which channels let water through membranes?
aquaporins
what are similar or differences between them?
difference between ECF and ICF?
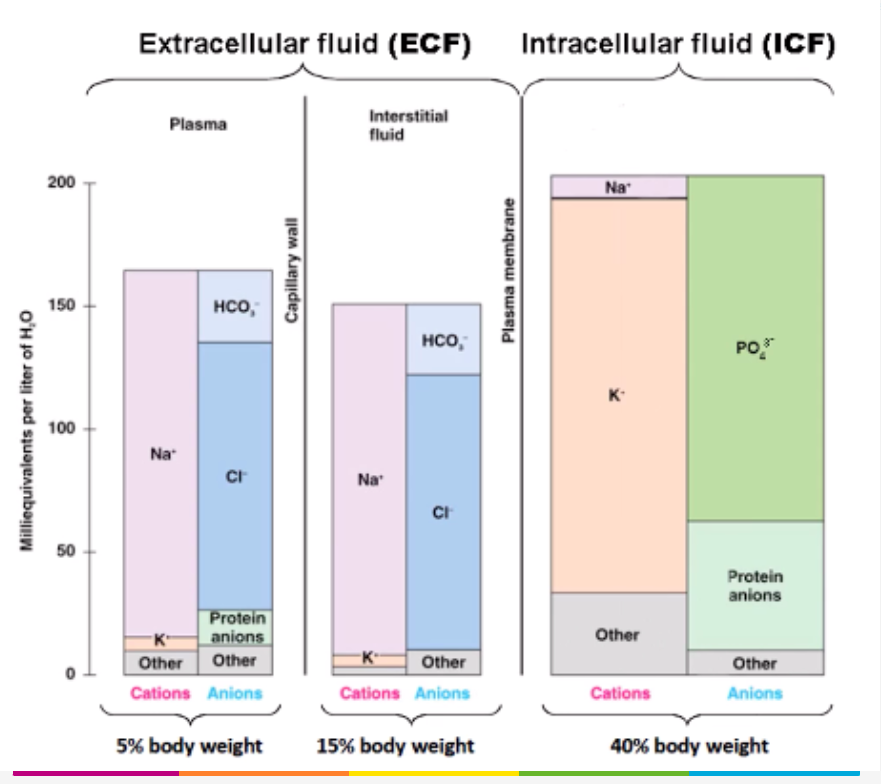
-Plasma and interstitial fluid: same electrolyte components BUT plasma has proteins - e.g. albumin and anions c.f. interstitial fluid
Intracellular fluid c.f. extracellular fluid: ICF has very little Na+. Lots of K+ and PO43- - (buffers acid / base situation), protein anions (think - sea with Na+ is ECF, banana tree: ICF). ECF has high Na+ and Cl-
what characteristics do osmoreceptors have?
(in the Subfornical organ: in the hypothalumus. (Organum Vasculosum of the lamina terminalis (OVLT) - dont need to know)
- characterised by: a) extensive vasculature b) lack of normal blood brain barrier
- where are the osmoreceptors found in brain?
- what is another stimuli that triggers sensation to drink?
- osmoreceptors: in hypothalamus
- baroreceptors: detect when there is decreased blood volume (in great veins, right atrium of heart -> relied to vasomoto center) -> relayed to hypothalamus
Q
what is the main stimulus for the thirst sensation?
increase in plasma osmolality
describe mechanism of aldosterone working
(where made? released from? what does it cause to do? result?)
aldosterone:
released from: adrenal cortex
released when: reduced Na+ or increased K+
function: increases reabsorbtion of Na or increased K secretion
result: homeostatic plasma levels of Na+ and K+.
aldosterone binds to kidney cells:
a) ENAC (Na channel) - can reabsorb more Na
b) Na/K pump ( pumps Na in / K out)
how does atrial natruiretic peptide work? released from? releaed when?
Atrial natriuretic peptide (ANP)
released from: cardiac Atria
released when: increased blood volume (stretches atria)
function: promotes excretion of Na+ and Cl-, in turn decreases water reabsorbtion (brings blood volume back towards normal)(acts on hypothalamus and adrenal cortex up the mechanism.)
what horomone does same role as aldoesterone (i think)
angiotension II
which channels in the kindey, controlled by ADH and aldosterone, controls the variable reabsorbtion of water?
- *-aquaporins
- ENAC
- Na/K pumps**
what are ways you can test blood glucose? (3)
fasting glucose test - (not eating / drinking anything other than water for 8hrs)
glucose tolerance test - after fasting and again after 2 hours after being given a glucose drink
glycated haemoglobin test (HbA1C) - measure of average blood sugar level over past 3 months.
state and say use of each type of blood test pls
- complete blood count:
- arterial blood gas: CO2 and O2 levels
- blood smear: represents a snapshot of cells in blood at the time. size, shape and colour of RBC and WBC can be measured - can determine diagnosis
- blood cultures: suspect a pathogen
what is hematocrit a measure of ?
Hematocrit, the proportion of red blood cells to the fluid component, or plasma, in your blood
the concentation of hydrogen ions is regualted by which systems?
how long does it take for each system to regulate?
1. chemical buffer system in blood and ICF: immediate action
2. Respiratory centre in brain stem:acts within 1-3 minutes
3. kidneys : hours to days
what are the three major chemical buffer systems in the body?
Bicarbonate (HCO3-) buffer system: H20 + CO2 ⇌ H2CO3 + HCO3- + H+
Proteins (Hb and albumin) buffer system
Phosphate buffer system
what is anion gap?
what happens if have high anion gap?
- measure the conc of Na, Cl and HCO3- in blood. - cations should be greater by anions by 8 to 12 mEq/L.
[Na+] - ([Cl-] + [HCO3-]) = 8 to 12 mEq/L
If your results show a high anion gap, you may have acidosis, which means higher than normal levels of acid in the blood
which part of brain controls for difference in breathing rate due to acid / alkaline blood lvels?
- change incurred by Pons and medulla
- expelling more co2 lowers the acid levels
how does the kidney produce bicarbonate?
- Glutamine -> glucose, HCO3-, NH4+ (excreted out and used to combine with H+ ions to make sure excreted into urine)
when the body is in acidosis, how do we ensure H+ stay out of renal tubule cells?
when the body is acidosis:
@ distal proximal tubule:
H+ get secreted out of renal tubule cell into lumen. BUT want to stay here. SO, use NH4+ and H2PO4 buffes to keep the H+ in the filtrate
what do you look for when get results from arterial blood gas? what does each one mean
- pH low (acidosis) or high (alkalosis)?
- what is PaCO2 value? (resp. indicator)
- what is HCO3- value? (metabolic indicator)
what test do you if have a metabolic acidosis?
check anion gap
Therefore, values greater than 12 define an anion gap metabolic acidosis.
describe briefly synthesis of phosphocreatine
what is it used for?
location?
phosphocreatine synthesis:
- transfer of phosphate group from ATP
- enzyme used: creatine kinase
- anaerobic conditions
function: ATP buffer (can restore ATP when needed)
Location: in tissues that have high, fluctuating energy demands - muscle and brain
-
explain proton motive force
- making a gradient to keep out of equilibrium.
- get an electrochemical gradient (gradient of BOTH electrical potential and chemical concentration across a membrane)
- transfer of H+ via proton pumps across membrane creates a source of energy (PMF): get a proton electrochemical gradient of proteins: proton motive force
can use thise electrochemical conc. gradient of protons across a membrane to power the synthase of ATP
which are the energy conversion pathways that occur in cellular resp?
- glycolysis
- krebs cycle
- electron transport chain
why / how is cyanide a poison?
- binds to cyctochrome c oxidase (4th complex in ECT)
- cyanide attaches to iorn within protein complex and inhibits activity of the complex system
- ECT can’t pump H+ into intermembrane space = pH of intermembrane space increases -> pH gradient decreases.
- ATP synthesis stops



