Type I hypersensitivity
- mediators
- examples of conditions
- Ix
- Tx
IgE mediated (anaphylaxis and atopic disease) Involves Mast cells
Ix - skin prick for specific IgE and RAST
Tx
- Antihistamines (decr vasc permeability and bronchoconstriction)
- Corticosteroids (decr inflammation)
- Adrenaline (helps vasoconstrict)
Type II hypersensitivity
Mechanism
Examples of diseases
‘Cytotoxic’, tissue-specific
- Antibody mediated -> target cell damage
- Due to defective ‘central tolerance’
- Due to self-reactive B cells that produce IgM and IgG +/- C’ activation -> attacks healthy host tissue (binds to Ag on host cells) and comes Ag-Ab complex at tissue site
Examples:
- Goodpastures
- Graves
- MG
- Rheumatoid
- Autoimmune haemolytic anaemia
- Haemolytic disease of newborn
- ITP
- Transfusion reactions
Central tolerance
Immune cells that are ‘self-reactive’ are destroyed in primary lymphoid organs (thymus for T cells and bone marrow for B cells)
Type II hypersensitivity: give examples of each
- Complement system activation
- Opsonisation and phagocytosis
- Natural killer cell activation
- Physical presence of Ab at receptor binding site impairs physiologic function
- Goodpastures syndrome -> Ab, C’ activation against collagen in lung and kidneys
- Autoimmune haemolytic anaemia; ABO, Rh-hemolytic disease of newborn
- Pernicious anaemia, guillain barre, Rh fever
- Graves disease (activation of TSH receptor -> hyperthyroidism)
and Myasthaenia Gravis (inhibition of nicotinic Ach receptor )
Type III hypersensitivity
Pathophys
Mediators involved
Examples of diseases
Immune complexes (Ag-Ab complexes) deposit in blood vessel walls causing inflammation and blood vessel damage through complement cascade activation (note C3 and C4 used in large amounts)
ex: SLE = vasculitis in kidneys (glomerulonephritis), joints (arthritis); other forms of glomerulonephritis ; Serum sickness; Farmers lung
Type IV hypersensitivity
- Mediators
- Pathophys
- Examples
T cell mediated (no Ab involved): Reaction occurs in 24-72hrs
- > CD4 (Helper T cells): releases cytokines which attract other immune cells
- > CD8 (Cytotoxic or ‘Killer’ T cells): directly kills things, specific targets
- > Leads to inflammation and tissue damage
Dendritic cell presents Ag to CD4 naive T cell in LNs -> activation/ maturation into Th1 cell which releases cytokines -> attracts other immune cells which leads to local inflammation -> erythema, oedema, fever
CD4+ (helper T cell) mediated:
- Contact dermatitis - Poison ivy and nickel allergy
- Tuberculin skin test (reaction to Mycobacterium tuberculosis protein injection into dermis)
- Multiple sclerosis (myelin)
- IBD (lining of intensive)
- GVHD
CD8+ (Killer T cells) mediated
- Type 1 diabetes mellitus (pancreatic islet cells)
- Hashimotos thyroiditis (thyroid epithelial cells)
- GVHD
Innate immune response
- Speed of response
- Memory?
- Specificity of response
What components?
Non-specific response (responds to molecular patterns ie PAMPs, DAMPs, rather than specific Ag)
Fast! Response in minutes to hours
No memory associated with this response (same reaction to Ag no matter how many times it is exposed)
- Mechanical (cilia, epithelial tight jxns)
- Chemical (ex low pH of stomach acid, enzymes, antibacterial peptides, defensives etc)
- Microbiome
- Cellular: monoctyes, macrophages, Neuts, eosinophils, basophils, mast cells
Adaptive immune response
What cells are involved
Speed of response?
Specificity?
Memory?
Involves B and T cells and immunoglobulins
- Highly specific (generation of 10^23 different T cell receptors)
- Slower response (~2 weeks to peak)
- Generation of memory (enhanced second response)
Relies on cells being primed -> differentiate into the right cell to fight that specific pathogen
Takes a few weeks
Immunologic memory -> clonal expansion of immune cells to fight the infection. on destruction of the pathogen, some of the clonal cells become plasma cells which on subsequent exposure undergo clonal expansions such that the immune response is much faster and stronger
Myeloid progenitor cells
Where are they made?
What cells do they differentiate into?
Made in bone marrow
Granulocytes
- Neutrophils
- Eosinophils
- Basophils
- Mast cells
Dendritic cells
Macrophages
Monocytes
Monocytes - function/role and what cells do they differentiate into?
Phagocytic/Ag presenting/produce cytokines
Differentiate into macrophages and dendritic cells
Dendritic cells
- role/purpose
Phagocytic/Ag presenting/produce cytokines:
Present Ag to T cells
- This connects innate to adaptive immune systems
Macrophages
Phagocytic (eat dead cells, invading pathogens)
and APC
-> Present Ag to T cells (This connects innate to adaptive immune systems)
Neutrophils
-> degranulate to produce free radicals -> direct killing
Eosinophils
-> degranulate to produce histamines and cytokines (allergy/parasites)
Mast cells
-> involved in asthma and allergic responses
Basophils
-> degranulate to produce histamine and cytokines (allergy)
Lymphoid progenitor cells
Made in bone marrow
- NK cells
- T cells
- B cells
NK cells
(innate)
Complete development in bone marrow.
Degranulate to produce cytotoxic molecules that directly kill the target cell via apoptosis
Specifically against viruses
B cells
- Adaptive immunity
- Complete development in bone marrow
- Live in lymph nodes
- Bind to Ag -> present the Ag on their surface -> displays the Ag to T cells -> activates T cells which help the B cell turn into a plasma cell which can produce lots and lots of antibodies (IgM/G/E/A) against that particular Ag
- Those Abs circulate in the blood
- This process takes a few weeks
Can turn into memory B cells for subsequent exposure
T cells
Adaptive immunity
- Completes development in thymus
- Naive T cells are presented an Antigen which leads it to become ‘primed’ and differentiate into
1. CD4 T cells = helper t cell, secretes cytokines that coordinate immune response against that Ag
2. CD8 T cells = cytotoxic (kill target cells)
Can turn into memory T cells for subsequent exposure
Where to B and T cells develop?
Common lymphoid progenitor cell
- > becomes immature B cell in bone marrow, then travels to spleen to become mature plasma cell -> secrets B cell receptors
- > some travel to thymus to differentiate into T cells
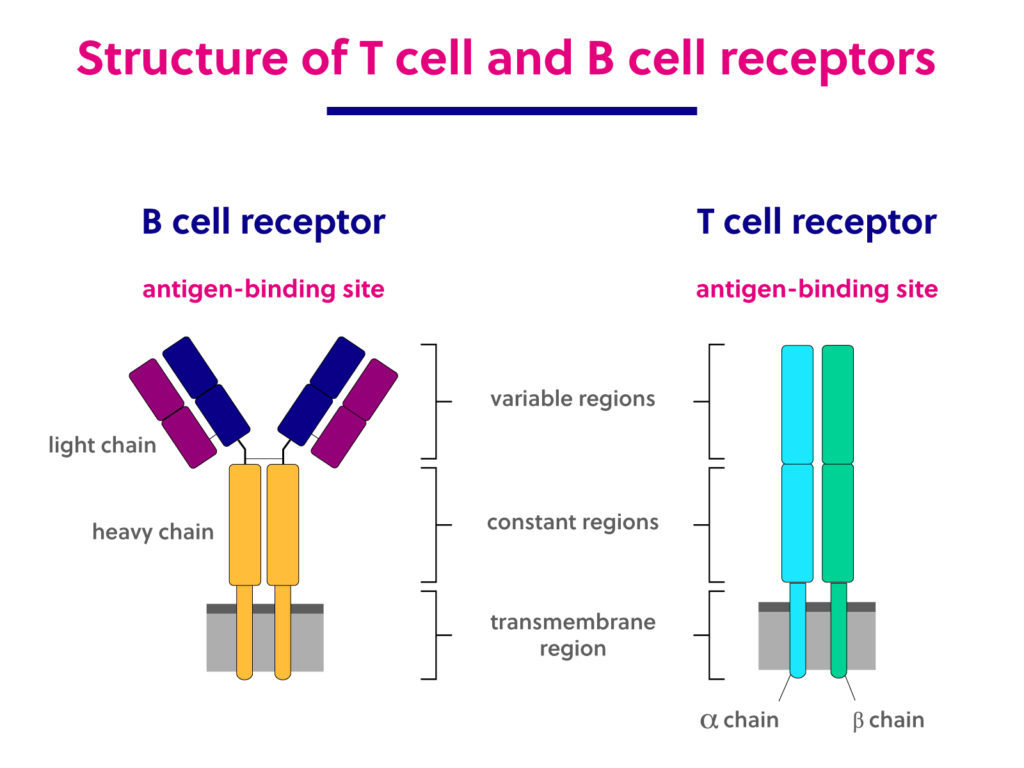
What part of the B cell receptor encodes the type of Ig it is?
The heavy chain genes encode this
What are the five types of Ig and what is the main role of each class?
IgM - 1st response -> activates C’ pathway most effectively
and doesn’t require T cell help
IgG - memory
- opsonisation + classical C’ pathway
IgA - acts at mucosal sites to prevent pathogens entering body
opsonisation
IgE - allergy mediator, induced by IL4, triggers granulocytosis of mast cells, eosinophils, basophils
IgD- helps mature B cells leave bone marrow
what is the main role of each class of Ig?
IgM
IgG
IgA
IgE
IgD
IgM - 1st response -> activates C’ pathway most effectively
and doesn’t require T cell help
IgG - memory
- opsonisation + classical C’ pathway
IgA - acts at mucosal sites to prevent pathogens entering body
opsonisation
IgE - allergy mediator, induced by IL4, triggers granulocytosis of mast cells, eosinophils, basophils
IgD- helps mature B cells leave bone marrow






