1. The net filtration pressure (NFP) represents the interaction of the hydrostatic and osmotic pressures and its value changes at different points along the capillary bed. Calculate NFP close to the arterial end of the capillary using the values below. (2 marks)
Hydrostatic pressure in capillary (HPc) arterial end = 36 mmHg
Capillary colloid osmotic pressure (Opc) = 26 mmHg
interstitial fluid colloid osmotic (OPif) = Approximately 1 mmHg
*Assume that the hydrostatic pressure of interstitial fluid (Hpif ) is 0 mmHg
- NFP = (HPc – HPif) – (OPc – OPif) – 1 mark for correct formula.
- NFP = (36 – 0) – (26 – 1)
- NFP = 36 – 25
- NFP = 11 mmHg – ½ mark for correct value and ½ for correct units
2. What features of albumin normally prevent it passing into the urine? (1 mark)
Large size (1/2 mark) and negative charge (1/2 mark)
3. Describe briefly the three main structures that make up the glomerular filtration barrier (3 marks)
(i) Fenestrated capillary endothelium (1 mark),
(ii) the glomerular basement membrane (1 mark)
(iii) glomerular epithelium, or podocytes (which have cellular extensions called foot processes that envelop the capillaries) (1 mark).
4. In Mina’s case, what does the low serum albumin indicate? (1 mark)
Ineffective glomerular filtration/damage has caused enough albumin to be lost in the urine to cause the levels in the blood to drop. (1 mark)
5. Failure of which side of the heart typically causes pleural effusions? (1 mark)
Left (1 mark)
6. Explain the difference between pleural effusions and pulmonary oedema (2 marks)
Pleural effusions are accumulation of fluid within the pleural space (1 mark), whereas pulmonary oedema is accumulation of fluid in the alveoli and alveolar interstitium (1 mark)
define nephrotic syndrome [3]
Nephrotic syndrome is broadly defined as a triad of heavy proteinuria > 3.5 g/day, hypoalbuminaemia, and oedema.
explain the effect of low serum albumin on NFP?
- Low serum albumin = low oncotic pressure (OPc)
- Less ‘force’ pulling water in
- NFP increases
- More fluid forced out in arterial end and less fluid absorbed in venous end
•Fluid accumulates in interstitium
what is heart failure? and what can cause it? [4]
- Heart fails to pump blood
- Causes: coronary artery diseases, hypertension, cardiomyopathy, valvular heart diseases [4]
explain the effect of heart failure on NFP and what is results in :)
- Heart fails to pump
- Blood accumulates in ventricle
- Congestion
•HPc increases in venous end
•NFP increases
•Less absorption in venous end
•oedema
explain the effect of increased capillary perm on NFP
- Vascular damage due to trauma, burn, inflammation
- Protein leaks into interstitium
- OPc decreases while OPif increases
- Less oncotic pressure drawing fluid in
- Fluid accumulates in interstitium
what is starling hypothesis?
- Fluid movement across capillaries is a balance between hydrostatic pressure and oncotic pressure.
explain are the pimary causes of nephrotic syndrome? [3]
- Minimal change disease:
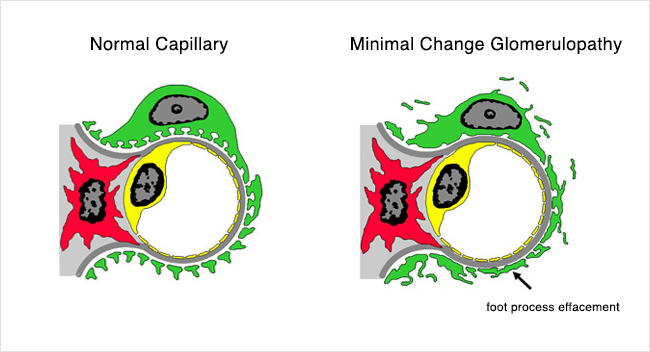
- Glomeruli appear normal on light microscopy, but on electron microscopy, FUSION of the FOOT PROCESSES of the PODOCYTES is seen, consistent with a disrupted podocyte actin cytoskeleton
- Immature differentiating CD35 stem cells appear to be responsible for the pathogenesi
- Membranous neuropathy – adults
- Caused by: an antibody to a protein on the podocyte called the phospholipase A2 receptor (PLA2R). In most people with MN, the body’s immune (defense) system makes an antibody (a protein that normally helps fight infections). Instead of targeting an infection, these antibodies attack the podocytes
- Autoimmune reaction against important antigens in the filtration barrier. This leads to the development of autoantibodies, formation of immune deposits and subsequent thickening of the glomerular basement membrane.
- This leads to the development of autoantibodies, formation of immune deposits and subsequent thickening of the glomerular basement membrane.
- Focal segmental glomerulosclerosis
- Scarring on glomerulus that is focal and only some glomeruli involved and segmental (only part of glomerulus affected). Scars the filter CD80 in podocytes resulting in increased permeability in glomeruli and thus proteinuria and haematuria
- This refers to a loss of podocyte foot process structure, causing them to spread out and this reduces the effectiveness of the filtration barrier.
what is nephrotic syndrome characterised by? [4]
- Nephrotic syndrome is a group of symptoms that indicate your kidneys are not working properly. Due to:
- Proteinuria > 3.5g/24 hours
- Hypoalbuniaemia (low blood albumin) – most lost because:
- Small protein
- Has negative charge, makes it more pushed out
- Normal % of albumin is 50% of blood proteins
- Causes symptoms because it effects the oncotic pressure in the capillary, so water isn’t pushed back in
- Oedema
- Severe hyperlipidaemia is often present:
- Liver goes into overdrive due to albumin loss and other protein loss which increases risk of blood clots and produces raised cholesterol
- Don’t develop kidney failure but are leaking HUGE amounts of protein but kidney function remains the same
what is a disease that increases liklihood of nephrotic syndrome?
- Diabetes mellitus
how can you treat nephrotic syndrome?
- -Reduce oedema:
- Loop diuretics e.g. IV FUROSEMIDE - IV since gut oedema may prevent oral absorption
- Thiazide diuretics e.g. IV BENDROFLUMETHIAZIDE Fluid and salt restriction while giving diuretics
- - Reduce proteinuria:
- ACE inhibitor e.g. RAMIPRIL
- Angiotensin receptor blocker e.g. CANDESARTAN o Eat normal rather than high protein diet
explain the different types of heart failure:
- Right sided heart failure
- Right-sided or right ventricular (RV) heart failure usually occurs as a result of left-sided failure.
- Left sided heart failure
- Systolic failure: The left ventricle loses its ability to contract normally.
- Diastoilic failure: The left ventricle loses its ability to relax normally (because the muscle has become stiff).
name 3 typical features of someone suffering from nephrotic syndrome [3]
explain why [1]
hyperlipidaemia
increased risk of venous/arterial thrombosis
higher risk of infection
This is because of loss of important proteins (e.g. immunoglobulins, albumin) through the glomeruli.
which cause of nephrotic syndrome occurs in children 90% of time?
minimal change disease
explain how left sided heart failure causes right sided heart failure [2]
Advanced left-sided heart failure commonly causes right-sided failure due to increased intrathoracic pressure and pulmonary hypertension.
what is combination of left and right failure is known as? [1]
The combination of left and right failure is known as congestive cardiac failure.
what are 3 primary determinants of stroke volume? [3]
Preload
Myocardial contractility
Afterload
define preload and afterload
Preload: stretching of cardiomyocytes at the end of diastole.
Afterload: pressure or load against which the ventricles must contract.


