* what is the net gain / loss of ATP during: *
a) glycolysis?
b) TCA cycle?
c) cori cycle?
what is the net gain / loss of ATP during:
a) glycolysis: Net 2 ATP gain via susbtrate level phosphorylation
b) TCA cycle: Net 38 ATP gain via oxidative phosphorylation
c) cori cycle: Net 4 loss . Anaerobic
to make glucose, you need a source of energy and carbon units.
what are 3 sources of carbon that can be used in gluceoneogenesis?
what are 2 sources of energy that can be used in gluceoneogenesis?
- *sources of carbon:**
- lactate (from muscle - glycolysis). exported to liver can be made into pyruvate as a carbon source
- amino acids - from muscle. (from proteolysis) sent to liver & can be made into pyruvate as a carbon source
- glycerol (from lipolysis). sent to liver
- *sources of energy:**
- ATP (from glycolysis and Krebs cycle)
- fatty acids (but cannot be used as C source !!)
what are the 3 steps of glycolysis that are metabolically irrervisble and need to be side stepped to in order to produce glucose in gluconeogenesis?
3 irreversible steps are in glycolysis:
- *1. Glucose –> glucose-6-phosphate.
2. P + fructose-6-phosphate –> fructose-1-6-bisphosphate.
3. pyruvate -> PEP (complicated)**
enyzmes used to reverse ^^ reactions:
- enzyme = gluocse-6-phosphatase (removes the P)
- enzyme = fructose, 1,-6-biphosphatase
- enzyme = (more complicated -> will come to later)
Acetyl co-A is a product of of fatty acid break down.
how do high levels of acetyl co-a influence gluconeogenesis?
high levels of Acetyl Co-A:
activates pyruvate carboxylase (used in step 1 of malate cycle: drives gluconeogenesis from pyruuvate -> PEP & eventually glucose)
inhibits: pyruvate dehydrogenase complex (prevents pyruvate being turned into acteyl co A & sparing it, leaving for gluconeogenesis)
the cori cycle spares pyruvate be ensuring that pyruvate is NOT converted to what?
where is a source of ^ instead?
the cori cycle only works if you conserve pyruvate, by removing it from muscle and recycling in the liver. cori cycle has to avoid pyruvate’s conversion to acetyl Co-A
INSTEAD
fatty acid metabolism produces acetyl co-A, creating another source of acetyl co-A & means that cori cycle can go ahead for gluconeogenesis. otherwise the pyrvate from cori cycle would be used to make actetly co-A . good thing !!
gluconeogensis from glycerol:
what is glycerol converted to? what does this get converted to?
where? (2)
- glycerol is converted to dihydroxyacetone phosphate only in the liver & kidneys
- dihydroxyacetone phosphate then reacts with glyceraldehyde-3-phosphate to produce fructose-1,6, bisphosphate (and from there .. = fructose-6-phosphate -> glucose-6-phosphate -> glucose)
Q
specifically, how is gluconeogensis controlled by:
- insulin?
- glucagon?
- adrenaline?
(.i.e. which enzymes blocked etc)
- *insulin:**
- inhibits gluconeogensis
- insulin dephosphorylates pyruvate dehydrogenase. this makes pyruvate dehydrogenase active & converts pyruvate -> acetyl coA, which enters krebs cycle. pyruvate is therefore not available to be made into glucose
- *glucagon & adrenaline:**
- promotes gluconeogensis
- glucagon increases cAMP levels. this causes pyruvate dehydrogenase to be phosphorlayed (by pyruvate dehydrogenase kinase) & inactive. pyruvate is then available for glucose production
explain how diabetes disrupts gluconeogensis pathway ox
insulin doesnt work:
SO
- pyruvate dehydrogenase remains phosphorylated & therefore inactive
- = less acetyl co-A to go into krebs cycle from pyruvate
- instead fats are broken down to produce fatty acids & acetyl co-A & goes into krebs cycle instead
- means that pyruvate is available for gluconeogenesis
which a.a are main glucogenic a.a? [2]
which a.a are ketogenic?
glucogenic amino acids: **alanine & gluatamine
lysine and leucine**
are ketogenic
which cells regulate water contents in the gut?
what is the mechanism of this?
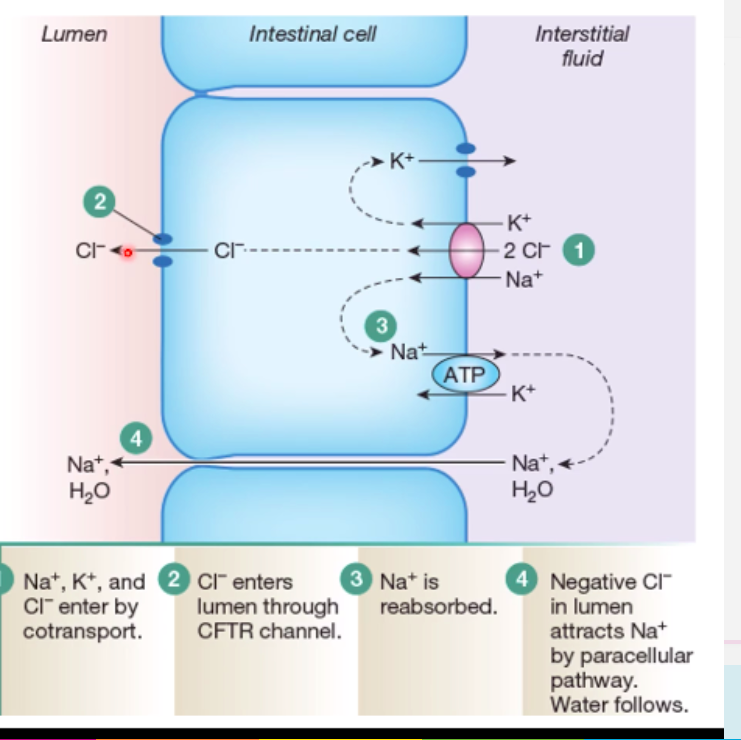
secretory cells of the intestinal crpyts:
- CFTR channel within these cells controls this:
a) Cl- moves from ECF via Na/K/CL2 cotransporter (as does Na & K)
b) Cl- enters lumen through CFTR channel
c) Na+ is reabsorbed via Na/K ATPase
d) negative Cl- in lumen attracts Na by paracellular pathway (through cell gaps)
e) water follows the Na into the lumen
how does cholera effect the secretory cells of the crypts?
- Vibrio cholerae releases toxins: has a Part A & Part B
- Part A incorporated into cell. binds to adenylate cyclase, which in turn makes more cAMP
- too much cAMP triggers CFTR to be constantly open AND blocks Na/CL symporter (so lots of Cl- is leaving cell and is not being reimbursed)
- Cl leaves cell into gut = water follows
= secretory diarrhoea
Q
what is MoA for when ORS treats cholera?
ORS MoA:
- ORS has Na, glucose and AA in it.
- Na & Gluocse transporters are still working with cholera
- Na prefers to be in ECF: leaves crpyt secretory cells
- *- pumped out via Na/K ATPase into ECF
- water follows = save wate**
what is hyperglycemia - why is it bad? explain the mechanism
hyperglycemia = high blood glucose
why bad?
- plasma and interstitial fluid is baso at equilibrium
- so high blood glucse = high interstitial glucose
- ECF Na & new glucose has high osmotic power = draws water from ICF (the cell) via aquaporins
- the water dilutes the Na & bit of glucose = hyponatraemia :( (low serum Na)
- kidneys: reabsorb Na BUT if too much glucose = excreted in urine.
- gluocose in urine has osmotic draw -> get osmotic diursesis bc water follows the glucose
= server water loss !
what can the following causes of oedema be caused by?
- increased capillary hydrostatic pressure
- loss of plasma proteins (2)
- increased capillary hydrostatic pressure = cirhosis causing portal hypertension
- loss of plasma proteins - severe malnutritrion (protein malnutrition like kwashiokor) & liver disease


gastric epithelial cells
- parietal cells produce HCl. But HCl is actually quite toxic. how does the body cell overcome this issue of not causing self harm via the HCl? (2)
1. HCl is only produced when food is in the stomach = get unstimualted and stimulated parietal cells:
a) unstimulated parietal cells have H+ ATPase Pumps in the cytosol
b) stimulated parietal cells have H+ ATPase Pumps on apical surface
- *2. surface mucus cells secrete mucus**
- without mucus = would directly interact with cells
- mucus works as:
a) physical barrier; gel layer
b) chemical barrier; bicarbonate
which cells produce gastrin?
when do cells produce gastrin?
where are they?
why is gastrin produced?
produced by: G cells !! g 4 gastrin xox
located @ atrium of stomach -> bc at the bottom of the stomach. if they sense that there are big proteins - stimulate the formation of more acid.
BUT HOW COMMUNICATE to the other cells?
- gastrin produced and excreted into blood. = therefore a hormone ! (endocrine activity)
- goes to ECL and parietal cells
what are 3 medical options for GORD?
why do u have to be careful if taking NSAIDS with GORD / GERD? (2)
- inhibited by PPI
- block the H2 receptor: (cant target others bc the receptors are so common)
- neutralised by antacids: form a protective raft over acid pockets
- NSAIDs: block the prostoglandins from binding to prostaglandin receptors on the parietal cells = means that body’s natural inhibitor is blocked :(.
- *- will cause less mucous and bicarbonate secretion :(**
how does Helicobacter pylori cause a peptic ulcer? (4)
- H. pylori produces urea in stomach.
- urea turns into NH3: as a result: 1. raises acid. 2. degels the mucin (lose mucous layer)
- builds up
- eventually mucin layer removed and mucosal damage is caused by the pepsin and H+ of HCl :(
which cells do you find in the body of stomach? [3]
which cells do you find in the antrum of stomach? [3]
which cells do you find in the body of stomach: parietal cells, chief cells, D cells
which cells do you find in the antrum of stomach: G cells, mucous cells, D cells
* MESS NOTES *
describe the differences of pH within the stomach and why they occur
cell surface = pH 7: HCO3- layer neutralises stomach acid = chemical barrier
then
mucous layer: physical barrier
then
stomach acid = pH 2
explain a) hormonal control of intestinal stage of stomach acid secretions xo
b) nervous control
Primarily inhibits gastric acid secretion when FOOD AND ACID ENTERS THE INTESTINES
NERVOUS CONTROL:
- *It signals the sympathetic system to stop gastric secretions**
- Inhibition of parietal and chief cells
HORMONAL CONTROL:
- *- Cholecystokinin, secretin and GIP (gastric inhibitory protein) produced by duodenum –> inhibit gastric secretions**
- Cholecystokinin and GIP released by presence of lipids and carbohydrates
- Secretin released when pH decreases (due to entrance of acidic chyme into the duodenum)
How can you diagnose H. pylori presence? (4)
- urea breath test: urea C13 is given to patient and H. pylori converts urea C13 to NH3 + C1302
- CLO test (Campylobacter-like organism test) : biopsy placed in media with urea and pH indicator conversion of urea to ammonia raises pH - changes colour
- blood antibody test
- stool antigen test
Acetyl Co-A is one of the starting molecules needed for TCA. But what is the equation for the formation of Acetyl Co-A from pyruvate?
what is the enzyme used to catalyse this reaction?
what nutrition is needed for this reaction?
- pyruvate + CoA + NAD+ –> acetyl Co-A + Co2 + NADH
- enzyme: pyruvate dehydrogenase (PDH)
- co-enzymes are members of the B-vitamin family. uses TPP (aka vitamin B1)




