If a woman has a urine dipstick test and tests positive for leukocyte esterase but negative for nitrates, what does this mean?
- UTI is caused by an organism that is not gram negative
- Usually Staphylococcus saprophyticus
(honeymoon cystitis)
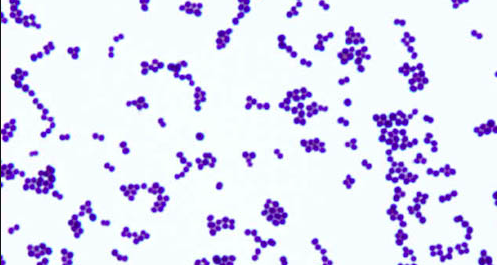
What is the most common organism causing a catheter acquired UTI?
Staph epidermidis
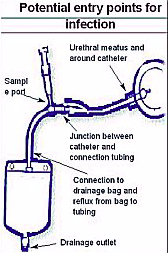
What is the most common presenting complaint of a male with a UTI?
Dysuria
Why may a patient have ankle oedema and high serum creatinine with SLE?
Oedema: nephrotic syndrome, loss of oncotic pressure in the blood as hypoalbuminemia so loss of fluid to interstitium
Creatinine: immune deposits in the blood causin ischameia and cell death of muscles
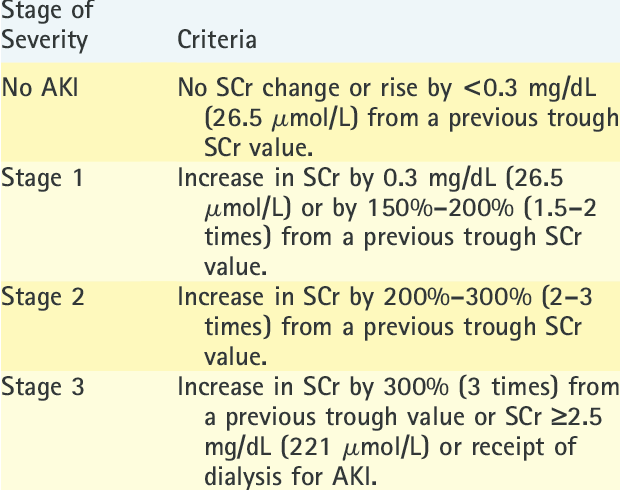
What is the definition of an AKI?
- Decline in the GFR/renal function over a short period of time with the decline in GFR being measured by increase in serum creatinine
- 3 stages
- eGFR should be >90ml/min

How much of the cardiac output does the kidney recieve?
25%
What are the some of the criteria used by NICE for an AKI?
- Rise in serum creatinine of 26umol/L or greater within 48 hours
- 50% or greater rise in serum creatinine within past 7 days
- Fall in urine output to less than 0.5mL/Kg for 6 hours in adults and 8 hours in children
- 25% or greater fall in eGFR in children in the past 7 days
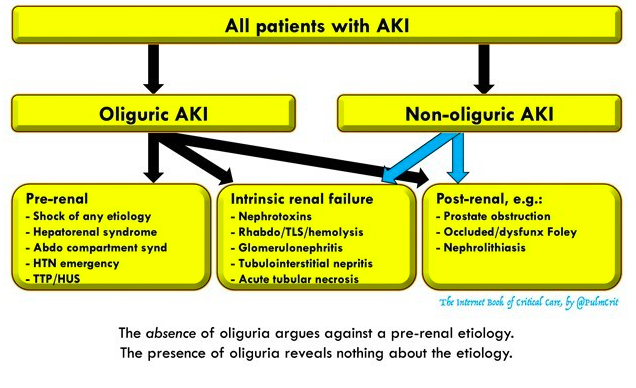
What are the two types of AKI?
- Oliguric or non-oliguric
- Oliguria: less than 500ml of urine a day or less than 20ml an hour
- Anuria less than 100ml urine a day. Usually indicates blockage of urine flow and severe damage.
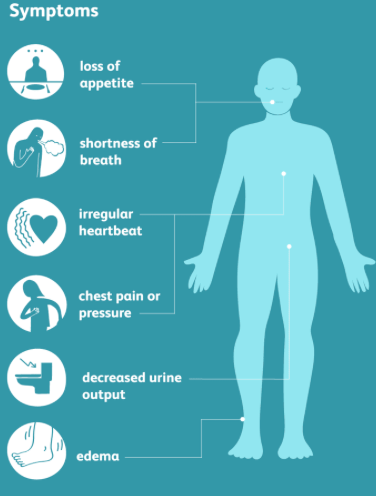
What is uraemia?
Signs anf symptoms of kidney failure characterised by a raised level of urea in the blood
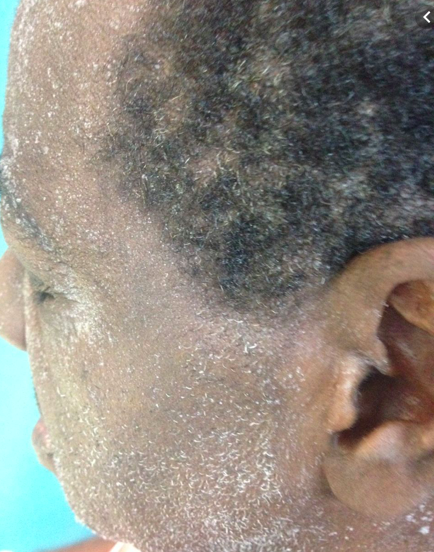
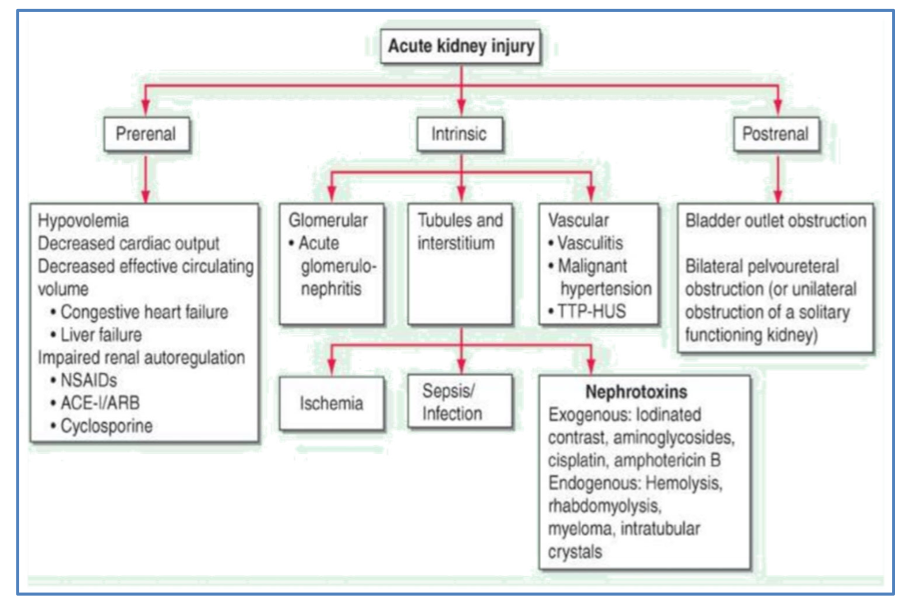
What are the three different classifications of causes of AKI and some examples of each?
- Prerenal: decreased renal perfusion, is reversible if recognised quickly. 85% of AKIs, e.g sepsis, hypovolaemia
- Renal: usually acute tubular injury (ATI), drugs, rhabdomyolysis, myeloma
- Post renal: obstruction to urine flow in one of three places. 10-15% of AKIs
How can pre-renal AKI become intrinsic AKI?
- If pre-renal AKI not identified quickly cells are starved of oxygen and the cells with highest metabolic requirements are at risk, proximal tubules
- This can then cause ATI to occur
How can we treat AKI?
- Depends on cause e.g pre-renal need to restore volume or pump, postrenal need to clear obstruction
- Correctly manage fluid and electrolytes
- ATI is supportive, need to avoid nephrotoxins, maintain good kidney perfusion, restrict solutes like potassium, provide nutritional support
- Dialysis if cannot conrol electrolytes or maintain acid-base balance

How does the treatment for intrinsic AKI differ to pre/post renal AKI?
Intrinsic treatment often requires immunosuppressants but the others require supportive treatment
What is the first test that should be done when you suspect an AKI?
Urine dipstick
What is fibromuscular dysplasian?
- Non-atherosclerotic, non inflammatory disease of the blood vessels that causes abnormal growth within the wall of an artery, usually in renal and carotid arteries
- Causes renal artery stenosis so may be hypertension and poorly perfused kidney
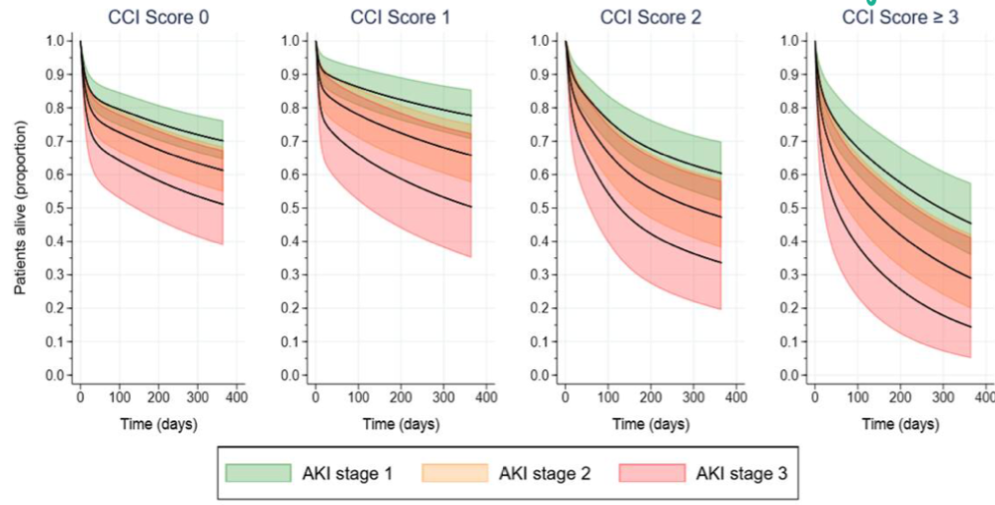
What is the mortality of AKI?
25% TO 50% depending on co-morbidities
What are the stages of CKD?

What are some of the causes of CKD?

What are some drugs that can cause intrinsic AKI?
- Nephrotoxi antibiotics like gentamicin
- ACE inhibitors
- NSAIDs
What will happen to a patients serum urea in the following scenarios:
- Upper GI bleed?
- Volume depletion?
- Malnutrition?
- Bleed: raised urea as blood Hb is digested so more urea. If someone has raised urea but not raised creatinine suspect this
- Volume: increase as more ADH so more UT1
- Malnutrition: decrease due to enzymes in the urea cycle
What is the definition of acute tubular injury and what are some risk factors for this?
Damage to kidney tubule cells due to ischaemia or nephrotoxic drugs
Risk factors are anything causing renal failure

What is this patient’s acid base status and why do they have a low bicarbonate level?
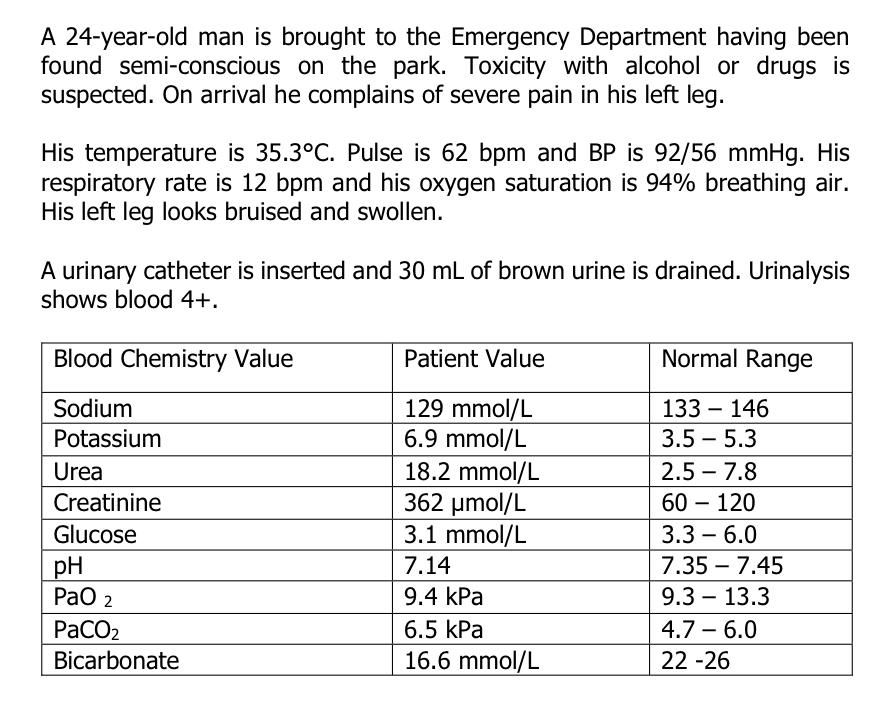
- Mixed metabolic and respiratory acidosis
- Low bicarb as ketoacidosis from alcohol and lactic acidosis from laying on the ground so bicarb reacts with this
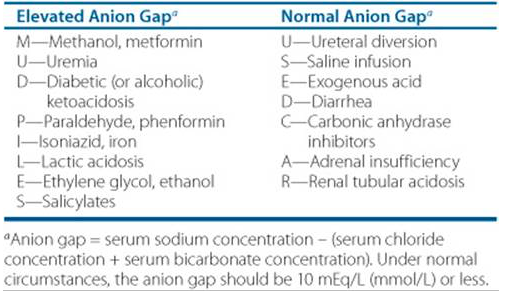
What are the causes of elevated anion gap metabolic acidosis?
- High gap: often due to lactic acidosis, ketoacidosis and methanol intake which react with bicarbonate to produce another anion
- Normal gap: low bicarb so chloride increases to compensate
https://www.youtube.com/watch?v=7657dEp51so
What has caused this lady’s AKI and are her serum sodium and potassium what we expect?
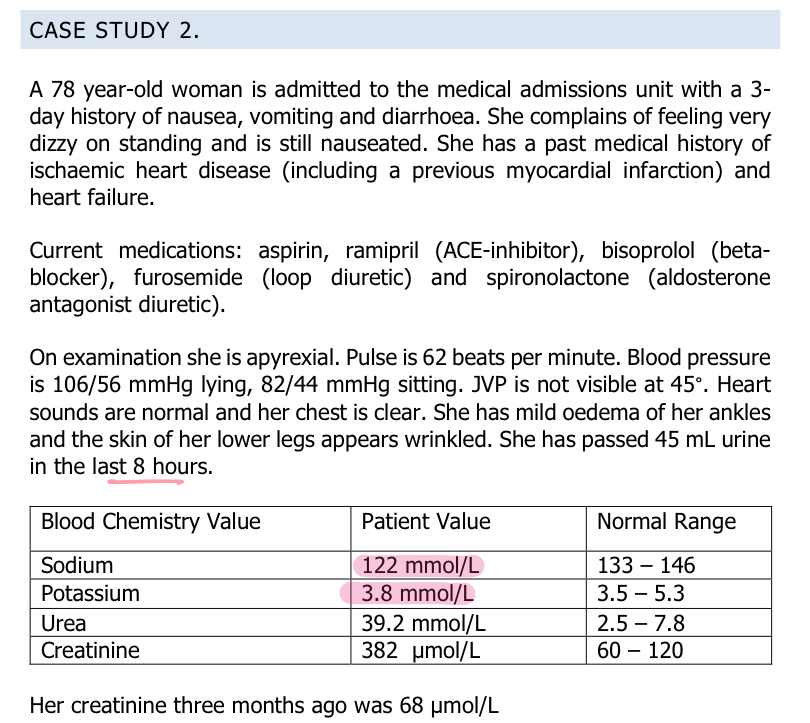

- Volume depletion due to D and V with contributions from spironolactone/ramipril being nephrotoxic. Prerenal
- Would expect high serum potassium as AKI
- Would expect low sodium due to diarrhoea and spironolactone
- Need to do urine dipstick to see if immunological or renal cause as this will change the management







