Sarcoidosis
- CXR
- Bloodwork
- Liver biopsy
- Sequelae
chest xray: enlarged hilar lymph nodes
bloodwork: elevated serum ACE level
liver biopsy: scattered granulomas which affect the portal triads to a greater degree than the lobular parenchyma
can cause: arthralgias and skin changes
can also cause skin lesions:
subcutaneous nodules (erythema nodosum), erythematous plaques, or macules that are slightly rddened and scaling
What is fat embolism syndrome?
>>pulm insufficiency, diffuse neuro impairement, thrombocytopenia, and anemia
>>fat globules dislodge from BM enter the marrow vascular sinusoids and occlue pulm nicrovessels imparing gas exchange
>>microvascular occlusion in the cerebral white matter, brain stem, and SC causes the neuro manifestation
CF
- CP
- Cause/Genetics
- Sequelae
>>CP: recurrent sinopulmonary infections pancreatic insufficiency, and GI malabsorption
>>cause: mutation affecting CFTR (cystic fibrosis transmembrane conductance regulator), a chloride channel that is activated by cAMP-mediated phosphorylation and subsequently gated by ATP
>>most common CFTR gene mut: found in approx 70% of cases, is a 3-bp deletion that removes a phenylalanine at AA position 508 (deltaF508).
>>>>this causes impaired post-translational processing (improper folding and glycosylation) of CFTR which is detected by the ER
>>>abnml protein is targeted for proteasomal degradation, preventing it from reaching the cell surface
>>most common cause of meconium ileus (inspissated green mass suggestive of distal ileum obstruction by dehydrated meconium)
deaths: cardiorespiratory complications-pneumonia (persistent, tx-resistant, infectious), bronchiectasis, bronchitic obstructive pulmonary diease, and cor pulmonale
Why do silicosis pts have increased susceptibility to pulmonary TB?
increased susceptibility to pulmonary TB due to disruption of macrophage phagolysosomes by internalized silica particles, macrophage killing of intracellular mycobacteria may be impaired
What is Kartagener syndrome?
>AR. form of primary ciliary dyskinesia, due to mutations that impair the structure or function of cilia, a form of primary ciliary dyskinesia (PCD) due to failure of dynein arms to develop normally
>>triad: situs inversus, chronic sinusitis, bronchiectasis
What are the 4 main clinical manifestations of asbestos exposure?
- pleural plaques-hallmark of asbestos exposure that typically affects the parietal pleura along the lower lungs and diaphragm.
>>plaques are composed of: discrete circumscrbied areas of dense collagen that frequently bacome calcified
>>pleural disease usually develops within 15yrs following intial exposure and is asymptomatic unless there is a significant colapse of adjacent lung parenchyma
- Asbestosis-characterized by progressive, diffuse PULMONARY FIBROSIS and the presence of asbestos bodies
>>clinical manifestation: 15-20yrs after intial exposure; get dyspnea, and reduced lung volumes (restrictive lung disease)
- bronchiogenic carcinoma-most common malignancy associated with asbestos exposre.
>>smoking and asbestos exposure have a synergistic effect on the development of lung carcinoma. a. in NONsmoking pts, increase risk by 6x
b. in smoking pts, 60x
4. malignant mesothelioma-rare malignancy of the pleura, asbestos=only known environmental RF.
>>less common than bronchogenic carcinoma in asbestos-exposed patients, but mesothelioma is more specific for heavy asbestos exposure
A. What is the function of the medullary respiratory center?
B. What are the three types of chemoreceptors?
MRC: controls the depth and rate of respiration based on input from central and peripheral chemoreceptors and airway mechanocreceptors
- Central chemoreceptors: located in medula, stimulated by decreases in pH of surrounding CSF. BBB is impermeable to H+, so blood pH has little effect on them. On the other hand, CO2 readily diffuses through the BBB and forms H+ in the CSF. Therefore, increased PaCO2 is the major stimulator of ctl chemoreceptors, leading to an increase in respiration.
In pts with COPD, response to PaCO2 is blunted and hypoxmia becomes important contributor to respiratory drive.
- peripheral chemoreceptors found in the carotid and aortic bodies are the primary sites for sensing arterial PaO2 and are stimulated by hypoxemia; can be suppressed with oxygen administration
- Pulmonary stretch receptors include myelinated and UNmyelinated C fibers in the lung and airways. these receptors regulate the duration of inspiration depending on the degree of lung distension (Hering-Breuer reflex) and act predominantly to protect the lung from hyperinflation.
ARDS
- major RF: acute necrotizing pancreatitis
- path: diffuse injury to alveolocapillary membranes results in interstitial and intraalveolar edema, acute inflamm, and alveolar hylaine membranes
- hyaline membranes: from alveolocapillary membrane leakage, consists of fibrin exudate and plasma protein rich edema fluid mixe with cytoplasmic and lipid remnants of necrotic epithelial cells
- acute stage: lungs are heavy, red, boggy
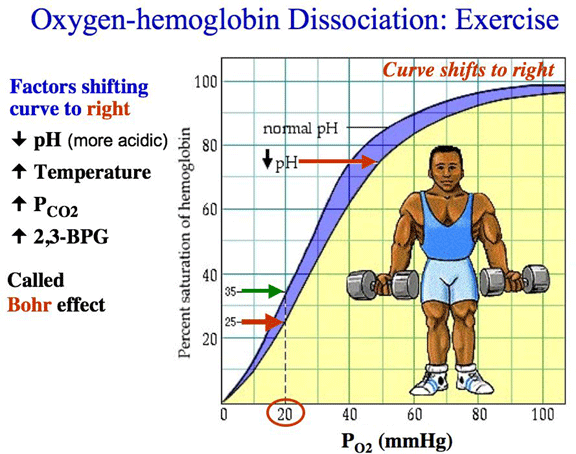
What is the Bohr effect?
Shifting to the right of the oxyhemoglobin curve (INCREASED: H+, 2,3DPG, and temperature)
What happends to HbS aggregates in the deoxy state?
- polymers form fibrous strands that decrease RBC membrane flexibility and promote sickling
- sickling at low pH, high 2,3-BPG
- inflexible erythrocytes lead to microvascular occlusion and microinfarcts
Pulmonary embolism
- risk groups: hospitalized and post-op patients
- CP: tachypnea, tachycardia, cough, pleuritic CP
- pt develops hypoxemia because of V/Q mismatch
Cyanide poisoning
- CP: rapidly developping cutaneous flushing, tachypnea, HA, tachycardia, N/V, confusion, weakness, respiratory distress, cardiac dysfunction
- Lab: severe lactic acidosis and lessened differece between arterial and venous O2
- tx: NITRITES**(oxidizing agent, causes methemoglobinemia), sodium thiosulfate
ALL; T-cell
- CP:
- mediastinal mass that can compress great vessels=SVC syndrome
- can compress esophagus=dysphagia
- can compress trachea=dyspnea and stridor
*
What is true of the pulmonary system at all times?
rate of blood flow through the pulmonary circulation must equal the rate of blood flow through the systemic circulation (at ALL times)
-arterial pressures and oxygen contents will be different
Equilibrium of O2 in a nml indiv at rest is…
- perfusion-limited!
- DIFFUSION limited in disease states:
- emphysema
- pulmonary fibrosis
- and in states of very high pulmonary blood flow (exercise)
What are som RF for ARDS?
What is the process?
- some RF: pulm infection and sepsis
- cytokines stim pulm epithelium
- inflamm response mediated by neutrophils
- capillary damage
- leakage of protein and fluid into the alveolar space
Pleura
- visceral pleura: covers all lung surfaces and does NOT carry pain fibers
- parietal pleura: outer boundary of pleural space
- costal pleura
- pleura innervated by phrenic nerve (C3-C5) at base of neck and over the shoulder:
- mediastinal pleura
- diaphragmatic pleura
- cervical pleura
Steroids for asthma tx
- inhaled for chronic asthma
- systemic for acute exacerbations
- inhibits inflamm mediator formation
- decreases leukocyte extravasation
- stimulates apoptosis of inflamm cells
- decrease mucus production by goblet cells
brachiocephalic vein obstruction
- s/s similar to SVC syndrome BUT on one side of thebody
- BCV drains ipsilateral jugular and subclavian veins
- bilat form SVC
- CP: face and arm swelling and engorgement of subq vein on ipsi neck
persistent bronchial asthma
- chronic AW inflamm and edema leads to bronchial wall thickening and remodeling
- AW HYPERresponsiveness and increased bronchoconstriction
Pulmonary HTN
- specific morphologic findings in branches of the puolmonary artery:
- increased arteriolar smooth muscle thickness (medial hypertrophy)
- intimal fibrosis
- significant luminal narrowing
- in severe HTN, lesions can progress to form interlacing tufts of small vascular chanels=plexiform lesions
- can occur in pulm HTN due to underlying lung, vascular, or cardiac dz and in idiopathic or familial pulm arterial HTN (PAH)
- PAH CP: dyspnea and exercise intolerance in women, 20-40yo
- familal form: inactivating mutations involving the pro-apoptotic BMPR2 gene
- resulting increas in endothelial and smooth mu cell proliferation leads to vascular remodeling, elevated pulm vascular resistance, and progressive pulm HTN
- can occur in pulm HTN due to underlying lung, vascular, or cardiac dz and in idiopathic or familial pulm arterial HTN (PAH)
Where do you place a chest tube for drainage of pleural effusion?
- through the skin and subcutaneous fat into the 4th or 5th intercostal space in the anterior axillary or midaxillary line
- tube traverses through the serratus anterior muscle, intercostal muscles, and parietal pleura
Cystic Fibrosis
- CP: white child with recent pulm infections and malabsorption
- AR D/O of exocrine secretion
- non-functional CFTR (CF transmembrane conductance regulator)
- responsible for transporting chloride ions across mucosal epithelial cell membranes
- with mut, transport of chloride and water from the cells is suppressed=secretion of viscous mucus
- stasis and accumulation of these viscous secretions in tissues
- Clinical findings:
- increased viscosity of bronchial secretions=impaired mucociliary clearance of bacteria
- repeated pulm infecions, **Pseudomonas aeruginosa
- mucus plugging of bronchi causes dilatation and bronchiectasis
- viscous pancreatic secretions are not transported to intestinal lumen, accumulate in pancreatic ducts
- pancreatic insufficiency causes s/s of malabsorption (steatorrhea and poor weight gain)
- fibrosis of pancreatic tissue
- decreased secretion of water by the intestinal epithelium may cause intestinal obstruction
- neonates with CF may develop meconium ileus
- increased viscosity of bronchial secretions=impaired mucociliary clearance of bacteria


