How is the diagnosis of dementia made?
The history and Clinical assessment indicates significant cognitive impairment in at least one (1) of the following:
- Learning and memory
- Language
- Executive function
- Complex attention
- Perceptual-motor function
- Social cognition
Impairment must be acquired and interfere with independence in normal activities. In the case of neurodegenerative dementia’s (Alzheimer’s), there is an insidious, progressive course. There is no other cause found for the disturbances (i.e. schizophrenia, etc.).
What 3 diseases cause cerebral degeneration?
- Alzheimer’s disease
- Parkinson’s disease
- Huntington’s Disease- less common
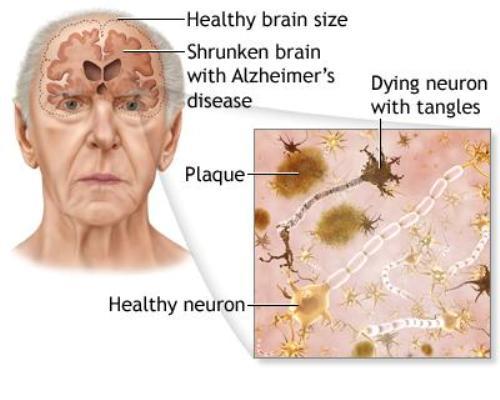
Describe Alzheimer’s type dementia
1. Most common form of dementia in elderly population
- Accounts for 60-80% of cases
- Neuronal damage is irreversible
- Histopathology: amyloid plaques, neurofibrillary tangles and degeneration of cholinergic neurons in the hippocampus and cerebral cortex- causes neuronal death.
- Results in cerebral atrophy on advanced radiologic imaging scans
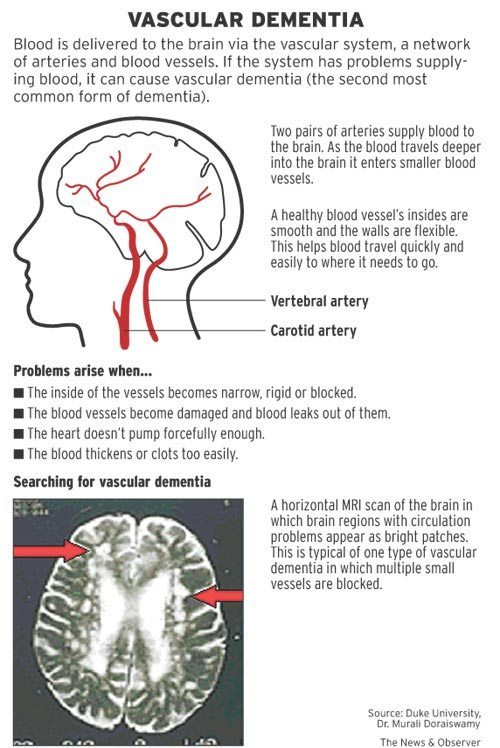
What causes vascular dementia?
Dementia that results from the death of neurons as a result of disruption of blood flow; diseased blood vessels (as in DM, HTN, Hypercholesterolemia) greatly pre-dispose to vascular dementia; CT head commonly shows white matter changes and evidence of infarcts:
- Multi-infarct dementia
- Stroke
- Arteritis
What infections can cause dementia?
- HIV/AIDs
- Syphilis
- Meningitis
- Encephalitis
- Abscess
- Creutzfeldt-Jakob disease
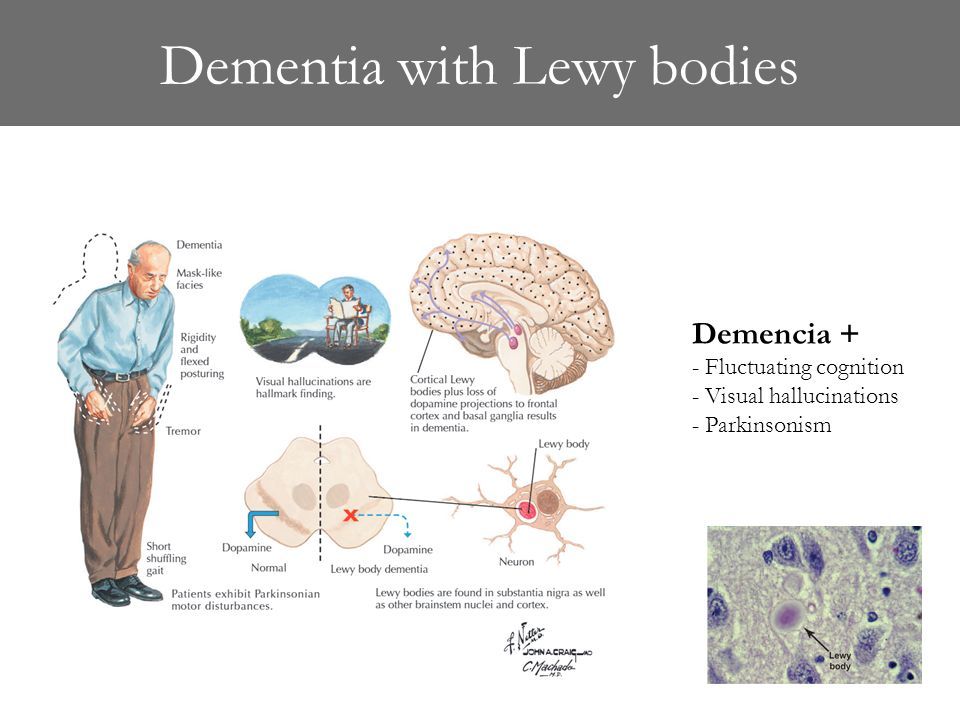
What is lewy body dementia?
- 2nd most common type of dementia
- Characterized by the presence of Lewy Body-like inclusions with neurons
- Gradual death and decline of brain cells; low levels of acetylcholine and dopamine observed;
- Distinctive features include: visual hallucinations, Parkinsonism movement disorders, cognitive fluctuations, dysautonomia, sleep disorders and neuroleptic sensitivity.
- Lewy Body dementia can be difficult to distinguish from Alzheimer’s with Parkinson’s disease
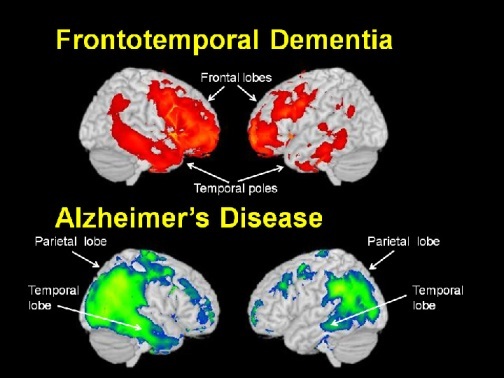
What is frontotemporal dementia?
- highly heritable-autosomal dominant (10-25% of patients) rare cause of dementia
- mean age of onset 58 years
- symptoms develop as a result of degeneration of the frontotemporal regions of the brain
- characterized by changes in personality, behavior and difficulty using and understanding language, loss of inhibition and empathy, development of repetitive behavior, in early stages;
- frontotemporal dementia patients have a relatively preserved short-term memory compared to Alzheimer’s
- later stages whole brain atrophy gives similar picture to AD
What are the signs and symptoms of dementia?
A. Insidious onset- progressive over years many times
B. Confusion/memory deficits
C. Language difficulties
D. Impaired abstract reasoning
E. Disorientation
F. Difficulty with learned tasks- ADLs
G. Agitation, anxiety, sleeplessness
H. Personality changes
I. Difficulty recognizing family/friends
J. Severe symptoms: loss of speech, appetite, weight loss, bladder/bowel incontinence, total care needs

What laboratory/diagnostic tests are used to diagnose dementia?
Tests:
Initial approach focuses on patient history, drug history, and use of cognition impairing medications.
Cognitive testing- Folstein Mini-Mental State Examination for screening of dementia
- Maximum score is 30
- Score of < 23 indicates cognitive impairment
- LOCAM-LT is mnemonic for Folstein components
L = level of consciousness
O = orientation
C = concentration/calculation
A = attention
M = memory
L = language
T = thought process
- Repeat cognitive testing every 3-6 months to document progression of disease over time
- Mini-cognitive test: Recall three unrelated words, clock-drawing task
Labs:
- Electrolytes/glucose/magnesium/calcium
- Liver function tests/albumin
- B12 level
- BUN/creatinine
- Thyroid function tests
- VDRL (venereal disease research laboratory test)
- HIV if indicated
- CBC
- Pan cultures (urine, blood, sputum)
- Drug screen
Imaging:
- CT of head or MRI head- to exclude or include tumor/subdural hematoma, infarction,hemorrhage, hydrocephalus, atrophy
- Lumbar puncture – r/o meningitis, neurosyphilis, normal pressure hydrocephalus
- Electroencephalography (EEG)
- Chest x-ray (CXR) – r/o CHF, lung disease, pulmonary embolism (PE), infection
- Electrocardiogram (EKG)
How do you manage a patient with dementia?
A. Supportive care, Social service consult, skilled nursing, long term care referral
B. Reduce or stop all non-essential medications.
C. Dietary consult- maintain nutrition
D. Avoid restraints if at all possible
E. Physical therapy/speech therapy as indicated
F. Screen for safety issues- fall precautions, cooking, wandering, driving
What medications are used for patients with dementia?
Cholinesterase inhibitors: offer the greatest benefit in patients with mild to moderate cognitive impairment; AD patients have reduced cerebral content of choline acetyltransferase, which leads to a decrease in acetylcholine synthesis and impaired cortical cholinergic function.
a. Donepezil (Aricept) 5mg at bedtime; titrate to 10mg daily at 4-6 weeks ; max dose 23mg. DRUG OF CHOICE; monitor for AV block, syncope, seizures, obtain baseline EKG prior to initiation of treatment
b Rivastigmine (Exelon) – monitor for hypotension, syncope and significant weight loss
c. Galantamine hydrobromide (Razadyne) – avoid if hepatic/renal impairment present or patients with cardiac conduction defects.
How is Memantine (Namenda) used in dementia?
- works to prevent progression of AD (neuroprotective); initiate with 7mg po daily; titrate in 7 mg increments of at least 1 week as tolerated to a target dose of 28 mg daily; max dose 28mg daily.
- Reduce for renal insufficiency; greater efficacy when paired with cholinesterase inhibitor; monitor for Stevens –Johnson Syndrome
When are atypical antipsychotics used in patients with dementia?
Preferred treatment for dementia related aggression and agitation in elderly patients.
a. Olanzapine (Zyprexa)
b. Quetiapine (Seroquel)
c. Risperidone (Risperdal)
d. Ziprasidone (Geodon)
How are benzodiazepines used in patients with dementia?
Oftenpreferred when controlling agitation and aggression
a. Clonazepam (Klonopin) – use cautiously; may cause paradoxical agitation or increase risk of falls or injury
b. Lorazepam (Ativan) – IV as needed


