What are the layers of the gut?
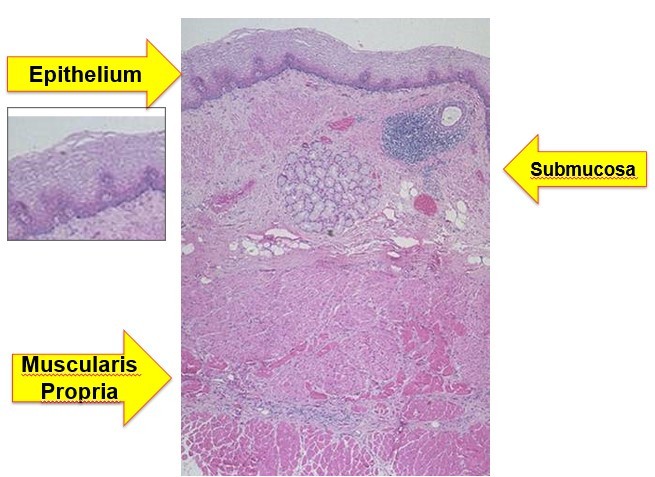
What is the Z line?
Transitional line from squamous to columnar
What are the parts of a normal stomach?
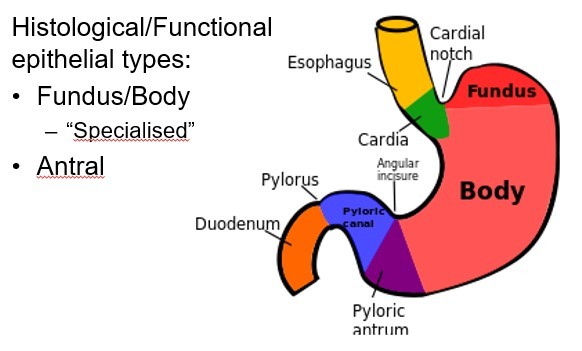
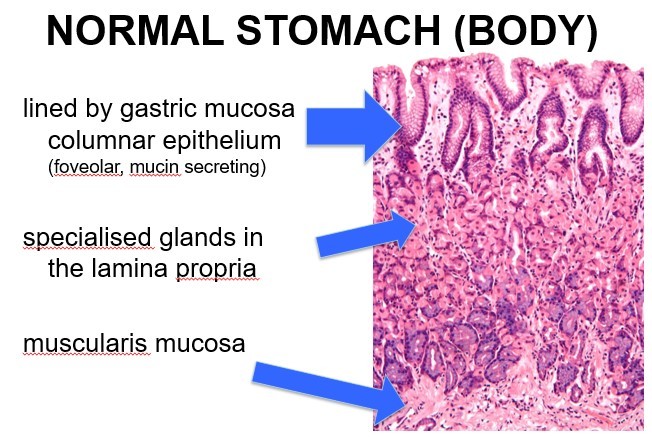
What are the layers of the stomach in the body?
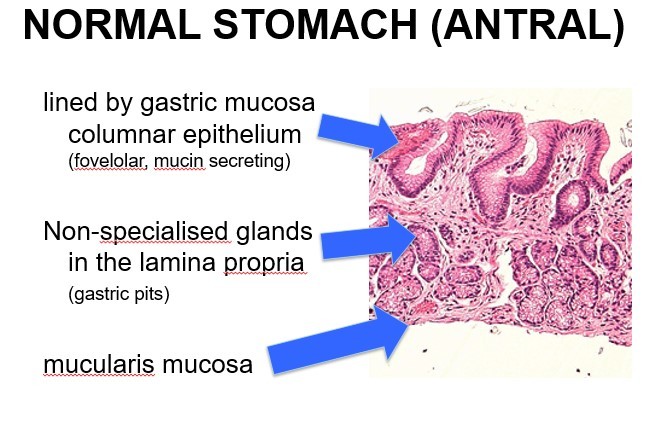
What are the layers of the stomach in the antrum?
What is normal duodenal epithelium?
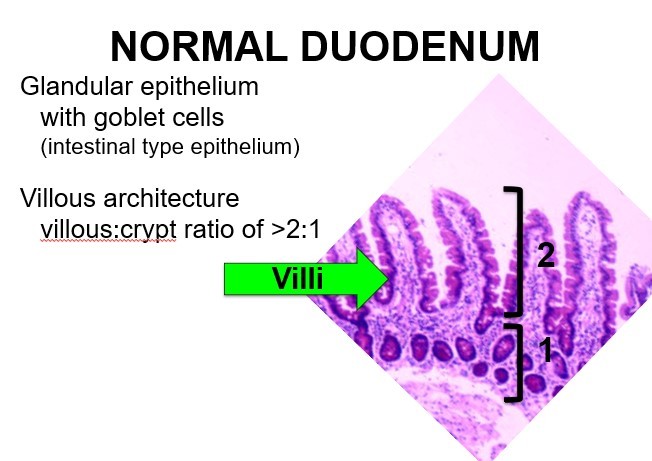
What is this?
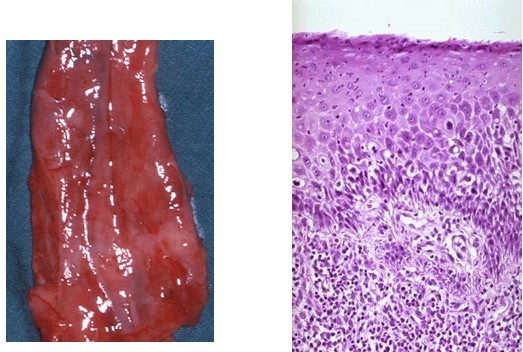
Acute oesophagitis
What is the presentation and complications of GORD?
- Gastro-oesophageal reflux disease
- Commonest cause of oesophagitis
- Reflux of acidic gastric contents
Ulceration
–necrotic slough
–inflammatory exudate
–granulation tissue
•Fibrosis
Complications
- haemorrhage
- perforation
- stricture
- Barrett’s oesophagus
What is this?
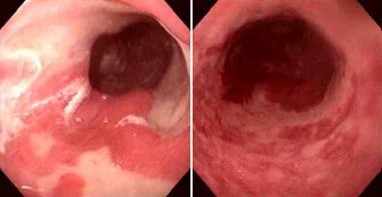
BARRETT’S OESOPHAGUS
•Re-epithelialisation by metaplastic columnar epithelium usually with goblet cells
(intestinal type epithelium)
•AKA columnar lined oesophagus (CLO)
What is 1,2 and 3?
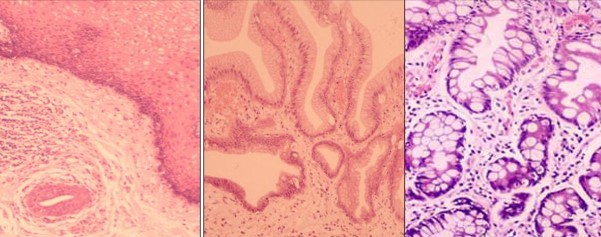
- Normal
- CLO
- CLO with IM
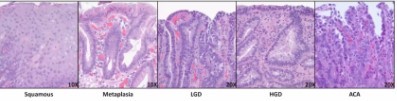
What changes lead to cancer?
Metaplastic glandular epithelium (intestinal type)
Dysplasia changes showing some of the cytological and histological features of malignancy but no invasion through the basement membrane
Adenocarcinoma invasion through the basement membrane
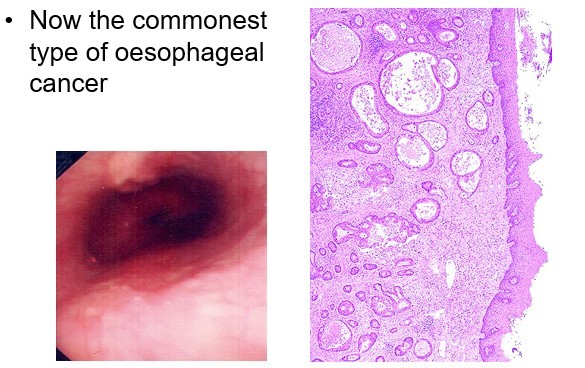
What is the most common type of oesophageal cancer?
Adenocarcinoma of the oesophagus (lower- associated with reflux)
What is this?
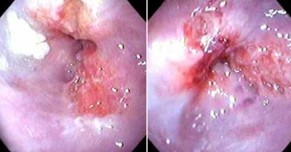
- Associated with alcohol and smoking
- Mid/lower oesophagus
- Invasion into the submucosa
What is this?
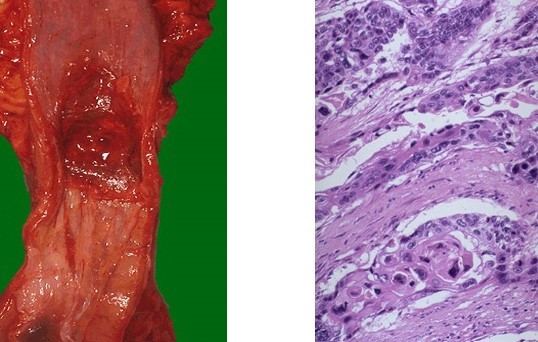
SCC of oesophagus
What is the prognosis of an oesophageal carcinoma?
- Prognosis poor
- Diagnosis of pre-invasive stage important
What is the oesophageal varices?
caused by: cirrhosis, Budd Chiari/ PV thrombosis
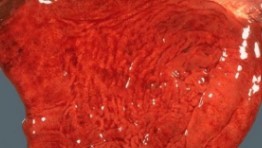
What is gastritis?
- inflammation of the gastric mucosa
- Acute gastritis - acute insult
- Chronic gastritis - chronic / persistent insult
What might cause acute gastritis?
Chemical
- aspirin/NSAIDs
- alcohol
- corrosives
Infection
e.g. Helicobacter pylori
What causes chronic gastritis?
- H. pylori associated
- Chemical (NSAIDs, bile reflux; antrum )
- Autoimmune (body, auto-antibodies e.g. antiparietal)
- Lymphocytes +/- Neutrophils
Mucosal Associated Lymphoid Tissue (MALT)induction
What is H Pylori associated gastritis?
•Cause
H. pylori
•Pattern
chronic gastritis +/- activity
•Outcome
CLO-IM-Dysplasia,
Adenocarcinoma
Lymphoma (MALToma)
How is Helicobacter a carcinogen?
- Helicobacter infection is associated with an 8x increased risk of (non-cardia) gastric cancer
- cag-A-positive H.pylori have a needle like appendage that injects toxin into intercellular junctions allowing the bacteria to attach more easily.
- This strain is associated with more chronic inflammation.
- Treatment of the infection with antibiotics drastically reduces the risk of cancer.
What else causes gastritis?
•Infection
e.g. CMV, strongyloides
(immunosuppression)
•Inflammatory bowel disease
Crohn’s Disease
What is this?
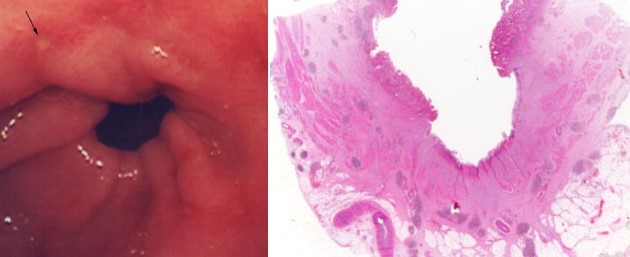
Gastric ulcers
All ulcers should be biopsied to exclude malignancy
What are the complications of ulcers?
•Bleeding
Anaemia
Shock (massive haemorrhage)
•Perforation
Peritonitis





