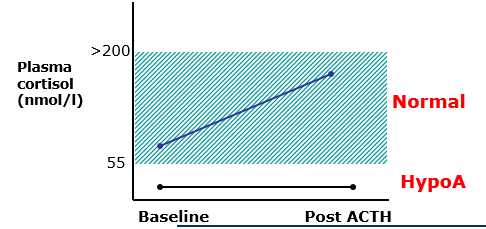
Describe the anatomy of the adrenal cortex?
From outside to the inside:
- Zona glomerulosa (25% of cortex)
- Zona fasciculata (60% of cortex)
- Zona reticularis (15% of cortex)
Outer layer and inner layer tend to be effected by addisons disease.
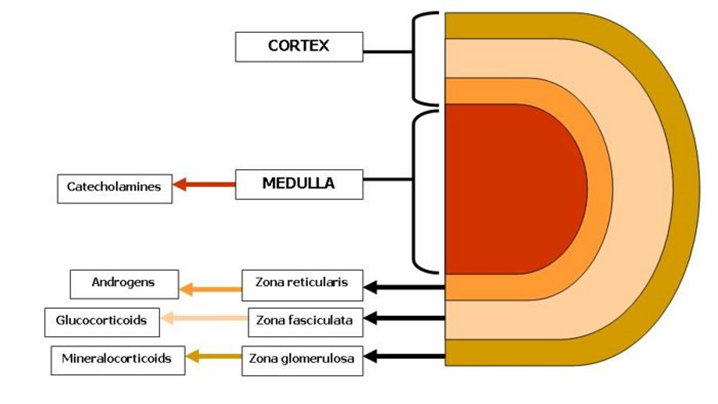
Draw a flow diagram detailing glucocorticoid release and it’s feedback mechanisms?
Describe the actions glucocorticoids?
- Part of the “fight or flight” response
- A “stress” hormone
- Counteracts the effects of stress
- Essential for life!
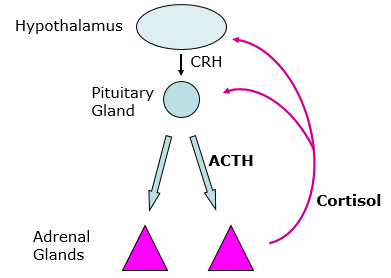
Describe aldosterone regulation?
Renin – angiotensin system
- blood pressure → renin release
- → angiotensin release
- → aldosterone release
Potassium concentration
- very small increases → aldosterone release
Renin release stimulated by:
- Baroreceptors in the wall of the afferent arteriole
- Cells of the macula densa in the early distal tubule which are stimulated by a reduction in Cl delivery
- Cardiac and arterial baroreceptors
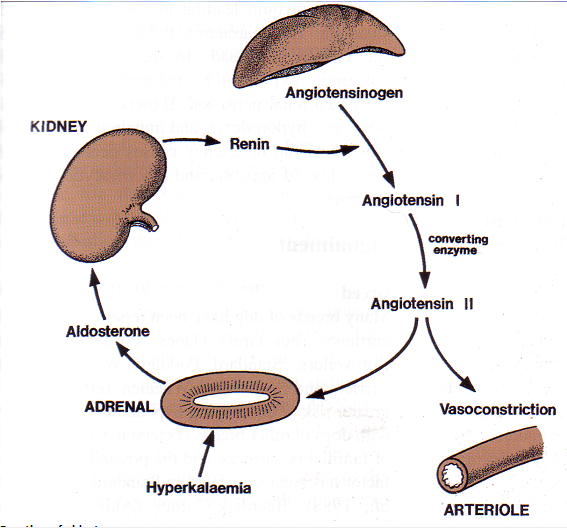
What is the function of aldosterone?
- Plays a central role in the regulation of BP
- Acts on cells of distal tubule and collecting duct to increase reabsorption of Na, Cl and hence water so increased BP
- Stimulates the secretion of K+ into the tubular lumen
- Stimulates secretion of H+ in exchange for K+ in the collecting tubules, so regulating acid/base
- It plays a central role in the regulation of blood pressure mainly by acting on the distal tubules and collecting ducts of the nephron, increasing reabsorption of ions and water in the kidney, to cause the conservation of sodium, secretion of potassium, increase in water retention, and increase in blood pressure and blood volume.
- Water follows Na
What is primary hypoadrenocorticism and what is it also known as?
- Addison’s disease
- Deficiency of glucocorticoids (cortisol) and deficiency of mineralocorticoids (aldosterone)
- Occurs with loss of 85-90% of adrenal cortex
- ACTH tends to be high as the pituitary is screaming at the adrenals to do something and they arent responding
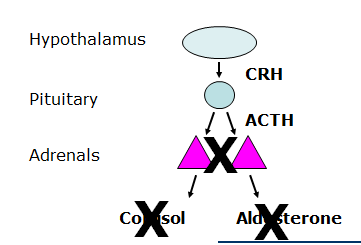
What are some of the causes of primary hypoadrenocorticism in canines?
Idiopathic atrophy
- probably immune-mediated destruction
- associated with other endocrinopathies
Iatrogenic
- drugs: mitotane, trilostane
- surgery: bilateral adrenalectomy
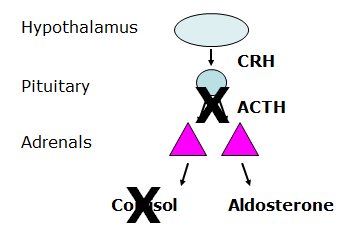
What is Secondary Hypoadrenocorticism?
- Pituitary stops producing ACTH
- Deficiency of ACTH
- Usually only cortisol deficient (electrolytes normal)
- Rare
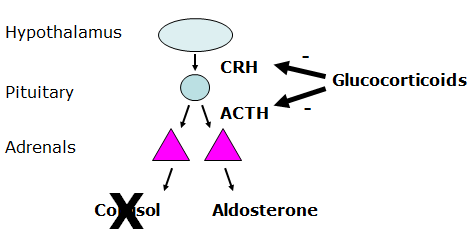
What is Iatrogenic hypoadrenocorticism?
- Exogenous steroids → adrenal atrophy
- oral, injectable, dermatological, otic or ophthalmic preparations
- Cortisol deficiency only
- Glucocorticoids can supress intrinsic adrenal activity. So be careful to taper of steroid drugs.
- Patient may have signs of Cushing’s syndrome whilst on steroids:
- PU/PD, alopecia, pot belly, hepatomegally
- Patient may develop signs of Addison’s disease if steroids abruptly discontinued
- Can be life-threatening
What is the signalment of canine hypoadrenocorticism?
- Young-middle aged dogs. Median age 4-6 years
- 70% females
- Any breed, but certain breed predispositions
- (Extremely rare in cats)
Breeds with an increased risk of hypoadrenocorticism include:
- Standard poodles
- Bearded collies
- Great Dane
- Rottweiler
- WHWT
- Soft coated wheaten terrier
- Nova Scotia Duck Tolling Retriever (can get a juvenille version of addisons disease, present 5months-1year of age with addisons)

What does pathognomonic mean?
A term, often used in medicine, that means characteristic for a particular disease. A pathognomonic sign is a particular sign whose presence means that a particular disease is present beyond any doubt. Labelling a sign or symptom “pathognomonic” represents a marked intensification of a “diagnostic” sign or symptom.
What is the pathophysiology of hypoadrenocorticism?
Aldosterone deficiency
- Loss of Na+, Cl, H20
- Retention of K+, H+
- Pre-renal azotaemia (apparent renal failure)
Glucocorticoid deficiency
- Decreased stress tolerance, gastrointestinal signs, weakness, appetite loss, anaemia, impaired gluconeogenesis
History and clinical signs:
- Chronic: waxing waning form with non-specific signs
- Acute: Addisonian “crisis” form with marked hypovolaemia and azotaemia, hypercalcaemic
What are the clinical signs of chronic hypoadrenocorticism?
- Usually vague and non-specific waxing and waning signs worsened by stress
- Anorexia, vomiting, diarrhoea, weakness, lethargy, depression and weakness
- Shivering, weight loss, PUPD, abdominal pain
- Consider Dx in any animal with waxing/waning signs – especially intermittent GI disease
What are the clinical signs of acute hypoadrenocorticism?
- Signs caused by hypovolaemic shock
- MAY have paradox of relative bradycardia (due to hyperkalaemia)
- Usually collapsed or extremely weak, hypothermic with recent Hx of V+/D+
- Abdominal pain, melena is sometimes a feature and the disease can resemble pancreatitis clinically
- Dehydrated bradycardic depressed dog think addisons
In an acute addisonian crisis what are common presenting signs?
- Depression 87 %
- Thin 82 %
- Weakness 66 %
- Dehydration 41 %
- Bradycardia 22 %
- Melena/hematochezia 17 %
What is the biochemical profile of hypoadrenocorticism?
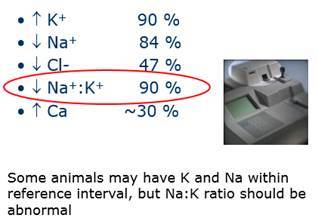
Classic findings
- hyperkalemia (K+)
- hyponatremia (¯Na+)
- hypochloridemia (¯Cl-)
- Na:K ratio <23
- Approx 90% will have one or more of these findings
Due to aldosterone deficiency
- A drop in renal tubular resorption of Na+ and Cl
- A drop in excretion of K+ (and H+) Acid base disturbances because acid not being released into tubule
What does the CBC (complete blood count) look like in a canine with hypoadrenocorticism?
Lack of stress leucogram (reverse stress leukogram)
- Absence of a lymphopenia is a strong indication of addisons.
Anemia (34%-71%)
- erythrocytosis due to lack of cortisol
- GI blood loss
Eosinophilia (10%)
- due to lack of cortisol
Lymphocytosis (13%)
- due to lack of cortisol
What is the biochemical profile and urinanalysis profile for hypoadrenocorticism?
- Azotemia (increase in renal parameters) ~61%
- Drop in urine specific gravity ~90% fails to go up because not enough Na to create a concentration gradient
- inappropriately low in dehydrated animal
- Na+ in urine filtrate impairs ability to retain water → medullary washout
- Hypercalcemia ~30%
- Hypoglycemia ~ 27 %
- Hyopcholseriama
Define azotaemia?
A medical condition characterized by abnormally high levels of nitrogen-containing compounds (such as urea, creatinine, various body waste compounds, and other nitrogen-rich compounds) in the blood.
Define Hyopcholseriama?
The presence of abnormally low (hypo-) levels of cholesterol in the blood (-emia).
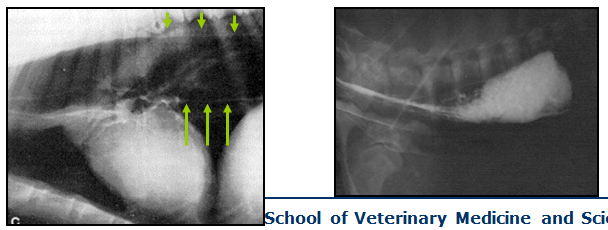
What causes megaoesophagus in hypoadrenocorticism?
Megaoesophagus (< 1%)
- due to muscle weakness??
- Drop in Na+ and K+ → drop in membrane potential
- Drop in cortisol associated with muscle weakness
- typically reversible with treatment
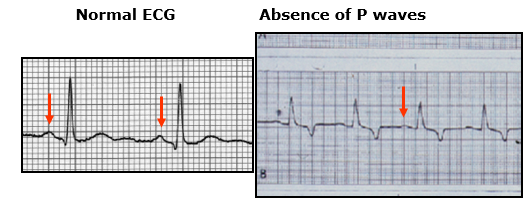
How can hypoadrenocorticism effect an echocardiogram?
Changes related to hyperkalemia (increase in K+)
- bradycardia
- peaked T waves
- widened QRS complexes
- Drop in P wave amplitude become progressively smaller
- disappearance of P waves
- ventricular asystole (failure to contract)
How is hypoadrenocorticism diagnosed?
Maintain high index of suspicion
- electrolyte abnormalities (Na+:K+ ratio <23)
- however not always abnormal
- lack of stress leukogram in sick dog
- young dog with history of chronic illness
- ACTH stimulation test (ask the adrenal glands to do a job and then they don’t do it huge indication of addisons. Take a blood sample of resting cortisol, inject acth then take post blood sample to measure cortisol= expensive)
- Measure cortisol: flat-line stimulation