What does the thyrocervical branch into?
- Transverse scapular
- Anterior jugular vien and arch
- External jugular
What is the primary cause of upper extremity DVT’s?
IV’s and central lines.
What is the second cause of a DVT?
Effort thrombosis
What are some effort thrombosis?
- Paget-von Shrötters syndrome
- Thoracic Outlet Compression (TOC) (1-2 % of patients)
What are the upper extremty causes for a DVT?
- IV’s and central catheters
- Effort thrombosis
- Tumors
- IV drug abuse
- Post-op complications
What is the physical assessment for edema?
- Entire ARM – (Where is obstruction?)
- SVC SYNDROME (What is location of edema?)
- AT IV SITE – Infiltration
- HAND EDEMA = Lymphadema
What is the physical assesment for pain?
- Heaviness / ache typical for DVT
- Hand pain – Arterial embolus?
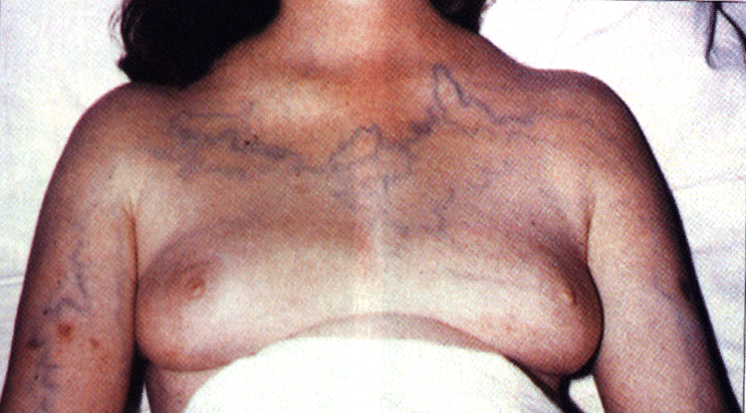
What SVC syndrome?
The superior vena cava is obstructed which causes venous collaterals.
What is a portacatheter?
A long-term central venous catheter with subcutaneous ports.
A hickman catheter is usually placed where?
In the SVC thorugh the subclavian vein.
What is a PICC line?
PERIPHERALLY INSERTED CENTRAL CATHETER
What happens after a PICC line is removed?
A fibrin sheath often remains in the vein.
What is a fibrin sheath made of?
It is essentially a cast of the line made from deposits of fibrin from the circulating blood
How does fibrin sheath form?
◦A venous catheter is a foreign substance.
◦Plasma proteins (fibrin and fibronectin) coat the catheter’s surface.
◦This promotes the adherence of blood platelets and bacteria.
◦Staph. bacteria adheres to the fibronectin which stimulates platelet activation and the compliment/ coagulation cascade.
◦The end result is either a fibrin sheath or thrombus.
What are the complications of fibrin sheath?
◦The fibrin sheath forms an adhesive “sock” around the end and sides of the catheter.
◦The substance surrounding the catheter is thick and glue-like and difficult to remove.
◦It can form within 24hrs after placement and most CVC’s are encased by 5-7 days.
◦Withdrawal of blood is impeded if the end of the catheter is covered.
◦Infusions must escape through the sheath possibly causing thrombus formation.
When taking down a patients history, what are some important things to ask?
◦Introductions/Ask the patient why he/she is being tested.
◦Symptoms? Look at order/ indications
◦History of DVT?
◦Trauma or surgery?
◦Central lines- current or previous
◦IV’s?
◦Dialysis access complications?
◦Recent weight lifting? Arm exercise?
◦Does the history match any of Virchow’s triad?
How should a patient be position for a scan for the BCV, SCV, IJV?
Supine.
What are the symptoms of PE?
- Swelling
- Pain
- Inflammation at IV site
- Preop
- Vein mapping for le bpg or cabg
- Vein mapping for dialysis access
- Malfunctioning central line
If you start to scan in the IJV mid neck in trans, where should you move?
Scan distally and proximally.
How should you point the probe in order to see the BCV?
Point the probe down.
How should you scan the SCV?
Turn probe at clavicle, pointing end towards the armpit, to line up with the proximal sublavian vein in long view.
How will the proximal SCV be displayed on the screen?
Prox. SCV will be horizontal on scnreen with bright echo below which is the pleura.
What is the pleura?
One of the two membranes around the lungs.
What are the two types of pleura?
Visceral and parietal.


