during fetal develop, the foregut, midgut and hindgut develop from what?
foregut: perotineum develops from ventral mesogastrium & dorsal mesogastrium:
i) the liver develops within the ventral mesogastrium. it exapnds
ii) dorsal mesogastrium: spleen develops in it,
get shift from
midgut & hindgut develop from dorsal mesogastrium
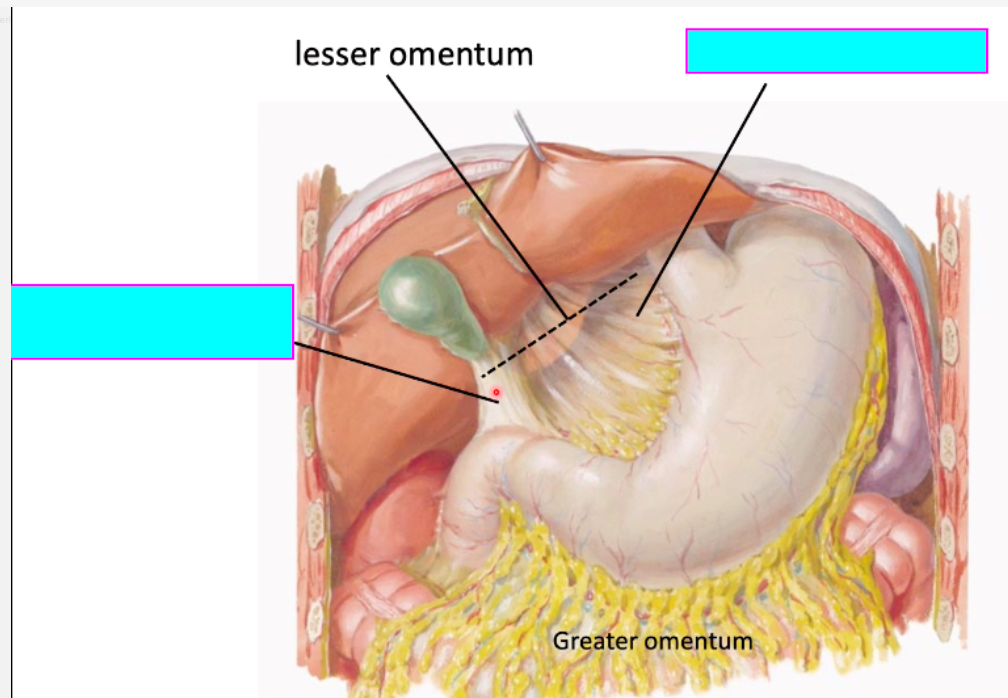
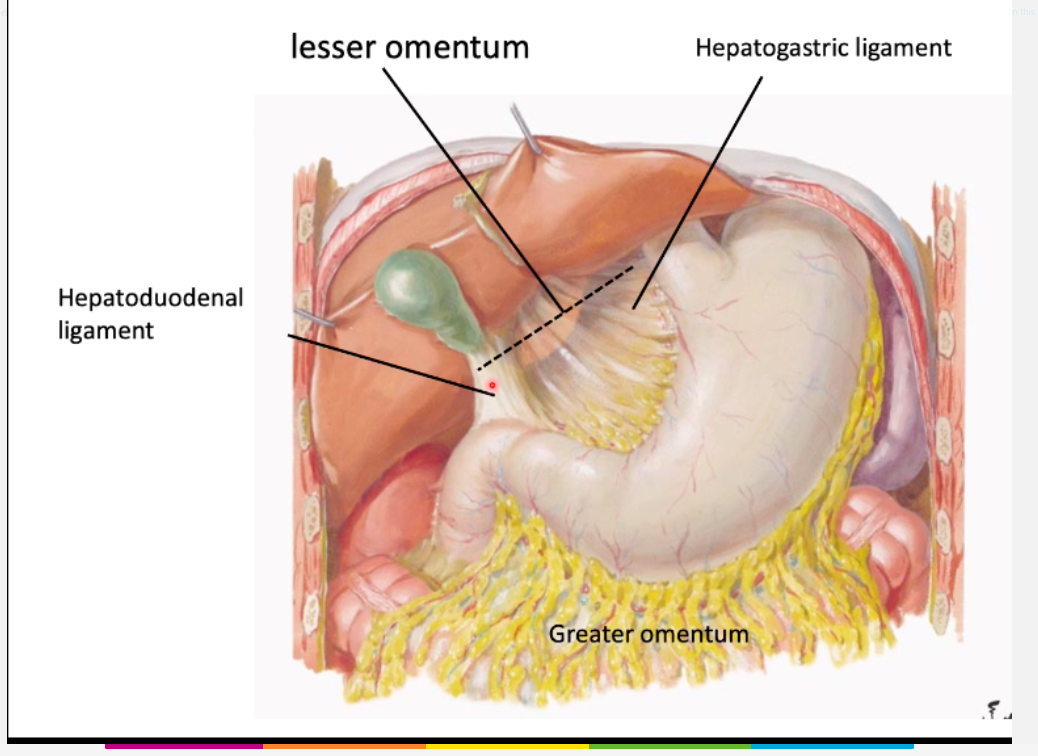
the dorsal mesogastrium forms connections between which structures? [2]
dorsal mesogastrium forms connections between:
stomach & spleen [1]
spleen and posterior ab. wall [1]
which three strucutres do you find in the free border of the lesser omentum?
- bile duct
- hepatic artery proper
- hepatic portal vein
which arteries do u find in the greater omentum?
= gastroepiploic arteries
where do u find the potential spaces in body? [2]
- *subphrenic recesses:**
- divided into L&R by falciform ligament
- *subhepatic recesses:**
- lesser sac on L
- hepatorenal recesss / pouch of morrison on the R
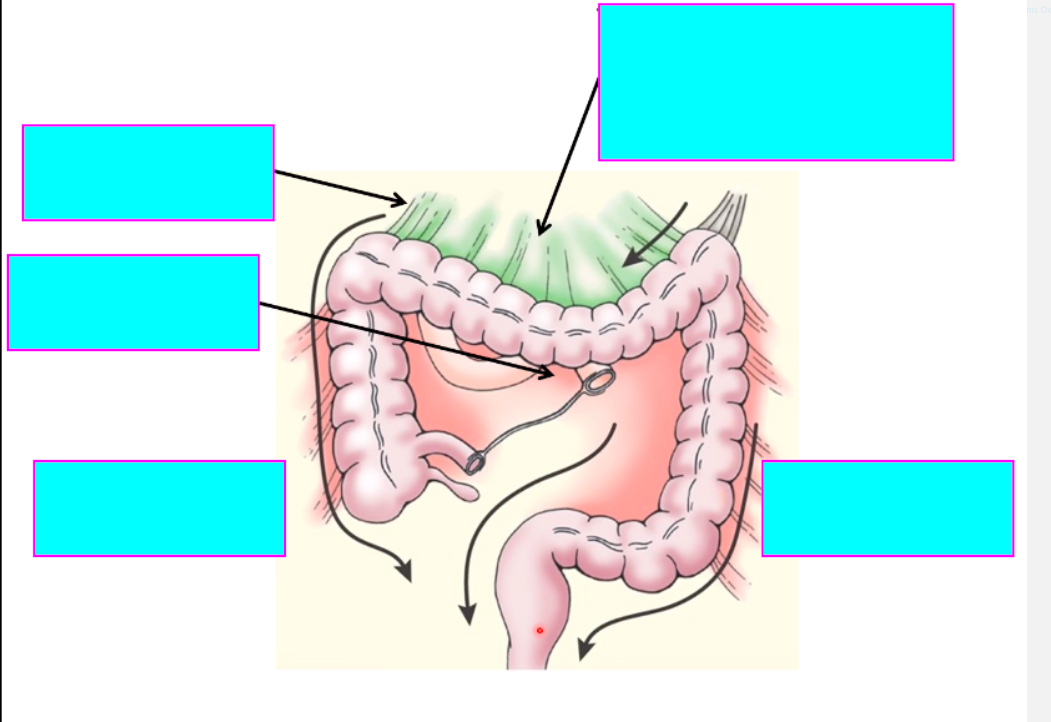
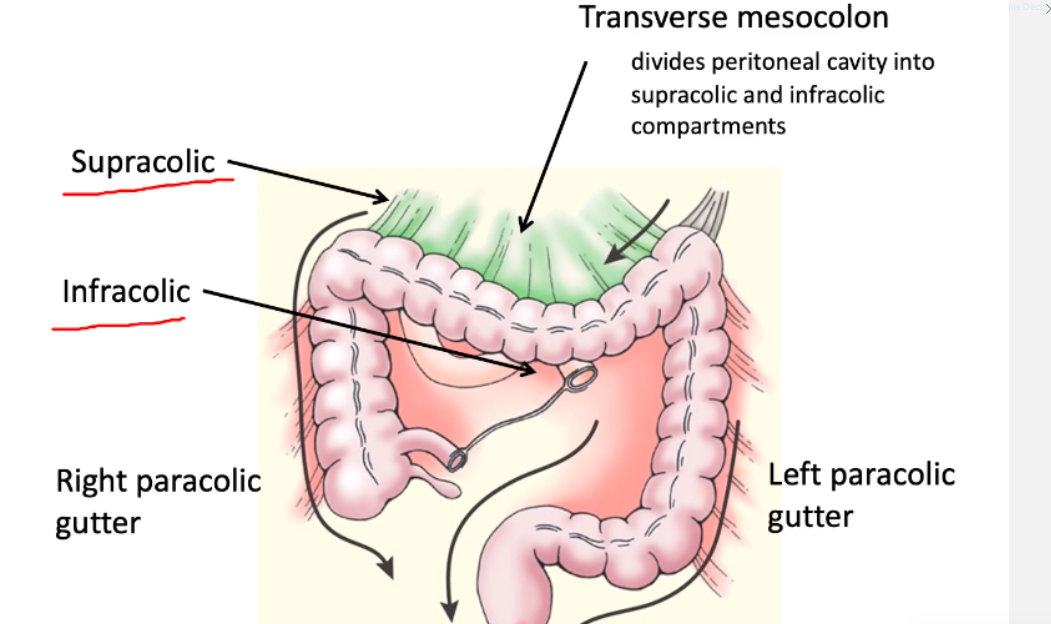
Q
whats the difference between primary or secondary strucutres?
give e.g.s
primary retroperitoneal srtuctures:
develop along posterior peritoneal wall & stay !
-great vessesl
- kidneys
- ureter
- lower rectum / anal canal
secondary retriperitoneal structures:
develop intrapetrioneally but move retro
- pancreas
- distal parts of duo
- upper rectum
what is v general overview of role of:
chylmicron
VLDL
IDL
LDL
HDL
- *chylomicron**: fat transport from GI tract –> rest of body
- *very low density lipo:** (similar to chylomicrons) fat transport -> rest of body. VLDL produced in the liver
- *intermediate DL**: left over chylomicrons –> become either LDL or VLDL
LDL: deliver cholesterol to cells
HDL; pick up excess cholesterol and send back to liver
what is the function of lipoprotein lipase?
what activates lipoprotein lipase?
where is lipoprotein lipase most active:
a) during periods of starvation?
b) after a meal
lipoprotein lipase: breaks down fats from inside lipoproteins and carries them into the cells
activated by: Apo C2
where is lipoprotein lipase most active:
a) during periods of starvation: muscle (where FA being used for energy in TCA)
b) after a meal: adipose cells (to form fat)
what is the function of low density liporpotein?
where AND how made? (which enzyme)
low density lipoprotein:
- function: deliver cholesterol to peripheral cells of the body
- produced @: liver
- formed by: remains of VLDLS after distribiting most of triglycerides. causes them to be more dense = IDLS. hepatic TAG ligase converts IDL to cholesterol rich LDL, having only Apo B100
what is familial hypercholeserolemia ? caused by mutation of which 3 genes?
- autosomal dom disease. mutation of one of three genes:
i) LDLR - receptor for receptor mediated endocytosis
ii) PCSK9: kinase that controls recyclingof LDLRs
iii) APOB: gene for ApoB which binds to LDL
= causes increased levels of cicrulating blood LDL bc not taken up into cells. increases chance of CHD.
causes heart attacks even in children
how can ur body create cholesterol? (which enzyme)
how does high cholesterol induce negative feedback of cholesetol production? (3)
- acetyl co-A –> cholesterol (via enzyme HMG-coA reductase)
high cholesterol induces negative feedback of cholesetol production
- *- reduces expression of HMG co-A reductase
- reduced gene expression of LDL (which brings the cholesterol)
- XS stored as cholesterol esters**
explain how having high LDLs leads to the formation of plaque formation & atherosclerosis
- high LDLs stay in blood system become damaged due to ROSs
- damaged LDLs get taken up by macrophages
- but bc there isnt anything really to kill - theyre just cholesterol: macrophages become foam cells (filled with chol)
- foam cells stick to walls of capillaries - fatty streaks -> fatty plaques -> atherosclerosis
explain mech. of HDLs reducing body cholesterol
- reverse transport pathway:
i) ApoA1 released by liver -> goes around body and picks up cholesterols from other cells through ABCA1 / G1 receptors
ii) changes the cholesterol -> cholesterol esters
iii) goes back to liver
iv) HDL transfers XS cholesterol ester to liver by binding to scavenger receptors (SR-B1)
explain the two ways statins reduce blood chol levels
- statins block the activity of HMG-Co A reductase. so less cholesterol is made [1]
causes more LDL receptors to be made & take in MORE LDLs -> reducing blood LDLs [1]
which lipoprotein carries fats from the liver to peripheral cells?
chylomicron
very low density lipo
intermediate DL
LDL
HDL
which lipoprotein carries fats from the liver to peripheral cells?
chylomicron
very low density lipo
intermediate DL
LDL
HDL
name two differences in the structure of HDLs & LDLs [2]
name two differences in the structure of HDLs & LDLs [2]
- Low-density lipoproteins contain **B-100 proteins
- HDL particles contain mostlyA-I and A-II proteins. high protein content, low fat cotent**
sources of endogenous reactive species? [3]
endogenous sources: mito, peroxisomes, ER
which micronutrient is important in imprinting home to the gut mucosa from peyers patches?
how does it occur (2)
vitmain A: precursor for retinoic acid !
- gut dendritic cells use retinoic acid to inform the niave T cells
- causes niave T cells to change transcription to express CCR9 & a4B& to do gut honing
which population are micronutrients most important in?
WHY? (3)
most important in paediatric population: (body growth & development; energy supply; healthy infants have 3x energy per kg body weights than adults)
which vitamins can be stored? how? where?
- *fat soluble: A D E K -**> can be stored in liver (but can be toxic in XS)
- absorbed with fats (readily absorb in micelles & chylomicrons)
why is commensal bacteria gut overgrowth clinically significant regarding vitamins?
commensal bacteria: providers AND consumers of B vitamins & vitamin K.
overgrowth: likely to have B12 deficiency & high B9
what are the clinical features of deficiences in
vitamin A
vitamin D
vitamin E
vitamin K
(fat soluble vitamins)
vitamin A: eyes -> xeropthalmia (Xerophthalmia refers to the spectrum of ocular disease caused by severe Vitamin A deficiency (VAD))
vitamin D: rickets (in adults = osteomalacia)
vitamin E: peripheral neuropathy
vitamin K: coagulopathy

















