What is S. aureus?
Common human pathogen
- 20-40% of humans
- Infects everyone: patients in hospitals, and normal hosts within the community
What are the most common causes of S. aureus infections?
Post-op infections: have started doing pre-op decolonizations which has decreased infection rates by 45%
Skin infections, soft tissues, bones, and articulations
Can provoque other invasive infections: bacteremia, endocarditis, pneumonia
What kind of bacteria is S. aureus?
- Spherical (cocci)
- Arranged in bunches (grappes/amas) —> staphylé = grappe de raisins
- Gram +
- Catalase + (hémolyse +)
- Also known as Staphylocoque doré
Can survive extreme conditions (extremophile): heat, dryness, salty environments
What is the staphylococcus genus? (4 ones to know)
30 ish species:
- S. aureus (most common)
- S. lugdunensis (coag. -) —> same pathogenicity as S. aureus
- S. epidermis —> opportunistic bacteria (infection tied to prosthetic material)
- S. saprophyticus —> UTI in middle aged women
Gram negative vs. gram positive:
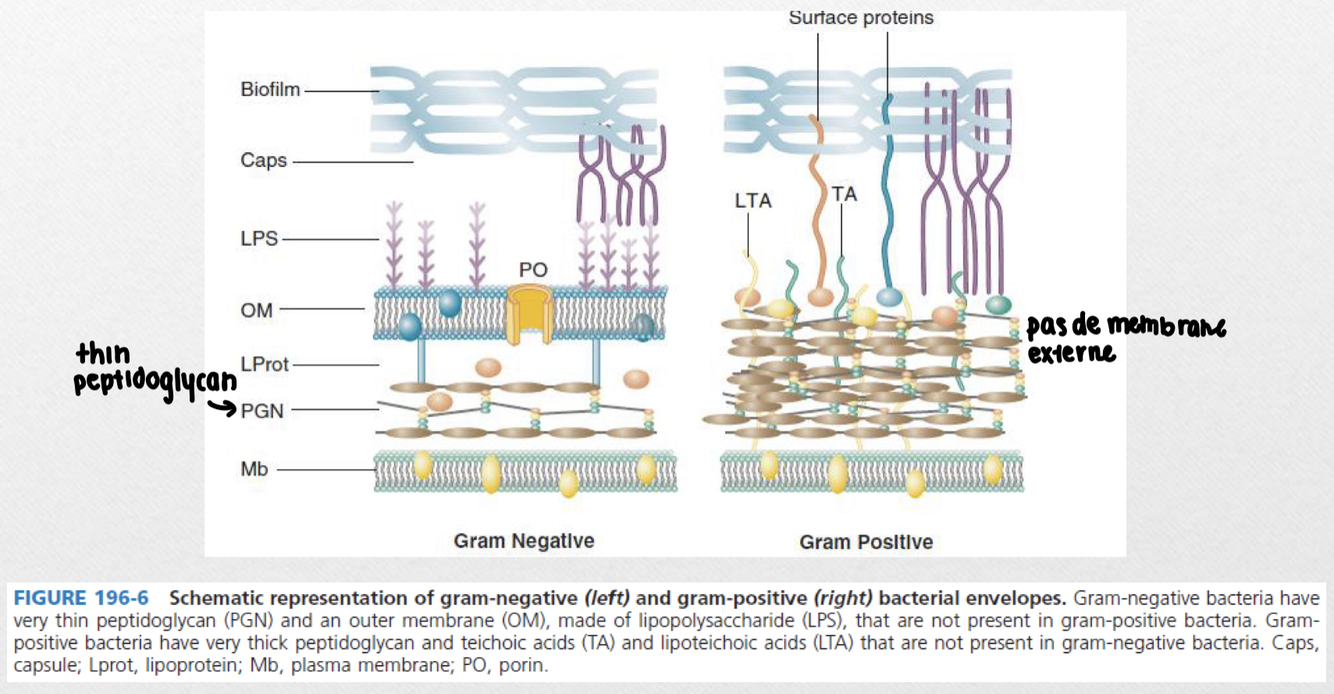
What is on the bacterial surface of S. aureus? (6 to know)
- Polysaccharide capsule: antiphagocytaire
- Adhésines: attached to peptidoglycan (surface proteins), allow for adhesion
- Biofilm: matrice de protéine et polysaccharides —> limit diffusion of antibiotics and nutrients, bacteria in latency form
- Acides teichoïques (AT) et acides lipoteichoïques (ALT): 50% of paroi, adhesion of enzymes to paroi/metabolism (AT) and inflammation (ALT)
- Peptidoglycans: more than 10 layers in gram + and 2 in gram - (allows for rigidity), recognized by the immune system (cytokines —> inflammation)
- Surface proteins (protein A): cache le peptidoglycans du système immunitaire —> capacité anti-phagocytaire
Which toxins are present? (4 main kinds)
Hemolytic:
4 kinds: alpha, beta, gamma, delta
- alpha-hemolysine is the main one: polymerases on membrane of eukaryotes to create pores (important in pneumonia and endocarditis)
- lysis of host cell —> releases cytokines
- Sphingomyelinase (toxine beta or beta-hemolysine): alters lipidic contents of membranes by enzymatic destruction
- Toxine delta: not really known
- Toxine gamma: leucocydine —> damages white blood cells
What is Panton–Valentine leukocidin (PVL)?
cytotoxin—one of the β-pore-forming toxins.
- The presence of PVL is associated with increased virulence of certain strains (isolates) of Staphylococcus aureus
- protein that attacks polymorphonucléaires and macrophages
- analogous of gamma-hemolysin
- < 2% of S. aureus strains —> SARM-H, SASM
- In about 100% of SARM associated to community
Bad clinical evolution: infections cutanées et penumonies nécrosantes sévères
What are enterotoxins?
Gastrointestinal effects
In 30% of S. aureus strains
6-8 million cases a year in the USA —> 10% hospitalized
What is the main enterotoxin of S. aureus?
Entérotoxine A —> more than 15 described, resistant to heat so when bacteria is destroyed by heat toxins stay present in environment —> food poisoning
- Sx 2-6 hrs after ingestion —> N/V but no fever… usually resolves itself
What are toxines exfoliatives?
A (phage) and B (plasmids)
Secretion of toxins in muqueuse or skin —> disseminated in organism
< 2% of S. aureus are carriers —> usually cause outbreaks in children under 1 year
What are the two syndromes that toxine exfoliative are responsible for?
- Generalized form (young pts) —> Staphylococcal Scalded Skin Syndrome
- Localized form (older kids and adults) —> Bullous impetigo
What is a superantigen?
Antigène qui active les lymphocytes T sans passer par la voie normale des cellules présentatrices d’antigènes
They induce:
- Non-specific proliferation of T lymphocytes
- Massive release of cytokines —> 20% of T lymphocytes activated
- Leads to exaggerated inflammatory response
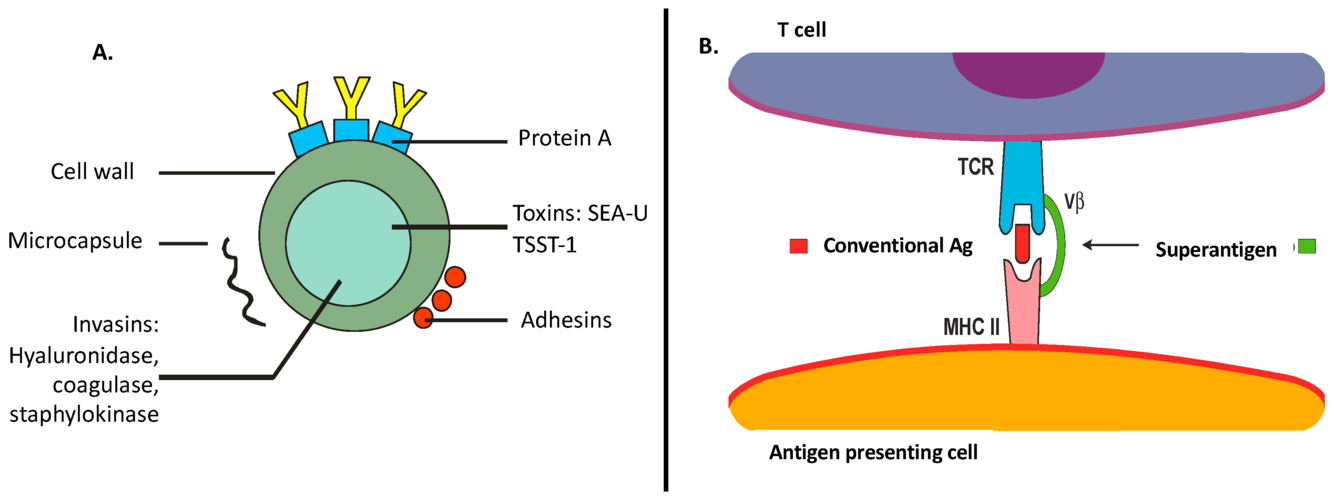
What is toxic shock syndrome? (TSST-1)
TSST-1 is a superantigen
Leads to local production of toxins which disseminate throughout organism
What are the important enzymes to S. aureus? (5)
- Coagulase:
- Prothrombine —> causes coagulation of plasma and formation of clots
- Staphylokinase:
- Fibrinolysis, breaks thrombus and allows for dissemination of bacteria
- Lipase:
- colonization and invation
- Hyaluronisase:
- Hydrolyses acide hyaluronique in conjonctive tissue which allows for initial progression of cutaneous infections
- B-lactamase:
- Enzymes that hydrolytically destroy beta-lactams (antibiotic resistance)
Which antibiotics can strains of S. aureus be resistant to?
Penicillin (all)
Methicillin (SARM)
SARM-AC (associated to the community) —> still effected by clindamycin… unlike SARM-HA (healthcare associted)
< 10 strains —> resistant to vancomycin
Histoire naturelle de S. aureus?
Permanent colonization: 20% of people —> same clone
Intermittent colonization: 30% of people —> different clone (vagina, nasopharynx, skin)
Transmission/contamination de S. aureus?
Interpersonal, air, objects
Bris de la barrière muqueuse ou cutanée and S. aureus?
adhésion et infection
28-43 infections/ 100 000 people per year —> about 700k a year in the States
Which layers of the skin are effected in different cutaneous lesions infected by S. aureus?
- Epidermis
- Impetigo
- Superficial dermis and hair follicles
- Folliculitis
- Deep dermis
- Furoncles, carboncules, Hidradenitis suppurativa
- Sub-cutaneous infection
- Cellulitis, erysipelas
What is impetigo?
Macule that evolves towards vesicles due to epidermolytic toxins (80% S. aureus, 20% S. pygenes)
The crust is yellow-brown, or honey-colored
What is folliculitis?
Infection centered on hair follicles
What are boils (furoncles)?
deep folliculitis, infection of the hair follicle —> mostly in hairier areas
What are carbuncles?
cluster of boils caused by bacterial infection


