What is the first thing you should do if a trauma patient comes in?
- Assess the whole patient for life-threatening injuries –deal with these first! These are important to check before checkingforlimb usage
- Airway
- Breathing
- Circulation
- Provide adequate analgesia, antibiotic cover and fluid support – adequate analgesia should be provided, can also allow you to assess the animal more readily if they are more comfortable. Antibiotics, esp if open fracture. Fluid support to maintain circulation
- Decontaminate and prevent any further contamination of open wounds
- Support grossly unstable fractures –a bit later in assessment andmanagement
- Assess for any neurological signs –the most important thing beyond initial assessment is whether there are any neuro signs Assessment of the trauma patient
Why is analgesia essential for a trauma case?
They will likely be in huge amounts of pain
If they are more comfortable, you can assess them better also
What should all animals involved in an RTA have done as part of the further investigation after airways, breathing and circulation has been checked?
They should always have their chest radiographed - its very easy to miss miaphragmatic hernia and pneumothroax on a normal clinical exam
US of chest may be useful to identify fluid
Check integrity of urinary tract
Check for internal haemorrhage
Monitor patient constantly
What is happening on this radiograph of a dog thats been involved in an RTA?
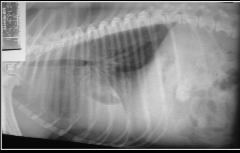
Haemothorax
What is happening on this contrast study radiograph of an animal that has been in an RTA?
What are treatment options?
Assessment of bladder function
At first it looks intact but can then see some leakage into the abdomen as can see free contrast agent
You might leave this and see if it will self heal, may need further treatment
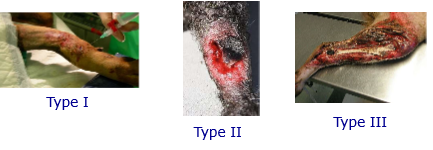
What are the classifications of open fractures?
- Type I -small wound. Little contamination. Treat as closed fracture. May even miss that there has been an open fracture! Treat as if it is. Ab given and wound opened and cleaned as a consequence
- Type II –extensive wound communicating with the fracture. Larger wound, may be able to see fracture within the soft tissues
- Type III –very extensive soft tissue damage and fractured bones are seen protruding through the skin. See relatively frequently, esp distal tibia in cat –comes through small amount of soft tissue in that area. Will be clearly visible and very heavily contaminated
What is a type I classification of an open fracture?
- Type I -small wound. Little contamination. Treat as closed fracture. May even miss that there has been an open fracture! Treat as if it is. Ab given and wound opened and cleaned as a consequence
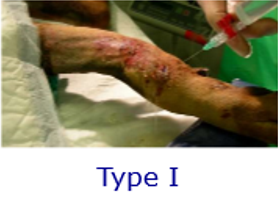
What is a type II open fracture classification?
- Type II –extensive wound communicating with the fracture. Larger wound, may be able to see fracture within the soft tissues
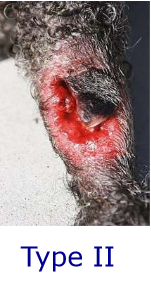
What is a type III open fracture classification?
- Type III –very extensive soft tissue damage and fractured bones are seen protruding through the skin. See relatively frequently, esp distal tibia in cat –comes through small amount of soft tissue in that area. Will be clearly visible and very heavily contaminated
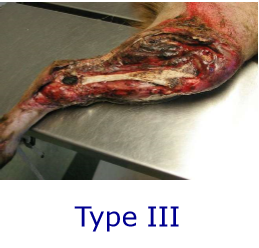
What can a shearing injury also be looked at like?
Shearing injuries could be looked at as a type 3 open fracture
What kind of things do you need to assess with a shearing injury?
Assess:
- blood supply
- damage to deeper tissues:
- nerves and ligaments –more difficult to assess. Ligaments –can check collaterals are intact, if lost malleolus, then the collateral ligaments will have gone with it
- bones
- superficial soft tissues
- These most commonly occur on the medial aspect of the hock or the radiocarpal joint –primarily as they are distal part of limb and little amount of soft tissue to protect them
What should you do to treat an open fracture before any surgical intervention etc?
- sterile water-soluble gel in wound
- wide clip
- Do this before you try to clean!! Clip itupand get all hair out of the way and once you have done this: 3.copious lavage
- Warm haartmans and 19g needle, squeeze into it and remove as much debris as you can.
- In early stages, it is contaminated, but not infected. Might become infected later due to hospital contamination –nosocomial infections! So always be aware of this, so always be sterile when touching and dealing!
- Can remove bits of skin etc. that are clearly dead. But if you are unsure –leave it! Want to maintain as much soft tissue structures as you can
- swab for bacteriology culture
- Rare
- IV broad-spectrum antibiotics
- sterile dressing
- Cover thewound! Prevent any further contamination
What are Pavlectics 6 basic principles with regards to an open fracture?
- Prevent further wound contamination
- Remove foreign debris and contamination
- Debride dead and dying tissue
- Provide adequate wound drainage
- Provide a viable vascular bed
- Select an appropriate method of closure
What is primary closure of a wound/open fracture?
This refers to wound closure immediately following the injury and prior to the formation of granulation tissue. In general, closure by primary intent will lead to faster healing and the best cosmetic result. Most patients presenting within 8 hours of injury can have the wound closed by primary intent. Simple and clean facial wounds, by virtue of the rich vascular supply to the face and the need for a good cosmetic result, can be closed by primary intent as late as 24 hours after the injury.
If primary closure is not an option for a wound/open fracture, how else can it heal?
If primary closure is not an option,
- delayed primary closure
- (pre-granulation)-3-5 days later
- secondary closure
- (granulation tissue present–5-10 d)
- Granulation tissue–pink,sometimes slightly fibrous but fairly vascular tissue. When you have this, you know the woundisnotcontaminated as the wound would not heal like this when contaminated
- second intention healing –leave wound to heal by natural process
- But don’t underestimate the time and cost that this can take! Can take several weeks and sometimes, you might be better to do something like attempt primary closure or refer on to do a skin graft –these can be quicker and less expensive than allowing secondary intention to take place
- granulation, contraction and epithelialisation
- Epithelialisation –around edge of wound, see pink line –cells migrate across surface of wound to cover it.
What is epithelialisation?
Epithelialisation –around edge of wound, see pink line –cells migrate across surface of wound to cover it.
healing by the growth of epithelium over a denudedsurface.
Which one of these wounds is ‘hyper-mature’ and what is this?
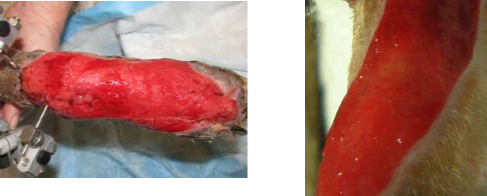
Chronic vs ‘healthy’ granulation tissue
Granulation tissue –can becomehyper mature. If it becomes a little paler and a bit fibrous (like left), this is too mature –needs to be more like right, redder and ‘angrier’
What dressing and bandages should you use for an open fracture/wound?
Which ones change and which stay the same?
- Primary (contact) layer changes
- adherent to wound
Other two layers stay the same:
- Secondary layer –absorbent (avoid maceration) e.g. cotton wool, softban
- Tertiary layer –supportive and allows evaporation –on the surface. Protects dressing from further contamination from environment e.g. Vetwrap, Elastoplast Dressings and
- Also support dressing –rob jones for example –especially if fracture is unstable
- Also helps with animals discomfort
Give an example of a secondary layer to a bandage for an open wound/fracture?
It is absorbent
e.g. cotton wool, softban
What is the tertiary layer of a dressing? give an example
Supportive and allows evaporation, on the surfacec
Protects underlying dressing from further contamination from environemnt
E.g. vetwrap, elastoplast
The primary (contact) layer changes depending upon the stage the wound is at, depending on the degree of damage to the tissues.
What primary layers could you use suring the DEBRIDEMENT STAGE?
Debridement stage: adherent
- wet-to-dry–straight forward,just a swab that you moisten with Hartman’s, place on wound and put light dressing over that, to allow it to dry out. Remove next day. Debride takes away dead tissue as it adheres to tissue as it dries. MOST EFFECTIVE
- dry-to-dry
- Hydrogel
The primary (contact) layer changes depending upon the stage the wound is at, depending on the degree of damage to the tissues.
What primary layers could you use suring the GRANULATION STAGE?
Granulation stage: dry, non-adherent
- Semi occlusive: absorptive e.g. Allevyn–place on and just absorbs some exudate and stores away from wound
- Occlusive: active rehydration e.g. Granuflex
What are the 2 ways you can manage pelvic fractures?
Conservative management
- less invasive, less expense, outcome less predictable (poorer?) and recovery more prolonged. Cage rest, takes 6-8 weeks. Few complications
Surgical management:
- invasive and expensive, but likely to provide more rapid and fuller return to function, rapid pain relief, and potentially better outcomes. Offers much more rapid recovery for the animals –good at giving immediate pain relief and get possibly better return to function, don’t get pelvic narrowing and don’t get distortion of pelvis you don’t get if you manage conservatively
What are some things you should consider when deciding whether a patient with a pelvic fracture needs surgery or not?
- is the patient ambulatory? If its up and walking, little advantage of using surgical stabilisation – the fracture might not be unstable, and as a consequence, they are only marginally displaced and can walk easily
- how long has fracture been present? If cat has been away for a week or so and comes back injured with broken pelvis, difficult to move the fragments if been this long! Better to leave it alone
- is the weight-bearing axis involved? Thw hip,Ileal shaft and then sacroiliac joint –weight baring axis, how weight goes from limbtospine–ifnoneofthisisaffected, animalshouldbeable to walkanddoesn’t really need surgery
- is the acetabulum involved? Articular fracture –if its broken, probably needs surgery! Can lead to OA
- is the pelvic canal diameter reduced ? (<50%) If greater than 50% -consider surgery, don’t want chronic constipation problems • is the patient intractably painful? Pelvis and lumbosacral outflow –if you an stabilise fractures, will reduce pain immediately
- are there multiple problems e.g. limb fracture? It wont be able to manage if its got pelvic fracture and other limb fracture
- But presence of neurological deficits (e.g. bladder function) can affect the decisions made regarding fracture repair Usually operate on ilial, acetabular, and bilateral fractures







