- Diversity= recombination, somatic hypermutation and addition of extra AA
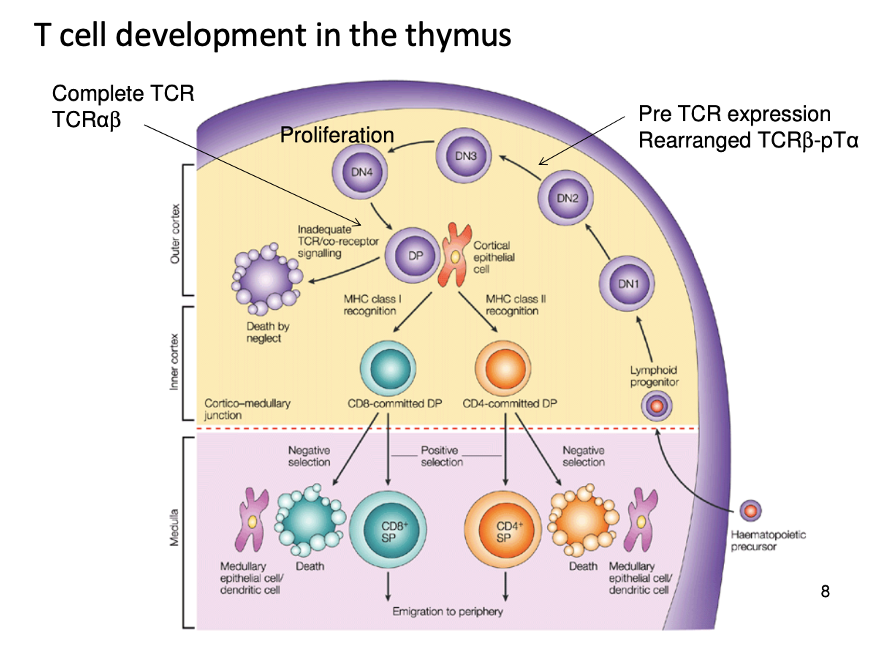
Explain T cell development in the thymus and how they differentiate
- precursors from bone marrow differentiate once in thymus
- DN stands for double negative as they don’t express CD4/8
- 4 stages of differentiation
- Key stages between D2 and 3 when the TCR starts to be expressed
- Pre-alpha associated with beta chain to maintain Beta chain on cell surface
- Allelic exclusion: once have one receptor on cell surface of T cell, then this cell doesn’t go through further recombination steps, ensures only one TCR per T cell
- B chain gets made first before alpha so needs to associate with pre-alpha chain
- Then starts producing the alpha chain and the two chains can come together
- Once D1–> D4 has occurred the cell then starts expressing both CD4 and CD8 cells (double positive cell, DP)
- TCR which bind MHCI down regulate CD4 to maintain CD8
- TCR which bind MHCII down regulate CD8 to maintain CD4
- This way the cells become single positive cells (CD4+ SP and CD8+ SP)
- Get positive selection at this process. If the cells are unable to recognise MHC, then they die
- In medulla (medulla epithelial cells or DC), go through negative selection process if recognise self-antigen
Tell me the first steps in TCR signalling
A single TCR/CD3 complex has 10 ITAM motifs (immune receptor tyrosine based motifs)
Phosphorylation of these ITAMs is a crucial first step in signalling
All occurs in periphery (secondary lymphoid organs)
This is performed by Src family kinases (e.g., Lck)
ITAM YXXLX7-11YXXL immunereceptor Tyrosine-based activation motif
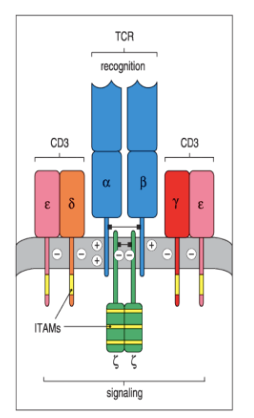
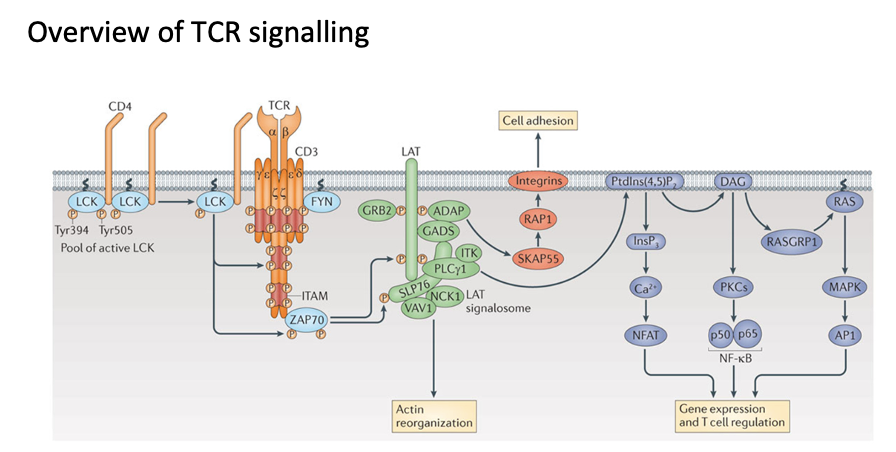
Rough overview of TCR signalling
- Proliferation, secretion of cytokines, expression of cytotoxic molecules
- Phosphates signify the activation of T cells.
- Lck is the enzyme that is required for phosphorylation of ITAM residues
- Antigen independent way is how the CD4 and CD8 co-receptor interact with peptides
- Lck brought near TCR cytoplasmic domains
How are T cells initiated for a response?
- T cells migrate from the thymus to the blood, lymph nodes and spleen
- Antigen is most often encountered in the lymph nodes/ spleen
- Processes antigen is recognised by a specific T cell- triggers a signalling cascade
- The T cell proliferates extensively, and its progeny differentiate into effector cells (CD4 cells produce cytokine and CD8 T cells become killers)
- Effector T cells migrate to the site of infection
- A small number of cells differentiate into memory T cells
E.g., infection with EBV, about 40-50% recognise one pathogen, infection with corona, doesn’t lead to that many T cells expanding
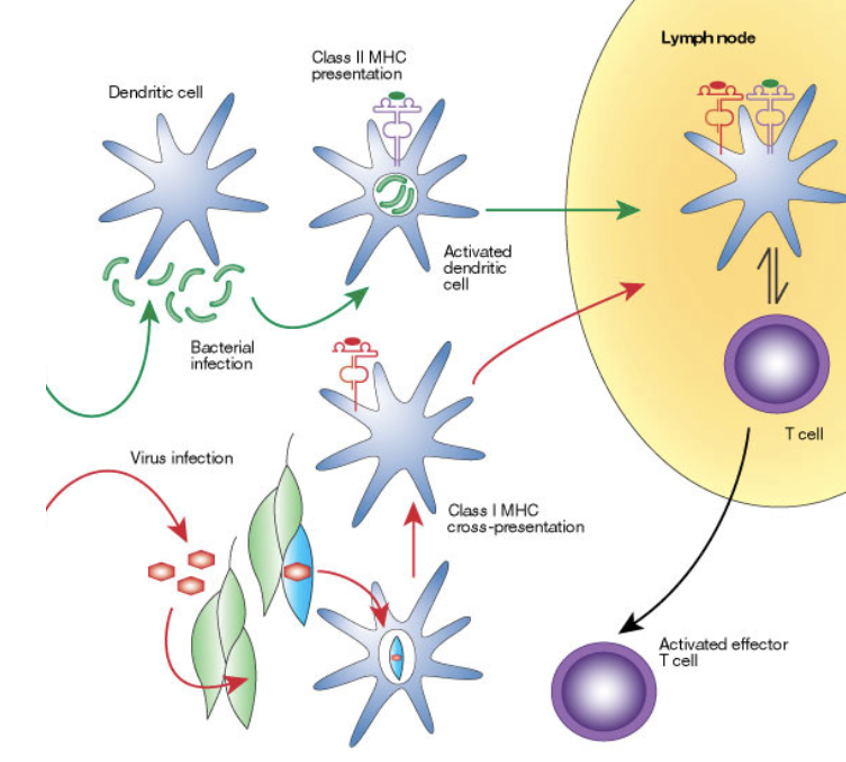
What do dendritic cells transport?
Dendritic cells transport processed antigen for presentation to T cells
As shown in the diagram, the leaf like cells represent dying cells and some dying cells may contain virus which then is taken up by DC for APC
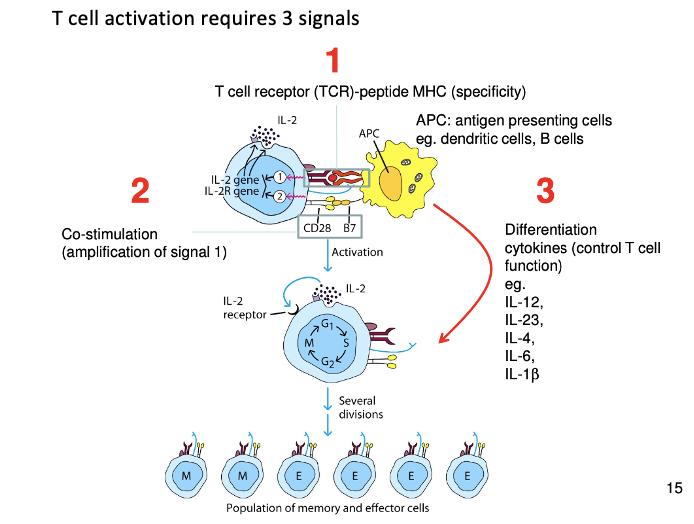
What are the signals that are involved in T cell activation?
Signal 1: peptide/ MHC: TCR
Signal 2: co-stimulation (induced by innate immunity)- antigen independent, signal 1 + signal 2 leads to expansion of T cells
Signal 3: cytokines (induced by innate immunity)- help to differentiate the naïve T cells
What is required for a successful T cell response?
Dendritic cell activation
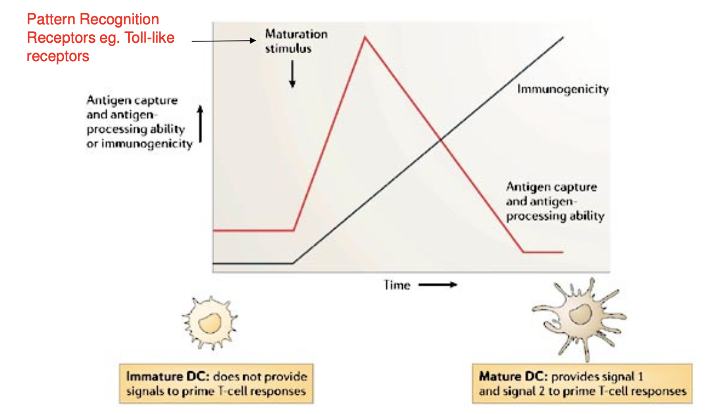
Tell me about dendritic cell maturation
DC present antigens to T cells
In an immature state, then become mature by responding to innate signals
Immatures are good are taking up pathogens for phagocytosis
Once mature, they can’t take up more antigens for, instead they become better at stimulating T cells and become more immunogenic
Explain how the activating signals of the T cells work together
1 cannot proliferate very well only once 1 and 2
2 is delivered by signal CD28 which binds to B7 which is expressed on APC
B7 is upregulated because of the innate immune system
IL-2 and upregulation of IL-2R are due to signal 1 and 2
Differentiation cytokines (3), these controls T cell function. List of some of the cytokines produced are above.
Differentiate into effector cell which can mediate the anti-viral immune response
Tell me about co-stimulation and the families which are involved in this
Also known as signal 2
Synergise with TCR signal 1 signalling
Required for most T cell responses in vivo
Two major families:
- Ig superfamily: CD28 (first co-stimulatory molecule discovered) and ICOS
- TNFR superfamily: CD27, OX40, 4-1 BB
Tell me about CD28 and its main roles, its ligands and explain what could happen if one is deficient in CD28
Main role: proliferation, survival, and IL-2 production
Ligands: CD80 and CD86 expressed constitutively at low levels but rapidly induced on APCs
CD28 deficient mice: defects in CD4 and CD8 responses to microbes (CD4>CD8). Defect in CD4 T cell help for B cells (germinal centre, Ab class switching)
Tell me about ICOS and ICOSL
ICOS
Main role: generation of Tfh cells that regulate germinal centre reactions and humoral immunity
ICOS deficient humans and mice: few Tfh and defect in germinal centre formation, Ab class switching and memory B cells