Drugs that can cause pancreatitis
Azathioprine
Corticosteroids
Didanosine
Estrogens
Lasix
HCTZ
Metronidazole
Opioids
Pentamidine
Sulfa drugs
Tetracycline
Tamoxifen
Valproate
Rare causes of pancreatitis
Infection
Hereditary
Hypercalcemia
Anatomic
Hypertriglyceridemia (generally > 1000)
Tumors
Toxins
Autoimmune (rare)
How does pancreatitis present?
- Low grade fever common (60%)
- Pain radiating to back (50%); worse in supine position
- 75% have N/V
- Rebound rare; guarding common (50%)
- Cullen sign is rare
- Grey Turner sign rare (but useful clue if you see it)
What is Cullen’s Sign?
Cullen’s sign is superficial edema and bruising in the subcutaneous fatty tissue around the umbilicus.
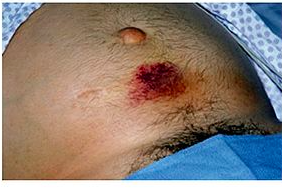
What is this?
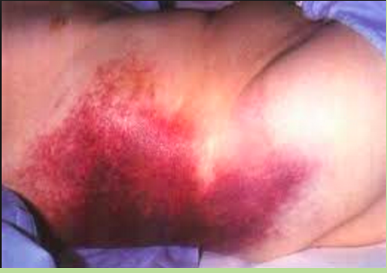
Grey Turner Sign in pancreatitis
What labs should be ordered for suspected pancreatitis?
- lipase (94% Sn; 96% Sp; LR+ 23; LR – .06)
- Amylase (less Sn and Sp than lipase)
- LFTs (100+ highly suggestive)
- Hematocrit (≥ 50 on admission predicts severe disease (LR+ 7.5))
- CRP (> 150mg/L at 48 hours predicts severe disease (LR+ 3.2-6.6))
___% of patients with pancreatitis can develop severe disease
20
What are the local complications of pancreatitis?
pseudocyst, necrosis, infections
What are the systemic complications of pancreatitis?
hyperglycemia, hypocalcemia, ARDS, AKI, DIC
•Death more likely with infected pancreatic necrosis and in patients with MSOF

What is the Initial treatment of acute pancreatitis?
is non-operative –Fluid resuscitation, pain management, maintenance of ventilation, adequate oxygenation, and renal perfusion
•15% of patients do not improve within 3 to 5 days. How should you procede?
- Order contrast-enhanced CT scan of the pancreas to rule out pancreatic necrosis
- Broad-spectrum antibiotics against enteric pathogens are indicated if necrotizing pancreatitis present
- Aggressive nutritional support and proper electrolyte replacement also important with severe pancreatitis
How common is diverticulosis?
- 5-10% of persons > 45 years of age
- 50% of those > 60 years old
- 80% in those > 85 years old
What is thought to cause diverticulosis?
–Low-fiber diets may cause due to decreased stool bulk
•Increases intraluminal pressure causing mucosa/submucosa to herniate through colon wall where blood vessels penetrate
How does dievrticulitis occur?
•Develops secondary to microscopic or frank perforation of diverticula (e.g. vasa recta perforate muscularis externa)
Where is diverticulitis most common?
85-95% in sigmoid/descending colon (LLQ pain)
What are the complications of diverticulitis?
abscess, peritonitis, sepsis, colon obstruction, fistula (colovesicular most common)



CRC




