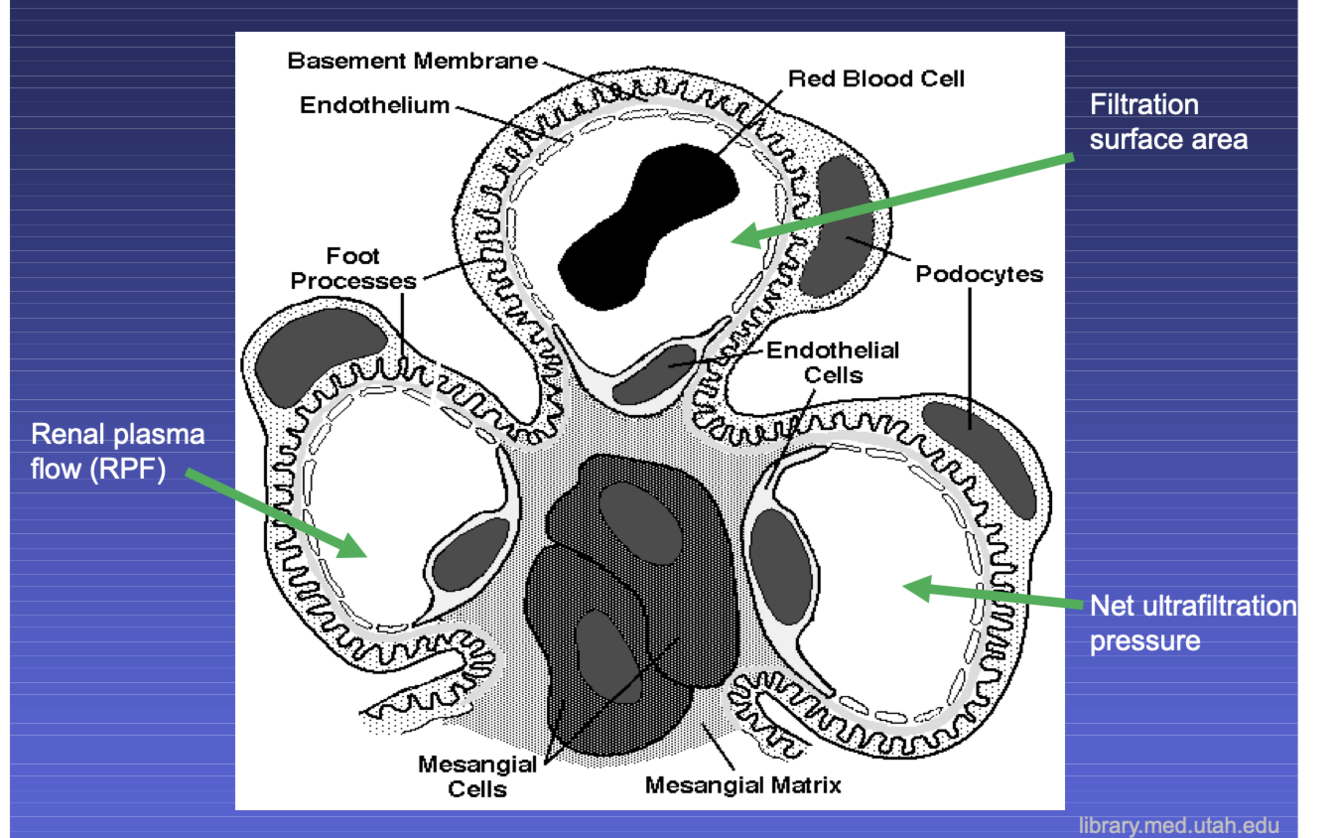
the part of the nephron that accepts blood from the systemic system into the nephron unit
glomerulus
how does the afferent arteriole regular the RAS system?
- the afferent arteriole is primed to produce renin until sufficient stretch (which indicates good cardiac output) and pressure occurs, in which point renin production decreases.
- renin release increases when there is increase in nervous system activity or when there’s reduced distal nephron sodium delivery. when we increase the release of renin a cascade results that increases proudction of angiotensin II which increases absorption of salt and fluid at the proximal tubule. It also facilitates the release of ADH hormone that results in water reabsorption. it increases CO and arterial pressur,e and when the artieral pressure is normal/sufficient, the RAS decreases in activity.
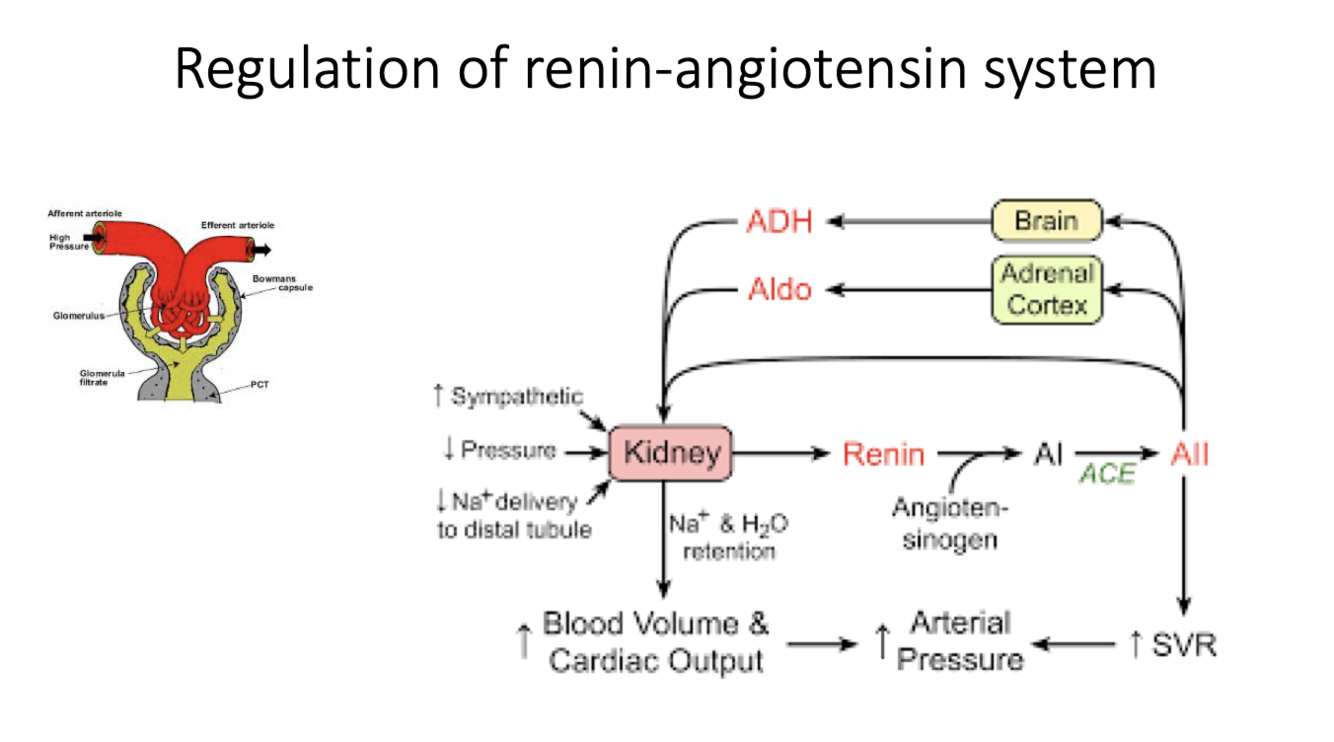
Primarily regulates serum osmolality; also responds to low blood volume states. Stimulates reabsorption of water in collecting ducts. Also stimulates reabsorption of urea in collecting ducts to maximizes corticopapillary osmotic gradient.
ADH
Primarily regulates ECF volume and Na+ content;
incresae release in decreasedblood volume states. Responds to hyperkalemia byK+ excretion.
aldosterone
Helps maintain blood volume and blood pressure. Affects baroreceptor function; limits reflex bradycardia, which would normally accompany its pressor effects.
angiotensin II
__ is secreted by JG cells in response to decreased renal perfusion pressue (detected by renal baroreceptors in the afferent artiole), increasing renal sympathetic discharge (beta 1 efect), and decreasing NaCL delivery to the macula densa cells
renin
Efferent arteriole allows for greater
hydrostatic pressure. this increases the glomerular filtration rate.
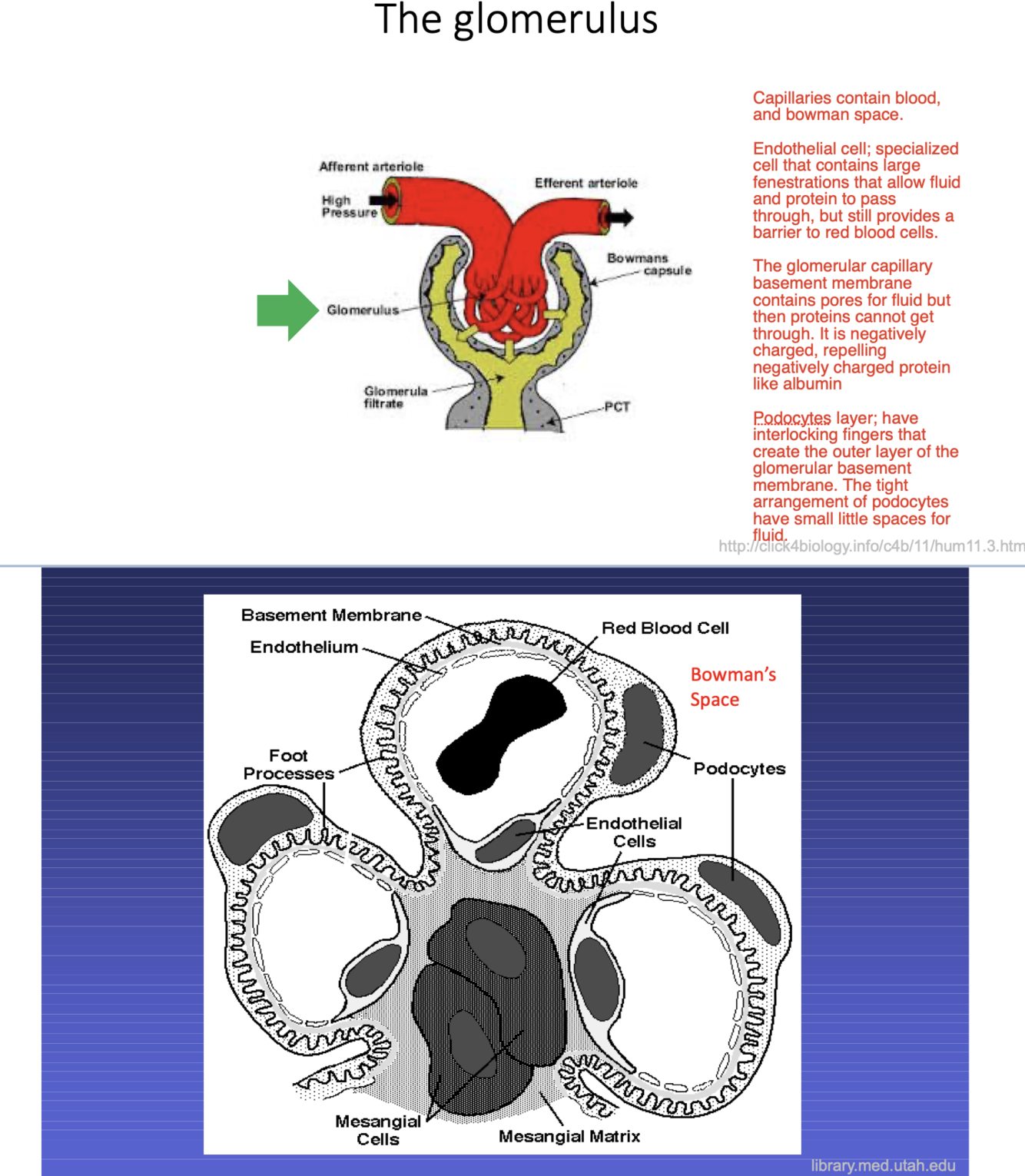
3 layers to the glomerular capillary barrier
- fenestrated capillary endothelium
- basement membrane with type 4 collagen chains and heparan sulfate
- visceral epithelial layer consisteing of PODOCYTE CELL. have interlocking fingers that create the outer layer of the glomerular basement membrane. The tight arrangement of podocytes have small little spaces for fluid.
Charge barrier—all 3 layers contain ⊝ charged glycoproteins that prevent entry of ⊝ charged molecules (eg, albumin).
Size barrier—fenestrated capillary endothelium (prevents entry of > 100 nm molecules/blood cells); podocyte foot processes interpose with glomerular basement membrane (GBM); slit diaphragm (prevents entry of molecules > 50–60 nm).
___ ___ __ is used to quantify solute clearance
glomerular filtration rate. • Typically based upon serine creatinine in blood. Endogenous waste product from muscle waste. Change in CK is caused by change in kidney clearance.
outline how starlings forces affect GFR
- *• Renal plasma flow;** the more blood flow, the more filtration rate.
- *• Filtration surface area**; the less surface area (due to disease), the reduced filtration
- *• Net ultrafiltration pressure;** hydrostatic and oncotic pressure and oncotic pressure of capillary and Bowmans space can affect movement of fluid that contains waste products of the blood.