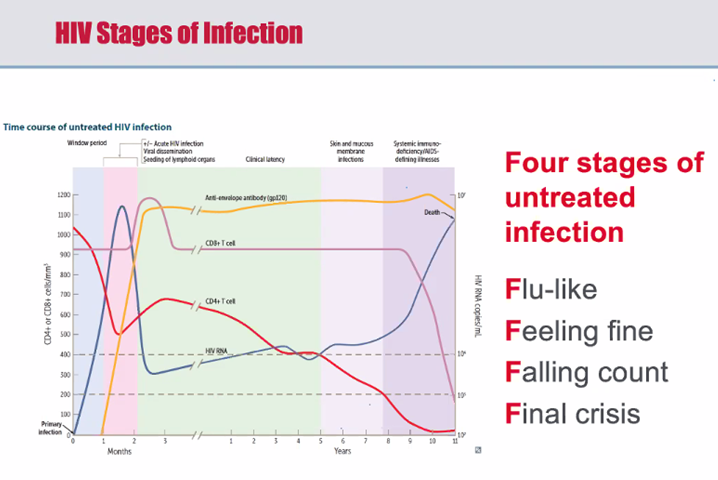
What are the four stages of untreated HIV infection?
- Flu-like
- Feeling fine
- Falling count
- Final crisis
What do ring-enhancing lesions on a head CT in HIV suggest? What do the other images show?
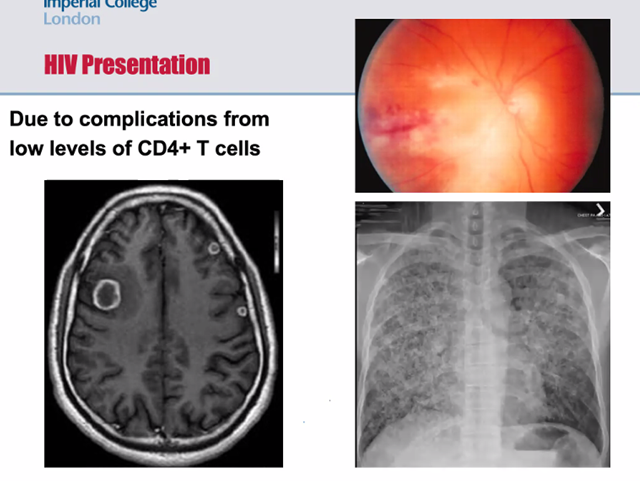
- Head - Toxoplasma gondii (parasite from cat faeces)
- Lungs - reticulonodular shadowing - pneumocystic pneumonia
- Retinal -
HIV also causes hairy leukoplakia - cannot be scraped off unlike candidiasis
Which herpes virus causes Kaposi’s sarcoma?
HHV8
What is the mode of transmission of HIV?
The virus is transmitted via blood, sexual fluids, and breast milk

Define HIV.
HIV is a retrovirus which infects and replicates in human lymphocytes (CD4 +ve T cells) and macrophages
This leads to immune system dysfunction, opportunistic infection, and malignancy = AIDS (acquired immunodeficiency syndrome)
What are the subtypes of HIV?
Virus subtypes include HIV1 (global epidemic) and HIV2 (↓ pathogenic, predominantly West Africa).
How common is HIV? What prevalence in UK? What % is unaware of their infection?
- ~37 million affected worldwide; 1.2 million deaths/yr.
- Africa has most of the disease and mortality
- UK has ~100 000 living with HIV (~1/500)
- 5% of MSM
- ~17% in UK are unaware
What is the pathophysiology of HIV?
- HIV binds via GP120 envelope glycoprotein to CD4 receptors on T helper cells, monocytes, and macrophages
- CD4 cells migrate to lymphoid tissue when the virus replicates, producing millions of new virons
- These are released and in turn infect new CD4 cells
- As infection progresses, depletion or impaired function of CD4 cells leads to low immune function
- HIV is a retrovirus - encodes reverse transcriptase, allowing DNA copies to be produced from viral RNA. This is error prone –> significant mutation rate –> treatment resistance
How does HIV present?
Primary HIV infection
- Symptomatic in 80% - 2-4 weeks after infection - seroconversion illness, acute retroviral syndrome
- Flu-like illness and erythematous/maculopapular rash, fever, myalgia, pharyngitis, mucosal ulceration, headache/aseptic meningitis
- Persistent generalised lymphadenopathy (>1cm in two or more non-contiguous sites but not inguinal for >3 months)
Latent phase - asymptomatic - in latent phase of chronic HIV infection
Late - complications of immune system dysfunction/malignancy
What are the available tests for HIV?
- ELISA for HIV antibody and antigen testing - 4th generation assay test; this reduces “window period” to average ~10days.
- Rapid point-of-care testing -immunoassay kit which gives a rapid result from a finger prick or mouth swab. Only CE-marked kits should be used. Needs serological confirmation.
- Viral load - quantifies HIV RNA. Monitors response to ART. But not diagnostic due to possibility of false positive result. Confirmation of seroconversion is still required in symptomatic primary HIV.
- Nucleic acid testing/viral PCR - tests HIV RNA levels- high in early infection when antibodies might be negative. Used to test vertical transmission.
- CD4 count - not for diagnosis. Monitors immune system function and disease progression. <200cells/microlitre is the defining criteria for AIDS.
Which HIV test is used for testing vertical transmission?
Nucleic acid testing/viral PCR - used to test vertical transmission in neonates as placental transfer of maternal antibodies can affect ELISA antibody testing up to 18months of age.
What can be detected first: antigen or antibody?
Usually antigen
Antibody takes time to make
Why is diagnosis of primary HIV a unique opportunity to prevent transmission?
There is increased viral load and genital shedding - even though HIV antibody testing may be negative, HIV RNA levels are high
What defines AIDS?
CD4 count <200cells/microlitre
What are the three categories of main HIV complications?
Complications:
- complications of immune dysfunction (opportunistic infection/malignancy)
- complicating comorbidity
- complications of treatment i.e. adverse drug events
List 5 different opportunistic diseases associated with HIV.
<500
- Tuberculosis
- Candidiasis - oral/oesophageal
- Kaposi’s sarcoma- tumour defining AIDS and HIV (HHV8)
<200
- Pneumocystis jirovecii →perihilar infiltrates on CXR
- Lymphoma - non-Hodgkin’s
<100
- Cryptococcus neoformans - systemic fungal infection; molluscum like papules
- Cryptosporidium - chronic diarrhoea in pre-ART HIV
- PML
<50
- CMV - causes retinitis, GI ulceration with “owl’s eye” inclusions on biopsy
- MAC
- Toxoplasma gondii - intracranial abscesses especially in AIDS
Summarise the treatment of HIV.
Anti-Retroviral Treatment (ART) - recommended to everyone with HIV regardless of CD4 count
Aims - to reduce viral load to an undetectable level
Consists of two nucleoside reverse transcriptase inhibitors (NRTI e.g. tenofovir and emtricitabine) plus one of
- ritonavir-boosted protease inhibitor - atazanavir
- non-nucleoside reverse transcriptase inhibitor- (NNRTI e.g. efavirenz)
- integrase inhibitor - raltegravir
What are the methods of prevention of HIV infection? (4)
Sexual transmission - use of condoms reduce transmission by 90%; even if both parters are HIV positive this does not protect from treatment resistance, other STIs, hepatitis so serosortic is unreliable.
PEP - post-exposure prophylaxis - short term ART used after potential HIV exposure; can be given up to 72hrs after exposure. First line in UK is Truvada (tenofovir/emtricitabine) and raltegravir for 28 days. Test after 8-12 weeks.
PrEP - pre-exposure prophylaxis - in those at high risk e.g. serodifferent relationships, condomless anal sex in MSM
Vertical transmission - all pregnant women with HIV should have commenced ART by 24 weeks gestation. Caesarean indicated if >50copies/mL viral load. Neonatal PEP given from birth to 4 weeks with formula feeding.
What is the first line PEP regimen? (BASH)
Truvada (tenofovir/emtricitabine) and raltegravir for 28 days. Test after 8-12 weeks.
In order of drugs by mechanism: NRTI/NRTI + II (TDF/FTC + RAL)
How effective is PEP for HIV prevention?
Reduces likelihood of HIV conversion by approximately 80%
Should be initiated within 2 hours and preferably within 24hours
Most efficacious if taken in first 72hrs
What is PrEP? What are the indications?
Pre-exposure prophylaxis:
- MSM
- HIV partner
- IV drug user
- high risk e.g. sex worker
What is the first line PrEP regimen?(BASH)
Daily oral tenofovir/emtricitabine (Truvada)
What is the preferred HIV regimen?
2 NRTI + 3rd drug (NNRTI/boosted PI/integrase)
- e.g. truvada + bictegravir
- OR abacavir + lamivudine + dolutegravir
Quadruple therapy is no more effective than triple therapy.
Sometimes now a two drug regimen of dolutegravir and lamivudine is recommended.
What drug classes for HIV are currently in use?
NRTI- nucleoside reverse transcriptase inhibitors
NNRTI - non-nucleoside reverse tanscriptase inhibitors
Boosted PI - protease inhibitors
INSTI/II - integrase strand transfer inhibitors
Boosters require lower doses of the drug to be required.


