Define bronchiectasis.
- Bronchiectasis is the permanent dilation of bronchi due to the destruction of the elastic and muscular components of the bronchial wall.
- It is often caused as a consequence of recurrent and/or severe infections secondary to an underlying disorder.
- The majority of patients will present with a chronic cough and sputum production.
Summarise the epidemiology of bronchiectasis.
- Prevalence in women is higher than men
- In UK incidence is 5 per 100,000
- Prevalence is increasing
- Prevalence higher in >60yr
What are the risk factors for bronchiectasis?
Anything that causes inflammatory damage to the airways. 40% have no clear initiating cause.
- Hx of severe LRTI - most common
- Aspiration/inhalation injury
- COPD
- Immunodeficiency
- Endobronchial tumours
- ABPA
- Connective tissue disorders - RhA
- IBD - e.g. UC>Crohn’s
- Yellow nail syndrome
- Congenital disorders - e.g. Cystic fibrosis, Young’s syndrome, primary ciliary dyskinesia, Mounier-Kuhn syndrome, Williams-Campbell syndrome
Briefly describe these syndromes:
Cystic fibrosis, Young’s syndrome, primary ciliary dyskinesia, Mounier-Kuhn syndrome, Williams-Campbell syndrome
CF - mutation of the CFTR gene leading to abnormalities in the Cl- channel causing viscous mucus and abnormal airway clearance. Also affects Gi tract, pancreas, liver and kidneys.
Young’s syndrome - similar features to CF (incl bronchiectasis, sinusitis, obstructive azoospermia) but without CFTR/Cl- mutations.
Primary ciliary dyskinesia - autosomal recessive disorder → defect in ciliary structure and/or function (Kartagener’s syndrome includes the triad of bronchiectasis, sinusitis, and situs inversus, and occurs in approximately 50% of patients with primary ciliary dyskinesia)
Mounier-Kuhn syndrome - tracheobronchomegaly
Williams-Campbell syndrome - bronchial cartilage deficiency
Which infections predispose to bronchiectasis?
- pneumonia
- pertussis
- pulmonary tuberculosis
- mycoplasma
- influenza or other viral infection.
Infections are associated with bronchial destruction–> bronchiectasis.
Explain the aetiology of bronchiectasis.
The aetiology falls into the following categories:
- Post-infectious
- Immunodeficiency
- Genetic
- Other
How is bronchiectasis classified?
Reid classification (morphological classification, not clinically useful)
- Cylindrical bronchiectasis
- Varicose bronchiectasis = alternating dilation and constriction
- Saccular/cystic bronchiectasis = associated with Pseudomonas; most severe; dilated distally
What are the presenting symptoms of bronchiectasis?
- Cough - long-lasting cough >8weeks
- Sputum production - large volumes daily
- Crackles - early inspiratory crackles
- High pitched inspiratory squeaks.
- Large airway rhonchi (low pitched snore-like sound).
- Dyspnoea
- Fever
- Fatigue
- Chest pain that is present between exacerbations and is usually non-pleuritic
- Haemoptysis
- Rhinosinusitis
- Weight loss
- Wheezing
- Clubbing
How do you diagnose bronchiectasis? What do investigations show?
- sputum culture and sensitivity - check for gram-positive bacteria; gram-negative bacteria; non-tuberculous mycobacteria; fungi
- CXR
- spirometry
- oxygen saturations
- FBC - may reveal high eosinophil count in bronchopulmonary aspergillosis, neutrophilia suggests superimposed infection or exacerbation
Other:
- high-resolution chest CT
- serum alpha-1 antitrypsin phenotype and level
- serum immunoglobulins
- sweat chloride test
- rheumatoid factor
- Aspergillus fumigatus skin prick test
- serum HIV antibody
- nasal nitric oxide (NNO)
- pulmonary function tests
How do you interpret the results of a sweat chloride test?
- >60 mmol/L (>60 mEq/L) cystic fibrosis is likely
- 40 to 59 mmol/L cystic fibrosis is possible
- <39 mmol/L cystic fibrosis is very unlikely
Why are patients with HIV predisposed to bronchiectasis?
Patients with HIV infection are predisposed to developing recurrent sinopulmonary infections and bronchiectasis, which is probably due to abnormal B-lymphocyte function
What does the NNO test look for in suspected bronchiectasis?
NNO - nasal nitric oxide
Done when there is suspicion of primary ciliary dyskinesia (PCD)
A low NNO should be followed up with confirmatory testing (nasal or bronchial brush biopsy for ciliary examination) because other conditions such as cystic fibrosis may present with low NNO.
- LOW (<100 parts per billion) = primary ciliary dyskinesia
- High NNO level excludes a diagnosis of PCD
What does pulmonary function testing show in bronchiectasis?
FEV1/FVC <70%
Reduced FEV1
Elevated residual volume so RV/TLC >35% due to gas trapping
Generate a management plan for bronchiectasis.
- 1st line - exercise(pulmonary rehab) and improved nutrition
- airway clearance therapy
- inhaled bronchodilator
- inhaled hyperosmolar agent -mannitol; nebulised hypertonic saline has been shown to reduce inflammatory mediators, improve sputum bacteriology, and improve quality of life scores
- high risk or known chronic pseudomonal infection - inhaled antibiotic - tobramycin/colistimethate sodium/gentamicin 14days
- recurrent infections/severe haemoptysis/focal disease - surgery to resect bronchiectatic areas of the lung. Lung transplantation in patients with FEV<30%.
- acute exacerbation - short-term oral antibiotics- amoxicillin/clarithromycin
- severe ventilatory failure - non invasive ventilation, supplemental oxygen
What are the complications of bronchiectasis?
Massive haemoptysis (>250mL/day) - recline the patient on the side that bleeding is suspected on. Endotracheal intubation. Thought to originate from bronchial arteries or bronchial-pulmonary anastomoses. (Refer to thoracic surgeon and/or interventional radiologist for bronchoscopy-guided haemostatic tamponade, bronchial artery embolisation, or surgical resection of area)
Respiratory failure - prevent tissue hypoxia by airway protection, oxygen, mechanical ventilation and treatment of underlying cause.
Cor pulmonale - early treatment prevents this. Evidence of pulmonary hypertension –> pulmonologist. Heart/lung transplant may be necessary in severe cases.
What is the prognosis for patients with bronchiectasis?
Prognosis is affected by other respiratory disease that co-exists with bronchiectasis, making it hard to determine.
QOL most affected by dyspnoea, sputum production and reduced FEV1
Pseudomonas species → more severe impairment.
What would you see on a CXR/CT of bronchiectasis?
(CXR with lack of normal tapering producing a tram line below)
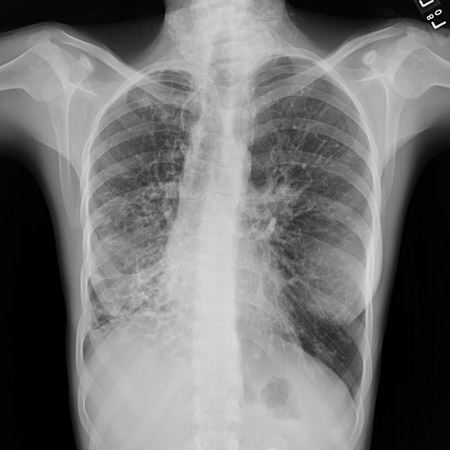
CXR - obscured hemidiaphragm, thin-walled ring shadows with or without fluid levels, tram lines (sign of thickened tapered walls of bronchiectasis), tubular or ovoid opacities
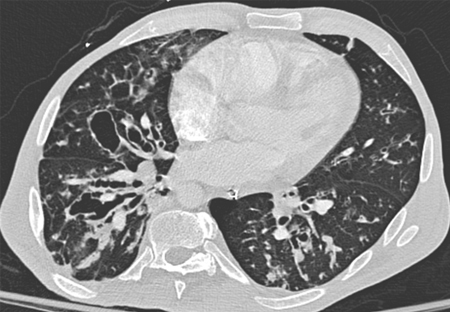
CT - thickened, dilated airways with or without air fluid levels; varicose constrictions along airways; cysts and/or tree-in-bud pattern
How do you treat an acute exacerbation of bronchiectasis?
Usually managed in primary care but some may need hospital admission
Previous microbiology guides antibiotic of choice
If no previous results: amoxicillin or clarithromycin first line


