Define ARDS.
ARDS/acute lung injury, may be caused by direct lung injury or occur secondary to severe systemic illness. Lung damage and release of inflammatory mediators cause increased capillary permeability and non-cardiogenic pulmonary oedema, often accompanied by multiorgan failure.
BMJ: Acute respiratory distress syndrome (ARDS) is a non-cardiogenic pulmonary oedema and diffuse lung inflammation syndrome that often complicates critical illness.If no risk factors for ARDS are present, then acute pulmonary oedema as a result of heart failure should be ruled out.
What are the three criteria for ARDS?
The diagnosis of ARDS is based on fulfilling three criteria:
- Acute onset (within 1 week)
- Bilateral opacities on chest x-ray
- PaO₂/FiO₂ (arterial to inspired oxygen) ratio of ≤300 on positive end-expiratory pressure (PEEP) or continuous positive airway pressure (CPAP) ≥5 cm H₂O.
What is the epidemiology of ARDS?
- Incidence in Europe is about 18/100,000
- No differences in incidence between men and women
- Greater incidence in the elderly
- Mortality is 40-50%
What are the risk factors for ARDS?
Pulmonary:
- Pneumonia - due to inflammation and direct injury by pathogen
- Gastric aspiration - causes direct injury to alveolar epithelium and alveolar-capillary membrane
- Drowning - but fast recovery
Other:
- Sepsis - systemic activation of inflammation and coagulation lead to indirect alveolar-capillary membrane injury - MOST COMMON RISK FACTOR
- Trauma with shock and multiple transfusions - 7-10% of patients with severe trauma. May be due to indirect injury from early haemorrhagic shock or later onset of multiple organ failure.
- Hypovolaemic shock
- Blood transfusions
- Lung transplantation
- Pancreatitis
- History of alcohol micule
- Burns and smoke inhalation
- Drugs/toxins (aspirin, heroin, paraquat)
- malaria
- obstetric events (eclampsia, amniotic fluid embolus)
Why are these risk factors for ARDS?
- Lung transplantation
- Blood transfusions
- History of alcohol misuse
Lung transplantation - primary graft dysfunction/aRDS occurs in 10-25%; may be due to ischaemic re-perfusion injury.
Blood transfusions - multiple blood product transfusions can cause TRALI; proposed mechanism involves recipient neutrophil activation by donor-antibody recognition of recipient neutrophil epitopes or by biologically active lipids released from stored red blood cells.
History of alcohol abuse is associated with increased incidence of ARDS in adults with septic shock due to depletion of endogenous antioxidants.
What is the pathophysiology of ARDS?
Early phase of ARDS =
- Acute hypoxaemic respiratory failure with increased alveolar-arterial oxygen gradient and poorly compliant lungs.
- Multiple organ damage may occur especially in sepsis. Right ventricular dysfunction is also common and associated with worse outcomes.
After early phase =
- In some patients have rapid resolution and return to normal lung histology and function (oedema is cleared by active transport of Na and Cl across epithelium).
- In others, early exudative inflammatory phase progresses to fibroproliferative phase–> fibrous tissue and collagen deposition, leading to irreversible and catastrophic lung fibrosis –> continued respiratory failure, high minute ventilation and poorly compliant lungs.
- Many different causes of ARDS but usually sepsis or pulmonary. Pathophysiology is not completely understood.
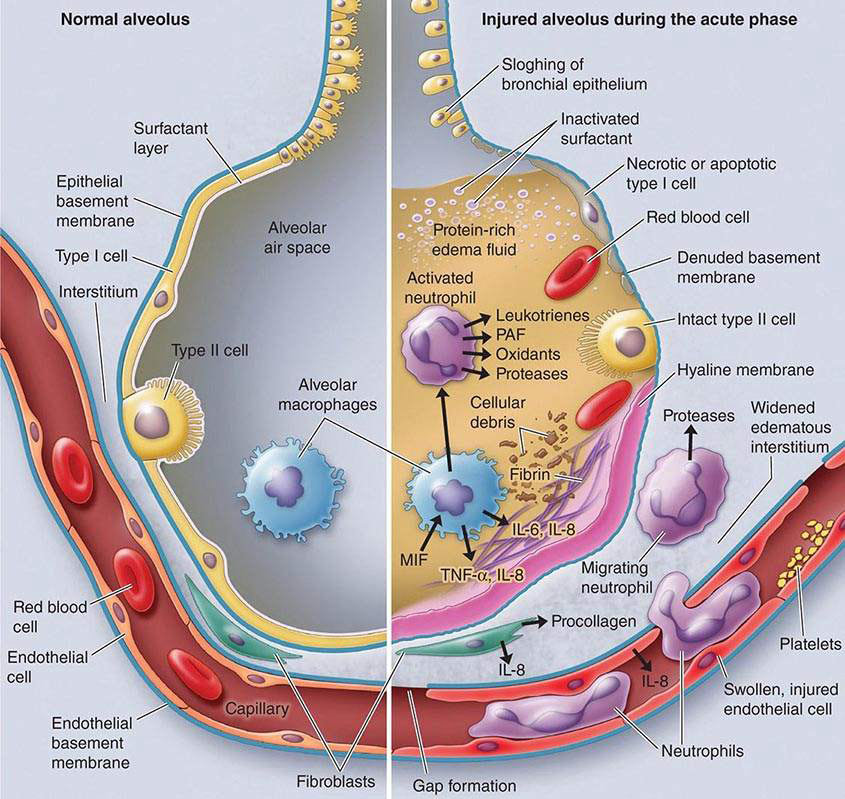
- Diffuse alveolar damage leads to injury to the alveolar-capillary membrane, made up of type I and II alveolar pneumocytes and capillary endothelial cells
- Air paces are flooded by proteinaceous oedema fluid, inflammatory cells and inflammatory mediators including cytokines, lipid mediators and oxidants
- Type I cell necrosis may occur exposing the BM –> fibrin deposition at BM –> hyaline membranes characteristic of diffuse alveolar damage
- Injury to type II cells and alveolar flooding contribute to surfactant dysfunction
- Mechanical ventilation with high pressures and high volumes may injure the lung further and cause a cytokine cascade
What are the signs you would see on physical examination?
- Cyanosis
- Tachypnoea
- Peripheral vasodilation
- Bilateral fine inspiratory crackles (BMJ: pulmonary crepitations)
- Frothy sputum
What are the presenting symptoms of ARDS?
- Critically ill with multi-system organ failure
- Dyspnoea
- Fever, cough, pleuritic chest pain - particularly if the underlying cause is pneumonia.
What investigations would you do for ARDS?
ABG - low PaO2 and a PaO2/FiO2 (inspired oxygen) ratio of over 300 on PEEP (+ve end-expiratory pressure) or CPAP over 5cm H2O is part of diagnostic criteria for ARDS
CXR - shows bilateral pulmonary infiltrates. Good sensitivity but poor specificity becayse could be due to multitude of other conditions.
Amylase and lipase - 3 times the upper limit in acute pancreatitis (common cause of ARDS)
Sputum / blood/urine cultures - if underlying infection
Also: BNP (<100ng makes HF unlikely and ARDS more likely), echo (usually normal),pulmonary artery catheterisation (PAocclusion pressure 18 or less suggests ARDS and excludes HF)
Briefly, how do you manage ARDS?
- Oxygen and ventilation (maintain at 88-95%, usually requires mechanical ventilation with titration of FiO2 [inspired oxygen])
- Prone positioning - only in patients with severe ARDS
- IV fluids - fluid balance should be maintained as slightly negative pr neutral (providing patient is not in shock).
- Treat infection if present
- Rescue therapies -in patients with refractory hypoxaemia despite FiO2 of 1.0 and high levels of PEEP. E.g. neuromuscular paralysis can improve ventilator-patient synchrony and improves oxygenation.
List 5 causes of cor pumonale.
- Lung disease – COPS, asthma, bronchiectasis, pulmonary fibrosis, lung resection
- Pulmonary vascular disease – PE, pulmonary vasculitis, primary pulmonary hypertension, aRDS, SCD, parasite infestation
- Thoracic cage abnormality – kyphosis, scoliosis, thoracoplasty
- Neuromuscular disease – myasthenia gravis, poliomyelitis, MND
- Hypoventilation – sleep apnoea, enlarged adenoids in children and cerebrovascular disease


