Why biopsy the skin?
- Establish a definitive diagnosis that cannot be reached by other, less invasive, testing methods
- Rule out certain conditions
Biopsy sampling do’s?
- Be gentle (no squeeze, scrubbing or clipping)
- Biopsy early
- Collect multiple samples representative of the range of the lesions
- Include crusts
- Biopsy before using anti-inflammatory therapy
- Label samples from different areas
- Submit a complete history, full signalment, precise description, list of differentials and a diagram
Do a review of normal histology of skin?
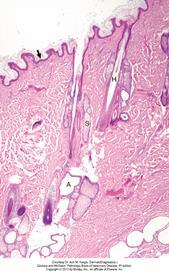
The epidermis (arrow) in haired skin has an undulating surface but lacks rete ridges. The epidermis in haired skin has fewer nucleated cell layers than the epidermis in nonhaired (hairless) skin such as that on the nose and pawpads; thus it is referred to as “thin” skin. Hair follicles (H), apocrine glands (A), and sebaceous glands (S) are present. The haired skin is thickest over the dorsal aspect of the body and on the lateral aspect of the limbs, and it is thinnest on the ventral aspect of the body and the medial aspect of the thighs. H&E stain
Name the different patterns?
Perivascular dermatitis
- Leuokcytes come into the skin, in the dermis (the structure that has blood vessels) – not the epidermis.
Interface dermatitis
- Most of the time hinting at an autoimmune disease
Vasculitis
- Target of inflammation seems to be the vasculature in the dermis. This can be an immune mediated process or a virus; numerous virus that can cause this.
Nodular and/or diffuse dermatitis
Vesicular/pustular dermatitis
- Intraepidermal
- Subepidermal
Folliculitis/furunculosis/sebaceous adenitis
- Inflammation/degeneration centred around hair follicle.
Panniculitis
- Inflammation centred around
Atrophic dermatoses
- Pattern that shows less or no inflammation – more denegerative process, lose skin structures, may be a lack of nutrients etc.
Describe Perivascular dermatitis?
Most common but unfortunately least specific diagnostic pattern
Least specific pattern – it is just inflammation of the skin; leukocytes are sent into the dermis.
- Prominent blood vessels
- Oedema of dermis
- Leukocytes around vessels
- Classified according to depth
- Superficial dermal
- Mid-dermal/perifollicular
- Deep dermal
- Cellular infiltrate varies eg
- Neutrophil
- May be an acute pyoderma etc.
- Neutrophil
- Lymphocytes
- Eosinophil (Type 1 hypersensitivity –parasitic? Allergic?)
- If seen eosinophils, mainly have two pathways: hypersensitivity reaction or parasitic infection.
- Classic examples can be canine atopy, pyoderma, flea bite hypersensitivity…
Describe Interface dermatitis?
- Little bit more serious and specific.
- Band like infiltration of most of the time, lymphocytes that are migrating up into the epidermis. There can be quite cell dense areas, or quite subtle. See degeneration of basal cell layer.
- May see more or less apoptotic keratinocytes – either being attacked or apoptosis is being induced; commonly the case with autoimmune diseases.
- Cell-rich or cell-poor band-like mononuclear infiltrate crossing dermo-epidermal junction
- Hydropic degeneration of basal keratinocytes
- +/- apoptosis (individual cells, mainly in basal layer)
- Pigment incontinence
- Associated with immune-mediated diseases
- Examples for interface dermatitis are dermatomyositis, erythema multiforme , lupoid dermatoses, VKH and many others..
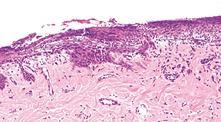
Describe vasculitis?
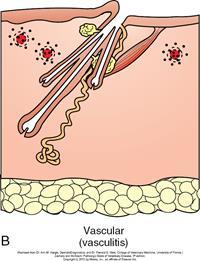
- Inflammation of blood vessels
- Leukocytes come in and target little vascular structures; may see micro-heamorrhages
- Can involve subcutaneous fat tissue.
- Tight perivascular cuffs of inflammatory cells with degeneration of vascular wall
- Suspect if see microhaemorrhages
- Variety of cell types
- +/-
- Panniculitis
- Dermal necrosis
- Atrophy of hair follicles
- Either primary or secondary to inflammation, infection, drug reactions, neoplasia, vaccination
- Can be difficult to find on sampling – need early lesion. Take multiple samples.
- Examples are dermatomyositis, rabies-vaccine induced panniculitis in dogs, pastern dermatitis in horses… also classical swine fever, malignant cattahal fever
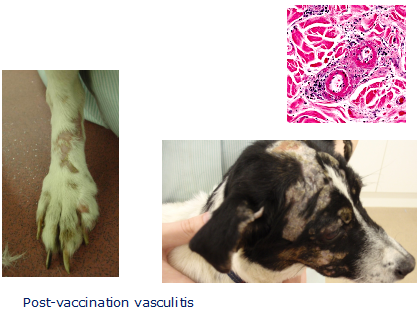
Image showing post vaccination vasculitis. Massive accumulation of Ag.Ab complexes depositing in vascular wall and activating complement cascade = inflammation.
Describe Nodular and/or diffuse dermatitis?
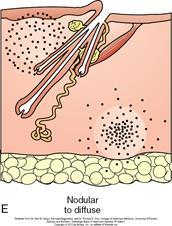
- Can have multifocal nodules – if let them go on, the will coalesce and merge.
- Depending on aetiological agent, cytokines are sent and this will lead to attraction of particular white blood cells.
- Convergence of nodules à diffuse pattern
- Cells vary:
- Neutrophils - pyogenic agents
- Histiocytes/macrophages - FBs, mycobacteria
- Neutrophils and macros – furunculosis, fungi?
- Eosinophilic – parasitic?
- Lymphocytic – insect bites, vaccine reactions
- Very common pattern in the dog.
Describe Intraepidermal vesicular/pustular dermatitis?
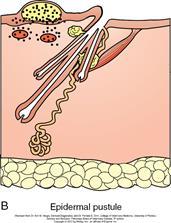
- Vesicle or pustular formation in epidermis = dermatitis(??)
- Clefting in epidermis –> vesicles or pustules
- Vesicular if just normal fluid.
- Pustular if infected, full of lots of neutrophils etc.
- Due to
- Spongiosis (intercellular oedema in epidermis)/epidermal inflammation
- parasites, infection
- Acantholysis
- infection, autoimmune disease
- Spongiosis (intercellular oedema in epidermis)/epidermal inflammation
- Intracellular oedema
- mechanical forces
The pattern of Intraepidermal vesicles/pustules is further classified by:
Position
Subcorneal (ie v superficial)
- Pemphigus foliaceus (PF), pyoderma
Suprabasilar (ie deeper)
- Pemphigus vulgaris
In follicular external root sheath
- PF
Cellular infiltrate
Neutrophils
- Bacterial pyoderma, PF
Eosinophils
- PF, parasite
What is this dog suffering from?
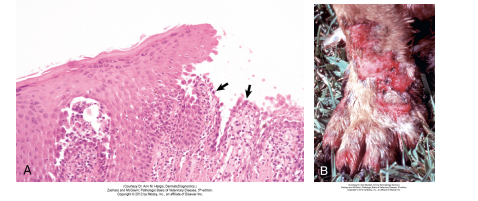
Pemphigus vulgaris, skin, dog. A, Suprabasilar clefting has left a row of basal cells (arrows) attached to the dermis. The single row of basal cells is fragile and easily damaged leading to formation of ulcers, with subsequent fluid loss and secondary bacterial infection. H&E stain.
B, Leg. Note the erythema and large confluent areas of ulceration. In contrast to pemphigus foliaceous (more commonly characterized by erosions and crusts), pemphigus vulgaris is characterized by larger more confluent ulcers because the acantholysis in pemphigus vulgaris occurs deeper in the epidermis (in the cells of the lower epidermis). Vesicles are not frequently seen as they rapidly progress to ulcers, the more common clinical lesion.
Describe Subepidermal vesicular/pustular dermatitis?
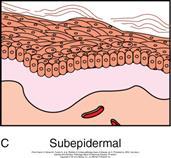
- Rare! (deeper still!)
- Entire epidermis lifts off.
- Autoimmune
- Bullous pemphigoid (see in horse on image)
- Thermal burns
- Severe dermal oedema
- Severe interface dermatitis
- but occasionally an artefact!
- Separation of epidermis from dermis
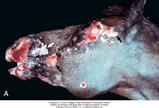
Describe Folliculitis/furunculosis/adenitis?
- Inflammation can affect various hair follicle structures, eg
- Perifollicular vascular plexus
- Perifolliculitis
- Follicular wall
- Mural folliculitis (PF, demodicosis)
- Lumen of hair follicle
- Luminal folliculitis (demodex, dermatophytes)
- Bulb
- Bulbitis (Alopecia areata)
- Sebaceous glands
- Sebaceous adenitis (auto-immune, poodle!)
- Perifollicular vascular plexus
- IF go into the wall, there is probably something in the hair follicle that attracts them and is known as luminal folliculitis.
- IF affects surrounding area and follicular wall, can cause breakdown and get release of hair into the dermis – causes massive foreign body reaction, leading to quite extensive furunculosis.
- If only cenered around bulb of hair follicle = bulbitis; specific pattern seen with alopecia areata.
- Sebaceous gland attack; quite specific attack of the gland.
- Furunculosis = perforating folliculitis with release of keratin into dermis, sets up marked inflammatory response
Describe Atrophic dermatosis?
- Not about inflammation, but instead you are losing structures of the skin! (atropy – dermis/ epidermis can get thinner, lose collagen – image showing classic case of HAC)
- Atrophy of
- Epidermis
- Hair follicles, collagen
- Sebaceous glands
- Orthokeratotic hyperkeratosis
- Follicular keratosis
- +/- calcinosis cutis if HAC
- Various endocrine causes – hormone assays to diagnose (eg HAC, hypothyroidism)
- Any chronic systemic disease or malnutrition etc.
Describe panniculitis?
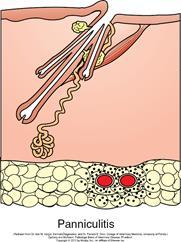
- Epidermis, follicle, dermis ok. Inflammation centred on subcutaneous fat.
- Inflammation of subcutaneous adipose tissue
- Sometimes an extension of follicular disease
- Multiple causes – histology/culture may help detect eg
- Infectious agents
- Vasculitis
- Foreign body
- Pancreatic disease
- Dog with panniculitis commonly seen in PM room with pancreatic disease. Seems to be something with the lipases.
- Often sterile idiopathic
- but must eliminate possibility of infection before treatment with corticosteroids
- Sometimes in dogs with pancreatitis or pancreatic carcinomas. Or in animals with Vitamin E deficiency or trauma
Define
Acanthocyte
Acantholysis
Acanthosis
Acanthocyte – epidermal cell free in a vesicle/pustule, caused by acantholysis
Acantholysis – loss of cohesion between cells of the living epidermis
Acanthosis – hyperplasia of stratum spinosum
Define
Apoptosis
Dyskeratosis
Epidermolysis
Apoptosis – individual cell death, requiring energy
Dyskeratosis - abnormal, premature or imperfect keratinisation of keratinocytes
Epidermolysis – degeneration of epidermal basal layer
–> separation of epidermis from dermis
Define
Exocytosis
Hydropic degeneration
Hyperkeratosis
Exocytosis – migration of inflammatory cells from dermis –> epidermis
Hydropic degeneration – vacuoles in stratum basale –> intrabasal or subepidermal clefts
Hyperkeratosis – increase in stratum corneum (orthokeratotic/parakeratotic; basket-weave/compact)
Define
Intracellular oedema
Necrolysis
Orthokeratosis
Intracellular oedema – occurs with hydropic degeneration of basal cells and ballooning degeneration (seen with herpes virus infections)
Necrolysis – epidermal necrosis with no dermal involvement and minimal inflammation
Orthokeratosis –excessive cornification – keratinocytes lose nuclei
Define
Parakeratosis
Pigment incontinence
Spongiosis
Parakeratosis - excessive cornification – keratinocytes retain nuclei
Pigment incontinence – release of melanin granules into superficial dermis
Spongiosis - intercellular oedema in the epidermis


