Define puberty and its age of onset in females and males
The process of acquiring physiological mechanisms for reproductive competence.
First capable of sexual reproduction of offspring.
Females: 8 - 13 y/o
Males: 9 - 14 y/o
Distinguish the physical changes occuring during puberty
Development of secondary sexual characteristsics
- Growth of pubic hair (axillary and groin)
- Development of the breast tissue in females
- Development of the genitals in males
Outline the stages of puberty observed in females and the associated hormone
- Thelarche: Development of the breasts. Associated with oestrogen. 9 y/o
- Pubarche: Growth of pubic and axillary hair. Associated with androgens (adrenarche). 12.5 y/o
- Growth spurt: Skeletal growth, muscle mass and organ growth. Associated with oestrogen.
- Menarche: Observed 2-3 years after thelarche. Commencing menses. Associated with oestradiol.
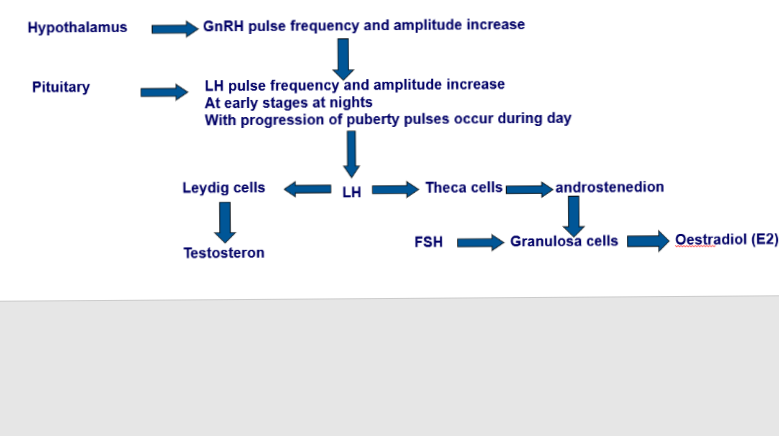
Describe the hormonal changes that take places during puberty in males and females
- Pulsatile release of GnRH increases at the beginning of puberty
- The hypothalamus and anterior pituitary gland become less sensitive to negative feedback, allowing for increased synthesis of oestrogen and progesterone
- Prior to puberty GnRH release is suppressed by neural control and negative feedback loops, this prevents the onset of puberty
Outline Gonadarche
Describes the activation of the gonads (ovaries/testes) by FSH and LH.
Prompts the release of oestrogen/testosterone.
This allows for sexual maturation.
Outline Adrenarche
The development of the zona reticularis of the adrenal cortex. Allows for the synthesis of androgens. Androgen production prompts the growth of axillary and pubic hair and also the development of acne.
This process begins before 8 y/o
Describe the regulation of the onset of puberty
- Hormonal: Pulsatile of release of GnRH increases, increasing FSH and LH secretion and their associated sex hormones. The hypothalamus and anterior pituitary become less sensitive to negative feedback, further increasing sex hormoen synthesis.
- Neural: The balance of promoting and inhibitory factors determines onset. Glial cells affect GnRH through growth factor dependent cell-to-cell signalling.
- Metabolic: Changes in metabolism may influence neural control of puberty onset.
Leptin levels: Increase at the beginning of puberty. Plateau at Tanner stage 2 in boys and then decrease. Levels continue to increase in girls.
Outline abnormal puberty
Precocious puberty: Early onset of puberty. Before 8 y/o in girls and 9 y/o in boys. Most commonly seen in girls, idiopathic. May indicate a lesion in boys.
Isolated precocious puberty: Early onset of sexual development without any other signs e.g. early thelearche.
Delayed puberty: Late onset of puberty. No onset at 14 y/o in girls and 15 y/o in boys. Most common in boys.
Precocious puberty: Outline the types of precocious puberty, possibly causes and treatment
Gonadotropin-dependent precocious puberty
Premature activation of the HPG axis
Causes: Idiopathic; CNS infection; hypothalamic hamartoma
Treatment: GnRH agonist may be used
Gonadotropin-independent precocious puberty
Presence of sex steroids independent of adrenal gonadotropins
Causes: Adrenal hyperplasia; HCG secreting tumour; Leydig/ovarian tumour
Treatment: Surgery, radio/chemo-therapy
Delayed puberty: Outline the types of delayed puberty and causes
1. Hypogonadotropic hypogonadism: Low FSH, LH and oestrogen/testosterone
2. Hypergonadotropic hypogonadism: High FSH and LH. Low oestrogen/testosterone.
Causes: Turner’s syndrome; cryptorchidism; testicular torsion; autoimmune
3. Normogonadotropic normogonadism: Normal hormone levels
Causes: Imperforate hymen; vaginal aplasia; PCOS; hypothyroidism; hyperprolactinemia


