Define haematochezia
Passage of fresh blood from rectum
State some potential causes of haematochezia
- Diveritcular disease or diverticulitis
- Infective colitis
- Hameorrhoids
- IBD
- Malignancy
- Angiodysplasia
What scoring system can be used to risk stratify pts presenting with lower GI bleed to see if can be managed as outpatient?
Oakland
*Looks at age, sex, PR fidings, HR, systolic BP, hb
What investigations should you do for someone with haematochezia?
Bedside
- Stool culture: rule out infection
- DRE
- Proctoscopy
Bloods
- FBC
- U&Es
- LFTs
- Clotting
- Group & save or crossmatch
Imaging
- Flexible sigmoidoscopy
- OGD
- Capusule endoscopy
- CT angiogram
Remind yourself of anatomy of anal sphincter complex
Anal sphincter complex has internal and external part:
Internal sphincter
- Involuntary- smoth muscle
- 80% resting anal pressure
- Autonomic control
External sphincter
- Voluntary- striated muscle
- 20% resting anal pressure
- Pudendal nerve
- Three sections:
- Deep
- Superficial
- Subcutaneous
Remind yourself what the dentate line is
Junction of hindgut and proctodaeum (ectoderm)
Above dentate line:
- Columnar epithelium
- Visceral pain receptors
Below dentate line
- Stratified squamous
- Somatic pain receptors
What are the anal cushions
- Three cusions of loose connective tissue arranged circumferentially around the dentate line.
- Positioned at 3-, 7- and 11- O’clock
- Contain haemorrhoidal (venous) plexus
- Venous plexus can dilate to help with continence
What are haemorrhoids?
State two different types
- Haemorrhoids= abnormal swelling or enlargment of anal vascular cushions
- Haemorrhoids can be:
- Internal: above dentate line
- External: below dentate line
State some risk factors for haemorrhoids
- Excessive straining from chronic constipation
- Increasing age
- Raised intra-abdominal pressure e.g.
- Pregnancy
- Chronic cough
- Ascites
Less common= pelvic or abdo mass, cardiac failure, portal hypertension
Discuss the classification of haemorrhoids (what are the 4 different degrees of haemorrhoids)
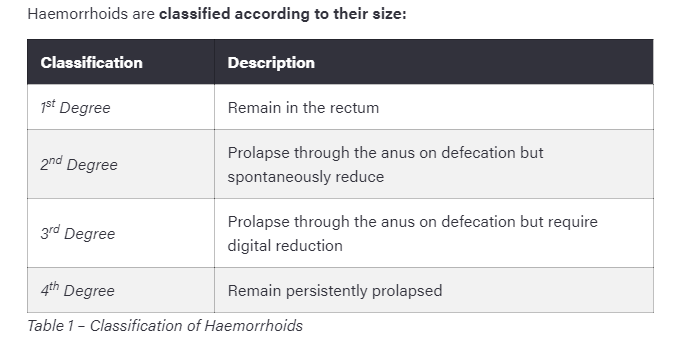

State the clinical features of haemorrhoids
- Painless haematochezia (typically on toilet tissue or after opening bowels. Blood NOT mixed with stool)
- Pruritis
- Anal lump
- Rectal fullness
What investigations should you do if you suspect haemohorroids?
Bedside
- Proctoscopy
Bloods
- FBC: ?anaemia
- Coagulation
Imaging
- May do further investigations if quering other cause of rectal bleeding
Discuss the management of haemorrhoids, consider:
- Conservative/lifestyle
- Medical
- Non-surgical
- Surgical
Nearly all managed conservatively:
Conservative/lifestyle
- Increase fibre
- Adequete fliud intake
- Avoid straining
Medical:
- Laxatives if necessary
- Anusol cream(contains chemicals to shrink haemorrhoids “astringents”)
- Germoloids ointment (contains lidocaine and zinc oxide- zinc oxide can reduce size)
- Anusol HC (contains hydrocortisone so only use short time)
Non-surgical
- Rubber band ligation
- Injection slcerotherapy (inject phenol oil to cause sclerosis & atrophy)
- Infra-red coagulation (infra-red light applied to damange arteries)
- Bipolar diathermy (use electrical current)
Surgical
- Haemorrhoid artery ligation (suture vessels that supply haemorrhoid to cut off blood supply)
- Haemorrhoidectomy (excising haemorrhoid)
- Staple haemorrhoidectomy (use device that excises ring of haemorrhoid tissue at same time as adding a circle of staples ot anal canal. Staples stay in place long term)
State some potential complications of haemorrhoidectomy
- Bleeding
- Infection
- Stricture
- Anal fissures
- Faecal incontinence
State some potential complications of haemorrhoids
- Thrombosis
- Ulceration or gangrene secondary to throbosis
- Skin tags
- Perianal sepsis
For thrombosed haemorrhoids, discuss:
- Why they occur/pathophysiology
- Presentation
- Whether they resolve spontaneously & management
Strangulation at base of haemorrhoid leading to thrombosis in the haemorrhoid
- Presentation:
- Painful (very)
- Tender (very)
- Purplish/blue lump around anus
- PR exam unlikely to be possible due to pain
- Will resolve with time but it can take couple of weeks. NICE suggest considering referral for surgery (excision) if present within 72hrs and pt has extremely painful thrombosed haemorrhoids. If not for referral, manage with stool softners, analgesia & ice packs. Symptoms often settle in 10 days.
What is a pilonidal sinus?
What age group most common in?
State some risk factors
- Formation of sinus in the cleft of the buttocks
- Younger age group (16-30yrs)
- Risk factors:
- Dark coarse body hair
- Caucasian
- Sit for prolonged periods of time
- Obesity
- Increased sweating
- Local trauma
- Poor hygiene
Discuss the pathophysiology of pilonidal sinuses
- Hair follicle in intergluteal cleft becomes inflamed or infected
- Inflammation obstructs the opening of the follicle
- Inflammtion obstructs the opening of the hair follicle
- Hair follicle begins to extend inwards forming a pit and hair is trapped in pit
- Foreign body type reaction then occurs leading to formation of a cavity= pilonidal cyst
- Pilonidal cyst connects with skin via sinus tract
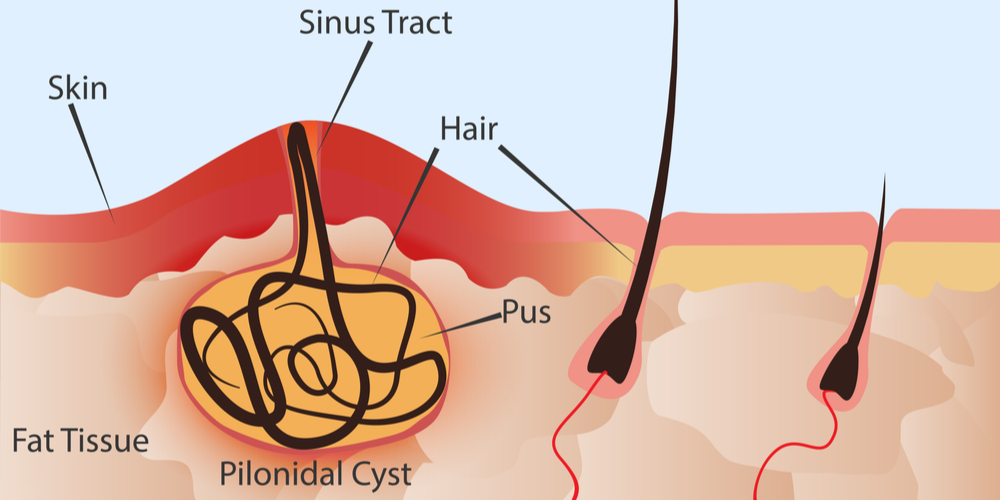
Describe clinical features of a pilonidal sinus
A pilonidal sinus can become infected and form an abscess; describe clinical features of pilonidal abscess
- Discharging sinus in intergluteal cleft area
- Intermittently painful
If pilonidal sinus becomes infected and abscess forms present with mass that is:
- Erytheamtous
- Fluctuant
- Tender
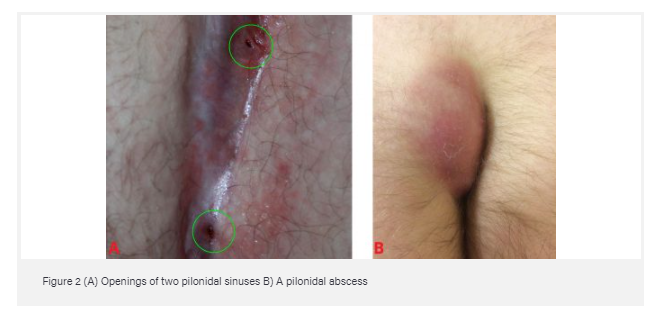
Discuss the management of pilonidal sinuses
Someties pilonidal disease eases with age & doens’t require surgical management.
Conservative
- Shaving the affected region
- Plucking sinus free of any hair
Surgery for chronic disease
- Excision of tract & layout open of wound
- Ecxision of tract & primary closure (higher reate reoccurrence, lower infection rate)
Pilonidial abscess:
- Abx if septic
- Incision & drainage with washout
- Removal of sinus at later date
What are perianal fistulas?
What are the majority of perianal fistulas associated with?
- Abnormal connection between anal canal and perianal skin
- Anorectal abscesses
Other risk factors:
- IBD
- Systemic disease: TB, HIV
- History of trauma
- Previous radiotherapy
Describe clinical presentation of anal fistulas
- Present with perianal abscess
- Discharge onto perineum (mucus, blood, pus or faeces)
- External opening on the perineum
- Fibrous tract may be felt underneath skin on DRE
What investigations are required for anal fistulas?
- Proctoscopy
- MRI if complex
Discuss the management of perianal fistulas
Most fistulas don’t heal on their own. Many surgical methods but most common ones are:
- Fistulotomy:lay tract open and allow to heal by secondary intention
- Seton insertion: allows fistula to drain in attempt to let fistula heal and close
May require several repeat procedures




