Signs of resp. distress in a child
· Intercostal recession
· Subcostal recession
· Tracheal tug
· Grunting
· Nasal flaring
· Tripoding
Normal respiratory rates in children
Neonates: 30-60
<1 year: 30-53
1-2 years: 22-37
3-5 years: 20-28
6-11 years: 18-25
12-15 years: 12-20
Differential diagnosis if a child has stridor
- Croup: barking cough, fever
- Foreign body aspiration: sudden onset, choking, no fever
- Epiglottitis: drooling, very unwell/ septic, do not examine the child, ask re vaccinations
- Bacterial tracheitis: harsh cough, chest pain, septic, no drooling, IV antibiotics and intubation needed
- Anaphylaxis
Varying severity of croup
• Mild: seal like barking cough but no stridor or sternal/ intercostal recession at rest
• Moderate: seal like barking cough with stridor and sternal recession at rest, no agitation or lethargy
• Severe: seal like barking cough with stridor and sternal/ intercostal recession associated with agitation or lethargy
• Impending respiratory failure: increasing upper airway obstruction, sternal/ intercostal recession, asynchronous chest wall and abdo movement, fatigue, pallor or cyanosis, decreased consciousness.
Degree of chest wall recession may diminish with the onset of resp failure as the child tires. Resp rate >70 indicated severe resp. distress
How is croup managed?
Steroids: dexamethasone or prednisolone orally OR budesonide nebuliser
Severe croup or children with impending resp. failure may need adrenaline nebulisers and an anaesthetic/ PICU review
- Symptoms should improve in 1-3 days
- Viral so antibiotics don’t help
What is bronchiolitis?
· Viral illness in children <2yrs of age causes oedema of airways with secretions +++
· Common causes: RSV, rhinovirus, adenovirus
· Causes crackles, wheeze and coryza
· Antibiotics, steroids and inhales/ nebulisers don’t work
· Treatment is supportive
· Gets worse over 5 days then improves
· Coryzal prodrome lasting 1-3 days followed by persistent cough, resp distress, wheeze/ crackles on chest
Management of bronchiolitis
- Investigations: nasopharyngeal aspirate - identifies virus for cohorting purposes
- Provide oxygen to maintain sats >92%
- Support feeding with smaller more freq. feeds or NG feeds
- In severe cases use IV fluids, resp. support such as high flow oxygen, CPAP, intubation, CXR
- Who are at risk of severe bronchiolitis? <6 weeks, preterm birth, chronic lung disease, congenital heart disease, immunodeficiency
What % of paeds admissions are due to resp. conditions?
Respiratory conditions responsible for 50% of all acute paeds admissions
Why do children aged 1-6 tend to vomit when they cough?
Increased intra-abdo pressure when coughing and immaturity of the lower oesophageal sphincter
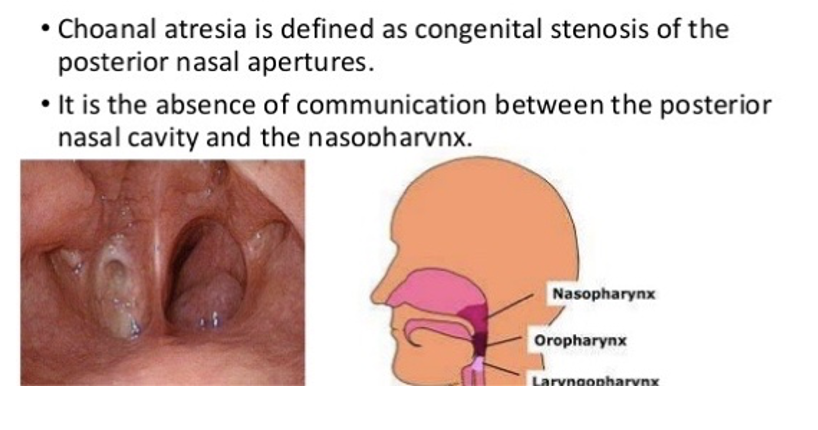
Choanal atresia
Nasal passages blocked by bone or tissue
- 1/10,000 births
- Bilateral atresia presents with respiratory distress or cyanosis at birth
- Improves on crying because mouth is open
- Early surgery is needed to open the blockage with nasal stents inserted until the nasal passage heals
Epidemiology of asthma in children
- Most common cause of wheeze in children
- Affects 1/10 children aged >5
- Boys affected more than girls
- Children can grow out of it
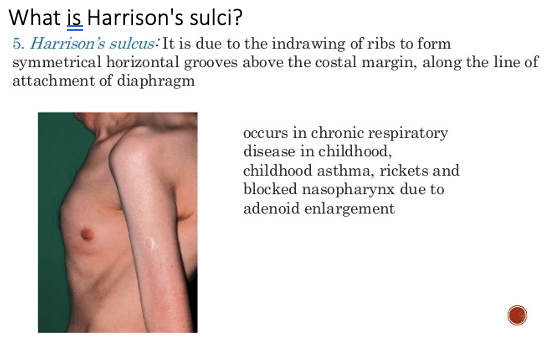
What is Harrison’s sulci?
Why do admissions for acute asthma exacerbations increase in stormy weather?
Thunderstorms cause large amounts of pollen to be released into the air
Diagnosis af childhood asthma
- Diagnosis made on clinical information
- Symptom diaries can be helpful to ascertain the triggers
- Children too young to undergo lung function tests are given a trial of medication and asthma can be diagnosed if the medication relieves symptoms
Overview of asthma management in children
- Medication given follows the pathway used for adults
- Relievers: reverse bronchoconstriction, short acting
- Preventers: inhaled steroids, reduce inflammation and reduce likelihood of bronchoconstriction
- MABs rarely used when symptoms are hard to control
- Inhaler technique checked at every appmt
- Younger children given medication through mask and spacer
- Parents advised to stop smoking
Stepwise management of asthma in children
- Short acting B agonist
- SABA + low dose inhaled CS
- SABA + CS + leukotriene receptor antagonist
- SABA + CS + long acting B agonist (stop leukotriene if not helping - contrast to adult guidelines)
- SABA + mild maintenance and reliever therapy (CS + LABA)
- SABA + moderate dose maintenance and reliever therapy
- SABA + increased ICS to high dose / trial of additional drug e.g. theophylline / refer to specialist
In children <5 years, refer to specialist when trial of leukotriene not successful
Definitions of moderate - severe asthma attacks
2-5 years:
Moderate = >92% sats + no features of severe asthma
Severe = <92%, too breathless to talk, HR >140, RR >40, use of accessory muscles
Life-threatening = <92%, silent chest, poor resp effort, agitation, altered consciousness, cyanosis
>5 years
Moderate: >92% sats, PEF >50%, no features of severe asthma
Severe: <92%, PEF 33-50%, can’t complete sentence, HR >125, RR>30, use of accessory muscles
Life threatening: <92%, <33% PEF, silent chest, poor resp. effort, altered consciousness, cyanosis
Management of mild - moderate acute asthma
Bronchodilator therapy
- give a beta-2 agonist via a spacer (for a child < 3 years use a close-fitting mask)
- give 1 puff every 30-60 seconds up to a maximum of 10 puffs
- if symptoms are not controlled repeat beta-2 agonist and refer to hospital
Steroid therapy
- should be given to all children with an asthma exacerbation
- treatment should be given for 3-5 days
What is cystic fibrosis?
Inherited genetic disorder affecting the lungs and digestive tract
Associated with shortened life expectancy
1 in 25 Caucasian Europeans are carriers of a CF gene with approximately 1 in 2500 live births having CF
Pathophysiology of cystic fibrosis
Mutation in a gene that codes for Cl- channel
Disruption in Cl- movement results in:
- thick mucous in airway
- blocked pancreatic duct >> pancreati insufficiency
- thick mucous in GI tract >> obstruction >> meconium ileus
- thick mucous in biliary tree >> cholestasis
- 98% males are infertile due to congenital absence of vas def
What should be suspected in a child presenting with nasal polyps?
Cystic fibrosis
Investigations for cystic fibrosis
- Chest radiograph: to assess for hyperinflation, there may be evidence of bronchial thickening (undertaken annually as part of annual assessment) Some units undertake CT scanning.
- Chloride sweat test (at diagnosis and annually if in receipt of CFTR potentiator/corrector therapy)
- Microbiological assessment e.g. cough swab/sputum sample (at every clinical encounter)
- Glucose tolerance test (at annual assessment at teenage and beyond)
- Liver function test and coagulation (at annual assessment)
- Bone profile (at annual assessment)
- Lung function testing – spirometry / lung clearance index
Epidemiology and aetiology of cystic fibrosis
- Affects 1/2500-3000 live births
- Rare in Africans and Asians
- Autosomal recessive
- Result from defects in the cystic fibrosis conductance membrane regulator (CFTR) gene - this gene encodes a protein that regulates chloride movement (along with water) across epithelial surfaces
- Defects in the gene cause mucous, sweat and pancreatic cells to produce thick and sticky secretions that damage the lungs and affect the GI tract
- 1/25 people carry one mutation so two people with the recessive allele need to produce an individual with CF
Clinical features of cystic fibrosis
- Respiratory problems
- Persistent wheeze
- Persistent mucous and resulting bronchiectasis
- Bowel problems from birth
- 20% of babies have meconium ileus - bowel obstruction as a result of thickened meconium that cannot be passed
- Thick secretions from the pancreas prevent absorption of fat-soluble vitamins leading to malnourishment and failure to thrive
- Loose-offensive smelling stools
- Usually detected following newborn screening


