3 stages of vomiting
- Nausea
- Retching - forceful gastric contents enter the esophagus
- Vomiting - expulsion of gastric contents by contraction of abdominal muscles and diaphragm
Intrathoracic pressure is negative during retching and positive during vomiting.
Vomiting is controlled by 2 centers
- Emetic center
- Medulla oblangata (CRTZ) - floor of the 4th ventricle
How is the emetic center stimulated?
- Humoral pathway - blood borne substances
- Neural pathways
- afferent vagal pathway
- sympathetic pathway
- vestibular pathway
- cerebrocortical pathway
- Direct extension from brain disease
- inflammatory
- space occupying lesion
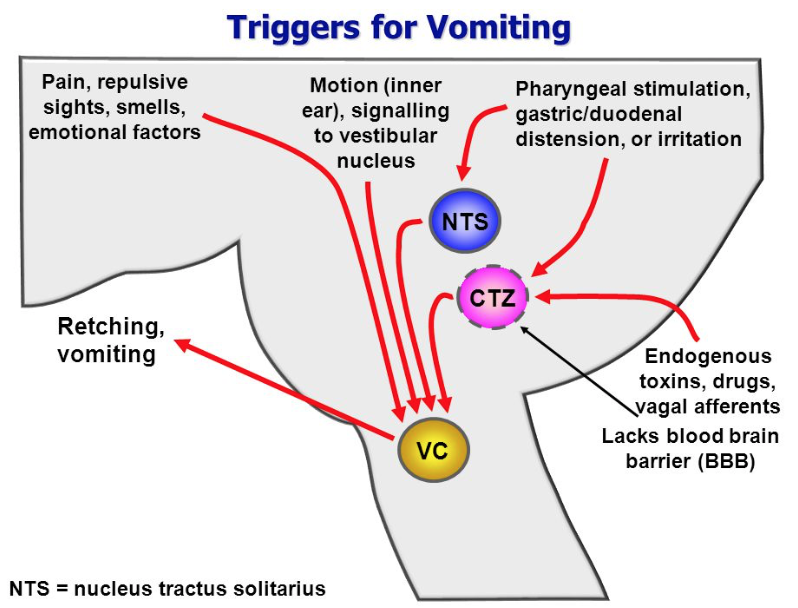
How is the neural pathway activated?
Via peripheral receptors throughout the body
- especially those of duodenum ~ “organ of nausea”
How does the humoral pathway stimulate vomiting?
Limited blood brain barrier in the medulla allows the CRTZ to be exposed to blood-borne chemicals (drugs, uremia, etc)
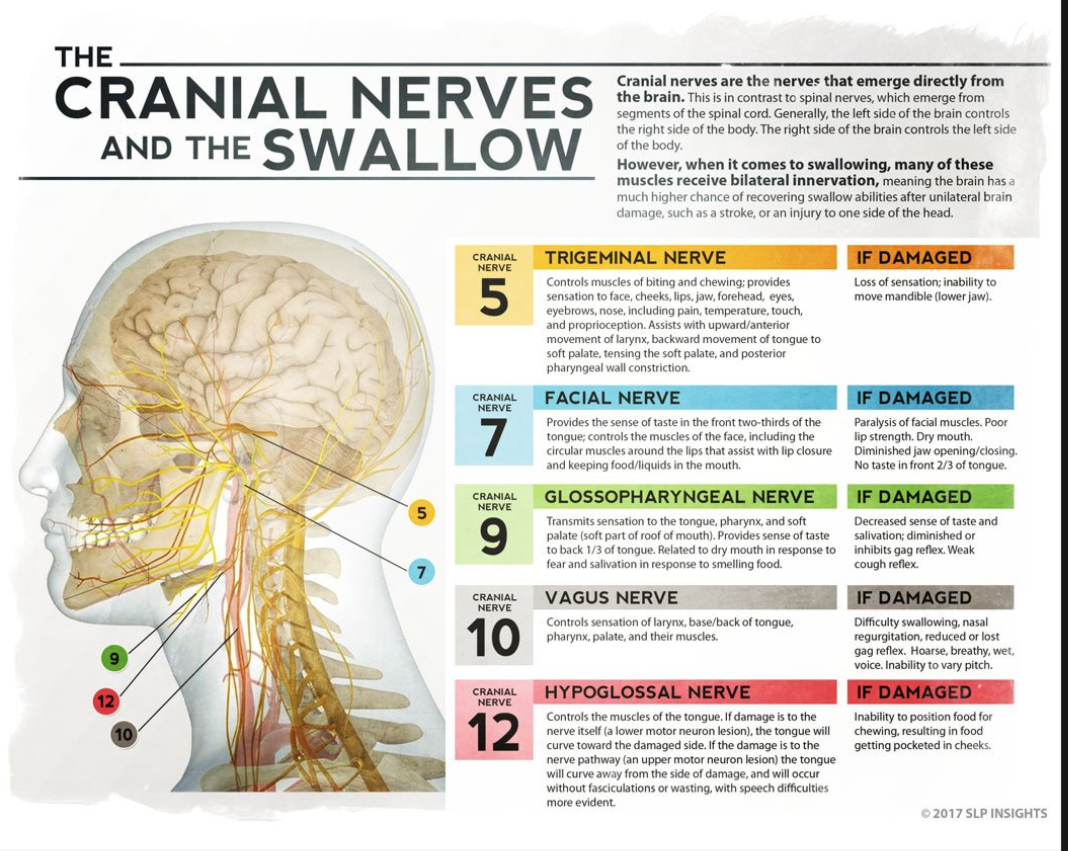
What are the three phases of swallowing and what CN are involved in each?
Oral phase
- Tongue makes bolus and moves bolus on midline and back (CN 12, sensory for this CN 5). This is voluntary until the bolus reaches pharynx.
- Dysphagia from oral phase disorders due to reduction in tongue function for the most part.
Clinical signs:
- Inability to hold food in mouth or transport it back
- Poor bolus formation
- Inability to initiate pharyngeal phase
- Weak tongue-action during pharyngeal phase.
- Rarely aspirate
_Pharyngeal phas_e
- Soft palate is elevated, palatopharyngeal folds move inward, vocal folds pull together, larynx elevated against epiglottis, Cripcopharyngeal muscles relax, UES opens, bolus enters esophagus, UES closes, pharyngeal muscles relax (CN 5, 7, 9, 10, 12 all involved)
- Geniohyoideus and mylohyoideus pull larynx forward letting the epiglottis close over the glottis. Concurrently the adductor muscles close the glottis
- Tongue stops forward and backward movements and prevents food going back into oral cavity.
- Dorsal pharyngeal constrictors stops food egress from pharynx, palatopharyngeal arch contracting stops food going back into nasopharynx5
- There’s a bunch of nuclei in the reticular formation termed the swallowing center. Vagus sends visceral info to medulla oblongata from tongue, pharynx and esophagus
Nerves involved:
CN 5 - Trigeminal:
- Sensory nerves from oral cavity
- Motor fibers for mucles of mastication, mylohyoideus and soft palate muscles
CN 7 - Facial:
- Sensory nerves from visceral receptors in the soft palate and nasopharynx
- Motor fibers to stylohyoideus and jugulohyoideus
CN 9 - Glossopharyngeal
- Sensory nerves to pharynx and part of tongue, with vagus
- Motor fibers to constrictors and dilators of pharynx
CN 10 - Vagus
- Motor with glossopharyngeal nerve (CN 9) to constrictors and dilators of pharynx.
- Also carries visceral efferent and afferent fibers to pharynx so intimately involved with all stages of swallowing
- Pharyngoesophageal nerve - from vagus and glossopharyngeal
- Motor nerves to caudal pharyngeal muscles (cricopharyngeus and thyropharyngeus), laryngeal muscles and cervical esophagus
CN 12 - Hypoglossal
- Motor fibers to tongue
Dysphagia of the pharyngeal phase usually with poor contractility and transport function of cranial and caudal pharyngeal constrictors.
Clincial signs:
- See deficiencies in the contractions delivering bolus from the oropharynx to the esophagus and contrast/food stuck in the valleculae, pharynx opening and piriform recesses but ability to form bolus and push it back, so incoordination of the cricopharynx, normal esophagus4
- Predominantly aspiration (also seen with cricopharyngeal dysphagia).
- Food can be stuck in pharyngeal recesses for hours, and pharyngral recesses enlarge so can regurg food from there hours later.
Esophageal phase:
- Transports bolus through esophagus, through gastroesophageal sphincter, to stomach (esophagus innervations vagus).
- A bolus should always stay a bolus…if it breaks up in the esophagus it indicates a motor deficiency, has been seen with myasthenia gravis.
Primary peristalsis = esophageal motility triggered by pharyngeal contraction.
- May need sufficient tactile or stretch stimulus for this to occur
Secondary peristalsis = esophageal motility triggered by esophageal luminal distension and tactile stimuli.
- Esophageal peristalsis can follow a couple of different sequences (normal)
- Swallow is followed by immediate peristalsis of esophagus (primary peristalsis)
- After a swallow the bolus sits in the cranial esophagus until another 1 or 2 swallows occurs, then all boluses are sent down together (still primary peristalsis)
- After a swallow the bolus sits in the cranial esophagus for a short period of time, then stimulates a peristaltic wave (secondary peristalisis)
- A few boluses accumulating in the cranial esophagus finally trigger a peristaltic wave (secondary peristalsis)
- Boluses can occasionally stall in the esophagus until a secondary peristaltic wave comes along
- Some separate esophageal from gastroesophageal phases where the gastroesophageal phase is the passage of food through the LES
- There is sometimes a small amount of reflux through the open LES, without contraction of the stomach and with almost immediate secondary peristaltic wave to push it back. That can be normal (relaxation can last 8-12 sec).
The LES is functional, not anatomic. It is the association between a bunch of things:
- Gastric rugal folds interdigitate near the cardia
- Focal thickening of inner smooth muscle of distal esophagus
- The oblique insertion of the esophagus into the stomach
- Flap-like cardiac incisura pushed up against the esophageal opening
- The deep oblique smooth muscle of the lesser gastric curvature forms a sling around the left side of the cardia
- Compression of the intra-abdominal esophagus by the intra-abdominal positive pressure
- The muscular sling of the diaphragm as the esophagus goes through it helps with closure.
Some add in the cricopharyngeal phase- relaxation of the cricopharyngeal sphincter, passage of bolus into UES, closure of the sphincter, relaxation of the pharyngeal muscles4
Dysphagia of this phase from inability to open or close UES, or incoordination between UES opening and pharyngeal contraction4
How does GDV lead to hypoxia?
Thoracic and diaphragmatic impingement results in decreased tidal volume, which causes ventilation/perfusion mismatch and results in hypoxia.
How does GDV result in arrhythmias, hemorrhagic enteritis?
Due to decreased tissue perfusion
How does a GDV result in anemia and hemoabdomen?
Avulsion of short gastric and right gastroepiploic vessels
Liver usually has ___ blood flow and ___ vascular resistance.
Liver usually has high blood flow and low vascular resistance.
- Portal vein pressure is 9mmHg
- Pressure of hepatic vein leading to CVC is 0mmHg
Functions of liver
- Blood reservoir
- Fat/protein metabolism - has high lymph flow: pores in hepatic sinusoids are very permeable and allow passage of fluids/proteins into the space of Disse
- Carbohydrate metabolism
- Blood cleansing - the louder cells (tissue macrophages) will clear GI origin bacteria and endotoxins from the portal vein via phagocytosis
- Immunoregulatory function
- Detoxifying
- Biliary excretion
How does PSS result in microhepatica?
Decreased blood flow and lack of insulin, glucagon and nutrients in the liver results in hepatic atrophy.
How does liver disease result in hepatic encephalopathy?
It’s related to decreased clearance of GI toxins such as ammonia, mercaptans, short fatty amino acids, GABA and endogenous benzodiazepines.
How does PSS result in urate stones?
Inadequate clearance of ammonia by the liver (because blood is getting shunted and bypasses the liver) results in increased urinary excretion of ammonia and uric acid - renal, cystic or urate urethral calculi may form.
Causes of acquired PSS
Portal hypertension:
- Liver disease
- Cirrhosis
- Idiopathic fibrosis
- Chronic hepatitis
- Portal vein thrombosis
- Post surgical occlusion of PSS
- Neoplasia
- Extra luminal compression of portal vein
Causes of acute hepatitis
Toxin/Drug:
- Acetaminophen
- Carprofen
- Tetracycline
- Sulfonamides
- Diazepam
- Methimazole
Hepatic lipidosis (cats):
- During starvation more fatty acids are mobilized and less lipoproteins are produced, which causes lipid accumulation
Vascular compromise:
- Liver love torsion
- Portal vein thrombosis
Infectious causes:
- Adenovirus type 1
- Helicobacter canis (rare)
- FIP: usually dry form which results in immune complex vasculitis and pyogranulomatous inflammation
- Hepatic abscess: can occur for many reasons
- immunosuppressed animals
- diabetes mellitus
- umbilical infection in young animals
- penetrating abdominal wound
- direct extension from local infection
- primary septic focus with seeding of liver through bloodstream (pyelonephritis, pyometra, endocarditis, other cause of sepsis)
How does liver disease result in decreased copper excretion?
Copper is usually excreted in bile. Liver disease with cholestasis and decreased bile flow could cause copper accumulation.
What breeds are predisposed to copper storage disease?
Belington terriers
- Bellington terriers accumulate copper throughout their life due to mutation that results in mellathionein that has strong affinity to copper.
West Highland White Terrier
- West Highland White Terriers do not accumulate copper throughout their life. They usually peak copper levels at around 6-12 months of age. Mechanism unknown.
Doberman
Cocker Spaniel
What is cholangiohepatitis?
Inflammation of bile ducts and adjacent hepatocytes. Usually seen in cats. Persians are predisposed. Thought to be due to ascending infection from GI (E. Coli).
What’s is cholecystitis?
Inflammation of gall bladder and associated bile ducts. Emphysematous cholecystitis commonly seen in pets with DM
Causes of biliary obstruction
Extra hepatic:
- Pancreatitis
- Pancreatic abscess/cyst
- Pancreatic neoplasia
- Bile duct neoplasia
- Intestinal neoplasia
- LN neoplasia
- Scar formation around the bile duct
- Cholelith
Intra hepatic:
- Cholestasis
- Periportal inflammation (cholangiohepatitis)
- Hepatic lipidosis
Causes of mucocele formation?
- Cholestasis resulting in biliary stasis
- Mucinous hyperplasia +/- chronic inflammation
Bacterial infection may occur secondarily
Describe the course of the esophagus.
Cervical - midline or left of midline
Heart base - aorta is now on the left with the esophagus on the right
Cat esophagus differ in 3 ways:
Cat esophagus:
- The proximal 70% of the esophagus is striated muscle, while the distal 30% is smooth muscle (whereas in dogs the entire esophagus is striated muscle).
- Herring bone I in cats the terminal esophagus is arranged in transverse ripples, which create this herringbone appearance
- “Cone” shaped at terminal portion






















