What are the signs of necrosis in MCI?
- Pathological Q waves
- QS complexes
- Poor R progression
What are the criteria for a pathological Q wave in MCI?
- longer than 0.04 sec
- greater than 0.4 mV
- greater than 25% size of R wave
Where is it normal to see QS complexes?
aVR and V1
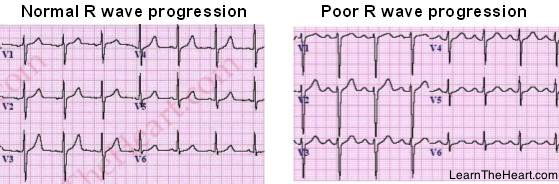
How does “poor R progression” look in MI?
What kind of MI might it indicate?
- R waves remain very small in V3/4
- Rs are a bit bigger, but still smaller than expected in V5/6
- can indicate actue anterior MI even in the absence of pathological Q waves
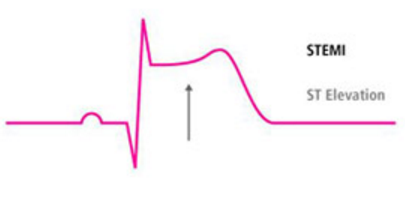
What is the main sign of lesion in the progression of an MCI?
(How does it often look? In what leads?)
ST elevation
- often as T-en-dome in various leads__
- inverse in aVL
- may have clear S wave
What is the main sign of ischemia in MCI progression?
How is this sign different in different stages?
T wave abnormalities
- hyperacute - high Ts hidden “en dome”
- acute - biphasic Ts
- subacute - coronary T (img below)
- old - inverse T

What are the 4 stages of MI progression as seen in an ECG?
And their approximate durations?
- Hyperacute - symptom onset until ~4 hours
- Acute - first 48-72 hours
- Subacute - 10 days
- Chronic/End-stage/Old/Definitive - past 10 days
What are the signs of hyperacute stage MI progression?
Ischemia and lesion only, so…
- ST elevation + T abnormality = T-en-dome
What are the ECG signs of acute stage MI?
Necrosis has begun, so…
- Pathological Q waves + poor R progression
- T-en-dome
- Sometimes biphasic T dips down after the “dome”
What is the ECG sign of subacute stage MI?
Necrosis has leaked K+ into the tissues, leading to…
- Coronary T waves - deep, peaked, symmetrical
- less lesion may mean less ST elevation
What are the ECG signs of definitive/old MI?
K+ elevation subsides, so…
- Coronary T disappears, but…
- Ischemia = primary repolarization abnormalities, including flat/negative Ts
- Necrosis = persistent patho-Q waves and smaller R waves in V3-6
Where can inferior infarcts be seen?
Occlusion of what artery usually causes them?
Other things to note with inferior infarcts?
leads II / III / aVF
occlusion of RCA
(reciprocals in anterior/left leads)
(Q waves may not persist)
Where can lateral infarcts be seen?
Occlusion of what artery usually causes them?
leads I / aVL / V5 / V6
(may see reciprocals in inferior leads)
circumflex artery occlusion
Where can anterior infarcts be seen?
How might they appear different than infarcts elsewhere?
Occlusion of what artery causes them?
in precordial leads, will see poor R progresson
may not see pathological Q waves
may see reciprocals in inferior leads
LAD occlusion
Where can posterior infarcts be seen?
They are often seen with what else?
reciprocal signs in precordial leads
(especially V1)
often seen with inferior infarcts (because both supplied via RCA)
What are the normal ID times in leads V1/V2?
in V5/V6?
What can prolongation mean?
- V1/2 - 0.04 sec
- V5/6 - 0.06 sec
- prolongation means BBB in the corresponding side (V1/2 = RBBB, V5/6 = LBBB)
How can LV hypertrophy be confirmed?
Sokoloff Index
- biggest R in V5/6 + deepest S in V1/2
- biggest R + deepest S > 3.5 mV (35 mm)
- (or axis < 10 degrees with positive aVL > 2 mV)
What are the signs of LBBB?
- wide QRS (> 0.12 s)
- broad/notched R waves in I + aVL
- broad rS or QS complexes in V1-4
What are the signs of RBBB?
- wide QRS
- M complex (rSR’) and ID > 0.04 s in V1/V2
- deep, wide S in left lateral leads
What is seen in any kind of BBB?
- wide QRS (≥ 0.12 sec)
- secondary repolarization abnormalities
- supraventricular impulses
- (differentiate it from PVCs / V.Tach)
How long is a normal QT interval?
0.35 - 0.44 seconds
What do polymorphic P waves of 3 or more forms indicate?
Multifocal Atrial Tachycardia if > 100 bpm
Wandering Atrial Pacemaker if < 100 bpm
How can an incomplete BBB appear on ECG?
BBB wave morphology (M complex or notched Rs) without the usual QRS wideness
What are the two types of WPW syndrome and how are they differentiated?
Look at V1, if QRS is…
- negative = Type B = bundle on right
- positive = Type A = bundle on left
- (remember “apple”, APL = A-Positive-Left)















