Acute Glaucoma
Epidemiology
Aetiology
Clinical Features
Investigations
Treatment
Epidemiology
biological: predominantly Asian females
Aetiology
↑ age / family history / hyperopia / medication (mydratic,eye drops) / pseudoexfoliaton
Clinical Features
abrupt onset of severe eye pain / redness / blurry vision / headaches / nausea / halos around lights / fixed mid-dilated pupil / conjunctival redness / corneal edema
Investigations
gonioscopy (gold standard) / tonometry (>30mmHg)
Treatment
step 1: triad for reducing intraocular pressure
topical timolol / topical pilocarpine / oral or intravenous acetazolamide
step 2: surgical management for improvement aqueous humour outflow
bilateral peripheral iridotomy

Epidemiology
Aetiology
Clinical Features
Investigations
Treatment
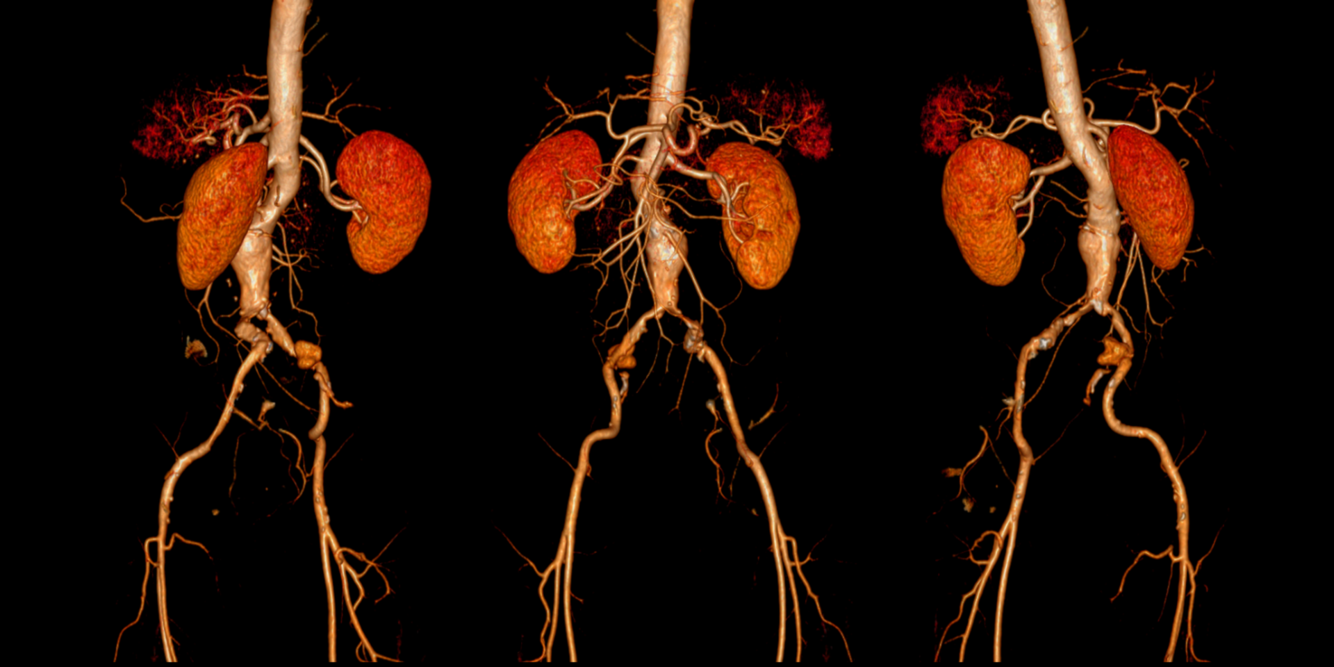
AAA | ABDOMINAL AORTIC ANEURYSM
- Epidemiology:
men>66 / women >70 / European descent
- Aetiology
COPD / family history / hyperlipidaemia / hypertension / smoking / coronary,cerebrovascular or peripheral arterial disease
- Clinical Features
abrupt onset of abdo/back pain, cardiovascular collapse / loss of conciusness
abdo aorta diameter > 3cm (5.5cm high rupture risk)
- AAA more likely to rupture in women than men*
- Investigations
single abdo ultrasound
- Treatment
3-4.4cm | small aneurysm | 12mo rescan
4.5-5.4cm | medium aneurysm | 3mo rescan
>=5.5cm | large aneurysm | refer within 2weeks to vascular surgery for intervention OR EVAR (elective endovascular repair) OR if ruptured open repair
DKA
Aetiology
Clinical Features
Investigations
Treatment
- Aetiology
- Clinical Features
- Investigations
- Treatment
Aetiology
Clinical Features
Investigations
Treatment
Complications

ACUTE COMPARTMENT SYNDROME
- Aetiology
fractures (most common)
other: hemorrhage, crush injuries, vascular puncture, severe circumferential burns / IV drugs / revascularization procedures / poor-fitting casts / ortopaedic intervention combined with patient taking anticoagulants
* Clinical Features
legs + forearm (most common)
early signs: severe deep pain (unless pt had anaesthetic nerve block/epidural)/ swelling / tense muscle compartment / parasthesias
late signs: ↓pulse / anesthesia / function loss / paralysis
- ↑ intracompartmental pressure > perfusion pressure (10-30mmHg) → arteriolar collapse → compromised blood flow*
- Investigations
measurement of intracompartmental pressure ( >20mmHg =abnormal / >40mmHg = diagnostic)
- Treatment
fasciotomy
- Complications
inexperienced clinician = inadequate decompression → myoglobinuria → renal failure (needs aggresive IV fluids)
death of muscle groups (withing 4-6h)

CORD PROLAPSE
Epidemiology/
Aetiology/ risk fx
Clinical Features
Treatment
Complications

Epidemiology
male fetuses predisposed
Aetiology
transverse lie (20% ) / footling breech (15%) / prematurity / abnormality / 2nd twin / multiparity / low birth weight (<2.5kg) / placenta praevia / long umbilical cord / high fetal station
Clinical Features
abdo exam: ill-fitting (one possible cause)
VE: check after rupture of artificial membrane
OVERT : cord can be palpated in vaginal canal
OCCULT: (hesrt rate changes) dropping cord
FUNIC: loops of cord - palpated through membrane
Treatment
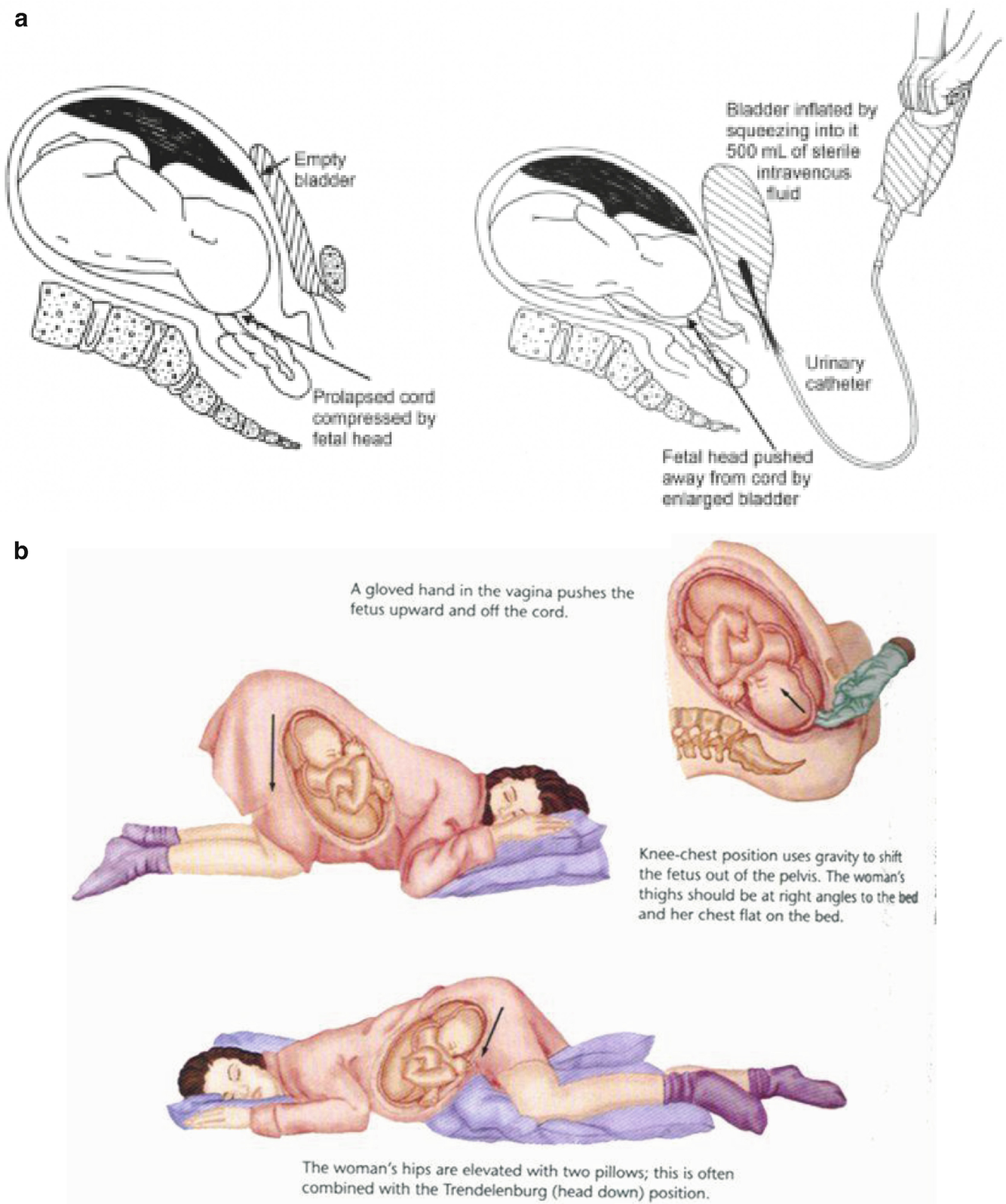
OVERT: 1.oxygen 4-6L/minute
- (see image)
- emergency C-section
- Terbutaline 0.25mg subcutanesouly
- vag delivery only if delivrty imminent (cervix fully dialted)
- ensure resus is available if needed post-delivery
OCCULT: 1. place mom in left lateral position
- fetal herat rate normal = labour with Oxygen admin. + fetal heart rate monitored
- fetal heart rate abnormal = C-section
FUNIC: decision between C-sec. prior to membrane rupture OR ARM (artificial membrane rupture) + prep C-section (in case cord becomes overt
Complications
death
Epidemiology
Aetiology
Clinical Features
Investigations
Treatment
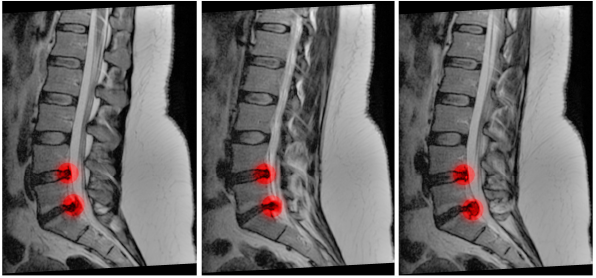
CAUDA EQUINA
- Epidemiology:
RARE
- Aetiology
MOST COMMON: central disc prolapse (usually L4/5 OR L5/S1)
OTHER: tumors / infections (abcess,disctitis) / trauma / haematoma
- Clinical Features
low back pain / bilateral sciatica (50% of cases) / reduced sensation in the perianal area / incontinence (late sign : indicates irreversible damage) / decreased anal tone (good practice to check, however this is not done in primary care)
- Investigations
Urgent MRI
- Treatment
surgical decompression (followed by tests and investigations)
Anaphylaxis
Clinical Features
Treatment
- Clinical Features

Sudden onset and rapid progression of symptoms (most reactions occur over several minutes)
Life-threatening airway and/or breathing and/or circulation problems
Skin and/or mucosal changes (flushing, urticaria, angioedema)
- Treatment
ABCDE approach
NOTES
Adrenaline can be repeated every 5 MINUTES
Best site for IM injection is ANTEROLATERAL aspect of the MIDDLE 3RD of THIGH
Acute Glaucoma
Epidemiology
Aetiology
Clinical Features
Investigations
Treatment
Epidemiology
Aetiology
↑ age / family history / hyperopia / medication (mydratic,eye drops) / pseudoexfoliaton
Clinical Features
abrupt onset of severe eye pain / redness / blurry vision / headaches / nausea / halos around lights / fixed mid-dilated pupil / conjunctival redness / corneal edema
Investigations
gonioscopy (gold standard) / tonometry (>30mmHg)
Treatment
step 1: triad for reducing intraocular pressure
topical timolol / topical pilocarpine / oral or intravenous acetazolamide
step 2: surgical management for improvement aqueous humour outflow
bilateral peripheral iridotomy


