What is asthma?
Chronic inflammatory disorder of intermittent airway obstruction and hyperactivity. Characterised by recurrent episodes of dyspnoea, cough, and wheeze.
What 3 factors contribute to airway narrowing in asthma?
- Bronchial muscle constriction
- Inflammation (caused by basophil and mast cell degranulation resulting in release of inflammatory mediators)
- Mucus plugging
What precipitates asthma?
- Cold air
- Exercise
- Emotion
- Allergies (house dust mite, pollen, fur)
- Infection
- Smoking and passive smoking
- Pollution
- NSAIDs
- Beta-blockers
What is the diurnal variation seen with asthma?
Morning dip in peak flow
(Also a noctunal cough)
What are the risk factors for asthma?
- Personal or FH of atopy
- Occupational exposure
- Eczema, atopic dermatitis, allergic rhinitis
- Cigarette smoking and vaping
- RSV in early life
- Nasal polyposis
- Exposure to high concentrations of allergens (e.g. house dust mite)
- Air pollution
What should you ask about in a history of an asthma patient?
- Precipitants
- Diurnal variation
- Exercise
- Disrupted sleep
- Acid reflux - sometimes treating reflux improves spirometry
- Other atopic disease - eczema, hayfever
- The home (especially bedroom) - pets, carpet, feather pillows or duvet , other soft furnishings
- Job - paint sprayers, food processors, welders, animal handlers.
- Days per week off work or school
What investigations would confirm asthma?
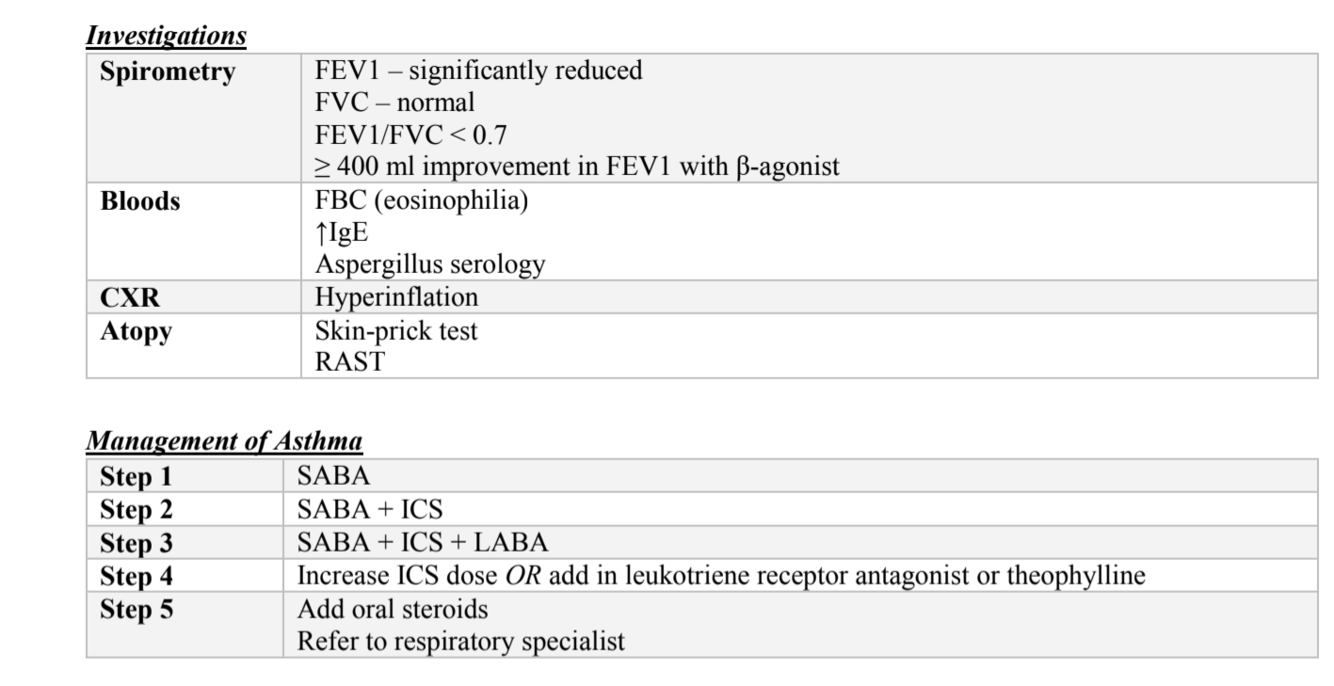
What ABG result would signify that an asthmatic needs to be transferred to ITU?
Normally the PaCO2 should be low in asthma attack but if it is normal or high then they need to be transferred to ITU for ventilation as this signifies a failing respiratory effort.
How do you manage asthma?
BTS guidelines
SABA throughout PRN but if >3 doses/week
- STEP 1 = Asthma suspected - SABA + consider low-dose ICS
- STEP 2 = Regular preventer - SABA + low dose ICS
- STEP 3 = Initial add-on therapy - SABA + low dose ICS + LABA (e.g. salmeterol) (fixed dose or MART)
- STEP 4 = Additional controller therapies - SABA + medium dose ICS OR LTRA +/- stop LABA if not working
- STEP 5 = Specialist therapies - refer to specialist

Describe the different severities of acute asthma.

What signs are associated with asthma?
Tachypnoea
Audible wheeze
Hyperinflated chest
Hyper-resonant percussion note
Decreased air entry
Widespread, polyphonic wheeze
What other differential diagnoses would you consider?
- Pulmonary oedema
- COPD
- Large airway obstruction
- SVC obstruction
- Pneumothorax
- PE
- Bronchiectasis
- Obliterative bronchiolotis
What are some high risk professions for asthma development?

What is the immediate management of acute asthma? What should be considered if the presentation is life-threatening?
- O2 maintain >94%
- SABA nebs 5mg
- Ipratropium bromide nebs 0.5mg +/- continue with the SABA nebs every 4-6hrs if effective
- Prednisolone tablets 40-50mg OD or IV hydrocortisone 100mg 6hrly
- CXR
If life threatening initially also consider:
- Seniors
- SABA NEBS 5mg every 15-30mins
- +/- Magnesium sulfate 1.2-2g IV over 20mins
If initial acute asthma management does not work after 15-30mins what should be considered?
- Continuous nebs of SABA at 5-10mg/hr
- Continue ipratropium bromide nebs every 4-6hrs
- Discuss with ICU
- Add IV magnesium sulfate 1.2-2g over 20min
- Add IV SABA
- OR Add IV aminophylline
- Mechanical ventilation
When can you discharge patients after an acute asthma attack?
- PEF >75% of predicted + PEF variability <25%
- Taking discharge meds for 12-24hrs already, PEF meter given, written action plan
- Prednisolone 40-50mg 5 days
Follow ups:
- GP follow up in 2 days
- Resp clinic follow up in 4 weeks
What is the normal PEFR in a 167cm female aged 25yrs?
~430 L/min

By what time point should SABA nebs be started in ED?
By 5mins
Reassess by 15-20mins
When should you admit a patient with acute asthma?
Life threatening features
Severe asthma features
Previous near fatal asthma
Afternoon or evening attack - have lower threshold for admission
What is the usual acute asthma action plan for patients to try at home?
10 puffs of salbutamol 4hrly
What are the signs and symptoms of life-threatening asthma?
- Exhaustion
- Hypotension
- Cyanosis
- Silent chest
- Poor respiratory effort
- Confusion


