layers of heart
pericardium
epicardium
myocardium
endocardium
pericardium
made of fibrous and serous pericardium (which in turn has a visceral (inner) and parietal (outer) component)
at inferior edge of pericardium is teh pericardial space which is filled with fluid to allow movement between pericardium and epicardium
epicardium
with coronary blood vessels
slippery tissue which has the vessels that supply the heart contained within
myocardium
with trabeculae carnae
cardiac muscle responsible for hearts pumping action
endocardium
endothelial lining of the chambers of the heart which is continuous with the vessels supplying the heart
right artrium
receives deoxygenated blood from SVC and IVC
blood then passes though tricuspid valve
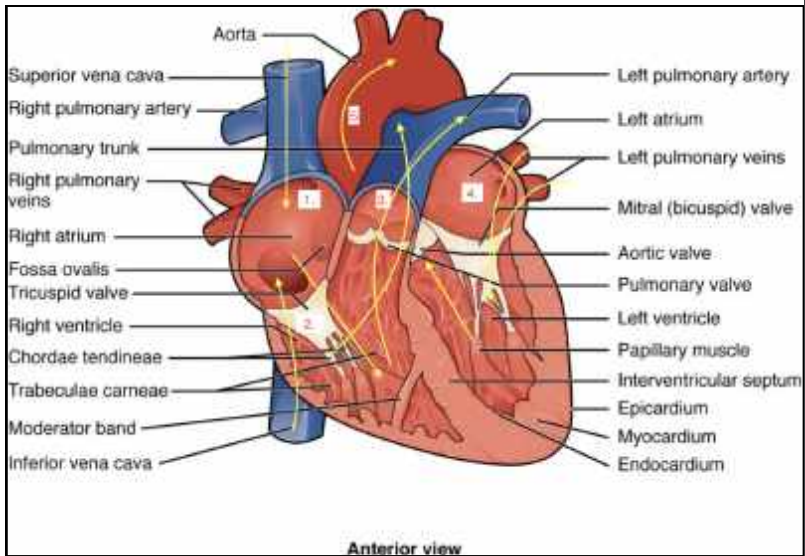
right ventricle
series of ridges known as trabeculae carnae made of myocardium projections
some of these trabeculae from papillary mauscles which connect to the tricuspid valve via chordae tendineae
deoxygenated blood then passes from RV to the L and R Pulmonary arteries through the pulmonary valve to the lungs
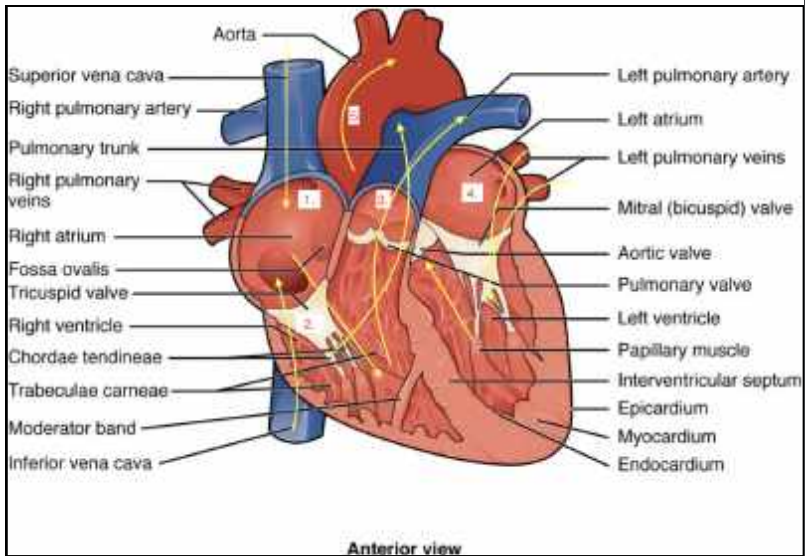
left atrium
receives oxygenated blood from the 4 pulmonary veins
blood passes through the LA to the LV via the bicuspid (mitral valve)
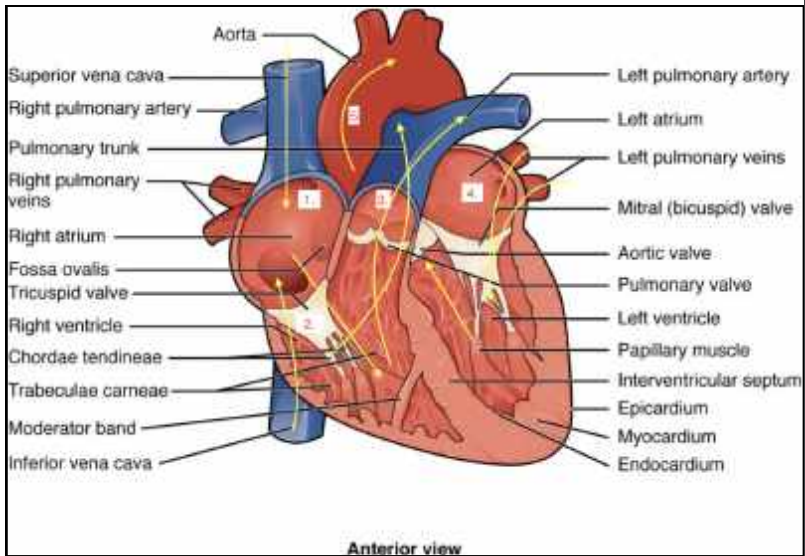
left ventricle
blood passess from LA to LV and is then ejected via the aortic (semilunar) valve
the blood passes into the ascending aorta and out to the body
some blood also goes to the coronary vessels
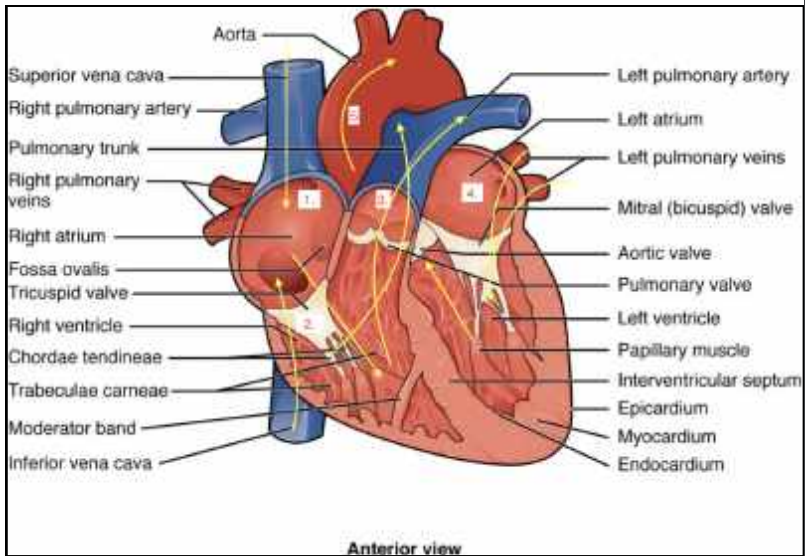
conduction of heart carried out by
Autorhythmic fibres
these fibres set the rhythm of the heart but also the path in which the rhythm is conducted
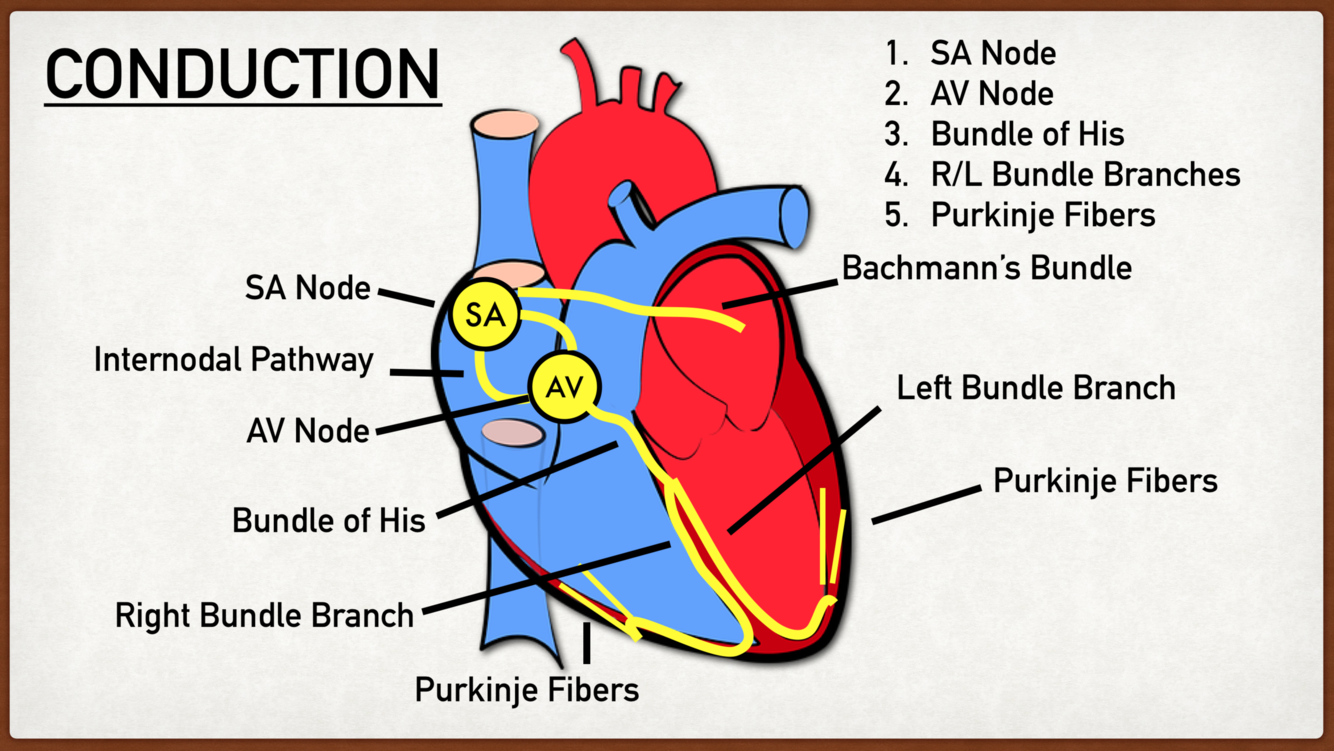
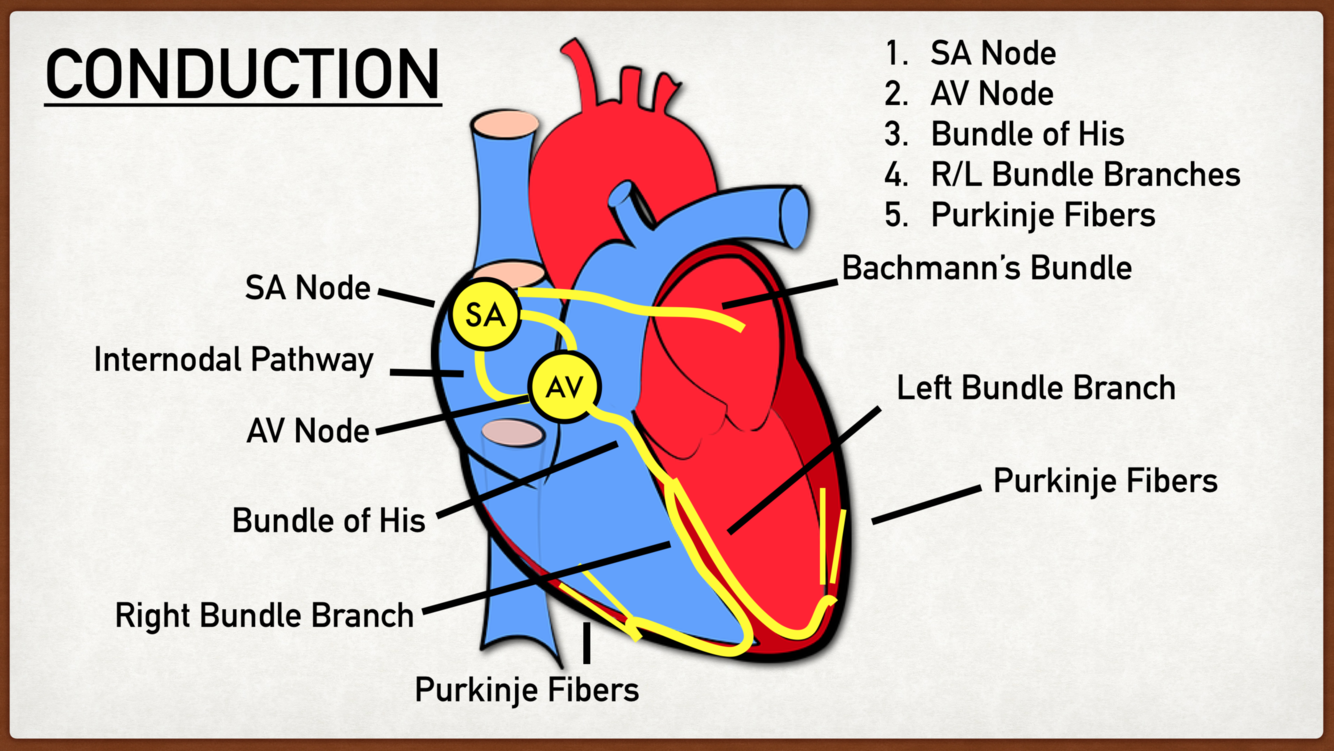
sequence of heart conduction
- Starts at Sino Atrial Node in the RA with spontaneous depolarisation
- Reaches the Atrioventricular Node which is the junction between RA and RV
- The conduction then reaches the Bundle of His which is the only site where Atrio-Ventricular conduction can occur as the fibrous skeleton of the heart usually separates A from V
- The fibres then branch left and right into the bundle branches through the interventricular septum
- Finally large diameter purkinje fibres conduct the action potentials into the trabeculae carnae of the myocardium to aid with ventricular contraction
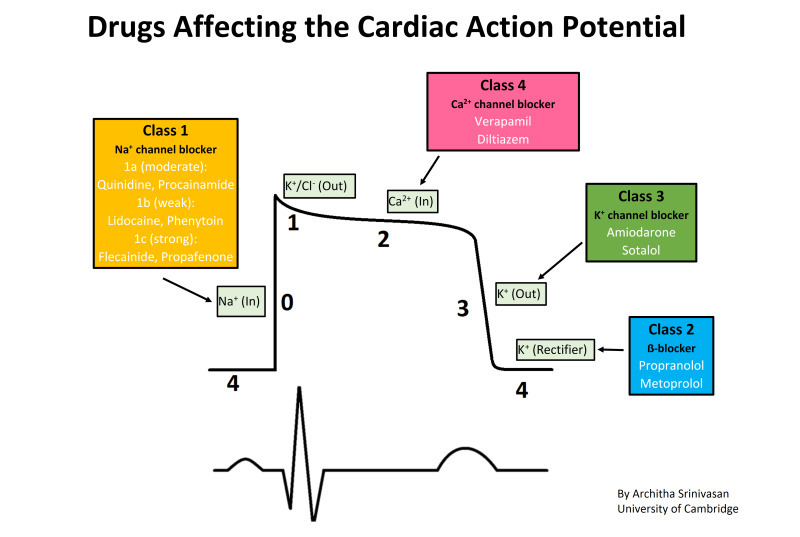
cardiac action potention
contractile working fibres after SA node
depolariation
plateau
repolarisation
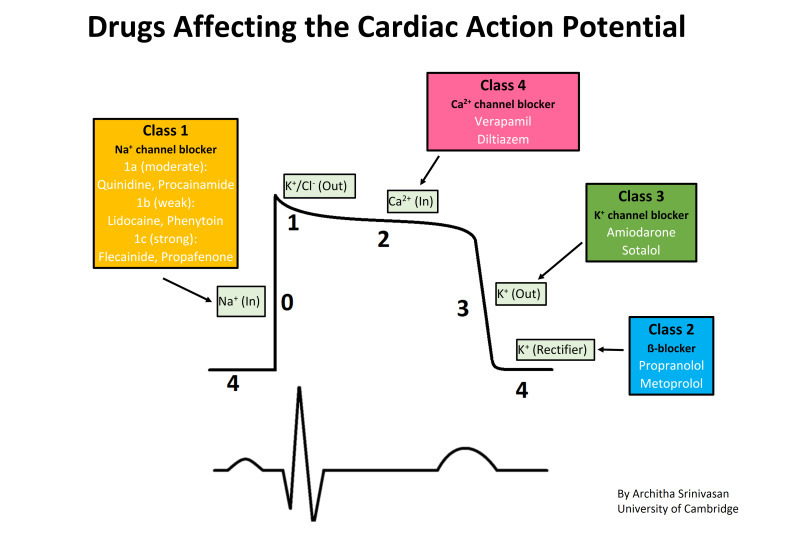
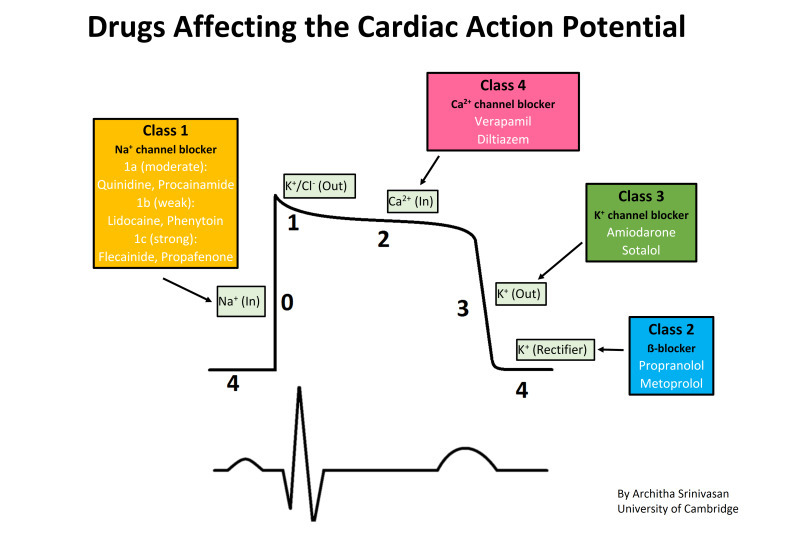
depolarisation stage in cardiac action potential
stage 0
rapid depolarisation by Na+ ions efflux
channels close soon after
plateau stage in cardiac action potentials
stages 1 and 2
Ca2+ ions maintain the depolaristion level by equalising the K+ outflow
increased calcium ion concentration ultimately triggers heart muscle contraction
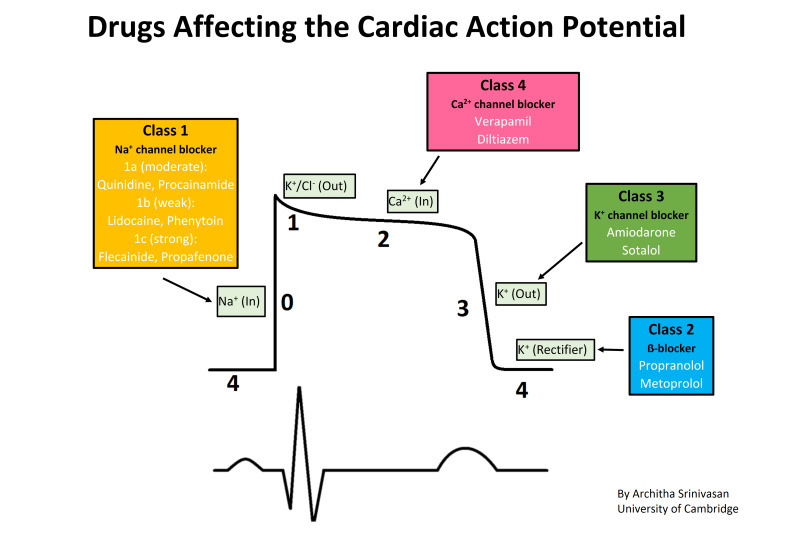
repolarisation stage in caridac action potential
stage 3
Ca2+ begin to close
K+ channels begin to open
production of ATP in the heart
mostly comes from oxidation of glucose and fatty acids
- smaller contributions from Lactic Acid, amino acids and ketone bodies
- some also produced by creatinine phosphate
dying/injured cells release creatinine into the blood - diagnostic sign
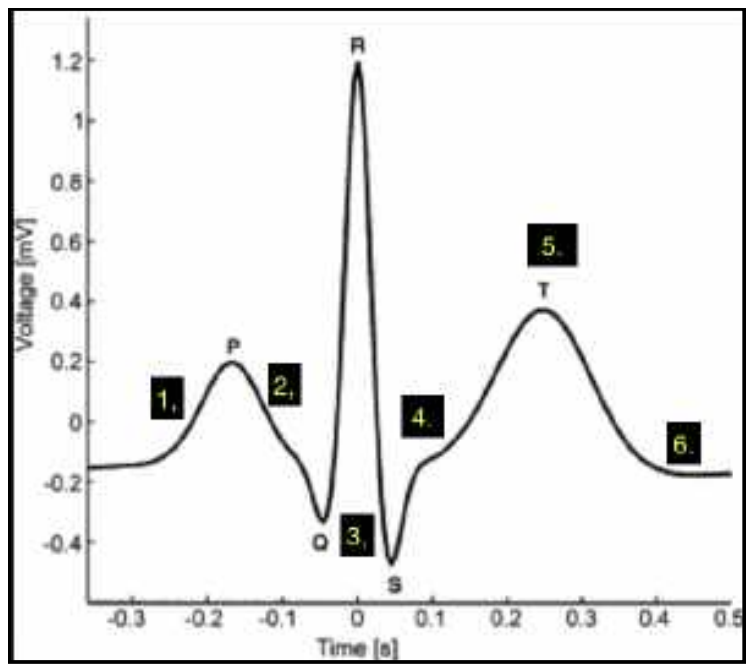
electrocardiogram ECG
- Raising part of P-Wave = Depolarisation of Atrial contractile fibres
- Descending part of P- Wave = Atrial Systole
- QRS complex = Depolarisation of Ventricular contractile fibres
- Flat portion following QRS = Ventricular Systole
- Repolarisation of Ventricular contracile fibres = T-wave
- Ventricular diastole (relaxation) = flat end point/beginning next cycle
caridac output
volume of blood ejected from either
- LV -> Aorta
- RV -> Pulmonary trunk
per min
stroke volume =
volume of blood ejected in a contraction
heart rate =
bpm
CO=
(cardiac output)
SV (ml/beat) x HR (bpm)
stroke volume x heart rate
typical adult male CO =
SV x HR
70 x 75
= 5250ml/min
5.25L/min
preload
degree of stretch of the heart before it contracts
(how much space can it make)
contractility
force of contraction














