Question
A 45-year-old patient requires a 14 cm segmental reconstruction of the left hemimandible following resection of an ameloblastoma. The surgical plan includes future placement of osseointegrated dental implants. The patient has a body mass index of 22 and normal peripheral vascular status. Which of the following free flaps provides the most suitable bone stock for this reconstructive goal?
a) Medial femoral condyle osteocutaneous flap
b) Radial forearm osteocutaneous flap
c) Serratus anterior with rib composite flap
d) Deep circumflex iliac artery (DCIA) flap
e) Anterolateral thigh fasciocutaneous flap
The correct answer is option D.
Rationale
The deep circumflex iliac artery (DCIA) flap is ideally suited for this reconstruction because it provides a long segment (up to 16 cm) of corticocancellous bone with excellent height and thickness, creating a foundation that closely mimics the native hemimandible. Its natural curvature matches the mandibular contour, and its robust bone stock offers superior support for osseointegrated dental implants, a key requirement in this case.
The other options are incorrect:
* a) Medial femoral condyle osteocutaneous flap: This flap provides only a small volume of bone (typically <7 cm), which is insufficient for a 14 cm hemimandibular defect.
* b) Radial forearm osteocutaneous flap: The radial bone is thin and primarily cortical, providing inadequate height and volume for both mandibular reconstruction and reliable dental implant placement.
* c) Serratus anterior with rib composite flap: Rib bone is thin, curved, and lacks sufficient width and cortical thickness for stable long-term dental implant retention.
* e) Anterolateral thigh fasciocutaneous flap: This is a soft-tissue-only flap that contains no bone, making it unsuitable for mandibular bony reconstruction.
References
1. Piotrowska-Seweryn A, Szymczyk C, Walczak DA, et al. Fibular free flap and iliac crest free flap in mandibular reconstruction in patients with mandibular ameloblastomas. J Craniofac Surg. 2022;33(7):1962-1970.
2. Iorio ML, Masden DL, Higgins JP. Cutaneous angiosome territory of the medial femoral condyle osteocutaneous flap. J Hand Surg Am. 2012;37(5):1033-1041.
3. Matsumoto H, Shinaoka A, Ohtsuka A, Kimata Y. Detailed vascular anatomy and flap harvest technique of the serratus anterior/rib composite flap. Plast Reconstr Surg. 2019;143(1):115-124.
Question
A 56-year-old man undergoes subtotal lower lip resection for squamous cell carcinoma, followed by immediate reconstruction with a free anterolateral thigh (ALT) flap. The lateral femoral cutaneous nerve was harvested as part of the ALT flap to provide sensory innervation to the reconstructed lip. To which of the following nerves should it be anastomosed to best restore sensation to the lower lip?
a) Ipsilateral mental nerve
b) Contralateral buccal branch of the facial nerve
c) Ipsilateral hypoglossal nerve
d) Contralateral great auricular nerve
e) Ipsilateral lingual nerve
The correct answer is option A.
Rationale
The goal of sensate lip reconstruction is to re-establish neural continuity between the flap and the native sensory pathway of the lip. The mental nerve is the terminal branch of the inferior alveolar nerve (V3) and provides sensory innervation to the lower lip and chin. Performing a neurotrophy between the lateral femoral cutaneous nerve (the sensory nerve of the ALT flap) and the ipsilateral mental nerve directly connects the reconstructed tissue to the original trigeminal nerve sensory map, offering the best potential for restored protective and fine sensation. This approach is described in the provided case, where the lateral femoral cutaneous nerve was sutured to the mental nerve.
The other options are incorrect:
* b) Contralateral buccal branch of the facial nerve: The buccal branch of the facial nerve (CN VII) is a motor nerve that innervates muscles of the midface and upper lip. Anastomosing a sensory nerve to a motor nerve would not restore sensation.
* c) Ipsilateral hypoglossal nerve: The hypoglossal nerve (CN XII) is a motor nerve to the tongue. An anastomosis here would not provide lip sensation and would potentially compromise tongue function.
* d) Contralateral great auricular nerve: This is a sensory nerve from the cervical plexus that supplies the skin over the parotid gland and earlobe. It is not involved in the natural sensory innervation of the lip and is more commonly used as a donor nerve for grafting, not as a recipient for lip reconstruction.
* e) Ipsilateral lingual nerve: The lingual nerve provides general sensation and taste to the anterior two-thirds of the tongue, not the lower lip.
References
1. Tsuge I, Yamanaka H, Katsube M, Sowa Y, Sakamoto M, Morimoto N. Lower lip reconstruction using a sensory anterolateral thigh flap as the first choice. Plast Reconstr Surg Glob Open. 2023;11(5):e5003.
2. Hanasono MM, Skoracki RJ, Yu P. A prospective study of donor-site morbidity after anterolateral thigh fasciocutaneous and myocutaneous free flap harvest in 220 patients. Plast Reconstr Surg. 2010;125(1):209-214.

Question: A 22-year-old man presents 18 months after developing a severe Volkmann ischemic contracture of his dominant right forearm following a crush injury. He has undergone previous nerve decompressions and therapy but has no active finger flexion and minimal wrist motion. Physical examination reveals a pronated forearm, flexed wrist, and clawed fingers with dense fibrosis of the volar forearm. Which of the following is the most appropriate surgical management to restore functional grip?
A) Carpal tunnel release
B) Flexor origin slide (Max Page procedure)
C) Free functional gracilis muscle transfer
D) Intensive hand therapy
E) Revision amputation above the elbow
The correct answer is Option C.
Rationale: In a patient with a long-standing, severe Volkmann contracture with no active finger flexion due to muscle fibrosis and no improvement after previous therapy, a free functional gracilis muscle transfer is the most appropriate option to restore grip. This procedure replaces the non-functioning, fibrosed forearm flexors with an innervated muscle (typically the gracilis) whose motor nerve (obturator) is coapted to a proximal donor nerve (median or anterior interosseous). A flexor origin slide (Option B) is only effective in patients who have preserved active finger flexion, which this patient lacks. Carpal tunnel release (Option A) addresses nerve compression but does not restore motor function lost to muscle fibrosis. Additional hand therapy (Option D) is unlikely to provide benefit 18 months after injury with established fibrosis. Amputation (Option E) should be a last resort when reconstruction is not possible.
References:
1. Sabapathy SR, Venkatramani H, Bhardwaj P, et al. Technical considerations and outcome of free functioning gracilis muscle transfer for finger flexion in patients with Volkmann’s ischemic contracture. Injury. 2021;52(12):3640-3645.
2. Stevanovic M, Sharpe F. Functional free muscle transfer for upper extremity reconstruction. Plast Reconstr Surg. 2014;134(2):257e-274e.
3. Ultee J, Hovius SE. Functional results after treatment of Volkmann’s ischemic contracture. Clin Orthop Relat Res. 2005;(431):42-49.
Question: A 45-year-old man presents with a 4 x 6 cm soft tissue defect over the lateral malleolus following a motorcycle accident. The surgical team is planning a local muscle flap for coverage. Which of the following muscles is the most appropriate choice, and what is its dominant vascular pedicle?
A) Abductor hallucis; medial plantar artery
B) Extensor digitorum brevis; lateral tarsal artery
C) Flexor digitorum brevis; lateral plantar artery
D) Peroneus brevis; peroneal artery
E) Soleus; posterior tibial artery
The correct answer is Option B.
Rationale: The extensor digitorum brevis muscle is ideally situated for coverage of lateral ankle and hindfoot defects. Its dominant pedicle, the lateral tarsal artery (a branch of the dorsalis pedis artery), provides reliable perfusion and allows for rotation to cover the lateral malleolar region. As a Mathes and Nahai Type II muscle with an expendable function, it is well-suited for local reconstruction in this area. The abductor hallucis (Option A) and flexor digitorum brevis (Option C) are located on the medial and plantar aspects of the foot, respectively, and are not suitable for lateral malleolar coverage. The peroneus brevis (Option D) is a tendon in the distal leg with minimal muscle bulk, and the soleus (Option E) is too proximal to reach the lateral malleolus without a free tissue transfer.
References:
1. Abdelrahman I, Elmasry M, Steinvall I, et al. Versatility of the extensor digitorum brevis muscle flap in lower limb reconstruction. Plast Reconstr Surg Glob Open. 2018;6(12):e2071.
2. Haq A, Singh V, Sharma S. The reverse flow extensor digitorum brevis flap for dorsal foot defects. J Plast Reconstr Aesthet Surg. 2021;74(11):2957-2964.

The third perforating branch of the profunda femoris artery, which is the blood supply for the lateral thigh flap, originates at a level that is immediately caudad to which of the following muscles?
(A) Adductor brevis
(B) Adductor longus
(C) Adductor magnus
(D) Gracilis
(E) Pectineus
The correct response is Option A.
The third perforating branch of the profunda femoris artery provides the predominant blood supply for the lateral thigh flap. The third perforating branch originates immediately caudad to the adductor brevis muscle, pierces the insertion of the adductor magnus, courses superficially, and then traverses between the biceps femoris and the vastus lateralis. It pierces the deep fascia at this point, and then emerges at the midpoint between the greater trochanter and lateral epicondyle of the femur.
The lateral thigh flap is a versatile flap that has a thin, cutaneous skin paddle and is innervated by the lateral cutaneous nerve of the thigh. As much as 8 * 25 cm can be transferred; however, split-thickness skin grafting is required for closure at the donor site if a flap with a width of greater than 8 cm is harvested. In addition, the lateral aspect of the thigh flap can be hair-bearing, especially in men, while the dermis is characteristically thick and stiff.
The adductor longus muscle originates at the pubic ramus and inserts on the medial epicondyle. The gracilis muscle in the thigh is perfused by the medial circumflex artery, while the pectineus muscle receives its vascularity from the first perforating branch of the profunda femoris.
The direct vascular supply to the arm flap shown is which of the following arteries?
A) Posterior interosseous
B) Posterior radial collateral
C) Profunda brachial
D) Recurrent radial

Correct answer is option B.
Flaps require preservation of the defined arterial and venous supply. Regional flaps can be based distally or proximally. The lateral arm flap was initially described by Song and popularized by Matloub, et al. and Katsaros, et al. This flap has considerable application in reconstruction of the upper extremity. It can be harvested from the same extremity; it has thin, pliable skin; and it can be innervated. The lateral arm flap can also include a segment of vascularized humerus or a segment of vascularized triceps tendon. The flap can also be segmentally contoured for hand defects. The lateral arm free flap is based on the posterior radial collateral artery, which is a branch of the profunda brachial artery. A reversed pedicled lateral arm flap can also be performed. This reverse flap is based on the radial recurrent artery. The superior ulnar collateral artery is the dominant pedicle of the medial arm flap. The medial arm flap is also useful for upper extremity coverage, but there are significant variations in the superior ulnar collateral artery which makes this flap a less-than-optimal choice for microvascular surgical reconstruction. The posterior interosseous artery is the dominant blood supply of the posterior interosseous artery flap. The posterior interosseous artery flap is also used for reconstruction of the hand because it has thin, pliable skin. As a pedicle flap, it can cover the wrist and extend to the first web space. Use of the posterior interosseous flap can compromise motor nerves to the extensor carpi ulnaris or extensor digiti quinti.
A 50-year-old man undergoes a total glossectomy for tongue cancer. A microvascular free flap reconstruction is planned with an anterolateral thigh free flap. After a vertical thigh incision is made, no perforators are found between the rectus femoris and vastus lateralis muscles. Exploration of the medial thigh demonstrates a large perforator between the rectus femoris and vastus medialis muscles. Which of the following is the most likely origin of this perforator?
a. Ascending branch of the lateral circumflex femoral artery
b. Common femoral artery
c. Descending branch of the lateral circumflex femoral artery
d. Medial circumflex femoral artery
e. Profunda femoris artery
The correct response is Option C.
An adequate perforator is not found on dissection of the anterolateral thigh (ALT) free flap in up to 5% of cases. When an ALT flap perforator traveling between the rectus femoris and vastus lateralis or through the vastus lateralis to supply the anterolateral thigh skin is not found, there is a higher chance of finding a perforator that supplies the anteromedial thigh skin. This perforator, present in about 50% of thighs, most commonly arises from the descending branch of the lateral circumflex femoral artery, via a branch that supplies the rectus femoris muscle. This perforator can take a course through the rectus femoris or between the rectus femoris and vastus medialis. Alternately, one or more anteromedial thigh perforators may arise directly from the superficial femoral artery.
When an ALT perforator cannot be located, the surgeon may salvage the situation by changing to an anteromedial thigh (AMT) free flap rather than exploring another donor site. Another alternative is to harvest a tensor fascial lata free flap, based on the ascending branch of the lateral circumflex femoral artery. The medial circumflex femoral artery, common femoral artery, and profunda femoris artery do not give rise to previously described cutaneous perforator flaps.
Reference(s)
- Namgoong S, Yoon YD, Yoo KH, Han SK, Kim WK, Dhong ES. Alternative choices for anterolateral thigh flaps lacking suitable perforators: a systematic review. J Reconstr Microsurg. 2018;34(7):465-471.
- Yu P. Inverse relationship of the anterolateral and anteromedial thigh flap perforator anatomy. J Reconstr Microsurg. 2014;30(7):463-468.
- Yu P, Selber J. Perforator patterns of the anteromedial thigh flap. Plast Reconstr Surg. 2011;128(3):151e-157e.
Which of the following is the most appropriate Mathes and Nahai classification of the rectus abdominis muscle?
A ) Type I
B ) Type II
C ) Type III
D ) Type IV
E ) Type V
The correct response is Option C.
The rectus abdominis muscle is a Mathes and Nahai classification Type III muscle.
The Mathes and Nahai classification of the vascular anatomy of muscles represents an important description in reconstructive surgery. Type I muscles have one vascular pedicle and include the gastrocnemius, rectus femoris, and tensor fascia lata. Type II muscles have a dominant and minor pedicle and include the abductor digiti minimi, abductor hallucis, biceps femoris, flexor digitorum brevis, gracilis, peroneus longus, peroneus brevis, platysma, semitendinosus, soleus, sternocleidomastoid, temporalis, trapezius, and vastus lateralis. Type III muscles have two dominant pedicles and include the gluteus maximus, rectus abdominis, serratus anterior, and semimembranosus. Type IV muscles have multiple segmental pedicles and include the extensor digitorum longus, extensor hallucis longus, flexor digitorum longus, flexor hallucis longus, sartorius, and tibialis anterior. Type V muscles have one dominant and secondary segmental pedicles and include the pectoralis major and latissimus dorsi.
A 54-year-old man is scheduled for correction of a defect on the back 1 week after resection of a 3 × 3-cm recurrent sarcoma. The skin was closed primarily, but necrosis and wound breakdown occurred. History includes radiation therapy to the spine for soft-tissue sarcoma 2 years ago. Physical examination shows a 5 × 5-cm defect in the mid back at T10 with exposed spinous processes. What is the most appropriate method for complete wound closure?
A) Latissimus dorsi flap
B) Rectus abdominis free tissue transfer
C) Split-thickness skin graft
D) Trapezius muscle flap
E) Wide undermining with primary reclosure
The correct response is Option A.
The latissimus dorsi flap provides sufficient skin and muscle to close the defect. It is a Mathes-Nahai Type V flap, primarily supplied by the thoracodorsal artery and vein, with secondary segmental pedicles from posterior intercostal and lumbar perforators. The flap can be mobilized as a turnover flap or advanced on its main blood supply. If necessary, interposition vein grafts can extend the vascular pedicle. This flap has a well-defined anatomy and is straightforward to harvest, commonly used for scalp, lower extremity, breast, and chest wall reconstructions.
A free rectus abdominis flap is less ideal due to limited recipient vessels in this area. Split-thickness skin grafting over irradiated wounds with exposed bone is unlikely to heal. A trapezius muscle flap won’t reach T10. Wide undermining risks further devascularization of irradiated skin, and primary reclosure is likely to cause tension, leading to necrosis and breakdown.
A 68-year-old man who underwent thoracic fusion has exposed spinal hardware at T2. Coverage with a paraspinous muscle flap is planned. What is the Mathes and Nahai classification for this flap?
A) I
B) II
C) III
D) IV
E) V
The correct response is Option D.
Paraspinous muscle flaps are considered the “workhorse” of spinal reconstruction, useful for covering exposed hardware and obliterating dead space. They are classified as Type IV flaps with multiple segmental pedicles, primarily supplied by segmental perforating vessels from the posterior intercostal vessels.
Minor pedicles include lateral row perforators from the posterior intercostal arteries.
A 73-year-old man comes to the office for evaluation of an 8-cm mandibular defect with commensurate skin loss 6 weeks after sustaining a gunshot wound to the face. Reconstruction with a free fibula composite flap with skin paddle is planned. Which of the following arteries is the most common origin for blood supply to the skin paddle?
A) Anterior tibial
B) Peroneal
C) Popliteal
D) Posterior tibial
E) Sural
The correct response is Option B.
The skin paddle of the free fibula flap receives its vascular supply from the peroneal, posterior tibial vessels, or from both. While a majority (95.8%) of the skin paddles receive their blood supply from the peroneal septocutaneous perforators, a few receive vascular contribution from both peroneal and posterior tibial systems, a few from only the posterior tibial system, and finally, a few from the popliteal artery.
The anterior tibial and sural arteries do not typically contribute to the skin paddle of the free fibula graft.
A 65-year-old woman presents with a 4 x 4-cm elliptical defect on the vertex of the scalp after resection of a trichilemmal cyst. Local advancement flaps are planned for closure with wide undermining. Division of which of the following layers is important during scalp flap advancement?
A) Dermis
B) Galeal aponeurosis
C) Innominate fascia
D) Pericranium
E) Subgaleal fascia
The correct response is Option B.
During a scalp advancement flap, release of the galeal aponeurosis is important, as this layer provides the majority of resistance to scalp advancement. Often scoring of the galea is performed in parallel 1-cm intervals to provide adequate release.
The layers of the scalp include: skin, dense connective tissue, galeal/epicranial aponeurosis, loose areolar connective tissue, and pericranium. Release of the other layers listed is not effective, as they do not provide appreciable resistance. The innominate and the subgaleal fascia are the same layer, otherwise known as the subaponeurotic layer or the loose areolar layer. Release of this layer does not offer appreciable laxity when performing advancement flaps.
An 84-year-old man comes to the office because he has had pain and purulent drainage from the left groin incision site since undergoing a left common iliac artery to common femoral bypass procedure performed for critical stenosis of the iliac artery three weeks ago. Temperature is 38.8 °C (101.8 °F), blood pressure is 140/90 mmHg, and pulse rate is 100/min. Physical examination shows an exposed vein graft at the groin incision site. A magnetic resonance angiogram shows a patent bypass graft; the superficial femoral artery is patent, but a profundus branch is occluded. Following debridement, wound coverage with which of the following flaps is the most appropriate next step?
(A) Anterior lateral thigh
(B) Gracilis muscle
(C) Rectus femoris muscle
(D) Sartorius muscle
(E) Vastus lateralis muscle
The correct response is Option D.
The sartorius muscle would provide the most reliable option for wound coverage for the patient discussed. The sartorius muscle flap originates from the anterior iliac spine and inserts into the medial tibia. Eight to eleven perforators off the superficial femoral artery segmentally supply the sartorius, a type V muscle flap. The proximal pedicle is located approximately 6 cm from the anterior superior iliac spine. The sartorius muscle is adjacent to the femoral vessels.
The anterior lateral thigh, rectus femoris, and vastus lateralis muscles all are supplied by branches of the lateral femoral circumflex vessel. The gracilis muscle is supplied by the medial femoral circumflex artery. Both medial and lateral circumflex arterial branches originate from the proximal portion of the profunda femoris artery. Occlusion of the profunda would make the use of these flaps risky and may result in flap loss.
The rectus femoris muscle is a type I muscle flap with a single dominant blood supply from the lateral femoral circumflex artery.
In a patient who has undergone resection of a squamous cell carcinoma of the floor of the mouth, which of the following free flaps will provide vascularized bone and a sensate skin paddle?
(A) Iliac crest flap
(B) Lateral arm flap
(C) Parascapular flap
(D) Serratus anterior flap
The correct response is Option B.
Because the lateral arm flap provides both vascularized bone and a sensate skin paddle, it is best used for reconstruction of this patient’s defect involving the floor of the mouth. Vascularity and skin sensibility are provided by the radial collateral artery and posterior brachial cutaneous nerve (C5-6), respectively. As much as 7 cm * 12 cm of skin can be elevated with the flap; in addition, because of its periosteal attachments, as much as one-third of the posterior lateral humerus (or 10 cm to 15 cm in length and 1 cm to 1.5 cm in diameter) can be harvested.
The iliac crest osteocutaneous flap, which is based on the deep circumflex iliac artery, can provide a skin paddle as large as 12 cm * 6 cm and a bone segment as large as 8 cm ( 18 cm. Although this flap can be used for reconstruction of large mandibular segments and extensive soft-tissue defects, the skin component is bulky and insensate. Meticulous closure of the donor site defect is required to prevent hernia formation.
The parascapular flap is based on the circumflex scapular artery. Advantages of this flap include multiple skin paddles, a large segment of bone, and a high degree of independent motion between the skin and bone segments. The serratus anterior and/or latissimus dorsi muscles can be included with the flap to reconstruct complex defects. However, the skin paddles of this flap are also bulky and lack a cutaneous sensory nerve.
The serratus anterior flap is extremely versatile. Skin, muscle, and an iliac bone graft can be included with this flap; its pedicle is long and has a large diameter. It can be harvested as a functional muscle flap with inclusion of the branches of the long thoracic nerve; however, the upper four to five muscle slips must be preserved in order to prevent winging of the scapula. This primary disadvantage of this flap is that any bone incorporated with it will be less substantial and have poor vascularization when compared with other osteocutaneous flaps. The skin component of this flap is also insensate.
A 59-year-old man comes to the office for follow-up examination three weeks after undergoing left total knee replacement. Physical examination shows a draining sinus on the distal aspect of the knee. Surgical removal of the hardware and flap reconstruction are planned. Which of the following is the dominant pedicle to the muscle flap that is most appropriate for reconstruction?
(A) Anterior tibial artery
(B) Ascending branch of the medial circumflex femoral artery
(C) Medial sural artery
(D) Perforating branch of the distal superficial femoral artery
(E) Proximal branches of the posterior tibial artery
The correct response is Option C.
The muscle flap best suited to reconstruct this defect is a medial head of gastrocnemius muscle rotation flap. Its dominant pedicle is the medial sural artery, which is a branch of the popliteal artery.
The ascending branch of the medial circumflex artery is the dominant pedicle to the gracilis flap, whereas the minor pedicles are perforating branches of the distal superficial femoral artery. A proximally based gracilis flap would not have the arc of rotation to adequately cover the knee. A distally based flap would require a delay procedure and is not the best choice for this defect.
The lateral sural artery is the dominant blood supply to the lateral head of the gastrocnemius, which is smaller, and, therefore, not as well suited for coverage of large patellar defects such as this one.
The soleus is based off the proximal two branches of the posterior tibial artery, branches of the proximal popliteal, and branches of the peroneal artery. It is used for reconstruction of defects of the middle third of the lower extremity and does not have an arc of rotation sufficient enough to cover this defect.
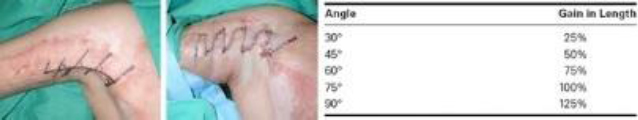
A 40-year-old man sustains burns to 35% of his total body surface area, including the neck, chest, axillae, and upper extremities. After skin grafting, a right anterior axillary dome scar contracture develops. The patient is scheduled for scar revision using Z-plasty. Which lateral limb angle results in a theoretical 75% gain in central limb length?
A) 30 degrees
B) 45 degrees
C) 60 degrees
D) 75 degrees
E) 90 degrees
The correct response is Option C.
The standard Z-plasty involves three incisions of equal length (two limbs and one central incision) and two equal angles. The central incision runs parallel to the scar, which may be excised with the fusiform defect acting as the central incision.
The resulting triangular skin flaps are transposed so the new central incision is perpendicular to the original. After closure, the scar is reoriented along the limb incisions, increasing the length of the original scar. This characteristic is useful for releasing scar contractures, as in this case. As the central incision lengthens (with a constant angle), the resultant scar also lengthens. Additionally, increasing the angles between the limbs (with a constant limb length) also increases the resultant scar.
Which of the following is NOT an indication for Z-plasty?
(A) Adjusting soft-tissue contour
(B) Dispersing linear scars
(C) Lengthening linear scar contractures
(D) Preventing burn scar contractures
The correct response is Option D.
The Z-plasty is a fundamental plastic surgery technique that involves the elevation and interposition of two equal, interposed triangular skin flaps. This procedure can be used to improve soft-tissue contour via reorientation of skin, realign scars within the lines of minimal tension, and lengthen linear scar contractures. However, it is not performed for prevention of burn scar contractures.
A 35-year-old paraplegic man presents with a 5 × 5-cm pressure ulcer over his left ischium involving the skin, subcutaneous tissue, and bone. After debridement, a gluteal rotation flap is planned for closure. Compared with a transposition flap, which of the following is the most significant benefit of using a rotation flap for coverage of this patient’s wound?
A) Ability to reuse flap for future surgery
B) Decreased recurrence rate
C) Improved pressure relief
D) Improved scar placement
E) Improved vascularity
The correct response is Option A.
Ischial pressure ulcers can be one of the most difficult wounds for which to achieve long-term coverage and success. The best outcomes arise from multidisciplinary care teams that focus on pressure alleviation (both perioperative and chronic), nutrition, smoking cessation, muscle spasm management, and vigilant observation. Despite best efforts, ischial pressure ulcers still have up to a 70% recurrence rate. Because of high recurrence rates, surgical planning needs take potential future wounds into consideration. Large rotation or advancement flaps have the benefit of being able to be re-rotated or re-advanced, whereas transposition flaps do not, and can make future surgery more difficult. With good surgical planning, rotation and transposition flaps would not have a difference in vascularity, scar placement, pressure relief, or recurrence rates.
During dissection for a microsurgical free parascapular flap, the circumflex scapular artery is located in the triangular space bordered by the teres minor, the long head of the triceps, and which of the following muscles?
(A) Infraspinatus
(B) Latissimus dorsi
(C) Subscapularis
(D) Teres major
(E) Trapezius
The correct response is Option D.
The scapular area supplied by the circumflex scapular artery is a commonly used donor site in reconstructive microsurgery because of the consistent and reliable vascular anatomy, easily accessible pedicle, and good vessel diameter and length. The circumflex scapular artery arises from scapular artery approximately 3 to 4 cm from its origin at the axillary artery. It then passes through the triangular space, which is bordered above by the teres minor, the teres major below, and the long head of triceps laterally. Flap size can reach 10 × 25 cm with generally closure of the defect directly with acceptable scarring. Parascapular osteocutaneous flaps can also be harvested using the lateral border of the scapula, which is useful for reconstruction of the hand and face.
A 35-year-old man is undergoing repair of a pressure sore on the left ischium using the musculocutaneous flap shown in the photograph. Which of the following is the Mathes and Nahai classification of this flap?
A ) Type I
B ) Type II
C ) Type III
D ) Type IV
E ) Type V
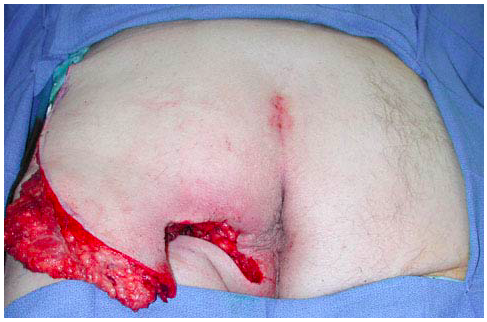
The correct response is Option C.
The gluteal musculocutaneous flap is a Type III flap, meaning it has two dominant pedicles (the superior and inferior gluteal arteries). These arteries are separated by the piriformis muscle and are sourced to the internal iliac system.
A Type I flap has a single dominant pedicle (ie, tensor fascia lata). A Type II flap has dominant and minor pedicle(s) (ie, gracilis). A Type IV flap has multiple segmental pedicles (ie, sartorius). A Type V flap has a dominant pedicle and secondary segmental pedicles (ie, latissimus).
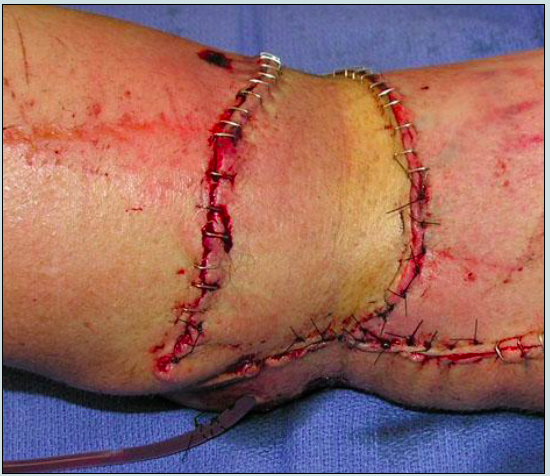
A 48-year-old man is brought to the emergency department after being involved in a high-speed motorcycle collision. Physical examination shows comminuted fractures of the left radius and ulna. A photograph of his wounds is shown. After debridement of the necrotic tissue, the brachial vessels and median nerve are exposed. Microsurgical techniques are not available. Which of the following is the most appropriate choice for tissue coverage in this patient?
A ) Groin flap
B ) Lateral arm flap
C ) Posterior interosseous artery flap
D ) Radial forearm flap
E ) Split-thickness skin graft
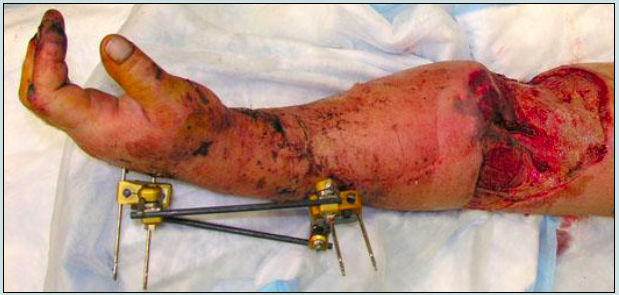
The correct response is Option B.
The vascular supply of the lateral arm flap is from the posterior radial collateral artery, a terminal branch of the deep brachial artery. This artery communicates distally with the ulnar artery, allowing the flap to be raised in a distally based fashion, as it was for the patient in this item. For most adult patients, a 12 × 6-cm flap can be harvested and still allow for primary donor site closure. The major extremity vessels are not disturbed with the harvest of this flap.
A groin flap would be difficult to mobilize sufficiently to reach the defect shown. It would also require leaving the arm attached to the torso for several weeks for vascular ingrowth prior to division and inset.
The posterior interosseous artery flap is based on the communication between the anterior and posterior interosseous arteries just proximal to the distal radioulnar joint. Its pedicle can be used in a distally based fashion to allow for coverage of defects of the hand and wrist. It cannot reach to cover defects at the elbow.
A radial forearm flap has two major disadvantages. It will remove a major vessel to a wrist and hand that is needed to heal a severe injury. It will also expose the radius fracture, requiring secondary flap reconstruction of the donor site. Split-thickness skin grafting is inappropriate to place over an exposed nerve, as sensitivity and pain would be expected to persist after healing. In addition, a skin graft would suffer secondary contraction, which would impair elbow extension.
A 25-year-old woman sustains a contact injury to the posterior aspect of the scalp. Following debridement, she has a 6 * 4-cm defect of the posterior scalp with exposed bone. Which of the following is the most appropriate next step in management?
(A) Excision and primary closure
(B) Full-thickness skin grafting
(C) Coverage with a rotation flap
(D) Hair transplantation
(E) Tissue expansion
The correct response is Option C.
In this 25-year-old woman who has a 6 * 4-cm defect of the posterior aspect of the scalp, the most appropriate management is coverage of the defect using a rotation flap. This flap provides local hair-bearing tissue and can be used to cover defects as large as 6 cm. In order to advance an adequate length of flap, multiple relaxing incisions must be performed within the galea. If the galea is not carefully divided, injury to the subcutaneous vessels or hair follicles may result, leading to the onset of alopecia or delayed wound healing.
Tissue expansion is most appropriate for patients who have large defects of the scalp (typically greater than 15%) because the scalp defect will be covered with similar tissue. Donor site scarring is not a factor in most cases, and the expanders can be left in place if further tissue expansion is required. In addition, the hair follicles will be oriented correctly; as much as 50% of the scalp can be covered with expanded tissue without altering hair growth. However, the process of tissue expansion involves multiple procedures and frequent office visits over a lengthy period of time. During the expansion process, the patient often expresses displeasure with his/her physical appearance.
Excision and primary closure combined with extensive undermining are only appropriate for patients who have defects measuring less than 5 cm. Patients with small areas of scalp alopecia may undergo multiple staged excisions of the alopecic scalp followed by advancement of hair-bearing tissue. Because this process involves fewer procedures and less follow-up, it can be used as an alternative to tissue expansion.
Although a full-thickness skin graft can be used for temporary wound coverage in a patient who will undergo further scalp reconstruction, it is not an appropriate long-term treatment because many donor sites do not provide adequate hair-bearing skin.
Hair transplantation is currently being used with increasing regularity for treatment of traumatic or age-related alopecia.
A 50-year-old man is scheduled to undergo mandibulectomy with floor of mouth resection for cancer. An osteocutaneous radial forearm free flap is being considered. Which of the following is the strongest contraindication to performing this flap?
A) Abnormal Allen test
B) Anterior mandibular tumor location
C) Defect length of 8 cm
D) History of prior radiation
E) Lack of availability of ipsilateral neck muscles as recipients
The correct response is Option A.
The osteocutaneous radial forearm free flap (OCRFFF) is based on the radial artery, one of the major sources of blood to the hand. An abnormal Allen test is a sign of insufficient ulnar artery blood flow and would be a major contraindication to utilizing this flap.
While the quantity of bone available for transfer from the radius is thought of as a limitation of this flap, many authors have reported safely harvesting up to 10 cm or more of bone length. The thickness of the bone is also a limitation and it is recommended that no more than one-third to one-half of the bone thickness be harvested to avoid an iatrogenic radial fracture, even when the remaining bone is prophylactically plated and/or bone grafted. Because of this, osseointegrated implants for dental restoration can rarely be performed. The bone component of the OCRFFF is well vascularized and associated with high rates of union and can tolerate osteotomies needed for anterior mandible restoration as well as be used for closing irradiated wounds. An advantage of this flap, in addition to providing a thin, pliable skin paddle, is that it has a long pedicle length that can often reach the inspilateral transverse cervical blood vessels or contralateral neck blood vessels without the need for interposition vein grafting.
A patient with a complex defect that requires replacement of skin, muscle, and bone is scheduled to have reconstruction with a single free flap from the subscapular system. Which of the following would NOT be used as part of this reconstruction?
A) Parascapular fasciocutaneous tissue
B) Serratus anterior muscle
C) Trapezius muscle
D) Vascularized rib
E) Vascularized scapular bone
Correct answer is option C.
Unlike the other tissues, the trapezius muscle is based on the transverse cervical artery (based on the thyrocervical trunk in 80% of cases or the subclavian artery in 20% of cases). The subscapular system allows for the creation of chimeric flaps that can include bone, muscle, fascia, fat, and skin. Flaps that have been used include the serratus anterior muscle and fascia, latissimus dorsi muscle and fascia, scapular and parascapular fascia and overlying skin, and scapular and rib bone. Such combinations allow for versatility in reconstructing complex three dimensional defects that are often encountered in the face.















































