how do calcium channel blockers work?
what are the two major types? & mech of action for each
- block Ca entry to vascualr smooth muscle and myocardial cells: interrupt excitation-contraction coupling
types:
- *1. dihydropyridine CCBs**: vasodilate dominately. reduced systemic vascular resistance
- *2. non dihydropyridine CCBs:** reduce HR, contractility, conduction. may worsen heart failure tho
what is the green?
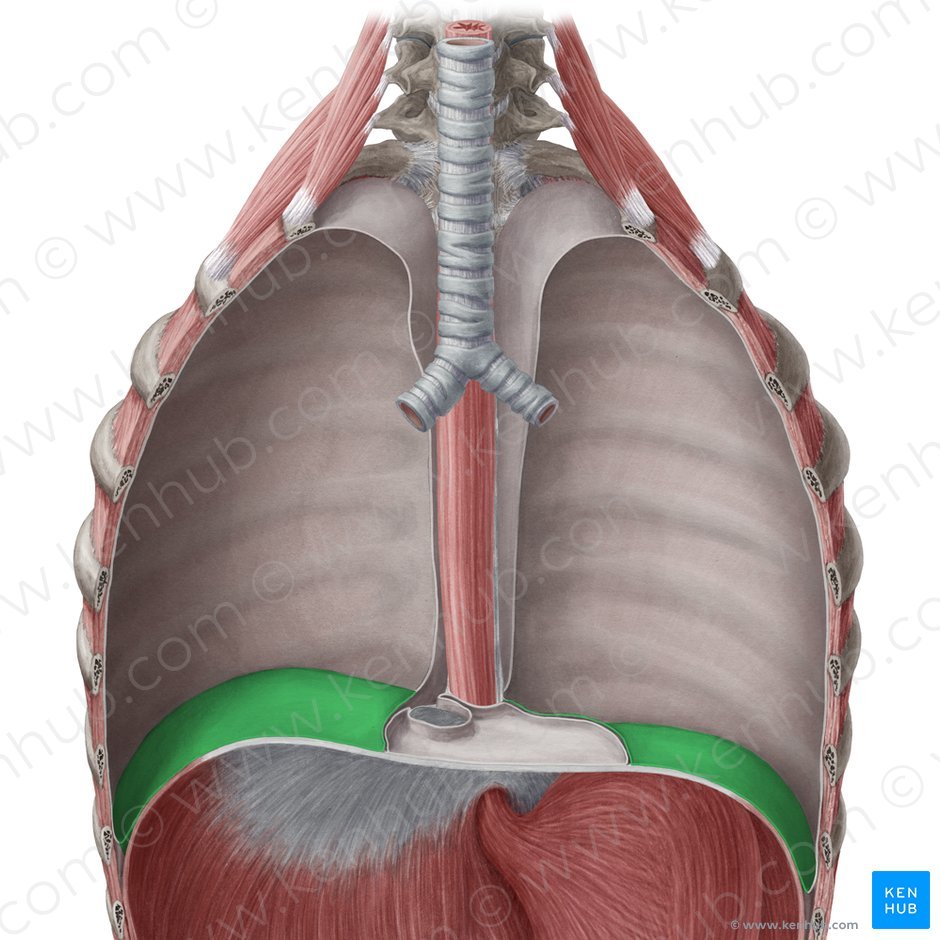
costodiaphragmatic recess :)
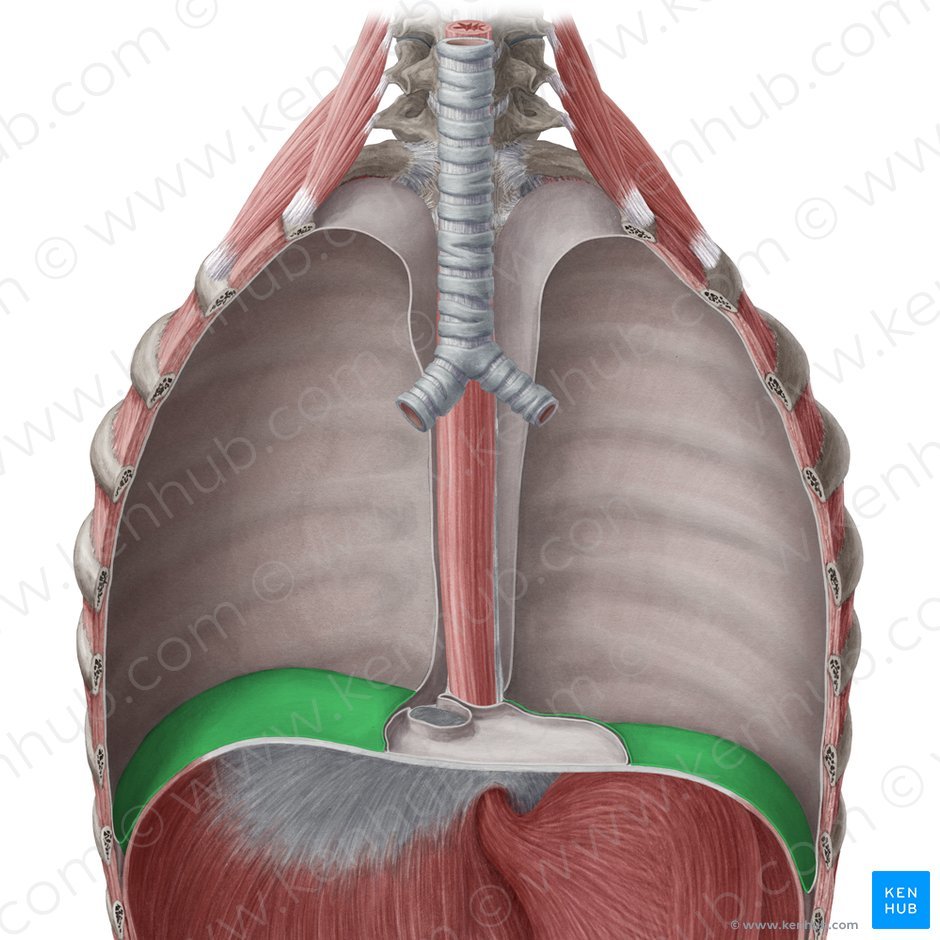
what is the nerve supply to the
i) diaphragmatic pleura? [2]
ii) mediastinal pleura? [1]
i) diaphragmatic pleura: intercostal and phrenic nerves
ii) mediastinal pleura: phrenic nerve
what is the nerve supply to the
i) diaphragmatic pleura? [2]
ii) mediastinal pleura? [1]
i) diaphragmatic pleura: intercostal and phrenic nerves
ii) mediastinal pleura: phrenic nerve
what are major classes of antihypertensive agents? (5)
1. angiotension converting enzyme inhibitors (ACE inhbitors): block conversion of angiotension I to II
2. angiotension II receptor blockers
3. dihydropyridine calcium channel blockers:
4. thiazide diuretics: inhibit Na-Cl contransporter in DCT = natriuresis
5. loop diuretics: Inhibit Na-K-Cl cotransporter in loop of Henle = natriuresis
what is effect of nitroglycerin (and glyceryl trinitrate) in low doses and high doses?
low dose:
- *- decreases preload
- decrease myocardial o2 demand**
high dose:
- *- decreases afterload
- decreaese myocardial o2 demand**
Q
what is MOA for beta blockers for treating angina?
Beta Blockers
- *- B1 receptor antagonist:**
- causes reduced HR (@ SA node)
- decrease in o2 demand at SA node
- negative inotropic effect
- decrease BP
- decreased myocardial oxygen demand
where is sensor for the hormonal control of BP?
JG cells
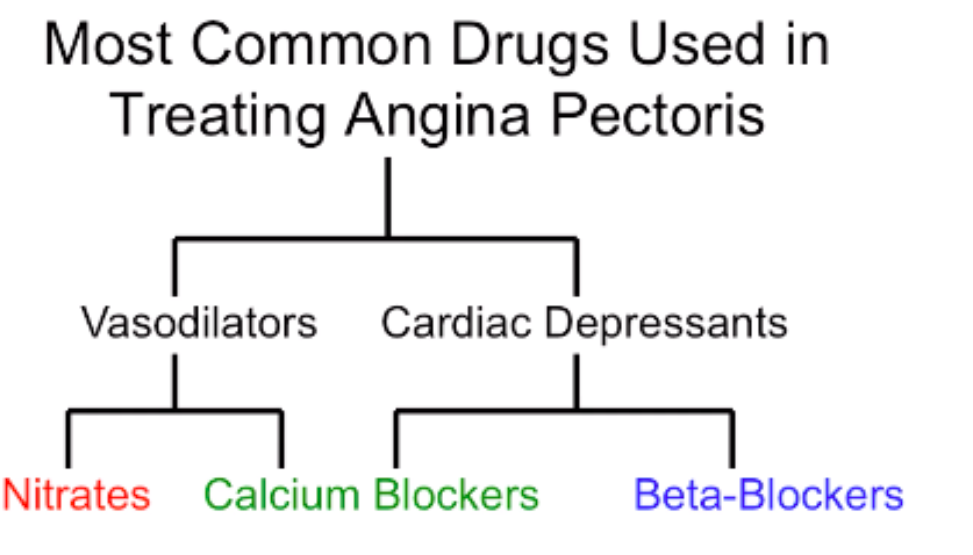
what is angina and how do u treat?
angina - restricted blood supply to heart
what is liddle syndrome / disease?
- enac channels undergo ubiquitination
- this causes inappropriately elevated sodium reabsorption in the distal nephron
- this makes have too much water retention and hypertension
how can sympathetic action of JGA cause a positive feedback of reninn release?
This raises the possibility of positive feedback; sympathetic stimulation increases renin release, angiotensin then increases noradrenaline release which in turn increases renin release leading to hypertension
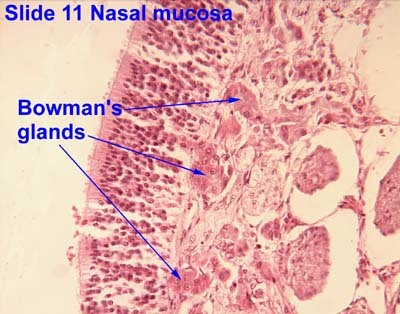
which gland in olfactory cavity produces mucous? [1]
Bowmans glands
what does activation of AT1 receptors cause to occur? [3]
AT1:
i) GCPR which increases Ca entry into smooth muscle & constriction to occur
ii) stimualtes noradrenaline release from sympathetic nerve terminlas (can increase BP via SNS too)
iii) found in cells of adrenal cortex: secretes aldosterone
what is bradykinin & how do ACE inhibitors interact with them?
- bradykinin: 9 amino acid peptire
- ACE inhibitors: increase bradykinin levels by inhibiting its degradation
- causes a dry cough in patients who take ACE inhibitors (why people often stop taking them)
- can cause angioedema - occurs 5x higher in African descent: which is why ACE inhibitors are not the first line of drugs for treating hypertension
why does changing resp. rate impact the excretion of co2 but not o2? [1]
pressure gradient for co2 is much less than for 02 (6 mmHg vs 60 mmHg) changing resp. rate can alter excretion of CO2 without significantly affecting uptake of O
Q
what are the nasopharynx, oropharynx and laryngopharynx innervated by? [3] (theyre different)
nasopharynx: CN V2
oropharynx: CN IX
laryngopharynx: CN X
at which structure does ithe internal laryngeal nerve and superior laryngeal artery enter larnyx?
Internal laryngeal nerve and superior laryngeal artery come through thyrohyoid membrane.
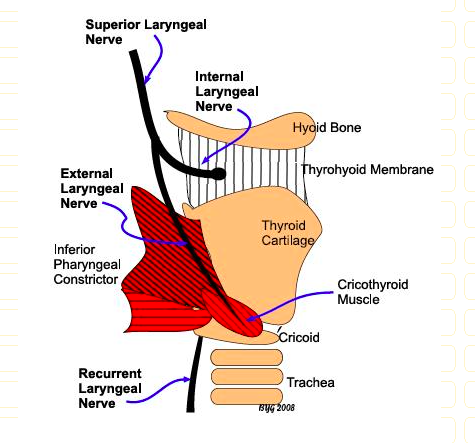
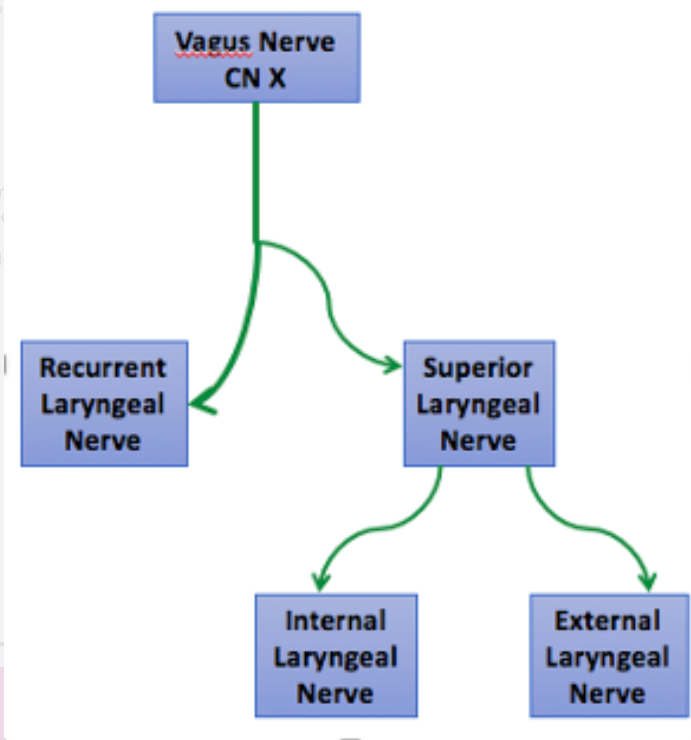
how many cartilages are there in the larynx?
which are the paired
which are the unpaired?
9 cartilages
three unpaired cartilages: epiglottis, thyroid and cricoid cartilage
three paired cartilages: arytenoid, corniculate and cuneiform
what are J receptors?
where found?
stimulated by?
causes?
J receptors:
- location: alveolar walls
- stimulated by: enlargement of pulmonary capillaries / pulm. oedema
- causes: brachycardia, hypotension
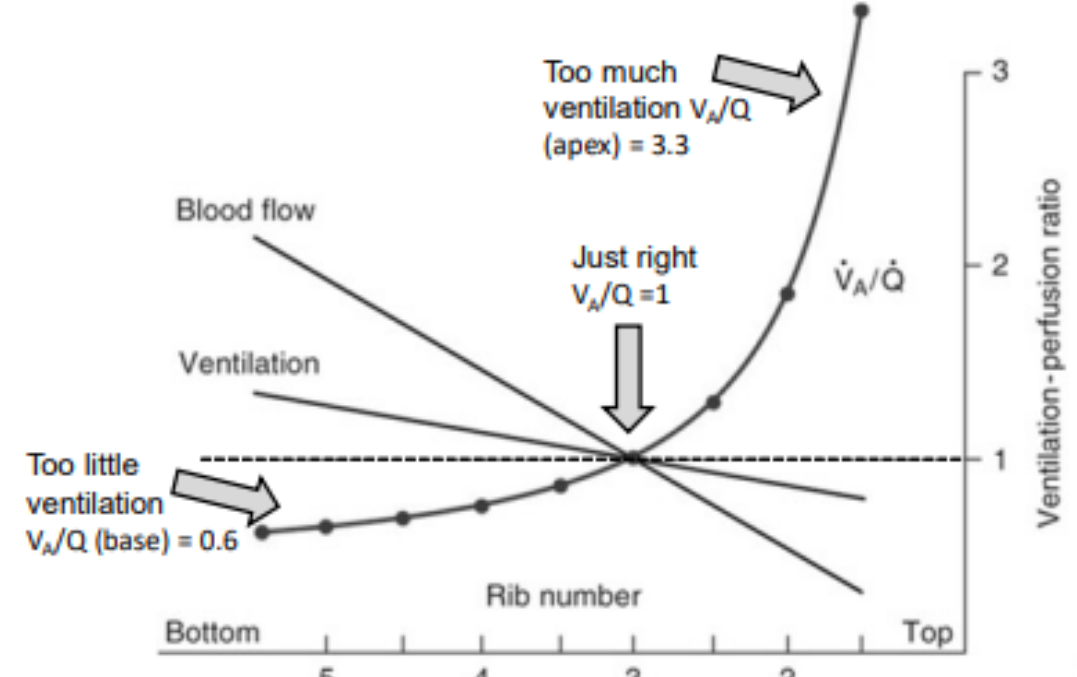
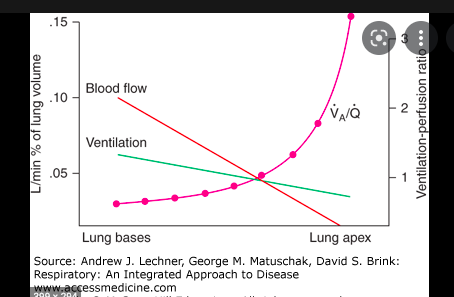
draw a graph of ventilation / perfusion of lungs
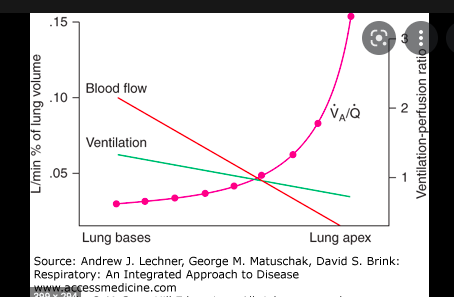
Q
what is ventilation AND blood flow (perfusion) like in base v apex?
which (ventilation or blood flow) shows a steeper decline with height of lung?
- blood flow and ventilation are higher at the base of the lungs c.f apex
- blood flow (Q on graph) shows a steeper decline with height than ventilation
At the base, blood flow is greater than ventilation yet at the apex, blood flow is worse than ventilation
what does hypoxia cause to occur to local blood vessels in alveoli?
hypoxia: causes vasoconstriction of the local blood vessels
If ventilation is reduced in one alveolus, then the capillaries around it constrict, and blood is redirected to better ventilated alveoli.
what is the V/Q (ventilation: perfusion ratio) like at the
a) base of the lung
b) apex of the lung?
what is the V/Q (ventilation: perfusion ratio) like at the
a) base of the lung: less than 1 - around 0.6
b) apex of the lung: more than 1